Abstract
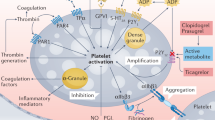
Prasugrel is a new P2Y12 receptor antagonist that has been investigated for the treatment of atherothrombosis in patients with cardiovascular disease undergoing percutaneous coronary intervention (PCI). Similar to other thienopyridines, prasugrel is a prodrug that requires biologic conversion to active metabolites.
Studies have demonstrated the ability of prasugrel to selectively and irreversibly inhibit ADP-induced platelet aggregation to a greater degree than clopidogrel. In a large randomized, double-blind, double-dummy clinical trial, it was demonstrated that treatment with prasugrel (n=6813; 60mg loading dose followed by 10 mg/day) significantly reduced the incidence of a composite endpoint of death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke during the median follow-up of 14.5 months, compared with clopidogrel (n=6795; 300mg loading dose followed by 75 mg/day) in patients with acute coronary syndromes scheduled to undergo PCI. The number of patients who would need to be treated with prasugrel instead of clopidogrel in order to prevent one primary efficacy outcome was 46.
Landmark analyses found that prasugrel not only reduced the incidence of individual clinical endpoints and stent thrombosis during the loading dose phase (randomization to 3 days), but also that these benefits continued throughout the maintenance phase (from 3 days until the end of the trial). Nonsurgical-related Thrombolysis In Myocardial Infarction (TIMI)-major and life-threatening bleeds were significantly more frequent in patients receiving prasugrel compared with clopidogrel. Patients with a history of stroke or transient ischemic attack (TIA) seem to be at especially high risk for bleeding, as well as patients aged >75 years and those weighing <60kg.
A prespecified analysis of net clinical benefit, which took into account the effects on both the primary efficacy and safety endpoints, was conducted. After taking into account the higher bleeding rates, the net clinical benefit still favored prasugrel use compared with clopidogrel. However, patients with prior stroke or TIA, patients older than 75 years, and patients weighing <60kg did not demonstrate a net clinical benefit with prasugrel use.
Prasugrel was approved for use in Europe by the European Commission in February 2009, and is currently available in the UK. In July 2009, the US Food and Drug Administration (FDA) approved the use of prasugrel for the reduction of thrombotic cardiovascular events (including stent thrombosis) in patients with acute coronary syndrome who are to be managed with PCI.






Similar content being viewed by others
References
Davi G, Patrono C. Platelet activation and atherothrombosis. N Engl J Med 2007; 357: 2482–94.
Ruggeri ZM. Mechanisms initiating platelet thrombus formation. Thromb Haemost 1997; 78: 611–6.
Ibanez B, Vilahur G, Badimon JJ. Pharmacology of thienopyridines: rationale for dual pathway inhibition. Eur Heart J 2006; 8 Suppl. G: G3–9.
Packham MA, Mustart JF. Platelet aggregation and adenosine diphosphate/ adenosine triphosphate receptors: a historical perspective. Semin Thromb Hemost 2005;31: 129–38.
Boeynaems JM, Communi D, Gonzalez JS, et al. Overview of P2 receptors. Semin Thromb Hemost 2005; 31: 139–49.
Storey FR. Biology and pharmacology of the platelet P2Y12 receptor. Curr Pharm Des 2006; 12: 1255–9.
Jin J, Kunapuli SP. Coactivation of two different G protein-coupled receptors is essential for ADP-induced platelet aggregation. Proc Natl Acad Sci U S A 1998; 95: 8070–4.
Sharis PJ, Cannon CP, Loscalzo J. The antiplatelet effects of ticlopidine and clopidogrel. Ann Intern Med 1998; 129: 394–405.
Hollopeter G, Jantzen HM, Vincent D, et al. Identification of the platelet ADP receptor targeted by antithrombotic drugs. Nature 2001; 409: 202–7.
Nichols RA. Identification of the P2Y12 receptor: a novel member of the P2Y family of receptors activated by extracellular nucleotides. Mol Pharmacol 2001; 60: 416–20.
Cattaneo M, Akkawat B, Lecchi A, et al. Ticlopidine selectively inhibits human platelet responses to adenosine diphosphate. Thromb Haemost 1991; 66: 694–9.
