Abstract
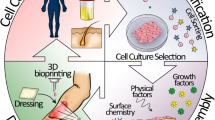
We aim to show that deeper needling of skin (1–3 mm depth) is a valuable tool for treating people with burn scars. Currently, numerous ablative cutaneous treatments and surgical procedures are the mainstay of treating burn scars. Needling takes us to a new paradigm of instigating a regenerative phase to remove scar collagen and replace it with normal lattice-patterned collagen, thereby reducing the appearance of nodular hypertrophic scars and contractions. This occurs because skin needling causes perforation of blood vessels and an automatic cascade of platelet-derived growth factors. The dominant growth factor is TGF-β3 which surges after needling in a way not seen in normal adult tissues but which is the usual pattern found in foetal regenerative wound repair. By repeating needling treatments, one can flatten hypertrophic/burn keloid scars and soften contractures and get closer to the ideal treatment of scars. The authors believe that skin needling should be done reasonably soon after the initial injury.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Rawlins JM, Lam WL, Karoo RO, Naylor IL, Sharpe DT. Quantifying collagen type in mature burn scars: a novel approach using histology and digital image analysis. J Burn Care Res. 2006;27(1):60–5.
Roy D. Ablative facial resurfacing. Dermatol Clin. 2005;23(3):549–59.. viii
Avram MM, Tope WD, Yu T, Szachowicz E, Nelson JS. Hypertrophic scarring of the neck following ablative fractional carbon dioxide laser resurfacing. Lasers Surg Med. 2009;41(3):185–8.
Costa IM, Damasceno PS, Costa MC, Gomes KG. Review in peeling complications. J Cosmet Dermatol. 2017;16(3):319–26.
Aust MC, Fernandes D, Kolokythas P, Kaplan HM, Vogt PM. Percutaneous collagen induction therapy: an alternative treatment for scars, wrinkles, and skin laxity. Plast Reconstr Surg. 2008;121(4):1421–9.
Fernandes D, Signorini M. Combating photoaging with percutaneous collagen induction. Clin Dermatol. 2008;26(2):192–9.
Aust MB, Fernandes SD. Illustrated guide to percutaneous collagen induction: basics, indications, use. New Malden: Quintessence Publishing; 2013.
Camirand A, Doucet J. Needle dermabrasion. Aesthet Plast Surg. 1997;21(1):48–51.
Orentreich DS, Orentreich N. Subcutaneous incisionless (subcision) surgery for the correction of depressed scars and wrinkles. Dermatol Surg. 1995;21(6):543–9.
Fernandes D. Percutaneous collagen induction: an alternative to laser resurfacing. Aesthet Surg J. 2002;22(3):307–9.
Aust MC, Knobloch K, Reimers K, Redeker J, Ipaktchi R, Altintas MA, et al. Percutaneous collagen induction therapy: an alternative treatment for burn scars. Burns. 2010;36(6):836–43.
Aust MC, Reimers K, Kaplan HM, Stahl F, Repenning C, Scheper T, et al. Percutaneous collagen induction-regeneration in place of cicatrisation? J Plast Reconstr Aesthet Surg. 2011;64(1):97–107.
Aust MC, Reimers K, Gohritz A, Jahn S, Stahl F, Repenning C, et al. Percutaneous collagen induction. Scarless skin rejuvenation: fact or fiction? Clin Exp Dermatol. 2010;35(4):437–9.
El-Domyati M, Barakat M, Awad S, Medhat W, El-Fakahany H, Farag H. Microneedling therapy for atrophic acne scars: an objective evaluation. J Clin Aesthet Dermatol. 2015;8(7):36–42.
El-Domyati M, Barakat M, Awad S, Medhat W, El-Fakahany H, Farag H. Multiple microneedling sessions for minimally invasive facial rejuvenation: an objective assessment. Int J Dermatol. 2015;54(12):1361–9.
Ferguson MW, O'Kane S. Scar-free healing: from embryonic mechanisms to adult therapeutic intervention. Philos Trans R Soc Lond Ser B Biol Sci. 2004;359(1445):839–50.
