Abstract
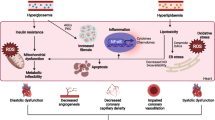
Betaine supplementation has been shown to alleviate altered glucose and lipid metabolism in mice fed a high-fat diet or a high-sucrose diet. We investigated the beneficial effects of betaine in diabetic db/db mice. Alleviation of endoplasmic reticulum (ER) and oxidative stress was also examined in the livers and brains of db/db mice fed a betaine-supplemented diet. Male C57BL/KsJ-db/db mice were fed with or without 1% betaine for 5 wk (referred to as the db/db-betaine group and the db/db group, respectively). Lean non-diabetic db/+ mice were used as the control group. Betaine supplementation significantly alleviated hyperin-sulinemia in db/db mice. Betaine reduced hepatic expression of peroxisome proliferator-activated receptor gamma coactivator 1 alpha, a major transcription factor involved in gluconeogenesis. Lower serum triglyceride concentrations were also observed in the db/db-betaine group compared to the db/db group. Betaine supplementation induced hepatic peroxisome proliferator-activated receptor alpha and carnitine palmitoyl-transferase 1a mRNA levels, and reduced acetyl-CoA carboxylase activity. Mice fed a betaine-supple-mented diet had increased total glutathione concentrations and catalase activity, and reduced lipid peroxidation levels in the liver. Furthermore, betaine also reduced ER stress in liver and brain. c-Jun N-ter-minal kinase activity and tau hyperphosphorylation levels were lower in db/db mice fed a betaine-supple-mented diet, compared to db/db mice. Our findings suggest that betaine improves hyperlipidemia and tau hyperphosphorylation in db/db mice with insulin resistance by alleviating ER and oxidative stress.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Abbreviations
- ACC:
-
Acetyl-CoA carboxylase
- AD:
-
Alzheimer’s disease
- BiP:
-
Immunoglobin heavy chain-binding protein
- CPT1a:
-
Carnitine palmitoyltransferase 1a
- eIF2gα:
-
Eukaryotic translation initiation factor 2 alpha
- ER:
-
Endoplasmic reticulum
- GSH:
-
Glu-tathione
- HO-1:
-
Heme oxygenase 1
- HOMA-IR:
-
Homeostatic model assessment of insulin resistance
- JNK:
-
C-Jun N-terminal kinase
- PGC-1gα:
-
Peroxisome proliferator-activated receptor gamma coacti-vator-1 alpha
- PPARgα:
-
Peroxisome proliferator-activated receptor alpha
- RPL19:
-
Ribosomal protein L19
- SCD1:
-
Stearyl-CoA desatu-rase
- TBARS:
-
Thiobarbituric acid reactive substance
- VLDL:
-
very-low-density lipoprotein
- XBP-1:
-
X-box binding protein 1
References
Kumashiro, N., Tamura, Y., Uchida, T., Ogihara, T., Fujitani, Y., Hirose, T., Mochizuki, H., Kawamori, R. and Watada, H. (2008) Impact of oxidative stress and peroxisome proliferator-activated receptor gamma coactivator-1alpha in hepatic insulin resistance. Diabetes, 57, 2083–2091.
Ozcan, U., Cao, Q., Yilmaz, E., Lee, A.H., Iwakoshi, N.N., Ozdelen, E., Tuncman, G., Görgün, C., Glimcher, L.H. and Hotamisligil, G.S. (2004) Endoplasmic reticulum stress links obesity, insulin action, and type 2 diabetes. Sci., 306, 457–461.
Nakatani, Y., Kaneto, H., Kawamori, D., Yoshiuchi, K., Hatazaki, M., Matsuoka, T.A., Ozawa, K., Ogawa, S., Hori, M., Yamasaki, Y. and Matsuhisa, M. (2005) Involvement of endoplasmic reticulum stress in insulin resistance and diabetes. J. Biol. Chem., 280, 847–851.
Han, M.S., Chung, K.W., Cheon, H.G., Rhee, S.D., Yoon, C.H., Lee, M.K., Kim, K.W. and Lee, M.S. (2009) Imatinib mesylate reduces endoplasmic reticulum stress and induces remission of diabetes in db/db mice. Diabetes, 58, 329–336.
