Abstract
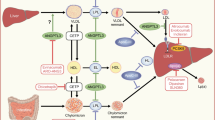
The principal function of high-density lipoprotein (HDL) is to facilitate the reverse cholesterol transport (RCT) and inhibition of atheroma formation. Epidemiological studies and interventional trials have suggested that HDL has cardioprotective properties. However, increasing HDL concentration may not necessarily increase RCT, especially if the increase in HDL levels is the result of inhibiting HDL cholesterol (HDL-C) flux. The results of recent phase III clinical trials utilizing a cholesterol ester transfer protein (CETP) inhibitor to increase HDL-C levels in hypoalphalipoproteinaemia have shown that this approach of elevating HDL-C levels is insufficient to combat atherosclerosis and reduce the risk of cardiovascular disease. Although there are several interventions that increase HDL-C by preventing its turnover in the circulation, a more desirable approach is to enhance de novo production of HDL in the liver and/or small intestine. To this end, our acquired knowledge of the apolipoprotein-I (apo A-I) gene promoter as well as the signalling pathways that modulate its expression, has fuelled the development of novel therapeutic strategies to increase HDL-C flux. Promising pharmacological agents that selectively regulate transcription of the apo A-I gene, therapeutic strategies to de-repress apo A-I gene expression, and infusion of recombinant apo A-I or apo A-I mimetics are under development and may be clinically beneficial in the near future.




Similar content being viewed by others
References
Franceschini G, Maderna P, Sirtori CR. Reverse cholesterol transport: physiology and pharmacology. Atheroscler 1991; 88: 99–107
Johnson WJ, Mahlberg FH, Rothblat GH, et al. Cholesterol transport between cells and high-density lipoproteins. Biochim Biophys Acta 1991; 1085: 273–98
Sviridov D, Nestel P. Dynamics of reverse cholesterol transport: protection against atherosclerosis. Atheroscler 2002; 161: 245–54
Brewer Jr HB, Santamarina-Fojo S. New insights into the role of the adenosine triphosphate-binding cassette transporters in high-density metabolism and reverse cholesterol transport. Am J Cardiol 2003; 91: 3E-11E
Santamarina-Fojo S, Gonzalez-Navarro H, Greeman L, et al. Hepatic lipase, lipoprotein metabolism, and atherogenesis. Arterioscler Thromb Vasc Biol 2003; 24: 1750–4
Eggerman TL, Hoeg JM, Meng MS, et al. Differential tissue-specific expression of human apoA-I and apoA-II. J Lipid Res 1991; 32: 821–8
Rye KA, Barter PJ. Formation and metabolism of pre-beta-migrating, lipid-poor apolipoprotein A-I. Arterioscler Thromb Vasc Biol 2004; 24: 421–8
Mulya A, Lee JY, Gebre AK, et al. Minimal lipidation of pre-beta HDL by ABCA1 results in reduced ability to interact with ABCA1. Arterioscler Thromb Vasc Biol 2007; 27: 1838–46
Duong PT, Weibel GL, Lund-Katz S, et al. Characterization and properties of pre-beta-HDL particles formed by ABCA1-mediated cellular lipid efflux to apoA-I. J Lipid Res 2008; 49: 1006–14
Favari E, Calabresi L, Adorni MP, et al. Small discoidal pre-b1 HDL particles are efficient acceptors of cell cholesterol via ABCA1 and ABCG1. Biochem 2009; 48: 11067–74
Asztalos BF, Schaefer EJ, Horvath KV, et al. Role of LCAT in HDL remodeling: investigation of LCAT deficiency states. J Lipid Res 2007; 48: 592–9
Tall AR. Plasma lipid transfer proteins. J Lipid Res 1986; 27: 361–7
von Eckardstein A, Huang Y, Assmann G. Physiological role and clinical relevance of high-density lipoprotein subclasses. Curr Opin Lipidol 1994; 5: 404–16
Asztalos BF, de la Llera-Moya M, Dallal GE, et al. Differential effects of HDL subpopulations on cellular ABCA1 and SR-B1-mediated cholesterol efflux. J Lipid Res 2005; 46: 2246–53
Zhang XK, Lehmann J, Hoffmann B, et al. Homodimer formation of retinoid X receptor induced by 9-cis-retinoic acid. Nature 1992; 358: 587–91
