Abstract
Precision medicine in oncology aims to treat a patient based on the molecular makeup of the individual’s tumor. Guidelines have already been adopted in certain tumor types for the use of targeted therapies as standard of care, including lung, colon and rectum, thyroid, kidney, and breast cancers; melanoma; and gastrointestinal stromal tumors. Of these tumor types, Latinos have a higher overall incidence rate of colorectal cancer and a higher overall mortality rate from thyroid cancer than non-Latino whites in the United States, though these trends may vary by state. While the potential benefit of precision medicine is substantial, research has shown that its implementation in the Latino population is limited. At the Rutgers Cancer Institute of New Jersey (RCINJ), during 2013–2017, 65.3% of new patient visits were non-Latino white patients and 8.9% were Latino. In a clinical trial evaluating the outcomes of patients who have had genomic testing on their tumors (N = 770), 71% were non-Latino white patients, while 11% were Latino. This ongoing trial consistently demonstrates that targeted therapy based on genomic profiling of tumors improves outcomes in cancer care and that Latinos are willing to participate in the clinical trial that involves genomic testing at a cancer center.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
In 2016, people of Latino ancestry comprised 17.8% (57,398,719) of the total estimated US population (323,127,515) [1]. The states with the highest percentages of people of Latino ancestry include New Mexico, Texas, California, Arizona, and Nevada, with New Jersey ranking eighth. However, these data reflect an ethnicity that is far from homogenous. The term “Latino” encompasses a wide range of people from a large geographical area. Varying elements, such as culture, environment, and genetic makeup, foster diversity among people of Latino ancestry.
Precision medicine focuses on treating cancer based on the molecular alterations and dysfunctions within a tumor, not solely on the tumor type itself. It provides a more streamlined approach to cancer care, allowing an individual patient’s tumor to be specifically targeted with available treatments, some of which may be FDA-approved for other diseases or tumors.
There is a great potential to treat cancer patients using precision medicine; however, research shows that its implementation in the Latino population is limited. For example, Latino representation in The Cancer Genome Atlas is <3%. In a 2016 analysis of genome-wide association studies, Popejoy and Fullerton showed that while nearly 20% of participants were of non-European descent, less than 1% were Latino [2]. While the data show that physicians have been less likely to offer genomic testing (including germline BRCA1/2 testing for breast cancer) to Latino versus white non-Latino women, there is evidence that Latino patients have positive attitudes and the willingness to participate in testing [3, 4]. The diversity among Latinos lends itself to the application of this targeted method of cancer care, but concern exists over whether a gap in the practice of precision medicine exists in this population.
Background
Latino Populations in the United States
Based on data from the US Census Bureau, 2016 American Community Survey (1-Year Estimates), the top 10 states with the highest percentages of people of Latino ancestry included New Mexico (48.5%), Texas (39.1%), California (38.9%), Arizona (30.9%), Nevada (28.5%), Florida (24.9%), Colorado (21.3%), New Jersey (20.0%), New York (19.0%), and Illinois (17.0%) [5]. Among these states, the most prevalent subpopulations of ethnicities varied from Mexican in New Mexico, Texas, California, Arizona, Nevada, Colorado, and Illinois to Cuban in Florida and to Puerto Rican in New Jersey and New York [5].
Latino Populations in New Jersey
Based on data from the US Census Bureau, 2016 American Community Survey (1-Year Estimates), ancestries within the Latino populations in New Jersey were 26.3% Puerto Rican, followed by Dominican (15.2%), Mexican (13.7%), Colombian (7.0%), Ecuadorian (6.7%), Peruvian (5.5%), Cuban (4.8%), and Salvadoran (4.6%) [6]. New Jersey is home to a diverse array of people of Latino ancestry, providing a unique opportunity for the Rutgers Cancer Institute of New Jersey (RCINJ), an NCI-designated comprehensive cancer center, to understand precision medicine and potential cancer-care disparities within the Latino population.
Targeted Therapies as Standard of Care
With a growing focus on cancer therapies that target dysregulated proteins along signaling pathways, guidelines for standard of care treatments for a wide array of cancer types have begun incorporating targeted agents into their clinical recommendations. For example, bevacizumab, a VEGF inhibitor has been recommended in National Comprehensive Cancer Network (NCCN) guidelines for some brain and CNS cancers, such as anaplastic gliomas and glioblastomas [7]. The NCCN guidelines have also incorporated targeted agents into their clinical guidelines for such cancer types as ovarian, thyroid, breast, and colorectal cancers [8,9,10,11].
Cancer Incidence and Mortality Rates Among Patients of Latino Ancestry
Among brain and CNS cancers, ovarian cancer, thyroid cancer, breast cancer, and colorectal cancer, data on 5-year (2010–2014), age-adjusted incidence rates (cases per 100,000) and death rates (deaths per 100,000) from the US Department of Health and Human Services on State Cancer Profiles show the following [12].
