Abstract
Background
The low contact stress rotating platform (LCS RP) knee (DePuy Orthopedics, Inc, Warsaw, Indiana), in use for last four decades in Western population, is reported to have a survival of more than 95% at 15 to 20 years. The reported Indian experience of this knee is limited to 5 years. Our aim was to report the clinical and radiological results of the LCS RP TKA design in the Indian population with a minimum followup of 10 years.
Materials and Methods
Fifty-five LCS knees (45 patients) operated between February 1997 and October 2001 were evaluated retrospectively. LCS design was generally selected if the patient was young (≤65 years of age), active and had no severe deformity. There were 40 female (88.9%) and 5 male (11.1%) patients; 47 knees had osteoarthritis (85.5%) and 8 knees had rheumatoid arthritis (14.5%). Knee Society Scores (KSS) and outcome questionnaire were filled at followup and radiographs were analyzed using Knee Society radiographic evaluation and scoring system.
Results
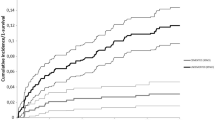
Of 45 patients (55 knees) enrolled, 37 patients (44 knees; 80%) were available for followup at 10 years. Average age was 59.6 years (range 40 to 77). Minimum followup was 10 years (average 12.3 years; range 10 to 15.3 years.). Three knees (6.8%) had been revised, one each for aseptic loosening, bearing dislocation and infection. Mean preoperative KSS of 33 improved to 91 postoperatively. Mean preoperative functional score of 45 improved to 76 postoperatively. Mean preoperative flexion of 113° (90°-140°) reduced to 102° (80°-135°) postoperatively. Erratic femoral rollback and tighter flexion gap to prevent spin out are the probable factors for decreased postoperative range of motion. Five (12%) patients could sit cross-legged and sit on the floor. Anterior knee pain was present in 4.6% (2/44 knees). The survival was 93.2% at 12.3 years. One patient (1.8%) had spin-out of the rotating bearing. No knee had osteolysis or progressive radiolucent lines on X-rays.
Conclusion
LCS implant has given good survival (93.2% at 12.3 years) with low rates of spin-out and anterior knee pain and no incidence of osteolysis. Limited flexion post surgery (104°) with only 12% managing to sit cross legged on the floor is a drawback.
Similar content being viewed by others
References
Bert JM. Dislocation/Subluxation of meniscal bearing elements after New-Jersey low-contact stress total knee arthroplasty. Clin Orthop Relat Res 1990;254:211–5.
Bragdon CR, O’Connor DO, Lowenstein JD, Jasty M, Biggs SA, Harris WH. A new pin-on-disk wear testing method for simulating wear of polyethylene on cobalt-chrome alloy in total hip arthroplasty. J Arthroplasty 2001;16:658–65.
Wang A. A unified theory of wear for ultra-high molecular weight polyethylene in multidirectional sliding. Wear 2001;248:38–47.
Pooley CM, Tabor D. Friction and molecular structure: The behaviour of some thermoplastics. Proc R Soc London 1972;329:251–74.
Jasty M, Goetz DD, Bragdon CR, Lee KR, Hanson AE, Elderf JR, et al. Wear of polyethylene acetabular components in total hip arthroplasty: An analysis of one hundred and twenty eight components retrieved at autopsy or revision operations. J Bone Joint Surg Am 1997;79:349–58.
Conditt MA, Stein JA, Noble PC. Factors affecting the severity of backside wear of modular tibial inserts. J Bone Joint Surg Am 2004;86:305–11.
Engh GA, Lounici S, Rao AR, Collier MB. In vivo deterioration of tibial baseplate locking mechanisms in contemporary modular total knee components. J Bone Joint Surg Am 2001;83:1660–5.
Parks NL, Engh GA, Topoleski LD, Emperado J. Modular tibial insert micromotion-a concern with contemporary implants. Clin Orthop Relat Res 1998;356:10–5.
Wasielewski RC, Parks N, Williams I, Surprenant H, Collier JP, Engh G. Tibial insert undersurface as a contributing source of polyethylene wear debris. Clin Orthop Relat Res 1997;345:53–9.
Kastner N, Gruber G, Aigner BA, Friesenbichler J, Pechmann M, Fürst F, et al. Sex-related outcome differences after implantation of low-contact-stress mobile-bearing total knee arthroplasty. Int Orthop 2012;36:1393–7.