Vu-Dac N, Chopin-Delannoy S, Gervois P, et al. The nuclear receptors peroxisome proliferator-activated receptor a and Rev-erbα mediate the species-specific regulation of apolipoprotein A-I expression by fibrates. J Biol Chem 1998; 273: 25713–20
Huuskonen J, Vishnu M, Chau P, et al. Liver X receptor inhibits the synthesis and secretion of apolipoprotein AI by human liver-derived cells. Biochem 2006; 45: 15068–74
Shaw JA, Bobik A, Murphey A, et al. Infusion of reconstituted high-density lipoprotein leads to acute changes in human atherosclerotic plaque. Circul Res 2008; 103: 1084–91
Navab M, Schechter I, Anantharamaiah GM, et al. Structure and function of HDL mimetics. Arterioscler Thromb Vasc Biol 2010; 30: 164–8
Lebherz C, Sanmiguel J, Wilson JM, et al. Gene transfer of wild-type apoA-I and apoA-I Milano reduce atherosclerosis to a similar extent. Cardiovasc Diabetol 2007; 6: 15–22
Vu-Dac N, Schoonjans K, Laine B, et al. Negative regulation of the human apolipoprotein A-I promoter by fibrates can be attenuated by the interaction of the peroxisome proliferator-activated receptor with its response element. J Biol Chem 1994; 269: 31012–8
Magee G, Sharpe PC. Paradoxical decreases in high-density lipoprotein cholesterol with fenofibrate: a quite common phenomenon. J Clin Pathol 2009; 62: 250–3
Staels B, Dallongeville J, Auwerx J, et al. Mechanisms of action of fibrates on lipid and lipoprotein metabolism. Circul 1998; 98: 2088–93
Pineda Torra I, Gervois P, Staels B. Peroxisome proliferator-activated receptor alpha in metabolic disease, inflammation, atherosclerosis, and aging. Curr Opin Lipidol 1999; 10: 151–9
Xu Y, Mayhugh D, Saeed A, et al. Design and synthesis of a potent and selective triazolone-based peroxisome proliferator-activated receptor a agonist. J Med Chem 2003; 46: 5121–4
Nissen SE, Nicholls SJ, Wolski K, et al. Effects of a potent and selective PPAR-α agonist in patients with atherogenic dyslipidemia or hypercholesterolemia: two randomized controlled trials. JAMA 2007; 297: 1362–73
Millar JS, Duffy D, Gadi R, et al. Potent and selective PPAR-α agonist LY518674 upregulates both apoA-I production and catabolism in human subjects with the metabolic syndrome. Arterioscler Thromb Vasc Biol 2009; 29: 140–6
Sierra ML, Beneton V, Boullay AB, et al. Substituted 2-[(4-aminomethyl)phenoxy-2-methylprotionic acid PPARd agonists, 1: discovery of a novel series of potent HDLc raising agents. J Med Chem 2007; 50: 685–95
Sakamoto J, Kimura H, Moriyama S, et al. Activation of human peroxisome proliferator-activated receptor (PPAR) subtypes by pioglitazone. Biochem Biophys Res Comm 2000; 278: 704–11
Qin S, Liu T, Kamanna VS, et al. Pioglitazone stimulates apolipoprotein A-I production without affecting HDL removal in HepG2 cells: involvement of PPAR-α. Arterioscler Thromb Vasc Biol 2007; 27: 2428–34
Lehmann JM, Moore LB, Smith-Oliver TA, et al. An anti-diabetic thiazolidinedione is a high affinity ligand for peroxisome proliferator-activated receptor γ (PPARg). J Biol Chem 1995; 270: 12953–6
Willson TM, Cobb JE, Cowan DJ, et al. The structure-activity relationship between peroxisome proliferator-activated receptor γ agonism and the antihyperglycemic activity of thiazolidinediones. J Med Chem 1996; 3: 665–8
Matthews L, Berry A, Tersigni M, et al. Thiazolidinediones are partial agonists for the glucocorticoid receptor. Endocrinol 2009; 150: 75–86
Wang YX, Lee CH, Tsiep S, et al. Peroxisome-proliferator-activated receptor delta activates fat metabolism to prevent obesity. Cell 2003; 113: 159–70
Oliver Jr WR, Shenk JL, Snaith MR, et al. A selective peroxisome proliferator-activated receptor delta agonist promotes reverse cholesterol transport. Proc Natl Acad Sci U S A 2001;98: 5306–11