Schultz GS, Wysocki A. Interactions between extracellular matrix and growth factors in wound healing. Wound Repair Regen. 2009;17(2):153–62.
Bandyopadhyay B, Fan J, Guan S, Li Y, Chen M, Woodley DT, et al. A “traffic control” role for TGFbeta3: orchestrating dermal and epidermal cell motility during wound healing. J Cell Biol. 2006;172(7):1093–105.
Occleston NL, Fairlamb D, Hutchison J, O'Kane S, Ferguson MW. Avotermin for the improvement of scar appearance: a new pharmaceutical in a new therapeutic area. Expert Opin Investig Drugs. 2009;18(8):1231–9.
Aust MC, Reimers K, Repenning C, Stahl F, Jahn S, Guggenheim M, et al. Percutaneous collagen induction: minimally invasive skin rejuvenation without risk of hyperpigmentation-fact or fiction? Plast Reconstr Surg. 2008;122(5):1553–63.
Yamaguchi Y, Hearing VJ. Melanocytes and their diseases. Cold Spring Harb Perspect Med. 2014;4(5):a017046.
Alam M, Warycha M. Complications of lasers and light treatments. Dermatol Ther. 2011;24(6):571–80.
Vaiyavatjamai P, Wattanakrai P. Side effects and complications of fractional 1550-nm erbium fiber laser treatment among Asians. J Cosmet Dermatol. 2011;10(4):313–6.
Onur E. The treatment of burn scar hypopigmentation and surface irregularity by dermabrasion and thin skin grafting. Plast Reconstr Surg. 1990;85(5):754–8.
Kahn AM, Cohen MJ. Treatment for depigmentation following burn injuries. Burns. 1996;22(7):552–4.
Cho S, Zheng Z, Park Y-K, Roh MR. The 308-nm excimer laser: a promising device for the treatment of childhood vitiligo. Photodermatol Photoimmunol Photomed. 2011;27(1):24–9.
Stoner M, Wood F. The treatment of hypopigmented lesions with cultured epithelial autograft. J Burn Care Rehabil. 2000;21:50–4.
Zhang DM, Hong WS, Fu LF, Wei XD, Xu AE. A randomized controlled study of the effects of different modalities of narrow-band ultraviolet B therapy on the outcome of cultured autologous melanocytes transplantation in treating vitiligo. Dermatol Surg. 2014;40(4):420–6.
Ross EV, Naseef GS, McKinlay JR, Barnette DJ, Skrobal M, Grevelink J, et al. Comparison of carbon dioxide laser, erbium:YAG laser, dermabrasion, and dermatome. J Am Acad Dermatol. 2000;42(1):92–105.
Laws RA, Finley EM, McCollough ML, Grabski WJ. Alabaster skin after carbon dioxide laser resurfacing with histologic correlation. Dermatol Surg. 1998;24(6):633–6.
Bernstein LJ, Kauvar ANB, Grossman MC, Geronemus RG. The short- and long-term side effects of carbon dioxide laser resurfacing. Dermatol Surg. 1997;23(7):519–25.
Thomas JR, Somenek M. Scar revision review. Arch Facial Plast Surg. 2012;14(3):162–74.
Busch KH, Bender R, Walezko N, Aziz H, Altintas MA, Aust MC. Combination of medical needling and non-cultured autologous skin cell transplantation (ReNovaCell) for repigmentation of hypopigmented burn scars. Burns. 2016;42(7):1556–66.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Aust, M., Fernandes, D., Bender, R. (2020). The Value of Medical Needling in Burn Scars. In: Kamolz, LP., Jeschke, M.G., Horch, R.E., Küntscher, M., Brychta, P. (eds) Handbook of Burns Volume 2. Springer, Cham. https://doi.org/10.1007/978-3-030-34511-2_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-34511-2_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-34510-5
Online ISBN: 978-3-030-34511-2
eBook Packages: MedicineMedicine (R0)