Han, K.L., Choi, J.S., Lee, J.Y., Song, J., Joe, M.K., Jung, M.H. and Hwang, J.K. (2008) Therapeutic potential of peroxi-some proliferators—activated receptor-alpha/gamma dual agonist with alleviation of endoplasmic reticulum stress for the treatment of diabetes. Diabetes, 57, 737–745.
Profenno, L.A., Porsteinsson, A.P. and Faraone, S.V. (2010) Meta-analysis of Alzheimer’s disease risk with obesity, diabetes, and related disorders. Biol. Psychiatry, 67, 505–512.
Beydoun, M.A., Beydoun, H.A. and Wang, Y. (2008) Obesity and central obesity as risk factors for incident dementia and its subtypes: a systematic review and meta-analysis. Obes. Rev., 9, 204–218.
Zhao, W.Q., Chen, H., Quon, M.J. and Alkon, D.L. (2004) Insulin and the insulin receptor in experimental models of learning and memory. Eur. J. Pharmacol., 490, 71–81.
Planel, E., Tatebayashi, Y., Miyasaka, T., Liu, L., Wang, L., Herman, M., Yu, W.H., Luchsinger, J.A., Wadzinski, B., Duff, K.E. and Takashima, A. (2007) Insulin dysfunction induces in vivo tau hyperphosphorylation through distinct mechanisms. J. Neurosci., 27, 13635–13648.
Ueland, P.M. (2011) Choline and betaine in health and disease. J. Inherited Metab. Dis., 34, 3–15.
Ji, C. and Kaplowitz, N. (2003) Betaine decreases hyperho-mocysteinemia, endoplasmic reticulum stress, and liver injury in alcohol-fed mice. Gastroenterology, 124, 1488–1499.
Ji, C., Shinohara, M., Kuhlenkamp, J., Chan, C. and Kaplowitz, N. (2007) Mechanisms of protection by the betaine-homocysteine methyltransferase/betaine system in HepG2 cells and primary mouse hepatocytes. Hepatology, 46, 1586–1596.
Erman, F., Balkan, J., Cevikbas, U., Koçak-Toker, N. and Uysal, M. (2004) Betaine or taurine administration prevents fibrosis and lipid peroxidation induced by rat liver by ethanol plus carbon tetrachloride intoxication. Amino Acids, 27, 199–205.
Kwon do, Y., Jung, Y.S., Kim, S.J., Park, H.K., Park, J.H. and Kim, Y.C. (2009) Impaired sulfur-amino acid metabolism and oxidative stress in nonalcoholic fatty liver are alleviated by betaine supplementation in rats. J. Nutr., 139, 63–68.
Lakshman, R., Cederbaum, A.I., Hoek, J.B., Konishi, M., Koop, D. and Donohu, T.M. (2005) Use of CYP2E1-trans-fected human liver cell lines in elucidating the actions of ethanol. Alcohol. Clin. Exp. Res., 29, 1726–1734.
Kathirvel, E., Morgan, K., Nandgiri, G., Sandoval, B.C., Caudill, M.A., Bottiglieri, T., French, S.W. and Morgan, T.R. (2010) Betaine improves nonalcoholic fatty liver and associated hepatic insulin resistance: a potential mechanism for hepatoprotection by betaine. Am. J. Physiol. Gastrointest. Liver Physiol., 299, G1068-G1077.
Song, Z., Deaciuc, I., Zhou, Z., Song, M., Chen, T., Hill, D. and McClain, C.J. (2007) Involvement of AMP-activated protein kinase in beneficial effects of betaine on high-sucrose diet-induced hepatic steatosis. Am. J. Physiol. Gastrointest. Liver Physiol., 293, G894-G902.
Folch, J., Lees, M. and Sloane Stanley, G.H. (1957) A simple method for the isolation and purification of total lipides from animal tissues. J. Biol. Chem., 226, 497–509.
