Abstract
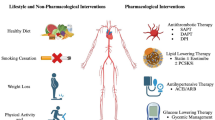
Oral prasugrel (Effient®; Efient®) provides rapid, potent inhibition of platelet aggregation. It is indicated (in combination with aspirin) for the prevention of atherothrombotic events in patients with acute coronary syndromes (ACS) undergoing percutaneous coronary intervention (PCI). In the pivotal clinical trial in this patient population, prasugrel-based therapy was associated with a significantly lower incidence of ischemic events than clopidogrel-based therapy. However, the efficacy of prasugrel was offset by a higher risk of bleeding than clopidogrel, with patients aged ≥75 years, those weighing <60 kg and those with a history of stroke or transient ischemic attack at the greatest risk. Prasugrel appears to have an overall favorable risk: benefit ratio in ACS patients undergoing PCI who do not have these three easily identifiable clinical characteristics. Limited pharmacoeconomic analyses suggest that prasugrel-based therapy is an economically attractive treatment strategy relative to clopidogrel-based therapy from a US healthcare payer perspective.




Similar content being viewed by others
References
Tcheng JE, Mackay SM. Prasugrel versus clopidogrel antiplatelet therapy after acute coronary syndrome: matching treatments with patients. Am J Cardiovasc Drugs 2012; 12(2): 83–91
Fintel DJ. Oral antiplatelet therapy for atherothrombotic disease: overview of current and emerging treatment options. Vasc Health Risk Manag 2012; 8: 77–89
Wright RS, Anderson JL, Adams CD, et al. 2011 ACCF/AHA focused update of the guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction (updating the 2007 guideline): a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 2011 May 10; 123(18): 2022–60
Mangiacapra F, Barbato E. Individual variability of response to antiplatelet therapy is an important determinant of adverse clinical outcome. High Blood Press Cardiovasc Prev 2010; 17(3): 121–30
Small DS, Farid NA, Payne CD, et al. Effect of intrinsic and extrinsic factors on the clinical pharmacokinetics and pharmacodynamics of prasugrel. Clin Pharmacokinet 2010; 49(12): 777–98
Vandvik PO, Lincoff AM, Gore JM, et al. Primary and secondary prevention of cardiovascular disease: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 2012 Feb; 141 (2 Suppl.): e637S–68S
Hillegass WB, Brott BC, Dobbs JC, et al. Oral antiplatelet therapy in diabetes mellitus and the role of prasugrel: an overview. Vasc Health Risk Manag 2011; 7: 445–59
Hasegawa M, Sugidachi A, Ogawa T, et al. Stereoselective inhibition of human platelet aggregation by R-138727, the active metabolite of CS-747 (prasugrel, LY640315), a novel P2Y12 receptor inhibitor. Thromb Haemost 2005 Sep; 94(3): 593–8
Effient® (prasugrel) tablets: US prescribing information. Indianapolis (IN): Eli Lilly and Company, 2011 Sep 27
Wiviott SD, Trenk D, Frelinger AL, et al. Prasugrel compared with high loading- and maintenance-dose clopidogrel in patients with planned percutaneous coronary intervention: the prasugrel in comparison to clopidogrel for inhibition of platelet activation and aggregation-thrombolysis in myocardial infarction 44 trial. Circulation 2007 Dec 18; 116(25): 2923–32
Angiolillo DJ. Variability in responsiveness to oral antiplatelet therapy. Am J Cardiol 2009 Feb 2; 103 (3 Suppl.): 27–34A
Mega JL, Close SL, Wiviott SD, et al. Genetic variants in ABCB1 and CYP2C19 and cardiovascular outcomes after treatment with clopidogrel and prasugrel in the TRITON-TIMI 38 trial: a pharmacogenetic analysis. Lancet 2010 Oct 16; 376(9749): 1312–9
Angiolillo DJ, Saucedo JF, Deraad R, et al. Increased platelet inhibition after switching from maintenance clopidogrel to prasugrel in patients with acute coronary syndromes: results of the SWAP (SWitching Anti Platelet) study. J Am Coll Cardiol 2010 Sep 21; 56(13): 1017–23
Montalescot G, Sideris G, Cohen R, et al. Prasugrel compared with high-dose clopidogrel in acute coronary syndrome: the randomised, double-blind ACAPULCO study. Thromb Haemost 2010 Jan; 103(1): 213–23
Wiviott SD, Braunwald E, McCabe CH, et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med 2007 Nov 15; 357(20): 2001–15
Wiviott SD, Braunwald E, McCabe CH, et al. Intensive oral antiplatelet therapy for reduction of ischaemic events including stent thrombosis in patients with acute coronary syndromes treated with percutaneous coronary intervention and stenting in the TRITON-TIMI 38 trial: a subanalysis of a randomised trial. Lancet 2008 Apr 19; 371(9621): 1353–63
Montalescot G, Wiviott SD, Braunwald E, et al. Prasugrel compared with clopidogrel in patients undergoing percutaneous coronary intervention for ST-elevation myocardial infarction (TRITON-TIMI 38): double-blind, randomised controlled trial. Lancet 2009 Feb 28; 373(9665): 723–31
