Abstract
Introduction
The aim of our study is to evaluate the feasibility, safety and efficacy of the percutaneous closure of PFO (abnormal communication between the right and left atrium).
Methods
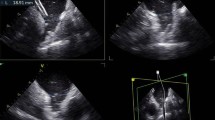
Between July 2009 and October 2012 percutaneous closure was performed in 37 patients. The presence of PFO was diagnosed through the use of ultrasound techniques: transcranial doppler with contrast (cTCD), transthoracic echocardiography(TTE) and transesophageal echocardiography (TEE). Follow-up was composed consisted of a Holter ECG 7 days after the closure with a 24 hour heart rhythm monitoring, to evaluate eventual arrhythmia cases and programmed controls which included a TTE at 1–3 months, TTE+ cTCD at 6–12 months, to evaluate the right positioning of the device and the complete closure of the defect.
Results
We obtained 100% of procedural success (correct and stable implantation of the device in a perfect position on the interatrial septum).No complications were recorded during the procedure and no new onset atrial fibrillation was detected in any patients after the PFO closure. The follow up with cTCD and TEE reported a closing rate of 86.7%. No new clinical cerebrovascular events occurred in treated patients until now.
Conclusion
Our experience describes the percutaneous PFO procedure as feasible, safe and effective with a high rate of procedural success, with an absence of significant adverse events and a high rate of complete closure.
Similar content being viewed by others
References
Schrader R. Indication and techniques of transcatheter closure of patent foramen ovale. J Interven Cardiol. 2003; 16:543–551
Homma S, Di Tullio MR, Patent foramen ovale and stroke. J Cardiol. 2010; 56:134–141
Overell JR, Bone I, and Lees KR, Interatrial septal abnormalities and stroke: A meta-analysis of casecontrol studies. Neurology. 2000; 55:1172–1179
Fazio G, Ferro G, Barbaro G, Ferrara F, Novo G, Novo S. Patent foramen ovale and thromboembolic complications. Curr Pharm Des. 2010; 16:3497–3502
Billinger M, Zbinden R, Mordasini R et al. Patent foramen ovale closure in recreational divers: effect on decompression illness and ischaemic brain lesions during long-term follow-up. Heart. 2011; 97:1932–1937
Reul J, Weis J, Jung A, Willmes K, Thron A. Central nervous system lesions and cervical disc herniations in amateur divers. Lancet. 1995; 345:1403–1405
Knauth M, Ries S, Pohimann S, et al. Cohort study of multiple brain lesions in sport divers: role of a patent foramen ovale. British medical journal. 1997; 314: 701–705
Wilmshurst P, FRCP; Nightingale S, FRCP, The Role of Cardiac and Pulmonary Pathology in Migraine: A Hypothesis. Headache. 2006; 46:429–434
Cabanes, L. et al. Atrial septal aneurysm and patent foramen ovale as risk factors for cryptogenic ictus in patients less than 55 years of age. A study using transesophageal echocardiography. Stroke. 1993; 24:1865–1873
Lechat, P. et al. Prevalence of patent foramen ovale in patients with ictus. N. Engl. J. Med. 1998; 318: 1148–1152
Webster, M. W. et al. Patent foramen ovale in young ictus patients. Lancet. 1988; 2:11–12
Job FP, Ringelstein EB, Grafen Y. Comparison of transcranial contrast Doppler sonography and transesophageal contrast echocardiography for the detection of patent foramen ovale in young ictus patients. Am. J. Cardiol. 1994; 74:381–384
Di Tullio M, Sacco RL, Gopal A, Mohr JP, Homma S. Patent foramen ovale as a risk factor for cryptogenic ictus. Ann. Intern. Med. 1992; 117:461–465
Yeung M, Khan KA, Shuaib A. Transcranial Doppler ultrasonography in the detection of venous to arterial shunting in acute ictus and transient ischaemic attacks. J. Neurol. Neurosurg. Psychiatry. 1996; 61:445–449
Handke M, Harloff A, Olschewski M, Hetzel A. Geibel A. Patent foramen ovale and cryptogenic ictus in older patients. N. Engl. J. Med. 2007; 357:2262–2268
Windecker S, Meier B. Is closure recommended for patent foramen ovale and cryptogenic stroke? Patent foramen ovale and cryptogenic stroke: to close or not to close? Closure: what else! Circulation. 2008; 118:1989–1998
Messé SR, Kasner SE. Is closure recommended for patent foramen ovale and cryptogenic stroke? Patent foramen ovale in cryptogenic stroke: not to close. Circulation. 2008;118: 1999–2004
Sacco RL, Adams R, Albers G, et al. Guidelines for prevention of stroke in patients with ischemic stroke or transient ischemic attack: a statement for healthcare professionals from the American Heart Association/American Stroke Association Council on Stroke: co-sponsored by the Council on Cardiovascular Radiology and Intervention: the American Academy of Neurology affirms the value of this guideline. Stroke. 2006; 37:577–617
O’Gara PT, Messe SR, Tuzcu EM, Catha G, Ring JC. A Call for Completion of Randomized Clinical Trials A Science Percutaneous Device Closure of Patent Foramen Ovale for Secondary Stroke. AHA/ASA/Am. Coll. Circulation. 2009; 119:2743–2747
Heinisch C, Bertog S, Wunderlich N et al. Percutaneous closure of the patent foramen ovale using the HELEX® Septal Occluder: acute and long-term results in 405 patients. EuroIntervention. 2012; 8:717–723
Khairy P, O’Donnell CP, Landzberg MJ. Transcatheter closure versus medical therapy of patent foramen ovale and presumed paradoxical thromboemboli: a systematic review. Ann Intern Med. 2003; 139:753–760
Windecker S, Wahl A, Nedeltchev K, Arnold M et al. Comparison of medical treatment with percutaneous closure of patent foramen ovale in patients with cryptogenic ictus. J Am Coll Cardiol. 2004; 44:750–758
Windecker, S. et al. Comparison of medical treatment with percutaneous closure of patent foramen ovale in patients with cryptogenic stroke. J. Am. Coll. Cardiol. 2004; 44:750–758
Furlan, A J et al. Study design of the CLOSURE I trial. A prospective, multicenter, randomized, controlled trial to evaluate the safety and efficacy of the Starflex septal closure system versus best medical therapy in patients with stroke or transient ischemic attack due to presumed paradoxical embolism through a patent foramen ovale. Stroke. 2010; 41:2872–2883
Patrick A. Calvert, Bushra S. Rana, Anna C. Kydd & Leonard M. Shapiro. Patent foramen ovale: anatomy, outcomes, and closure. Nat Rev Cardiol. 2011; 8:148–160
Mas JL, Arquizan C, Lamy C, Zuber M, Cabanes L, Derumeaux G et al. Recurrent cerebrovascular events associated with patent foramen ovale, atrial septal aneurysm, or both. NEngl J Med. 2001; 345:1740–1746
Fazio G, Ferro G, Carità P, Lunetta M, Gullotti A, Trapani R, Fabbiano A, Novo G, Novo S. The PFO anatomy evaluation as possible tool to stratify the associated risks and the benefits arising from the closure. European Journal of Echocardiography. 2010; 11:488–491
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Evola, S., Trovato, R.L., Kauroo, B.A.W. et al. The percutaneous treatment of Patent Foramen Ovale, an effective and safe therapeutic choice. cent.eur.j.med 8, 638–643 (2013). https://doi.org/10.2478/s11536-013-0209-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.2478/s11536-013-0209-y