Aebi, H. (1984) Catalase in vitro. Methods Enzymol., 105, 121–126.
Griffith, O.W. (1980) Determination of glutathione and glutathione disulfide using glutathione reductase and 2-vinylpyri-dine. Anal. Biochem., 106, 207–212.
Ohkawa, H., Ohish, N. and Yagi, K. (1979) Assay for lipid peroxidation in animal tissues by thiobarbituric acid reaction. Anal. Biochem., 95, 351–358.
Zhang, P., McGrath, B., Li, S., Frank, A., Zambito, F., Reinert, J., Gannon, M., Ma, K., McNaughton, K. and Cavener, D.R. (2002) The PERK eukaryotic initiation factor 2 alpha kinase is required for the development of the skeletal system, postnatal growth, and the function and viability of the pancreas. Mol. Cell. Biol., 22, 3864–3874.
Liang, H. and Ward, W.F. (2006) PGC-1alpha: a key regulator of energy metabolism. Adv. Physiol. Educ., 30, 145–151.
Duval, C., Müller, M. and Kersten, S. (2007) PPARalpha and dyslipidemia. Biochim. Biophys. Acta, 1771, 961–971.
Satapati, S., He, T., Inagaki, T., Potthoff, M., Merritt, M.E., Esser, V., Mangelsdorf, D.J., Kliewer, S.A., Browning, J.D. and Burgess, S.C. (2008) Partial resistance to peroxisome pro-liferator-activated receptor-α agonists in ZDF rats is associated with defective hepatic mitochondrial metabolism. Diabetes, 57, 2012–2021.
Benhamed, F., Denechaud, P.D., Lemoine, M., Robichon, C., Moldes, M., Bertrand- Michel, J., Ratziu, V., Serfaty, L., Housset, C., Capeau, J., Girard, J., Guillou, H. and Postic, C. (2012) The lipogenic transcription factor ChREBP dissociates hepatic steatosis from insulin resistance in mice and humans. J. Clin. Invest., 122, 2176–2194.
Lee, J.Y., Cho, H.K. and Kwon, Y.H. (2010) Palmitate induces insulin resistance without significant intracellular triglyceride accumulation in HepG2 cells. Metab., 59, 927–934.
Yoon, J.C., Puigserver, P., Chen, G., Donovan, J., Wu, Z., Rhee, J., Adelmant, G., Stafford, J., Kahn, C.R., Granner, D.K., Newgard, C.B. and Spiegelman, B.M. (2001) Control of hepatic gluconeogenesis through the transcriptional coactivator PGC-1. Nat., 413, 131–138.
Craig, S.A. (2004) Betaine in human nutrition. Am. J. Clin. Nutr., 80, 539–549.
Natalello, A., Liu, J., Ami, D., Doglia, S.M. and de Marco, A. (2009) The osmolyte betaine promotes protein misfolding and disruption of protein aggregates. Proteins, 75, 509–517.
Guo, Z., Jiang, H., Xu, X., Duan, W. and Mattson, M.P. (2008) Leptin-mediated cell survival signaling in hippocampal neurons mediated by JAK STAT3 and mitochondrial stabilization. J. Biol. Chem., 283, 1754–1763.
Kim, B., Backus, C., Oh, S., Hayes, J.M. and Feldman, E.L. (2009) Increased tau phosphorylation and cleavage in mouse models of type 1 and type 2 diabetes. Endocrinol., 150, 5294–5301.
Clodfelder-Miller, B.J., Zmijewska, A.A., Johnson, G.V. and Jope, R.S. (2006) Tau is hyperphosphorylated at multiple sites in mouse brain in vivo after streptozotocin-induced insulin deficiency. Diabetes, 55, 3320–3325.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This is an Open-Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (https://doi.org/creativecommons.org/licenses/by/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Jung, Gy., Won, SB., Kim, J. et al. Betaine Alleviates Hypertriglycemia and Tau Hyperphosphorylation in db/db Mice. Toxicol Res. 29, 7–14 (2013). https://doi.org/10.5487/TR.2013.29.1.007
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.5487/TR.2013.29.1.007