Liebowitz MD, Fievet C, Hennuyer N, et al. Activation of PPARdelta alters lipid metabolism in db/db mice. FEBS Lett 2000; 473: 333–6
van der Hoorn JW, Jukema JW, Havekes LM, et al. The dual PPARalpha/gamma agonist tesaglitazar blocks progression of pre-existing atherosclerosis in APOE*3Leiden: CETP transgenic mice. Br J Pharmacol 2009; 156: 1067–75
Saad MF, Greco S, Osei K, et al. Ragaglitazar improves glycemic control and lipid profile in type 2 diabetic subjects: a 12-week, double-blind, placebo-controlled dose-ranging study with an open pioglitazone arm. Diabetes Care 2004; 27: 1324–9
Goldstein BJ, Rosenstock J, Anzalone D, et al. Effect of tesaglitazar, a dual PPARa/g agonist, on glucose and lipid abnormalities in patients with type 2 diabetes: a 12-week dose-ranging trial. Curr Med Res Opin 2006; 22: 2575–90
Oleksiewicz MB, Southgate J, Iversen L, et al. Rat urinary bladder carcinogenesis by dual-acting PPARalpha + gamma agonists. PPAR Res 2008; 2008: 103167
Lovas K, Rost TH, Skorve J, et al. Tetradecylthioacetic acid attenuates dyslipidemia in mal patients with type 2 diabetes mellitus, possibly by dual PPAR-a/d activation and increased mitochondrial fatty acid oxidation. Diabetes Obes Metab 2008; 11: 304–14
Grav HJ, Tronstad KJ, Gudbrandsen OA, et al. Changed energy state and increased mitochondrial beta-oxidation rate in liver or rats associated with lowered proton electrochemical potential and stimulated uncoupling protein 2 (UCP-2) expression: evidence for peroxisome proliferator-activated receptor-alpha independent induction of UCP-2 expression. J Biol Chem 2003; 278: 30525–33
Shen L, Zhang Y, Wang A, et al. Synthesis and identification of [1,2,4]thiadiazole derivatives as a new series of potent and orally active dual agonists of peroxisome proliferator-activated receptors a and d. J Med Chem 2007; 50: 3954–63
Shen L, Zhang Y, Wang A, et al. Synthesis and structure-activity relationships of thiadiazole-derivatives as potent and orally active peroxisome proliferator-activated receptors a/d dual agonists. Bioorganic Med Chem 2008; 16: 3321–41
Goldenberg I, Benderly M, Goldbourt U, et al. Secondary prevention with bezafibrate therapy for the treatment of dyslipidemia: an extended follow-up of the BIP trial. J Am Coll Cardiol 2008; 51: 459–65
Goldenberg I, Boyko V, Tennenbaum A, et al. Long-term benefit of high-density lipoprotein cholesterol-raising therapy with bezafibrate. Arch Intern Med 2009; 169: 508–14
Nakajima T, Tanaka N, Kanbe H, et al. Bezafibrate at clinically relevant doses decreases serum/liver triglycerides via down-regulation of a sterol regulatory element-binding protein-1c in mice: a novel peroxisome proliferator-activated receptor alpha-independent mechanism. Mol Pharmacol 2009; 75: 782–92
Schmitz G, Langmann T. Transcriptional regulatory networks in lipid metabolism control ABCA1 expression. Biochim Biophys Acta 2005; 1735: 1–19
Pinaire JA, Reifel-Miller A. Therapeutic potential of retinoid X receptor modulators for the treatment of the metabolic syndrome. PPAR Res 2007; 2007: 94156
Leibowitz MD, Ardecky RJ, Boehm MF, et al. Biological characterization of a heterodimer-selective retinoid X receptor modulator: potential benefits for the treatment of type 2 diabetes. Endocrinol 2006; 147: 1044–53
Bramlett KS, Houck KA, Borchert KM, et al. A natural product ligand of the oxysterol receptor, liver X receptor. J Pharm Exp Therap 2003; 307: 291–6
Venkateswaran A, Laffitte BA, Joseph SB, et al. Control of cellular cholesterol efflux by the nuclear oxysterol receptor LXR alpha. Proc Natl Acad Sci U S A 2000; 97: 12097–102
Taylor AH, Raymond J, Dionne JM, et al. Glucocorticoid increases rat apolipoprotein A-I promoter activity. J Lipid Res 1996; 37: 2232–43
De Bosscher K, Haegeman G. Latest perspectives on anti-inflammatory actions of glucocorticoids. Mol Endocrinol 2009; 23: 281–91
