Summary
Introduction: Degenerative cervical myelopathy (DCM) leads to functional impairment by compression of the spinal cord and nerve roots. In DCM, the dynamics of cerebrospinal fluid pressure (CSFP) and intraspinal pressure (ISP), as well as spinal cord perfusion pressure (SCPP) remain not investigated yet. Recent technical advances have enabled investigation of these parameters in acute spinal cord injury (SCI). We aim to investigate the properties of CSFP/ISP and spinal cord hemodynamics during and after decompressive surgery in DCM.
Materials and Methods: Four patients with DCM were enrolled; during surgery and 24 h postoperative, ISP at level was measured in one patient, and CSFP was measured in two patients. In one patient, CSFP was recorded at bedside before surgery.
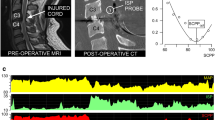
Results: All measurements were conducted without adverse events and were well tolerated. With CSFP analysis, post-decompression Queckenstedt’s test was responsive in two patients (i.e., jugular vein compression resulted in an elevation of CSFP pressure). In the patient whose CSFP was tested at bedside, Queckenstedt’s test was not responsive before decompression. Individual optimum SCPPs were calculated to be between 70 and 75 mmHg.
Conclusion: ISP and CSFP can reflect spinal compression and sufficient decompression. A better understanding and systematic monitoring possibly lead to improved hemodynamic management and may allow early recognition of postoperative complications such as swelling and bleeding.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Davies BM, McHugh M, Elgheriani A, Kolias AG, Tetreault L, Hutchinson PJ, Fehlings MG, Kotter MR (2017) The reporting of study and population characteristics in degenerative cervical myelopathy: a systematic review. PLoS One 12:e0172564. https://doi.org/10.1371/journal.pone.0172564
Davies BM, Mowforth OD, Smith EK, Kotter MR (2018) Degenerative cervical myelopathy. BMJ (Clin Res Ed) 360:k186. https://doi.org/10.1136/bmj.k186
Yamaguchi S, Mitsuhara T, Abiko M, Takeda M, Kurisu K (2018) Epidemiology and overview of the clinical spectrum of degenerative cervical myelopathy. Neurosurg Clin N Am 29:1–12. https://doi.org/10.1016/j.nec.2017.09.001
Fehlings MG, Tetreault LA, Wilson JR, Skelly AC (2013) Cervical spondylotic myelopathy: current state of the art and future directions. Spine 38:S1–S8. https://doi.org/10.1097/BRS.0b013e3182a7e9e0
Fehlings MG, Tetreault L, Hsieh PC, Traynelis V, Wang MY (2016) Introduction: degenerative cervical myelopathy: diagnostic, assessment, and management strategies, surgical complications, and outcome prediction. Neurosurg Focus 40:E1. https://doi.org/10.3171/2016.3.Focus16111
Akter F, Kotter M (2018) Pathobiology of degenerative cervical myelopathy. Neurosurg Clin N Am 29:13–19. https://doi.org/10.1016/j.nec.2017.09.015
Tetreault L, Goldstein CL, Arnold P, Harrop J, Hilibrand A, Nouri A, Fehlings MG (2015) Degenerative cervical myelopathy: a spectrum of related disorders affecting the aging spine. Neurosurgery 77(Suppl 4):S51–S67. https://doi.org/10.1227/neu.0000000000000951
Fujimoto K, Kanchiku T, Imajo Y, Suzuki H, Funaba M, Nishida N, Taguchi T (2017) Use of central motor conduction time and spinal cord evoked potentials in the electrophysiological assessment of compressive cervical myelopathy. Spine 42:895–902. https://doi.org/10.1097/brs.0000000000001939
Liu H, MacMillian EL, Jutzeler CR, Ljungberg E, MacKay AL, Kolind SH, Madler B, Li DKB, Dvorak MF, Curt A, Laule C, Kramer JLK (2017) Assessing structure and function of myelin in cervical spondylotic myelopathy: evidence of demyelination. Neurology 89:602–610. https://doi.org/10.1212/wnl.0000000000004197
Jutzeler CR, Ulrich A, Huber B, Rosner J, Kramer JLK, Curt A (2017) Improved diagnosis of cervical spondylotic myelopathy with contact heat evoked potentials. J Neurotrauma 34:2045–2053. https://doi.org/10.1089/neu.2016.4891
Fehlings MG, Tetreault LA, Kurpad S, Brodke DS, Wilson JR, Smith JS, Arnold PM, Brodt ED, Dettori JR (2017) Change in functional impairment, disability, and quality of life following operative treatment for degenerative cervical myelopathy: a systematic review and meta-analysis. Global Spine J 7:53s–69s. https://doi.org/10.1177/2192568217710137
Fehlings MG, Tetreault LA, Riew KD, Middleton JW, Aarabi B, Arnold PM, Brodke DS, Burns AS, Carette S, Chen R, Chiba K, Dettori JR, Furlan JC, Harrop JS, Holly LT, Kalsi-Ryan S, Kotter M, Kwon BK, Martin AR, Milligan J, Nakashima H, Nagoshi N, Rhee J, Singh A, Skelly AC, Sodhi S, Wilson JR, Yee A, Wang JC (2017) A clinical practice guideline for the management of patients with degenerative cervical myelopathy: recommendations for patients with mild, moderate, and severe disease and nonmyelopathic patients with evidence of cord compression. Global Spine J 7:70s–83s. https://doi.org/10.1177/2192568217701914