Boneu B, Destelle G, on behalf of the Study Group. Platelet anti-aggregating activity and tolerance of clopidogrel in atherosclerotic patients. Thromb Haemost 1996; 76: 939–43.
Savi P, Nurden P, Nurden A, et al. Clopidogrel: a review of its mechanism of action. Platelets 1998; 9: 251–5.
Jarvis B, Simpson K. Clopidogrel: a review of its use in the prevention of atherothrombosis. Drugs 2000; 60: 347–77.
Schomig A, Neumann FJ, Kastrati A, et al. A randomized comparison of antiplatelet and anticoagulant therapy after the placement of coronary-artery stents. N Engl J Med 1996; 334: 1084–9.
Hall P, Nakamura S, Maiello L, et al. A randomized comparison of combined ticlopidine therapy versus aspirin therapy alone after successful intravascular ultrasound-guided stent implantation. Circulation 1996; 93: 215–22.
Leon MB, Baim DS, Popma JJ, et al. A clinical trial comparing three antithrombotic drug regimens after coronary-artery stenting. N Engl J Med 1998; 339: 1665–71.
Bertrand ME, Legrand V, Boland J, et al. Randomized multicenter comparison of conventional anticoagulation versus antiplatelet therapy in unplanned and elective coronary stenting: the Full ANTicoagulation versus ASpirin and TIClopidine (FANTASTIC) study. Circulation 1998; 98: 1597–60.
Urban P, Macaya C, Rupprecht HJ, et al. Randomized evaluation of anti-coagulation versus antiplatelet therapy after coronary stent implantation in high-risk patients: the Multicenter Aspirin and Ticlopidine Trial after Intracoronary Stenting (MATTIS) trial. Circulation 1998; 98: 2126–32.
Moussa I, Oetgen M, Roubin G, et al. Effectiveness of clopidogrel and aspirin versus ticlopidine and aspirin in preventing stent thrombosis after coronary stent implantation. Circulation 1999; 99: 2364–6.
Betrand ME, Rupprecht HJ, Urban P, et al., for the CLASSICS Investigators. Double-blind study of the safety of clopidogrel with and without a loading dose in combination with aspirin compared with ticlopidine in combination with aspirin after coronary stenting. The Clopidogrel Aspirin Stent International Cooperative Study (CLASSICS). Circulation 2000; 102: 624–9.
Mehta SR, Yusuf S, Peters RJ, et al. Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: the PCI-CURE study. Lancet 2001; 358: 527–33.
Steinhubl SR, Berger PB, Mann III JT, et al. Early and sustained dual oral antiplatelet therapy following percutaneous coronary intervention: a randomized controlled trial. JAMA 2002; 288: 2411–20.
Mueller C, Roskamm H, Neumann FJ, et al. A randomized comparison of clopidogrel and aspirin versus ticlopidine and aspirin after the placement of coronary artery stents. J Am Coll Cardiol 2003; 41: 969–73.
Patti G, Colonna G, Pasceri V, et al. Randomized trial of high loading dose clopidogrel for reduction of periprocedural myocardial infarction in patients undergoing coronary intervention: results from the ARMYDA-2 (antiplatelet therapy for reduction of myocardial damage during angioplasty) study. Circulation 2005; 111: 2099–106.
Sabatine MS, Cannon CP, Gibson CM, et al. Effect of clopidogrel pretreatment before percutaneous coronary intervention in patients with ST-elevation myocardial infarction treated with fibrinolysis: the PCI-CLARITY study. JAMA 2005; 294: 1224–32.
von Beckerath N, Taubert D, Pogatsa-Murray G, et al. Absorption, metabolization, and antiplatelet effects of 300-, 600-, and 900-mg loading doses of clopidogrel: results of the ISAR-CHOICE (Intracoronary Stenting and Antithrombotic Regimen: Choose Between 3 High Oral Doses for Immediate Clopidogrel Effect) Trial. Circulation 2005; 112: 5946–50.
Levine GN, Berger PB, Cohen DJ, et al. Newer pharmacotherapy in patients undergoing percutaneous coronary interventions: a guide for pharmacists and other health care professionals. Expert opinion from the American Heart Association’s Diagnostic and Interventional Catheterization Committee and Council on Clinical Cardiology, and the American College of Clinical Pharmacy’s Cardiology Practice Research Network. Pharmacotherapy 2006; 26: 1537–56.