Kassel O, Sancono A, Kratzschmar J, et al. Glucocorticoids inhibit MAP kinase via increased expression and decreased degradation of MKP-1. EMBO J 2001; 20: 7108–16
Beers A, Haas MJ, Wong NCW, et al. Inhibition of apolipoprotein AI gene expression by tumor necrosis factor: roles for MEK/ERK and JNK signaling. Biochem 2006; 34: 2408–13
De Bosscher K, Vanden Berghe W, Haegeman G. The interplay between the glucocorticoid receptor and nuclear factor kB or activator protein-1: molecular mechanisms for gene repression. Endocr Rev 2003; 24: 488–522
Morishima A, Ohkubo N, Maeda N, et al. NFkB regulates plasma apolipoprotein A-I and high density lipoprotein cholesterol through inhibition of peroxisome proliferator-activated receptor a. J Biol Chem 2003; 278: 38188–93
Clark AR. Anti-inflammatory functions of glucocorticoid-induced genes. Mol Cell Endocrinol 2007; 275: 79–97
Dewint P, Gossye V, De Bosscher K, et al. A plant-derived ligand favoring monomeric glucocorticoid receptor conformation with impaired transactivation potential attenuates collagen-induced arthritis. J Immunol 2008; 180: 2608–15
O’Brien T, Katz K, Hodge D, et al. The effect of treatment of hypothyroidism and hyperthyroidism on plasma lipids and apolipoproteins AI, AII and E. Clin Endocrinol 1997; 46: 17–20
Romney JS, Chen J, Carr FE, et al. Identification of the thyroid hormone responsive messenger RNA spot11 as apolipoprotein A1 messenger RNA and effects of the hormone on the promoter. Mol Endocrinol 1992; 6: 943–50
Taylor AH, Wishart P, Lawless DE, et al. Identification of functional positive and negative thyroid hormone-responsive elements in the rat apolipoprotein AI promoter. Biochem 1996; 35: 8281–8
O’Shea PJ, Williams GR. Insight into the physiological actions of thyroid hormone receptors from genetically modified mice. J Endocrinol 2002; 175: 553–70
Grover GJ, Mellstrom K, Malm J. Therapeutic potential for thyroid hormone receptor-beta selective agonists for treating obesity, hyperlipidemia, and diabetes. Curr Vasc Pharmacol 2007; 5: 141–54
Murao K, Wada Y, Nakamura T, et al. Insulin and glucose regulation of apolipoprotein AI gene expression. J Biol Chem 1998; 273: 18959–65
Lam JK, Matsubara S, Mihara K, et al. Insulin induction of apolipoprotein AI: role of Sp1. Biochem 2003; 42: 2680–90
Zheng X-L, Matsubara S, Diao C, et al. Epidermal growth factor induction of apolipoprotein A-I is mediated by the Ras-MAP kinase cascade and Sp1. J Biol Chem 2001; 276: 13822–9
Zheng X-L, Matsubara S, Diao C, et al. Activation of apolipoprotein AI gene expression by protein kinase A and kinase C through transcription factor, Sp1. J Biol Chem 2000; 275: 31747–54
Wehmeier K, Beers A, Haas MJ, et al. Inhibition of apolipoprotein AI gene expression by 1,25-dihydroxyvitamin D3. Biochem Biophys Acta 2005; 1737: 16–26
Nijenhuis T, van der Eerden BCJ, Zugel U, et al. The novel vitamin D analog ZK191784 as an intestine-specific vitamin D antagonist. FASEB J 2006; 20: 2171–73
Wang J-H, Keisala T, Solakivi T, et al. Serum cholesterol and expression of apoAI, LXRβ, and SREBP2 in vitamin D receptor knock-out mice. J Steroid Biochem Mol Biol 2009; 113: 222–6
Wehmeier KR, Mazza A, Hachem S, et al. Differential regulation of apolipoprotein A-I gene expression by vitamin D receptor modulators. Biochim Biophys Acta 2008; 1780: 264–73
Colston K, MacKay AG, James SY, et al. EB 1089: a new vitamin D analogue that inhibits the growth of breast cancer cells in vivo and in vitro. Biochem Pharmacol 1992; 44: 2273–80
Masson D, Lagrost L, Athias A, et al. Expression of the pregnane X receptor in mice antagonizes the cholic acid-mediated changes in plasma lipoprotein profile. Arterioscler Thromb Vasc Biol 2005; 25: 2164–9
