Abstract
Quality of life (QOL) has become an essential measure of a patient’s welfare. In this chapter, we aim to identify the impact of different neurocutaneous syndromes on QOL. Based on these findings, we have made practical recommendations on how clinicians can assess and improve QOL, aided by clinical vignettes.
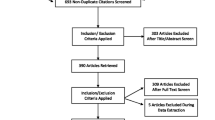
We undertook a comprehensive literature review searching for all the diseases outlined within this book on published works. We identified over 70,000 papers and further searched under the relevant syndrome/disease name and health-related quality of life or quality of life. Of 796 papers, we identified a smaller number including assessment of QOL. We found that the Neurocutaneous Syndromes (NCS) can negatively affect QOL in many ways including variability in impact of different disease manifestations/complications, ill health, pain and the psychosocial domain.
It is important to consider the QOL in all contact with patients and families affected by NCS. Structured assessment, repeated as needed, can be very informative. Appropriate surveillance for the specific syndrome, disease manifestations, complications and age can be challenging. However, with a structured/evidence-based approach, supported with liaison from appropriate experts, management can be optimised with significant implications for quality of life.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
World Health Organisation WHO QOL Measuring Quality of Life. 2012.
Jenkinson C. Quality of life. Encyclopedia Britannica. 2020;
Amin S, Mallick AA, Lux A, O’Callaghan F. Quality of life in patients with tuberous sclerosis complex (TSC). Eur J Paediatr Neurol. 2019;23:801–7.
Vranceanu A-M, Merker VL, Park ER, Plotkin SR. Quality of life among children and adolescents with neurofibromatosis 1: a systematic review of the literature. J Neuro-Oncol. 2015;122:219–28.
Oduber CEU, Khemlani K, Sillevis Smitt JH, et al. Baseline Quality of Life in patients with Klippel–Trenaunay syndrome. J Plastic Reconstr & Aesthetic Surg. 2010;63:603–9.
Huq AJ, Bogwitz M, Gorelik A, et al. Cohort study of Gorlin syndrome with emphasis on standardised phenotyping and quality of life assessment. Internal Med J. 2017;47:664–73.
Kelly MH, Brillante B, Kushner H, et al. Physical function is impaired but quality of life preserved in patients with fibrous dysplasia of bone. Bone. 2005;37:388–94.
Harvey JA, Nguyen H, Anderson KR, et al. Pain, psychiatric comorbidities, and psychosocial stressors associated with Klippel-Trenaunay syndrome. J Amer Acad Dermatol. 2018;79:899–903.
Zarrabeitia R, Fariñas-Álvarez C, Santibáñez M, et al. Quality of life in patients with hereditary haemorrhagic telangiectasia (HHT). Health Qual Life Outcomes. 2017;15:19.
van der Ploeg HM, van der Ploeg MNS, van der Ploeg-Stapert JD. Psychological aspects of the Klippel-Trenaunay syndrome. J Psychosom Res. 1995;39:183–91.
Geirdal AØ, Dheyauldeen S, Bachmann-Harildstad G, Heimdal K. Living with hereditary haemorrhagic telangiectasia: coping and psychological distress - a cross-sectional study. Disabil Rehabil. 2013;35:206–13.
Hagen SL, Grey KR, Korta DZ, Kelly KM. Quality of life in adults with facial port-wine stains. J Am Acad Dermatol. 2017;76:695–702.
Dabora SL, Jozwiak S, Franz DN, et al. Mutational analysis in a cohort of 224 tuberous sclerosis patients indicates increased severity of TSC2, compared with TSC1, disease in multiple organs. Am J Hum Genet. 2001;68:64–80.
Pfister M, Zalaman IM, Blumenstock G, et al. Impact of genotype and mutation type on health-related quality of life in patients with hereditary hemorrhagic telangiectasia. Acta Otolaryngol. 2009;129:8626.
Loaëc M, Morinière S, Hitier M, et al. Psychosocial quality of life in hereditary haemorrhagic telangiectasia patients. Rhinology. 2011;4-7
Staps P, de Groot IJM, van Gerven MHJC, Willemsen MAAP. Daily functioning and quality of life in patients with Sjögren-Larsson syndrome. Neuropediatrics. 2019;50:89–95.
Ferner RE, Huson SM, Thomas N, et al. Guidelines for the diagnosis and management of individuals with neurofibromatosis 1. J Med Genet. 2007;44:81–8.
Dunning-Davies BM, Parker APJ. Annual review of children with neurofibromatosis type 1. Arch Dis Child Educ Pract Ed. 2016;101:102–11.
Amin S, Kingswood JC, Bolton PF, et al. The UK guidelines for management and surveillance of tuberous sclerosis complex. QJM: An Internat J Medic. 2019;112:171–82.
Ng KH, Ng SM, Parker A. Annual review of children with tuberous sclerosis. Arch Dis Child Educ Pract Ed. 2015;100:114–21.
de Vries PJ, Belousova E, Benedik MP, et al. TSC-associated neuropsychiatric disorders (TAND): findings from the TOSCA natural history study. Orphanet J Rare Diseases. 2018;13:157.
Varni JW. The Peds QL measurement model for the paediatric quality of life inventory. pedsql.org.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Parker, A.P.J., Wilkinson, F.J., O’Callaghan, F.J., Amin, S. (2022). Improving Quality of Life in the Neurocutaneous Syndromes. In: Panteliadis, C.P., Benjamin, R., Hagel, C. (eds) Neurocutaneous Disorders. Springer, Cham. https://doi.org/10.1007/978-3-030-87893-1_52
Download citation
DOI: https://doi.org/10.1007/978-3-030-87893-1_52
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-87892-4
Online ISBN: 978-3-030-87893-1
eBook Packages: MedicineMedicine (R0)