Sadoghi P, Leithner A, Weber P, Friesenbichler J, Gruber G, Kastner N, et al. Radiolucent lines in low-contact-stress mobile-bearing total knee arthroplasty: A blinded and matched case control study. BMC Musculoskelet Disord 2011;12:142.
Callaghan JJ, O’Rourke MR, Iossi MF, Liu SS, Goetz DD, Vittetoe DA, et al. Cemented rotating-platform total knee replacementa concise followup, at a minimum of fifteen years, of a previous report. J Bone Joint Surg Am 2005;87:1995–8.
Buechel FF Sr, Buechel FF Jr, Pappas MJ, D’Alessio J. Twenty-year evaluation of meniscal bearing and rotating platform knee replacements. Clin Orthop Relat Res 2001;388:41–50.
Dixon MC, Brown RR, Parsch D, Scott RD. Modular fixed-bearing total knee arthroplasty with retention of the posterior cruciate ligament: A study of patients followed for a minimum of fifteen years. J Bone Joint Surg Am 2005;87:589–603.
Brassard MF, Insall JN, Scuderi GR, Colizza W. Does modularity affect clinical success? A comparison with a minimum 10 year followup. Clin Orthop 2001:388:26–32.
Laskin RS. The genesis total knee prosthesis: A 10 year followup study. Clin Orthop Relat Res 2001:388:95–102.
Maini PS, Kailey PV, Talwar N. Hybrid fixation in rotating platform mobile bearing total knee arthroplasty using low contact stress knee. Indian J Orthop 2006;40:219–23.
Bhan S, Malhotra R. Results of rotating-platform, low-contact-stress knee prosthesis. J Arthroplasty 2003:18: 1016–22.
Buechel FF Sr. Long term followup after mobile-bearing total knee replacement. Clin Orthop Relat Res 2002;404:40–50.
Sorrells RB, Stiehl JB, Voorhorst PE. Midterm results of mobile-bearing total knee arthroplasty in patients younger than 65 years. Clin Orthop Relat Res 2001;390:182–9.
Kim YH, Kim JS, Choi Y. Osteolysis after unidirectional and multidirectional mobile bearing total knee arthroplasty in young patients. J Arthroplasty 2009:24:586–93.
Duffy GP, Crowder AR, Trousdale RR, Berry DJ. Cemented total knee arthroplasty using a modern prosthesis in young patients with osteoarthritis. J Arthroplasty 2007:22:67–70.
Callaghan JJ, Squire MW, Goetz DD, Sullivan PM, Johnston RC. Cemented rotating-platform total knee replacement a nine to twelve year followup study. J Bone Joint Surg Am 2000;82:705–10.
Dennis DA, Komistek RD, Mahfouz MR, Haas BD, Stiehl JB. Multicentre determination of in vivo kinematics after total knee arthroplasty. Clin Orthop Relat Res 2003;416:37–57.
Haas BD, Komistek RD, Stiehl JB, Anderson DT, Northcut EJ. Kinematic comparison of posterior cruciate sacrifice versus substitution in a mobile bearing total knee arthroplasty. J Arthroplasty 2002;17:685–92.
Maniar R. Rationale for the posterior-stabilized rotating-platform knee. Orthopedics 2006;29:S23–7.
Meftah M, Ranawat AS, Ranawat CS. Ten-year followup of a rotating-platform, posterior-stabilized total knee arthroplasty. J Bone Joint Surg Am 2012;94:426–32.
Maniar RN, Gupta H, Singh A, Johorey AC, Singhi T. Five- to eight-year results of a prospective study in 118 arthroplasties using posterior-stabilized rotating-platform knee implants. J Arthroplasty 2011;26:543–8.
Maniar RN, Singhi T. High-flex rotating platform knee implants two- to 6-year results of a prospective study. J Arthroplasty 2012;27:598–603.
Meftah M, Ranawat AS, Ranawat CS. Safety and efficacy of a rotating-platform, high-flexion knee design three- to five-year followup. J Arthroplasty 2012;27:201–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maniar, R.N., Singhi, T., Gangaraju, B. et al. Mid term results of LCS knee: The Indian experience. IJOO 47, 57–62 (2013). https://doi.org/10.4103/0019-5413.106903
Published:
Issue Date:
DOI: https://doi.org/10.4103/0019-5413.106903