Masson D, Qatanani M, Sberna AL, et al. Activation of the constitutive androstane receptor decreases HDL in wild-type and human apoA-I transgenic mice. J Lipid Res 2008; 49: 1682–91
Zhou C, King N, Chen KY, et al. Activation of pregnane X receptor induces hypercholesterolemia in wild-type and accelerates atherosclerosis in apolipoprotein E deficient mice. J Lipid Res 2009; 50: 2004–13
Harnish DC, Malik S, Kilbourne E, et al. Control of apolipoprotein AI gene expression through synergistic interactions between hepatocyte nuclear factors 3 and 4. J Biol Chem 1996; 271: 13621–8
Delerive P, Galardi CM, Bisi JE, et al. Identification of liver receptor homolog-1 as a novel regulator of apolipoprotein AI gene transcription. Mol Endocrinol 2004; 18: 2378–87
Digby JE, Lee JM, Choudhury RP. Nicotinic acid and the prevention of coronary artery disease. Curr Opin Lipidol 2009; 20: 321–6
Lai E, De Lepeleire I, Crumley TM, et al. Suppression of niacin-induced vasodilation with an antagonist to prostaglandin D2 receptor subtype 1. Clin Pharm Ther 2007; 81: 849–57
van der Hoorn JWA, de Haan W, Berbee JFP, et al. Niacin increases HDL by reducing hepatic expression and plasma levels of cholesterol ester transfer protein in APOE*3 Leiden CETP mice. Arterioscler Thromb Vasc Biol 2008; 28: 2016–22
Soga T, Kamohara J, Matsumoto S, et al. Molecular identification of nicotinic acid receptor. Biochem Biophys Acta 2003; 28: 364–9
Gille A, Bodor ET, Ahmed K, et al. Nicotinic acid: pharmacological effects and mechanisms of action. Ann Rev Pharmacol Toxicol 2008; 48: 4.1-4.28
Aktories K, Jakobs KH, Schultz G. Nicotinic acid inhibits adipocyte adenylate cyclase in a hormone-like manner. FEBS Lett 1980; 115: 11–4
Taggart AK, Kero J, Gan X, et al. (D)-b-Hydroxybutyrate inhibits adipocytes lipolysis via the nicotinic acid receptor PUMA-G. J Biol Chem 2005; 280: 26649–52
Havel RJ. Conversion of plasma free fatty acids into triglycerides of plasma lipoprotein fractions in man. Metabol 1961; 10: 1031–4
Lamon-Fava LH, Diffenderfer MR, Barrett PHR, et al. Extended-release niacin alters the metabolism of plasma apolipoprotein (apo) A-I and apoB-containing lipoproteins. Arterioscler Thromb Vasc Biol 2008; 28: 1672–8
Siripurkpong P, Na-Bangchang K. Effects of niacin and chromium on the expression of ATP-biding cassette transporter A1 and apolipoprotein A-I genes in HepG2 cells. J Nutr Biochem 2009; 20: 261–8
Wu Z-H, Zhao S-P. Niacin promotes cholesterol efflux through stimulation of the PPARg-LXRa-ABCA1 pathway in 3T3-L1 adipocytes. Pharmacol 2009; 84: 282–7
Blumenthal RS. Overview of the adult treatment panel (ATP) III guidelines. Adv Stud Med 2002; 2: 148–57
Gardner CD, Tribble DL, Young DR, et al. Population frequency distributions of HDL, HDL2, and HDL3 cholesterol and apolipoproteins A-I and B in healthy men and women and associations with age, gender, hormonal status, and sex hormone use: the Stanford Five City Project. Prev Med 2000; 31: 335–45
Deroo BJ, Korach KS. Estrogen receptors and human disease. J Clin Invest 2006; 116: 561–70
Huxley VA. Sex and the cardiovascular system: the intriguing tale of how women and men regulate cardiovascular function differently. Adv Physiol Educ 2007; 31: 17–22
Klos KL, Boerwinkle E, Ferrell RE, et al. ESR1 Polymorphism is associated with plasma lipid and apolipoprotein levels in Caucasians of the Rochester Family Heart Study. J Lipid Res 2008; 49: 1701–6
Deleon MJ, Horani MH, Haas MJ, et al. Effects of dehydroepiandrosterone on rat apolipoprotein AI gene expression in the human hepatoma cell line, HepG2. Metabol 2002;51: 376–9
Taylor AH, Fox-Robichaud AH, Egan C, et al. Estradiol decreases apolipoprotein AI expression in adult male rats via site B. J Mol Endocrinol 2000; 25: 207–19
Harnish DC, Evans MJ, Scicchitano MS, et al. Estrogen regulation of the apolipoprotein AI gene promoter through transcription cofactor sharing. J Biol Chem 1998; 273: 9270–8