Magnaes B, Hauge T (1980) Surgery for myelopathy in cervical spondylosis: safety measures and preoperative factors related to outcome. Spine 5:211–214. https://doi.org/10.1097/00007632-198005000-00002
Pearce JM (2006) Queckenstedt’s manoeuvre. J Neurol Neurosurg Psychiatry 77:728. https://doi.org/10.1136/jnnp.2005.083618
Tachibana S, Iida H, Yada K (1992) Significance of positive Queckenstedt test in patients with syringomyelia associated with Arnold-Chiari malformations. J Neurosurg 76:67–71. https://doi.org/10.3171/jns.1992.76.1.0067
Williams B (1976) Cerebrospinal fluid pressure changes in response to coughing. Brain J Neurol 99:331–346. https://doi.org/10.1093/brain/99.2.331
Kwon BK, Curt A, Belanger LM, Bernardo A, Chan D, Markez JA, Gorelik S, Slobogean GP, Umedaly H, Giffin M, Nikolakis MA, Street J, Boyd MC, Paquette S, Fisher CG, Dvorak MF (2009) Intrathecal pressure monitoring and cerebrospinal fluid drainage in acute spinal cord injury: a prospective randomized trial. J Neurosurg Spine 10:181–193. https://doi.org/10.3171/2008.10.Spine08217
Squair JW, Belanger LM, Tsang A, Ritchie L, Mac-Thiong JM, Parent S, Christie S, Bailey C, Dhall S, Street J, Ailon T, Paquette S, Dea N, Fisher CG, Dvorak MF, West CR, Kwon BK (2017) Spinal cord perfusion pressure predicts neurologic recovery in acute spinal cord injury. Neurology 89:1660–1667. https://doi.org/10.1212/wnl.0000000000004519
Werndle MC, Saadoun S, Phang I, Czosnyka M, Varsos GV, Czosnyka ZH, Smielewski P, Jamous A, Bell BA, Zoumprouli A, Papadopoulos MC (2014) Monitoring of spinal cord perfusion pressure in acute spinal cord injury: initial findings of the injured spinal cord pressure evaluation study*. Crit Care Med 42:646–655. https://doi.org/10.1097/ccm.0000000000000028
Chen S, Smielewski P, Czosnyka M, Papadopoulos MC, Saadoun S (2017) Continuous monitoring and visualization of optimum spinal cord perfusion pressure in patients with acute cord injury. J Neurotrauma 34:2941–2949. https://doi.org/10.1089/neu.2017.4982
Nurick S (1972) The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain J Neurol 95:87–100. https://doi.org/10.1093/brain/95.1.87
Kalsi-Ryan S, Beaton D, Curt A, Duff S, Popovic MR, Rudhe C, Fehlings MG, Verrier MC (2012) The graded redefined assessment of strength sensibility and prehension: reliability and validity. J Neurotrauma 29:905–914. https://doi.org/10.1089/neu.2010.1504
Kaplan L, Kennedy F (1950) The effect of head posture on the manometrics of the cerebrospinal fluid in cervical lesions: a new diagnostic test. Brain J Neurol 73:337–345. https://doi.org/10.1093/brain/73.3.337
Bae YJ, Lee JW, Lee E, Yeom JS, Kim KJ, Kang HS (2017) Cervical compressive myelopathy: flow analysis of cerebrospinal fluid using phase-contrast magnetic resonance imaging. Eur Spine J 26:40–48. https://doi.org/10.1007/s00586-016-4874-9
Gallagher MJ, Hogg FRA, Zoumprouli A, Papadopoulos MC, Saadoun S (2019) Spinal cord blood flow in patients with acute spinal cord injuries. J Neurotrauma 36:919–929. https://doi.org/10.1089/neu.2018.5961
Menacho ST, Floyd C (2019) Current practices and goals for mean arterial pressure and spinal cord perfusion pressure in acute traumatic spinal cord injury: defining the gaps in knowledge. J Spinal Cord Med 16:1–7. https://doi.org/10.1080/10790268.2019.1660840
Rashnavadi T, Macnab A, Cheung A, Shadgan A, Kwon BK, Shadgan B (2019) Monitoring spinal cord hemodynamics and tissue oxygenation: a review of the literature with special focus on the near-infrared spectroscopy technique. Spinal Cord 57:617–625. https://doi.org/10.1038/s41393-019-0304-2
Squair JW, Belanger LM, Tsang A, Ritchie L, Mac-Thiong JM, Parent S, Christie S, Bailey C, Dhall S, Charest-Morin R, Street J, Ailon T, Paquette S, Dea N, Fisher CG, Dvorak MF, West CR, Kwon BK (2019) Empirical targets for acute hemodynamic management of individuals with spinal cord injury. Neurology 93:e1205–e1211. https://doi.org/10.1212/wnl.0000000000008125
Neville L, Egan RA (2005) Frequency and amplitude of elevation of cerebrospinal fluid resting pressure by the Valsalva maneuver. Can J Ophthalmol 40:775–777. https://doi.org/10.1016/s0008-4182(05)80100-0
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Ethics declarations
The authors declare that they have no conflict of interest.
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Zipser, C.M. et al. (2021). Safety and Feasibility of Lumbar Cerebrospinal Fluid Pressure and Intraspinal Pressure Studies in Cervical Stenosis: A Case Series. In: Depreitere, B., Meyfroidt, G., Güiza, F. (eds) Intracranial Pressure and Neuromonitoring XVII. Acta Neurochirurgica Supplement, vol 131. Springer, Cham. https://doi.org/10.1007/978-3-030-59436-7_70
Download citation
DOI: https://doi.org/10.1007/978-3-030-59436-7_70
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-59435-0
Online ISBN: 978-3-030-59436-7
eBook Packages: MedicineMedicine (R0)