Brain and CNS Cancers
The highest incidence rates of brain and CNS cancers among Latinos are reported in Florida (6.1), Connecticut (6.1), Rhode Island (6.0), and New Jersey (6.0). Nonetheless, the incidence rates of cancers of the brain and CNS in each of these states are higher in non-Latino whites who also suffer higher mortality rates for brain and CNS cancers than Latinos in these states.
Breast Cancer
The highest incidence rates of breast cancer among Latinos are reported in Hawaii (151.6), Montana (134.3), Connecticut (127.5), and Oklahoma and Colorado (tied at 104.4). Of these five states, incidence rates of this cancer type in non-Latino whites are higher in Connecticut, Oklahoma, and Colorado. In each of the aforementioned states, non-Latino whites have higher mortality rates for breast cancer than Latinos.
Ovarian Cancer
The highest incidence rates of ovarian cancer among Latinos are reported in Oklahoma (15.7), Colorado (12), Wisconsin (11.2), and Virginia and New Mexico (tied at 11.1). Of these five states, incidence rates of this cancer type in non-Latino whites are higher in Wisconsin, Virginia, and New Mexico. This population also has higher mortality rates for ovarian cancer than Latinos in each of the aforementioned states.
Colorectal Cancer
The highest incidence rates of colorectal cancer among Latinos are reported in Hawaii (43.3), Connecticut (42.9), Montana (42), and New Jersey (38.9). Incidence rates of this cancer type in non-Latino whites are lower in each of these four states. In all of the aforementioned states except Hawaii, non-Latino whites have higher mortality rates for colorectal cancer than Latinos.
Thyroid Cancer
The highest incidence rates of thyroid cancer among Latinos are reported in Connecticut (21.2), Utah (19.6), New Hampshire (18.7), and Montana (18.3). Of these four states, incidence rates of this cancer type in non-Latino whites are all lower. In each of the four aforementioned states, the mortality rates are higher among non-Latino whites.
Our Experience
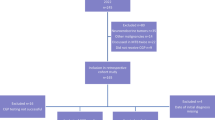
At the Rutgers Cancer Institute of New Jersey (RCINJ), we designed a protocol that longitudinally follows patients with rare or refractory tumors who underwent tumor genomic profiling (NCT02688517). Patients provided their informed consent to participate in this study, which was approved by the Rutgers University New Brunswick Health Sciences IRB (Pro2012002075).
Using precision medicine at RCINJ, we analyzed readily available data from selected tumor groups to determine if disparities exist between Latino patients and non-Latino whites. Initial analysis of 93 patients shows that 43 patients were of Latino ancestry, while 50 patients were non-Latino white (Table 14.1). Cancer groups included breast, central nervous system (CNS), colorectal, gastrointestinal, genitourinary, gynecologic, thyroid, pulmonary, skin, unknown primary, and other cancers. The median ages for Latino patients and non-Latino white patients were 50 and 60.5 years, respectively.
Next-Generation Sequencing (NGS)
Formalin-fixed, paraffin-embedded tumor specimens were sent to a Clinical Laboratory Improvement Amendments (CLIA)-approved, laboratory for next-generation sequencing. Sequencing included the entire coding regions of cancer-related genes as well as introns of genes involved in fusions.
Results
Thirty-three percent of Latino ancestry patients and 30% of non-Latino white patients received targeted therapy. Interestingly, patients of Latino ancestry who received targeted therapy survived an average of 10 months longer than their white counterparts. In addition, Latino ancestry patients who did not receive targeted therapy survived an average of 4 months longer than their non-Latino white counterparts. Paradoxically, the Latino ancestry patients had more advanced disease (higher stage) at the time of diagnosis.
Discussion
Precision medicine in cancer care provides physicians with the ability to offer targeted treatment options to patients based on the molecular makeup of the individuals’ tumor. Given disparities in cancer healthcare in Latino populations and the cost and effort involved in genomic testing, we hypothesized that precision medicine has the potential to increase disparities in care for Latino ancestry patients and may hinder the progress of precision-based medicine in this population. In this study, we found that, at our institution, there may not be a disparity between Latino ancestry patients and non-Latino white patients with regard to the implementation of precision medicine in their clinical care. A limitation to our study is the small sample size. Having a larger sample size may affect the outcome of our analysis, and an ongoing analysis will contribute to our final conclusions.
The Cancer Genome Atlas (TCGA) provides a large repository for data on genomic characteristics of tumors, which have been de-identified but made publicly available [13, 14]. Hispanics were recently shown to represent <3% (N = 5729, n = 149) of the patients included in the TCGA database [15]. This finding reflects the underrepresentation of Latinos on larger and broader genome studies.