Sammartino A, Cirillo D, Mandato VD, et al. Osteoporosis and cardiovascular disease: benefit-risk of hormone replacement therapy. J Endocrinol Invest 2005; 28: 80–4
Rossouw JE. Implications of recent clinical trials of postmenopausal hormone therapy for management of cardiovascular disease. Ann N Y Acad Sci 2006; 1089: 444–53
Joensuu H, Holli K, Oksanen H, et al. Serum lipid levels during and after adjuvant toremifene or tamoxifen therapy for breast cancer. Breast Cancer Res Treat 2000; 63: 225–34
Mastroianni A, Bellati C, Facchetti G, et al. Increased plasma HDL-cholesterol and apo A-I in breast cancer patients undergoing adjuvant tamoxifen therapy. Clin Biochem 2000; 33: 513–6
Francucci CM, Daniel e P, Iori N, et al. Effects of raloxifene on body fat distribution and lipid profile in healthy post-menopausal women. Endocrinol Invest 2005; 28: 623–31
Tam S-P, Zhang X, Cuthbert C, et al. The effects of dimethyl sulfoxide on apolipoprotein A-I in the human hepatoma cell line, HepG2. J Lipid Res 1997; 38: 2090–102
Berrougui H, Grenier G, Loued S, et al. A new insight into resveratrol as an atheroprotective compound: inhibition of lipid peroxidation and enhancement of cholesterol efflux. Atheroscler 2009; 207: 420–7
Mooradian AD, Haas MJ, Wadud K. Ascorbic acid and alpha-tocopherol down-regulate apolipoprotein A-I gene expression I HepG2 and Caco-2 cell lines. Metabol 2006; 55: 159–67
Robinson I, de Serna DG, Gutierrez A, et al. Vitamin E in humans: an explanation of clinical trial failure. Endocrin Pract 2006; 12: 576–82
Moats C, Rimm EB. Vitamin intake and risk of coronary disease: observation versus intervention. Curr Atheroscler Rep 2007; 9: 508–14
Steinhubl SR. Why have antioxidants failed in clinical trials? Am J Cardiol 2008; 101: 14D-9D
Anderson JW, Johnstone BM, Cook-Newell ME. Meta-analysis of the effects of soy protein intake on serum lipids. N Engl J Med 1995; 333: 276–82
Anthony MS, Clarkson TB, Hughes CL, et al. Soybean isoflavones improve cardiovascular risk factors without affecting the reproductive system of peripubertal rhesus monkeys. J Nutr 1996; 126: 43–50
Hodgson JM, Puddey IB, Beilin LJ, et al. Supplementation with isoflavonoid phytoestrogens does not alter serum lipid concentrations: a randomized controlled trial in humans. J Nutr 1989; 128: 728–32
Lamon-Fava LH. Genistein activates apolipoprotein A-I gene expression in the human hepatoma cell line Hep G2. J Nutr 2000; 130: 2489–92
Lamon-Fava LH, Micherone D. Regulation of apoA-I gene expression: mechanism of action of estrogen and genistein. J Lipid Res 2004; 45: 106–12
Akiyama T, Ishida J, Nakagawa S. Genistein, a specific inhibitor of tyrosine-specific protein kinases. J Biol Chem 1987; 262: 5592–6
Urizar NL, Liverman AB, Dodds DT, et al. A natural product that lowers cholesterol as an antagonist ligand for FXR. Science 2002; 296: 1703–6
Claudel T, Sturm E, Duez H, et al. Bile acid-activated nuclear receptor FXR suppresses apolipoprotein A-I transcription via a negative FXR response element. J Clin Invest 2002; 109: 961–71
Sharma B, Salunke R, Srivastava S, et al. Effects of gug-gulsterone isolated from Commiphora mukul in high-fat diet induced diabetic rats. Food Chem Toxicol 2009; 47: 2631–9
Szapary PO, Wolfe ML, Bloedon LT, et al. Guggulipid for the treatment of hypercholesterolemia: a randomized controlled trial. JAMA 2003; 290: 765–72
Despres J-C, Golay A, Sjostrom L, et al. Effects of rimonabant on metabolic risk factors in overweight patients with dyslipidemia. N Engl J Med 2005; 353: 2121–34
Van Gaal LF, Rissanen AM, Scheen AJ, et al. Effects of the cannabinoid-1 receptor blocker rimonabant on weight reduction and cardiovascular risk factors in overweight patients: 1-year experience from the RIO-Europe study. Lancet 2005; 365: 1389–97
