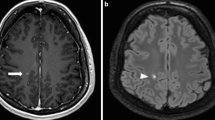
Abstract
Particularly in endemic regions, parenchymal neuro-Behçet syndrome (p-NBS) should be considered in the differential diagnosis when patients are admitted with chronic and progressive gait disturbances. As there are no other biomarkers for NBS, magnetic resonance imaging (MRI) remains the gold standard in the differential diagnosis of p-NBS as well as in predicting prognosis and treatment response. The most commonly confused disease with p-NBS is multiple sclerosis. One of the main clinical differences between p-NBS and MS is that patients with the relapsing form of MS usually recover well, while those with the relapsing form of p-NBS do not. The other difference between MS and NBS relies on different MRI patterns and cerebrospinal fluid findings.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Kocer N, Islak C, Siva A, et al. CNS involvement in neuro-Behcet’s syndrome: an MR study. Am J Neuroradiol. 1999;20:1015–24.
Siva A, Saip S. The spectrum of nervous system involvement in Behcet’s syndrome and its differential diagnosis. J Neurol. 2009;256:513–29.
Lee HS, Kim do Y, Shin HY, et al. Spinal cord involvement in Behcet’s disease. Mult Scler. 2016;22:960–3.
Uygunoglu U, Pasha M, Saip S, Siva A. Recurrent longitudinal extensive transverse myelitis in a neuro-Behcet syndrome treated with infliximab. J Spinal Cord Med. 2015;38:111–4.
Uygunoglu U, Zeydan B, Ozguler Y, et al. Myelopathy in Behcet’s disease: the bagel sign. Ann Neurol. 2017;82:288–98.
Siva A. Common clinical and imaging conditions misdiagnosed as multiple sclerosis: a current approach to the differential diagnosis of multiple sclerosis. Neurol Clin. 2018;36:69–117.
Siva A, Esatoglu SN, Uygunoglu U, et al. Could neurological involvement in Behcet’s disease occur atypically? (P5.410). Neurology. 2018;90(15 Supplement).
Maggi P, Absinta M, Grammatico M, et al. Central vein sign differentiates multiple sclerosis from central nervous system inflammatory vasculopathies. Ann Neurol. 2018;83:283–94.
Cohen-Aubart F, Psimaras D, Galanaud D, et al. Cerebral pseudo-tumoral neuro-Behcet: histological demonstration of an inflammatory and vascular disease. Clin Neurol Neurosurg. 2017;161:48–50.
Imataki O, Uchida S, Yokokura S, Uemura M, Kadowaki N. Central nervous system peripheral T cell lymphoma manifesting as Lymphomatosis cerebri that was misdiagnosed as Neuro-Behçet’s disease: a case report. Case Rep Oncol. 2018;11(3):806–13.
Taskapilioglu O, Seferoglu M, Akkaya C, et al. Delayed diagnosis of a neuroBehcet patient with only brainstem and cerebellar atrophy: literature review. J Neurol Sci. 2009;277:160–3.
Yazici H, Seyahi E, Hatemi G, Yazici Y. Behcet syndrome: a contemporary view. Nat Rev Rheumatol. 2018;14:107–19.
Uygunoglu U, Saip S, Siva A. Chapter 28: Behcet’s syndrome and nervous system involvement. In: Lisak RP, Truong DD, Carroll WM, et al., editors. International neurology. 2nd ed. Chichester/Hoboken: John Wiley & Sons, Ltd; 2016. p. 88–93.
Uygunoğlu U, Siva A. Behçet’s syndrome and nervous system involvement. Curr Neurol Neurosci Rep. 2018;18(7):35.
Salvarani C, Brown RD Jr, Calamia KT, et al. Primary central nervous system vasculitis: analysis of 101 patients. Ann Neurol. 2007;62(5):442–51.
Yesilot N, Bahar S, Yilmazer S, et al. Cerebral venous thrombosis in Behcet’s disease compared to those associated with other etiologies. J Neurol. 2009;256:1134–42.
Saruhan-Direskeneli G, Yentür SP, Mutlu M, Shugaiv E, Yesilot N, Kürtüncü M, et al. Intrathecal oligoclonal IgG bands are infrequently found in neuro-Behçet’s disease. Clin Exp Rheumatol. 2013;31(3 Suppl 77):25–7.
Hirohata S, Isshi K, Oguchi H, et al. Cerebrospinal fluid interleukin-6 in progressive neuro-Behçet’s syndrome. Clin Immunol Immunopathol. 1997;82(1):12–7.
Akman-Demir G, Tuzun E, Icoz S, et al. Interleukin-6 in neuro-Behçet’s disease: association with disease subsets and long-term outcome. Cytokine. 2008b;44(3):373–6.
Hirohata S, Kikuchi H. Changes in biomarkers focused on differences in disease course or treatment in patients with neuro-Behçet’s disease. Intern Med. 2012a;51(24):3359–65.
Aldinucci A, Bonechi E, Biagioli T, et al. CSF/serum matrix metallopeptidase-9 ratio discriminates neuro Behçet from multiple sclerosis. Ann Clin Transl Neurol. 2018;5(4):493–8.
Belghith M, Bahrini K, Kchaou M, Maghrebi O, Belal S, Barbouche MR. Cerebrospinal fluid IL-10 as an early stage discriminative marker between multiple sclerosis and neuro-Behçet disease. Cytokine. 2018;108:160–7.
Berlin C. Behçet syndrome with involvement of the central nervous system. Arch Derm Syphilol. 1944;49:227–33.
McMenemey WH, Lawrence BJ. Encephalomyelopathy in Behçet disease: report of necropsy findings in two cases. Lancet. 1957;2:353–8.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Uygunoglu, U., Siva, A. (2021). Neuro-Behçet Syndrome: Differential Diagnosis. In: Tüzün, E., Kürtüncü, M. (eds) Neuro-Behçet’s Disease. Springer, Cham. https://doi.org/10.1007/978-3-030-55273-2_7
Download citation
DOI: https://doi.org/10.1007/978-3-030-55273-2_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-55272-5
Online ISBN: 978-3-030-55273-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)