Targeted treatments are being recommended as standard of care for many cancer types. For example, the guidelines of the National Comprehensive Cancer Network (NCCN) recommend the immune checkpoint inhibitors, nivolumab or pembrolizumab, for colon and rectal cancers that are mismatch repair deficient or have microsatellite instability, and agents targeting receptor tyrosine kinases (e.g., vandetanib, cabozantinib, lenvatinib, and sorafenib) in some thyroid cancer types [8, 9]. Given the higher incidence rates of these two cancers in Latinos, it is crucial to ensure that this population has access to tumor molecular analysis.
References
U.S. Census Bureau. American Community Survey 5-Year Estimates. 2012–2016. https://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=ACS_16_5YR_B03003&prodType=table.Accessed 25 Jan 2018.
Popejoy AB, Fullerton SM. Genomics is failing on diversity. Nature. 2016;538(7624):161–4. https://doi.org/10.1038/538161a.
Cragun D, Weidner A, Lewis C, Bonner D, Kim J, Vadaparampil ST, et al. Racial disparities in BRCA testing and cancer risk management across a population-based sample of young breast cancer survivors. Cancer. 2017;123(13):2497–505. https://doi.org/10.1002/cncr.30621.
Ramirez AG, Chalela P, Gallion KJ, Munoz E, Holden AE, Burhansstipanov L, et al. Attitudes toward breast cancer genetic testing in five special population groups. J Health Dispar Res Pract. 2015;8(4):124–35.
U.S. Census Bureau. American Community Survey 1-Year Estimates. Hispanic or Latino origin by specific origin: United States. 2016. https://factfinder.census.gov/faces/nav/jsf/pages/index.xhtml. Accessed 1 Feb 2018.
U.S. Census Bureau. American Community Survey 1-Year Estimates. Hispanic or Latino origin by specific origin: New Jersey. 2016. https://factfinder.census.gov/faces/nav/jsf/pages/index.xhtml. Accessed 1 Feb 2018.
National Comprehensive Cancer Network (NCCN), Inc. NCCN guidelines version 1.2017-August 18, 2017: central nervous system cancers. https://www.nccn.org/. Accessed 11 Dec 2017.
National Comprehensive Cancer Network (NCCN), Inc. NCCN guidelines version 2.2017-May 17, 2017: thyroid carcinoma. https://www.nccn.org/. Accessed 11 Dec 2017.
National Comprehensive Cancer Network (NCCN), Inc. NCCN guidelines version 2.2017-March 13, 2017: colon cancer. https://www.nccn.org/. Accessed 11 Dec 2017.
National Comprehensive Cancer Network (NCCN), Inc. NCCN guidelines version 4.2017-November 9, 2017: ovarian cancer including fallopian tube cancer and primary peritoneal cancer. https://www.nccn.org/. Accessed 11 Dec 2017.
National Comprehensive Cancer Network (NCCN), Inc. NCCN guidelines version 3.2017-November 10, 2017: breast cancer. https://www.nccn.org/. Accessed 11 Dec 2017.
U.S. Department of Health and Human Services. State cancer profiles. https://statecancerprofiles.cancer.gov/index.html. Accessed 27 Nov 2017.
Cerami E, Gao J, Dogrusoz U, Gross BE, Sumer SO, Aksoy BA, et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov. 2012;2(5):401–4. https://doi.org/10.1158/2159-8290.CD-12-0095.
Gao J, Aksoy BA, Dogrusoz U, Dresdner G, Gross B, Sumer SO, et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci Signal. 2013;6(269):pl1. https://doi.org/10.1126/scisignal.2004088.
Spratt DE, Chan T, Waldron L, Speers C, Feng FY, Ogunwobi OO, et al. Racial/ethnic disparities in genomic sequencing. JAMA Oncol. 2016;2(8):1070–4. https://doi.org/10.1001/jamaoncol.2016.1854.
Acknowledgments
We thank the patients; Frances Di Clemente for assistance with data abstraction and analysis; Joseph Miktus, Erin Caswell, and Sindy Simoes; and the service provided by the Biospecimen Repository Service Core Facility. We thank Susan Moench and Jennifer Hostettler for assistance with drafting and editing.
Funding: This research was supported by a generous gift to the Genetics Diagnostics to Cancer Treatment Program of the Rutgers Cancer Institute of New Jersey and RUCDR Infinite Biologics and NIH P30CA072720.
Ethics Statement: The patients provided informed consent to participate in the Rutgers CINJ genomic tumor profiling protocol (NCT02688517), which was approved by the Institutional Review Board (IRB) of Rutgers University New Brunswick Health Sciences (Pro2012002075).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2020 The Author(s)
About this chapter
Cite this chapter
Rodriguez-Rodriguez, L. (2020). Is Precision Medicine Widening Cancer Care Disparities in Latino Populations? The Rutgers Cancer Institute of New Jersey Experience. In: Ramirez, A., Trapido, E. (eds) Advancing the Science of Cancer in Latinos. Springer, Cham. https://doi.org/10.1007/978-3-030-29286-7_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-29286-7_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-29285-0
Online ISBN: 978-3-030-29286-7
eBook Packages: MedicineMedicine (R0)