Pi-Sunyer XF, Aronne LJ, Heshmati HM, et al. Effect of rimonabant, a cannabinoid-1 receptor blocker, on weight and cardiometabolic risk factors in overweight or obese patients; RIO-North America: a randomized controlled trial. JAMA 2006; 295: 761–75
Scheen AJ, Finer N, Hollander P, et al. Efficacy and tolerability of rimonabant in overweight or obese patients with type 2 diabetes: a randomized controlled study. Lancet 2006; 368: 1660–72
Osei-Hyiaman D, DePetrillo M, Pacher P, et al. Endo-cannabinoid activation at hepatic CB1 receptors stimulates fatty acid synthesis and contributes to diet-induced obesity. J Clin Invest 2005; 115: 1298–305
Bensaid M, Gary-Bobo M, Esclangon A, et al. The cannabinoid CB1 receptor antagonist SR141716 increases ACRP30 mRNA expression in adipose tissue of obese fa/fa rats and in cultured adipocytes cells. Mol Pharmacol 2003; 63: 908–14
Ligaray K, Hachem S, Mazza A, et al. Repression of apolipoprotein A-I gene expression by anandamide [abstract no. 0214-OR]. The 67th Annual Meetings of the American Diabetes Association, Chicago, IL. Diabetes 2007; 56 Suppl. 1: A56
Ettinger WH, Varma VK, Sorci-Thomas M, et al. Cytokines decrease apolipoprotein accumulation in medium from HepG2 cells. Arterioscler Thromb 1994; 14: 8–13
Song H, Saito K, Fujigaki S, et al. IL-1b and TNF-α suppress apolipoprotein (apo) E secretion and apo A-I expression in HepG2 cells. Cytokine 1998; 10: 275–80
Haas MJ, Horani M, Mreyoud A, et al. Suppression of apolipoprotein AI gene expression in HepG2 cells by TNFα and IL-1β. Biochim Biophys Acta 2003; 1623: 120–8
Tacer KF, Kuzman D, Seliskar M, et al. TNF-α interferes with lipid homeostasis and activates acute and proatherogenic processes. Physiol Genomics 2007; 31: 216–27
Foldes G, von Haehling S, Anker SD. Toll-like receptor modulation in cardiovascular disease: a target for intervention? Expert Opin Investig Drugs 2006; 15: 857–71
Katsargyris A, Klonaris C, Bastounis E, et al. Toll-like receptor modulation: a novel therapeutic strategy in cardiovascular disease? Expert Opin Ther Targets 2008; 12: 1329–46
Fris-Moller N, Reiss P, Sabin CA, et al. Class of retroviral drugs and the risk of myocardial infarction. N Engl J Med 2007; 356: 1723–35
van der Valk M, Kastelein JJ, Murphy RL, et al. Nevirapine-containing antiretroviral therapy in HIV-1 infected patients results in an anti-atherogenic lipid profile. AIDS 2001; 15: 2407–14
van Leth F, Phanuphak P, Stroes E, et al. Nevirapine and efavirenz elicit different changes in lipid profiles in antiretroviral-therapy-naïve patients infected with HIV-1. PLoS Med 2004; 1: e19
Franssen R, Sankatsing RR, Hassink E, et al. Nevirapine increases high-density lipoprotein cholesterol concentrations by stimulation of apolipoprotein A-I production. Aterioscler Thromb Vasc Biol 2009; 29: 1336–41
Sirtori C, Calabresi L, Franceschini G, et al. Cardiovascular status of carriers of the apolipoprotein A-I Milano mutant, the Limone sul Garda study. Circulation 2001; 103: 1949–54
Calabresi L, Canavesi M, Bernini F, et al. Cell cholesterol efflux to reconstituted high-density lipoproteins containing the apolipoprotein A-I Milano dimer. Biochemistry 1999; 38: 16307–14
Nissen SE, Tsunoda T, Tuzcu EM, et al. Effect of recombinant apo A-I Milano on coronary atherosclerosis in patients with acute coronary syndromes: a randomized controlled trial. JAMA 2003; 290: 2292–300
Bielicki JK, McCall MR, Stolzfus LJ, et al. Evidence that apolipoprotein A-IMilano has reduced capacity, compared with wild-type apolipoprotein A-I, to recruit membrane cholesterol. Arterioscler Thromb Vasc Biol 1997; 17: 1637–43
Weibel GL, Alexander ET, Joshi MR, et al. Wild-type apo A-I and the Milano variant have similar abilities to stimulate cellular lipid mobilization and efflux. Arterioscler Thromb Vasc Biol 2007; 27: 2022–9