Wiviott SD, Braunwald E, Angiolillo DJ, et al. Greater clinical benefit of more intensive oral antiplatelet therapy with prasugrel in patients with diabetes mellitus in the trial to assess improvement in therapeutic outcomes by optimizing platelet inhibition with prasugrel-thrombolysis in myocardial infarction 38. Circulation 2008 Oct 14; 118(16): 1626–36
Murphy SA, Antman EM, Wiviott SD, et al. Reduction in recurrent cardiovascular events with prasugrel compared with clopidogrel in patients with acute coronary syndromes from the TRITON-TIMI 38 trial. Eur Heart J 2008 Oct; 29(20): 2473–9
Antman EM, Wiviott SD, Murphy SA, et al. Early and late benefits of prasugrel in patients with acute coronary syndromes undergoing percutaneous coronary intervention: a TRITON-TIMI 38 (TRial to assess Improvement in Therapeutic Outcomes by optimizing platelet inhibitioN with prasugrel-Thrombolysis In Myocardial Infarction) analysis. J Am Coll Cardiol 2008 May 27; 51(21): 2028–33
Wiviott SD, Desai N, Murphy SA, et al. Efficacy and safety of intensive antiplatelet therapy with prasugrel from TRITON-TIMI 38 in a core clinical cohort defined by worldwide regulatory agencies. Am J Cardiol 2011 Oct 1; 108(7): 905–11
Pride YB, Wiviott SD, Buros JL, et al. Effect of prasugrel versus clopidogrel on outcomes among patients with acute coronary syndrome undergoing percutaneous coronary intervention without stent implantation: a TRial to assess Improvement in Therapeutic Outcomes by optimizing platelet inhibitioN with prasugrel (TRITON)-Thrombolysis in Myocardial Infarction (TIMI) 38 substudy. Am Heart J 2009 Sep; 158(3): e21–6
O’Donoghue M, Antman EM, Braunwald E, et al. The efficacy and safety of prasugrel with and without a glycoprotein IIb/IIIa inhibitor in patients with acute coronary syndromes undergoing percutaneous intervention: a TRITON-TIMI 38 (Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet Inhibition With Prasugrel-Thrombolysis In Myocardial Infarction 38) analysis. J Am Coll Cardiol 2009 Aug 18; 54(8): 678–85
Morrow DA, Wiviott SD, White HD. Effect of the novel thienopyridine prasugrel compared with clopidogrel on spontaneous and procedural myocardial infarction in the Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet Inhibition with Prasugrel-Thrombolysis in Myocardial Infarction 38: an application of the classification system from the universal definition of myocardial infarction. Circulation 2009 Jun; 119(21): 2758–64
Sorich MJ, Vitry A, Ward MB, et al. Prasugrel vs. clopidogrel for cytochrome P450 2C19-genotyped subgroups: integration of the TRITON-TIMI 38 trial data. J Thromb Haemost 2010 Aug; 8(8): 1678–84
Hochholzer W, Wiviott SD, Antman EM, et al. Predictors of bleeding and time dependence of association of bleeding with mortality: insights from the Trial to Assess Improvement in Therapeutic Outcomes by Optimizing Platelet Inhibition With Prasugrel-Thrombolysis in Myocardial Infarction 38 (TRITON-TIMI 38). Circulation 2011 Jun 14; 123(23): 2681–9
Thygesen K, Alpert JS, White HD, et al. Universal definition of myocardial infarction. Eur Heart J 2007 Oct; 28(20): 2525–38
Plavix® (clopidogrel bisulfate) tablets: US prescribing information. Bridge-water (NJ): Sanofi-Aventis, 2011 Dec
Mahoney EM, Wang K, Arnold SV, et al. Cost-effectiveness of prasugrel versus clopidogrel in patients with acute coronary syndromes and planned percutaneous coronary intervention: results from the trial to assess improvement in therapeutic outcomes by optimizing platelet inhibition with Prasugrel-Thrombolysis in Myocardial Infarction TRITON-TIMI 38. Circulation 2010 Jan 5; 121(1): 71–9
Mauskopf JA, Graham JB, Bae JP, et al. Cost-effectiveness of prasugrel in a US managed care population. J Med Econ 2012; 15(1): 166–74
Biondi-Zoccai G, Lotrionte M, Agostoni P, et al. Adjusted indirect comparison meta-analysis of prasugrel versus ticagrelor for patients with acute coronary syndromes. Int J Cardiol 2011 Aug 4; 150(3): 325–31
Chin CT, Roe MT, Fox KA, et al. Study design and rationale of a comparison of prasugrel and clopidogrel in medically managed patients with unstable angina/non-ST-segment elevation myocardial infarction: the TaRgeted platelet Inhibition to cLarify the Optimal strate Gyto medicallY manage Acute Coronary Syndromes (TRILOGY ACS) trial. Am Heart J 2010 Jul; 160(1): 16–22
Acknowledgments and Disclosures
This article was reviewed by E.R. Bates, Internal Medicine, University of Michigan, Ann Arbor, Michigan, USA.
The preparation of this article was not supported by any external funding. During the peer review process, the manufacturer of the agent under review was offered an opportunity to comment on the article. Changes resulting from comments received were made by the author on the basis of scientific and editorial merit.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lyseng-Williamson, K.A. Prasugrel: A Guide to Its Use in Patients with Acute Coronary Syndromes Undergoing Percutaneous Coronary Intervention in the US. Am J Cardiovasc Drugs 12, 207–216 (2012). https://doi.org/10.2165/11209640-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11209640-000000000-00000