Grines CL, Bonow RO, Casey DE, et al. Prevention of premature discontinuation of dual antiplatelet therapy in patients with coronary artery stents: a scientific advisory from the American Heart Association, American College of Cardiology, Society for Cardiovascular Angiography and Interventions, American College of Surgeons, and American Dental Association, with Representation from the American College of Physicians. J Am Coll Cardiol 2007; 49: 378–402.
Siller-Matula J, Schror K, Wojta J, et al. Thienopyridines in cardiovascular disease: focus on clopidogrel resistance. Thromb Haemost 2007; 97: 385–93.
Nguyen TA, Diodati JG, Pharand C. Resistance to clopidogrel: a review of the evidence. J Am Coll Cardiol 2005; 45: 1157–64.
Gurbel PA, Bliden KP, Hiatt BL, et al. Clopidogrel for coronary stenting: response variability, drug resistance, and the effect of pretreatment platelet reactivity. Circulation 2003; 107: 2908–13.
Serebruany VL, Steinhubl SR, Berger PB, et al. Variability in platelet responsiveness to clopidogrel among 544 individuals. J Am Coll Cardiol 2005; 45: 246–51.
O’Donoghue M, Wiviott SD. Clopidogrel response variability and future therapies: clopidogrel: does one size fit all? Circulation 2006; 114: e600–6.
Gurbel PA, Bliden KP, Samara W, et al. Clopidogrel effect on platelet reactivity in patients with stent thrombosis: results of the CREST study. J Am Coll Cardiol 2005; 46: 1827–32.
Gurbel PA, Bliden KP. Durability of platelet inhibition by clopidogrel. Am J Cardiol 2003; 9: 1123–5.
Spertus JA, Kettelkamp R, Vance C, et al. Prevalence, predictors, and outcomes of premature discontinuation of thienopyridine therapy after drug-eluting stent placement: results from the PREMIER registry. Circulation 2006; 113:2803–9.
Pfisterer M, Brunner-LaRocca HP, Buser PT, et al., for the BASKET-LATE Investigators. Late clinical events after clopidogrel discontinuation may limit the benefit of drug-eluting stents. J Am Coll Cardiol 2006; 48: 2584–91.
Eisenstein EL, Anstrom KJ, Kong DR, et al. Clopidogrel use and long-term clinical outcomes after drug-eluting stent implantation. JAMA 2007; 197: 159–68.
Sugidachi A, Asai F, Ogawa T, et al. The in vivo pharmacologic profile of CS-747, a novel antiplatelet agent with platelet ADP receptor antagonist properties. Br J Pharmacol 2000; 129: 1439–46.
Sugidachi A, Asai F, Yoneda K, et al. Antiplatelet action of R-99224, an active metabolite of a novel thienopyridine-type Gi-linked P2T antagonist, CS-747. Br J Pharmacol 2001; 132: 47–54.
Hasegawa M, Sugidachi A, Ogawa T, et al. Steroselective inhibition of human platelet aggregation by R-138727, the active metabolite of CS-747 (Prasugrel, LY640315), a novel P2Y12 receptor inhibitor. Thromb Haemost 2005; 94: 593–8.
Savi P, Labouret C, Delesque N, et al. P2Y12, a new platelet ADP receptor, target of clopidogrel. Biochem Biophys Res Commun 2001; 283: 37–83.
Frelinger AL, Jakubowski JA, Barnard MR, et al. The active metabolite of prasugrel inhibits ADP-stimulated thrombo-inflammatory markers of platelet activation: influence of other blood cells, calcium, and aspirin. Thromb Haemost 2007; 98: 192–200.
Sugidachi A, Ogawa T, Kurihara A, et al. The greater in vivo antiplatelet effects of prasugrel as compared to clopidogrel reflect more efficient generation of its active metabolite with similar antiplatelet activity to that of clopidogrel’s active metabolite. J Thromb Haemost 2007; 5: 1545–51.
Hashimoto M, Sugidachi A, Isobe T, et al. The influence of P2Y12 receptor deficiency on the platelet inhibitory activities of prasugrel in a mouse model: evidence for specific inhibition of P2Y12 receptors by prasugrel. Biochem Pharmacol 2007; 74: 1003–9.