Anantharamaiah GM, Jones JL, Brouillette CG, et al. Studies of synthetic peptide analogs of amphipathic helix I: structure of peptide/DMPC complexes. J Biol Chem 1985; 260: 10248–55
Datta B, Chaddha M, Hama S, et al. Effects of increasing hydrophobicity on the physical-chemical and biological properties of a class A amphipathic helical peptide. J Lipid Res 2001; 42: 1096–104
Gomaraschi M, Calabresi L, Rossoni G, et al. Anti-inflammatory and cardioprotective activities of synthetic high-density lipoprotein containing apolipoprotein A-I mimetic peptides. J Pharmacol Exp Therap 2008; 324: 776–83
Datta G, White CR, Dashti N, et al. Anti-inflammatory and recycling properties of an apolipoprotein mimetic peptide, Ac-hE18-NH2. Atherosclerosis 2010; 208: 134–41
Rubin EM, Krauss RM, Spangler EA, et al. Inhibition of early atherogenesis in transgenic mice by human apolipoprotein AI. Nature 1991; 353: 265–7
Plump AS, Scott CJ, Breslow JL. Human apolipoprotein A-I gene expression increases high-density lipoprotein and suppresses atherosclerosis in the apolipoprotein E-deficient mouse. Proc Natl Acad Sci U S A 1994; 91: 9607–11
Duverger N, Kruth H, Emmanuel F, et al. Inhibition of atherosclerosis development in cholesterol-fed human apolipoprotein A-I-transgenic rabbits. Circulation 1996; 94: 713–7
Benoit P, Emmanuel F, Caillaud JM, et al. Somatic gene transfer of human apo A-I inhibits atherosclerosis progression in mouse models. Circulation 1999; 99: 105–10
Tangirala RK, Tsukamoto K, Chun SH, et al. Regression of atherosclerosis induced by liver-directed gene transfer of apolipoprotein A-I in mice. Circulation 1999; 100: 1816–22
Cimmino G, Chen W, Speidl WS, et al. Safe and sustained over-expression of functional apoA-I/HDL in apoA-I null mice by muscular AAV8 gene transfer. J Cardiovasc Pharmacol 2009; 54: 405–11
Kitajima K, Marchadier DH, Burstein H, et al. Persistent liver expression of murine apo A-I using vectors based on adeno-associated viral vectors serotypes 5 and 1. Atherosclerosis 2006; 186: 65–73
Gao GP, Alvira MR, Wang L, et al. Novel adeno-associated viruses from rhesus monkeys as vectors for human gene therapy. Proc Natl Acad Sci U S A 2002; 99: 11854–9
Cabana VG, Lukens JR, Rice KS, et al. HDL content and composition in acute phase response in three species: triglyceride enrichment of HDL a factor in its decrease. J Lipid Res 1996; 37: 2662–74
Van Lenten BJ, Hama SY, de Beer FC, et al. Anti-inflammatory HDL becomes pro-inflammatory during the acute phase response: loss of protective effect of HDL against LDL oxidation in aortic wall cocultures. J Clin Invest 1995; 96: 2758–67
Ansell BJ. The two faces of ’good’ cholesterol. Cleveland Clin J Med 2007; 74: 697–705
Kathiresan S, Willer CJ, Peloso GM, et al. Common variants at 30 loci contribute to polygenic dyslipidemia. Nat Genet 2009; 41: 56–65
Brooks-Wilson A, Marcil M, Clee SM, et al. Mutations in ABCA1 in Tangier disease and familial high-density lipoprotein deficiency. Nat Genet 1999; 22: 336–45
Altmann SW, Davis HR, Zhu L, et al. Niemann-Pick C1-Like1 protein is critical for intestinal cholesterol absorption. Science 2004; 303: 1201–4
Acknowledgements
This work is supported by the University of Florida — Jacksonville College of Medicine research grant to Michael Haas. The authors declare that no conflicts of interest exist that prejudice the impartiality of this review article, and that there are no financial or other conflicts of interest associated with the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Haas, M.J., Mooradian, A.D. Therapeutic Interventions to Enhance Apolipoprotein A-I-Mediated Cardioprotection. Drugs 70, 805–821 (2010). https://doi.org/10.2165/11535410-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11535410-000000000-00000