Asai F, Jakubowski JA, Naganuma H, et al. Platelet inhibitory activity and pharmacokinetics of prasugrel (CS-747) a novel thienopyridine P2Y12 inhibitor: a single ascending dose study in healthy humans. Platelets 2006; 17: 209–17.
Matsushima N, Jakubowski JA, Asai F, et al. Platelet inhibitory activity and pharmacokinetics of prasugrel (CS-747) a novel thienopyridine P2Y12 inhibitor: a multiple-dose study in healthy humans. Platelets 2006; 17: 218–26.
Jakubowski JA, Payne CD, Brandt JT, et al. The platelet inhibitory effects and pharmacokinetics of prasugrel after administration of loading and maintenance doses in healthy subjects. J Cardiovasc Pharmacol 2006; 47: 377–84.
Jakubowski JA, Matsushima N, Asai F, et al. A multiple dose study of prasugrel (CS-747), a novel thienopyridine P2Y12 inhibitor, compared with clopidogrel in healthy humans. Br J Clin Pharmacol 2006; 63: 421–30.
Jakubowski JA, Payne CD, Weerakkody GJ, et al. Dose-dependent inhibition of human platelet aggregation by prasugrel and its interaction with aspirin in healthy subjects. J Cardiovasc Pharmacol 2007; 49: 167–73.
Niitsu Y, Jakubowski JA, Sugidachi A, et al. Pharmacology of CS-747 (prasugrel, LY640315), a novel, potent antiplatelet agent with in vivo P2Y12 receptor antagonist activity. Semin Thromb Hemost 2005; 31: 184–94.
Fayer Rehmal JL, Eckstein JA, Farid DA, et al. Interactions of two major metabolites of prasugrel, a thienopyridine antiplatelet agent, with the cytochromes P450. Drug Metab Disp 2006; 34: 600–7.
Farid DA, Payne CD, Small DS, et al. Cytochrome P450 3A inhibition by ketoconazole affects prasugrel and clopidogrel pharmacokinetics and pharmacodynamics differently. Clin Pharmacol Ther 2007; 81: 735–41.
Wickremsinhe ER, Tian Y, Ruterbories KJ, et al. Stereoselective metabolism of prasugrel in humans using a novel chiral liquid chromatography-tandem mass spectrometry method. Drug Metab Disp 2007; 35: 917–21.
Farid NA, Smith RL, Gillespie TA, et al. The disposition of prasugrel, a novel thienopyridine, in humans. Drug Metab Disp 2007;35:1096–104.
Hirota T, Asai H, Asai F, et al. Efficacy of CS-747, a new potent antiplatelet agent [abstract no. PII-5]. Clin Pharmacol Ther 1999; 65: 148.
Saw J, Steinhubl SR, Berger PB, et al. Lack of adverse clopidogrel-atorvastatin clinical interaction from secondary analysis of a randomized, placebo-controlled clopidogrel trial. Circulation 2003; 108: 921–4.
Dmall DS, Farid NA, Li YG, et al. Effect of ranitidine on the pharmacokinetics and pharmacodynamics of prasugrel and clopidogrel. Curr Med Res Opin 2008; 24: 2251–7.
Gilard M, Arnaud B, Le Gal G, et al. Influence of omeprazole on the antiplatelet action of clopidogrel associated to aspirin. J Thromb Haemost 2006; 4: 2508–9.
Gilard M, Arnaud B, Cornily JC, et al. Influence of omeprazole on the antiplatelet action of clopidogrel associated with aspirin: the randomized, double-blind OCLA (Omeprazole Clopidogrel Aspirin) study. J Am Coll Cardiol 2008; 51: 256–60.
Ho PM, Maddox TM, Wang L, et al. Proton pump inhibitors may attenuate the benefits of clopidogrel among ACS patients: empirical evidence from 3,311 ACS patients [abstract no. 6241]. Circulation 2008; 118(18 Suppl.): S1165.
Aubert RE, Epstein RS, Teagarden JR, et al. Proton pump inhibitors effect on clopidogrel effectiveness: the clopidogrel Medco outcomes study [abstract no. 3998]. Circulation 2008; 118(18. Suppl.): S815.
Dunn SP, Macaulay TE, Brennan DM, et al. Baseline proton pump inhibitor use is associated with increased cardiovascular events with and without the use of clopidogrel in the CREDO trial [abstract no. 3999]. Circulation 2008; 118(18 Suppl.): S815.
Small DS, Farid NA, Payne CD, et al. Effects of the proton pump inhibitor lansoprazole on the pharmacokinetics and pharmacodynamics of prasugrel and clopidogrel. J Clin Pharmacol 2008; 48: 475–84.
O’Donoghue M, Wiviott SD, Murphy SA, et al. Absence of an interaction between drugs metabolized by cytochrome P450 enzymes and the benefit of treatment with prasugrel versus clopidogrel inpatients with acute coronary syndromes undergoing percutaneous intervention: a TRITON-TIMI 38 analysis [abstract no. 1032–143]. J Am Coll Cardiol 2009; 53 Suppl. A: A328.
Lau WC, Waskell LA, Watkins PB, et al. Atorvastatin reduces the ability of clopidogrel to inhibit platelet aggregation: a new drug-drug interaction. Circulation 2003; 107: 32–7.
Mitsios JV, Papathanasiou AI, Rodis FI, et al. Atorvastatin does not affect the antiplatelet potency of clopidogrel when it is administered concomitantly for 5 weeks in patients with acute coronary syndromes. Circulation 2004; 109:1335–8.
Serebruany VL, Midei MG, Malinin AI, et al. Absence of interaction between atorvastatin or other statins and clopidogrel: results from the interaction study. Arch Intern Med 2004; 164: 2051–7.
Waneweser P, Windecker S, Billinger M, et al. Effect of atorvastatin and pravastatin on platelet inhibition by aspirin and clopidogrel treatment in patients with coronary stent thrombosis. Am J Cardiol 2007; 99: 353–6.
Saw J, Brennan DM, Steinhubl SR, et al. Lack of evidence of a clopidogrel-statin interaction in the CHARISMA trial. J Am Coll Cardiol 2007; 50: 291–5.
Riondino S, Petrini N, Donato L, et al. Effects of rosuvastatin on platelet inhibition by clopidogrel in cardiovascular patients. J Thromb Thrombolysis. Epub 2008 Jul 18.
Farid NA, Small DS, Payne CD, et al. Effect of atorvastatin on the pharmacokinetics and pharmacodynamics of prasugrel and clopidogrel in healthy subjects. Pharmacotherapy 2008; 28: 1483–94.
Jernberg T, Payne CD, Winters KJ, et al. Prasugrel achieves greater inhibition of platelet aggregation and a lower rate of non-responders compared with clopidogrel in aspirin-treated patients with stable coronary artery disease. Eur Heart J 2006; 27: 1166–73.
Brandt JT, Payne CD, Wiviott SD, et al. A comparison of prasugrel and clopidogrel loading doses on platelet function: magnitude of platelet inhibition is related to active metabolite formation. Am Heart J 2007; 153: e9–16.
Weerakkody GJ, Jakubowski JA, Brandt JT, et al. Comparison of speed of onset of platelet inhibition after loading doses of clopidogrel versus prasugrel in healthy volunteers and correlation with responder status. Am J Cardiol 2007; 100: 331–6.
Wiviott SD, Antman EM, Winters KJ, et al., for the JUMBO-TIMI 26 Investigators. Randomized comparison of prasugrel (CS-747, LY640315), a novel thienopyridine P2Y12 antagonist, with clopidogrel in percutaneous coronary intervention: results of the Joint Utilization of Medications to Block Platelets Optimally (JUMBO)-TIMI 26 Trial. Circulation 2005; 111: 3366–73.
Bovill EG, Terrin ML, Stump DC, et al. Hemorrhagic events during therapy with recombinant tissue-type plasminogen activator, heparin, and aspirin for acute myocardial infarction: results of the Thrombolysis in Myocardial Infarction (TIMI), phase II trial. Ann Intern Med 1991; 115: 256–5.
Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). J Am Coll Cardiol 2004; 44: E1–211.
Wiviott SD, Trank D, Frelinger AL, et al., for the PRINCIPLE-TIMI 44 Investigators. Prasugrel compared with high loading- and maintenance-dose clopidogrel in patients with planned percutaneous coronary intervention: the prasugrel in comparison to clopidogrel for inhibition of platelet activation and aggregation — Thrombolysis in Myocardial Infarction 44 trial. Circulation 2007; 116: 2923–32.
Montalescot G, Sideris G, Meuleman C, et al. A randomized comparison of high clopidogrel loading doses in patients with non-ST-segment elevation acute coronary syndromes: the ALBION (Assessment of the BEST Loading Dose of Clopidogrel to Blunt Platelet Activation, Inflammation and Ongoing Necrosis) trial. J Am Coll Cardiol 2006; 48: 931–8.
von Beckerath N, Taubert D, Pogatsa-Murray G, et al. Absorption, metabolization, and antiplatelet effects of 300-, 600-, and 900-mg loading doses of clopidogrel: results of the ISAR-CHOISE (Intracoronary Stenting and Antithrombotic Regimen: Choose Between 3 High Oral Doses for Immediate Clopidogrel Effect) trial. Circulation 2005; 112: 2946–50.
Payne CD, Li YG, Brandt JT, et al. Switching directly to prasugrel from clopidogrel results in greater inhibition of platelet aggregation in aspirin-treated subjects. Platelets 2008; 19: 275–81.
Montalescot G, Sideris G, Cohen R, et al. Prasugrel 10mg provides greater platelet inhibition than clopidogrel 900/150mg in UA/NSTEMI ACS — the ACAPULCO study [abstract no. 4408]. Eur Heart J 2008; 29: 716.
Angiolillo DJ, Bates ER, Bass TA. Clinical profile of prasugrel, a novel thienopyridine. Am Heart J 2008; 156: s16–22.
ClinicalTrials.gov. Third Optimizing Anti-Platelet Therapy in Diabetes MellitUS (OPTIMUS-3) [ClinicalTrials.gov identifier NCT00642174]. US National Institutes of Health, ClinicalTrials.gov [online]. Available from URL: http://www.clinicaltrials.gov [Accessed 2008 Nov 18].
Wiviott SD, Antman EM, Gibson CM, et al., for the TRITON-TIMI 38 Investigators. Evaluation of prasugrel compared with clopidogrel in patients with acute coronary syndromes: design and rationale for the TRial to assess Improvement in Therapeutic Outcomes by optimizing platelet InhibitioN with prasugrel Thrombolysis In Myocardial Infarction 38 (TRITON-TIMI 38). Am Heart J 2006; 152: 627–35.
Wiviott SD, Braunwald E, McCabe CH, et al., for the TRITON-TIMI 38 Investigators. Prasugrel versus clopidogrel in patients with acute coronary syndrome. N Engl J Med 2007; 357: 2001–15.
Antman EM, Wiviott SD, Murphy SA, et al. Early and late benefits of prasugrel in patients with acute coronary syndromes undergoing percutaneous coronary intervention: a TRITON-TIMI 38 (Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet InhibitioN with Prasugrel — Thrombolysis In Myocardial Infarction) analysis. J Am Coll Cardiol 2008; 51: 2028–33.
Murphy SA, Antman EM, Wiviott SD, et al. Reduction in recurrent cardiovascular events with prasugrel compared with clopidogrel in patients with acute coronary syndromes from the TRITON-TIMI 38 trial. Eur Heart J 2008; 29: 2473–9.
Wiviott SD, Braunwald E, McCabe CH, et al. Intensive oral antiplatelet therapy for reduction of ischaemic events including stent thrombosis in patients with acute coronary syndromes treated with percutaneous coronary intervention and stenting in the TRITON-TIMI 38 trial: a subanalysis of a randomized trial. Lancet 2008; 371: 1353–63.
Wiviot SD, Braunwald E, Angiolillo DJ, et al. Greater clinical benefit of more intense oral antiplatelet therapy with prasugrel in patients with diabetes mellitus in the Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet InhibitioN with Prasugrel — Thrombolysis In Myocardial Infarction 38. Circulation 2008; 118: 1626–36.
Serebruany VL, Alberts MJ, Hanley DF. Prasugrel in the poststroke cohort of the TRITON trial: the clear and present danger. Cerebrovasc Dis 2008; 26: 93–4.
Bhatt DL. Intensifying platelet inhibition: navigating between Scylla and Charybdis. N Engl J Med 2007; 357: 2078–81.
Diener HC, Bogousslavsky J, Brass LM, et al. Aspirin and clopidogrel compared with clopidogrel alone after recent ischaemic stroke or transient ischaemic attack in high-risk patients (MATCH): randomized, double-blind, placebo-controlled trial. Lancet 2004; 364: 331–7.
Kaul S, Shah PK, Diamond GA. Weighted composite endpoint analysis of TRITON-TIMI 38: disconnect between analytical equivalence and clinical importance [abstract no. 4587]. Circulation 2008; 118(18 Suppl.): S916.
Serebruany VL. Platelet inhibition with prasugrel and increased cancer risks: potential causes and implications. Am J Med 2009; 122: 407–8.
ClinicalTrials.gov. A comparison of prasugrel and clopidogrel in acute coronary syndrome subjects (TRILOGY ACS) [ClinicalTrials.gov identifier NCT00699998]. US National Institutes of Health, ClinicalTrials.gov [online]. Available from URL: http://www.clinicaltrials.gov [Accessed 2008 Aug 26].
King SB, Smith SC, Hirshfeld JW, et al. 2007 focused update of the ACC/AHA/SCAI 2005 guideline update for percutaneous coronary intervention: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2008; 51: 172–209.
Harrington RA, Becker RC, Cannon CP, et al. Antithrombotic therapy for non-ST-segment elevation acute coronary syndromes: American College of Chest Physicians evidence-based practice guidelines. 8th ed. Chest 2008; 133: 670–707S.
Smith SC, Feldman TE, Hirshfeld JW, et al. ACC/AHA/SCAI 2005 guideline update for percutaneous coronary intervention: a report of the American College of Cardiology/American Heart Association task force on practice guidelines. J Am Coll Cardiol 2006; 47: e1–121.
Varenhorst C, Braun O, James S, et al. Greater inhibition of platelet ‘aggregation with a prasugrel 60mg loading dose compared with a clopidogrel 600mg loading dose in aspirin-treated patients [abstract]. Eur Heart J 2007; Suppl.: 189.
Winters KJ, Payne CD, Ernest CS, et al. Prasugrel 60mg versus clopidogrel 600mg: greater platelet inhibition with prasugrel is explained by higher concentrations of the active metabolite [abstract]. Eur Heart J 2007; Suppl.: 218.
Bassand JP. Unmet needs in antiplatelet therapy. Eur Heart J 2008; 10 Suppl.: D3–11.
Storey RF. Variability of response to antiplatelet therapy. Eur Heart J 2008; 10 Suppl.: A21–7.
Gurbel PA, Bliden KP, Hayes KM, et al. The relation of dosing to clopidogrel responsiveness and the incidence of high post-treatment platelet aggregation in patients undergoing coronary stenting. J Am Coll Cardiol 2005; 45: 1392–6.
Matetzky S, Shenkman B, Guetta V, et al. Clopidogrel resistance is associated with increased risk of recurrent atherothrombotic events in patients with acute myocardial infarction. Circulation 2004; 109: 3171–5.
ClinicalTrials.gov. Clopidogrel Optimal Loading Dose Usage to Reduce Recurrent EveNTs/Optimal Antiplatelet Strategy for InterventionS (CURRENT/OASIS7) trial [ClinicalTrials.gov identifier NCT00335452]. US National Institutes of Health, ClinicalTrials.gov [online]. Available from URL: http://www.clinicaltrials.gov [Accessed 2008 Aug 26].
Abuzahra M, Pillai M, Caldera A, et al. Comparison of higher clopidogrel loading and maintenance dose to standard dose on platelet function and outcomes after percutaneous coronary intervention using drug-eluting stents. Am J Cardiol 2008; 102: 401–3.
Weerakkody GJ, Jakubowski JA, Brandt JT, et al. Greater inhibition of platelet aggregation and reduced response variability with prasugrel versus clopidogrel: an integrated analysis. JCardiovasc Pharmacol Ther 2007; 12:205–12.
Acknowledgments
The preparation of this review was not supported by any external funding and no conflicts of interest exist with any author.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baker, W.L., White, C.M. Role of Prasugrel, a Novel P2Y12 Receptor Antagonist, in the Management of Acute Coronary Syndromes. Am J Cardiovasc Drugs 9, 213–229 (2009). https://doi.org/10.2165/1131209-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/1131209-000000000-00000