Abstract
Intravenous esomeprazole (Nexium®) is approved in Europe for the prevention of rebleeding following therapeutic endoscopy for acute bleeding gastric or duodenal ulcers.
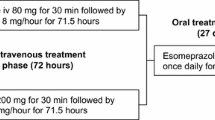
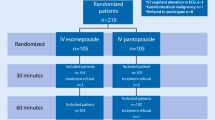
In a pivotal clinical trial, patients with peptic ulcer bleeding and high-risk stigmata who received intravenous esomeprazole for 72 hours following endoscopic haemostatic therapy were significantly less likely than those receiving intravenous placebo to experience recurrent peptic ulcer bleeding at days 3, 7 and 30. In addition, the need for repeat endoscopic haemostatic therapy, the total amount of blood transfused and the number of additional hospital days required because of rebleeding were significantly lower in intravenous esomeprazole recipients than in intravenous placebo recipients. All patients received oral esomeprazole for 27 days following intravenous study drug administration.
Intravenous esomeprazole was generally well tolerated in the pivotal trial, with infusion-site reactions being among the most commonly reported adverse events.
Two pharmacoeconomic analyses conducted from a healthcare payer perspective used decision-tree models with 30-day time horizons to examine the cost effectiveness and cost utility of intravenous esomeprazole in patients with bleeding peptic ulcers who had undergone endoscopic haemostatic therapy.
With regard to the incremental cost per bleed averted, intravenous esomeprazole was predicted to be dominant in Spain and cost effective in Sweden and the US compared with no intravenous esomeprazole. Efficacy results and resource utilization data from the pivotal clinical trial were inputted into this model, and the results of the analysis were generally robust to plausible variations in key variables.
In the cost-utility analysis, which was conducted in the UK and is available as an abstract and poster, esomeprazole was considered to be the most cost-effective treatment alternative, compared with omeprazole or pantoprazole. For this analysis, clinical outcomes data were obtained from a systematic review and mixed treatment comparison (given the absence of head-to-head trial data), and utility values were proxied from the literature.
In conclusion, intravenous esomeprazole prevents peptic ulcer rebleeding in patients who have undergone endoscopic haemostatic therapy. Pharmacoeconomic analyses support the use of intravenous esomeprazole following endoscopic haemostatic therapy in patients with peptic ulcer bleeding and high-risk stigmata.
Similar content being viewed by others
References
Longstreth GF. Epidemiology of hospitalization for acute upper gastrointestinal hemorrhage: a population-based study. Am J Gastroenterol 1995 Feb; 90 (2): 206–10
Barkun A, Leontiadis G. Systematic review of the symptom burden, quality of life impairment and costs associated with peptic ulcer disease. Am J Med 2010 Apr; 123 (4): 358–66
Barkun A, Sabbah S, Enns R, et al. The Canadian Registry on Nonvariceal Upper Gastrointestinal Bleeding and Endo-scopy (RUGBE): endoscopic hemostasis and proton pump inhibition are associated with improved outcomes in a real-life setting. Am J Gastroenterol 2004 Jul; 99 (7): 1238–46
Lanas A, Calvet X, Feu F, et al. First Spanish consensus on peptic ulcer bleeding management [in Spanish]. Med Clin (Barc) 2010 Nov 6; 135 (13): 608–16
Adler DG, Leighton JA, Davila RE, et al. ASGE guideline: the role of endoscopy in acute non-variceal upper-GI hemorrhage. Gastrointest Endosc 2004 Oct; 60 (4): 497–504
Barkun AN, Bardou M, Kuipers EJ, et al. International consensus recommendations on the management of patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med 2010 Jan 19; 152 (2): 101–13
British Society of Gastroenterology Endoscopy Committee. Non-variceal upper gastrointestinal haemorrhage: guidelines. Gut 2002; 51 Suppl. IV: 1–6
Scottish Intercollegiate Guidelines Network. Management of acute upper and lower gastrointestinal bleeding: a national clinical guideline [online]. Available from URL: http://www.sign.ac.uk/pdf/sign105.pdf [Accessed 2011 Feb 24]
Medical News Today. AstraZeneca secures approval for Nexium® (esomeprazole) in peptic ulcer bleed, Europe [media release; online]. Available from URL: http://www.medicalnewstoday.com/articles/148911.php [Accessed 2011 Feb 22]
AstraZeneca UK Limited. Nexium I.V. 40 mg powder for solution for injection/infusion: UK summary of product characteristics [online]. Available from URL: http://www.medicines.org.uk/EMC/medicine/14054/SPC/Nexium+I.V.+40mg+Powder+for+solution+for+injection+infusion/ [Accessed 2011 Feb 22]
AstraZeneca UK Limited. Nexium 20 mg and 40 mg tablets: UK summary of product characteristics [online]. Available from URL: http://www.medicines.org.uk/EMC/medicine/14307/SPC/Nexium+20mg+%26+40mg+Tablets/ [Accessed 2011 Feb 22]
AstraZeneca LP. Nexium® I.V. (esomeprazole sodium) for injection: US prescribing information [online]. Available from URL: http://www.accessdata.fda.gov/drugsatfda_docs/label/2010/021689s018lbl.pdf [Accessed 2011 Mar 24]
Wyeth Pharmaceuticals Inc. Protonix® I.V. (pantoprazole sodium) for injection: US prescribing information [online]. Available from URL: http://www.accessdata.fda.gov/drugsatfda_docs/label/2010/020988s040lbl.pdf [Accessed 2011 Mar 24]
Blatchford O, Davidson LA, Murray WR, et al. Acute upper gastrointestinal haemorrhage in west of Scotland: case ascertainment study. BMJ 1997 Aug 30; 315 (7107): 510–4
Theocharis GJ, Thomopoulos KC, Sakellaropoulos G, et al. Changing trends in the epidemiology and clinical outcome of acute upper gastrointestinal bleeding in a defined geographical area in Greece. J Clin Gastroenterol 2008 Feb; 42 (2): 128–33
Vreeburg EM, Snel P, de Bruijne JW, et al. Acute upper gastrointestinal bleeding in the Amsterdam area: incidence, diagnosis, and clinical outcome. Am J Gastroenterol 1997 Feb; 92 (2): 236–43
van Leerdam ME, Vreeburg EM, Rauws EAJ, et al. Acute upper GI bleeding: did anything change? Time trend analysis of incidence and outcome of acute upper GI bleeding between 1993/1994 and 2000. Am J Gastroenterol 2003 Jul; 98 (7): 1494–9
Targownik LE, Nabalamba A. Trends in management and outcomes of acute nonvariceal upper gastrointestinal bleeding: 1993–2003. Clin Gastroenterol Hepatol 2006 Dec; 4 (12): 1459–66
Rockall TA, Logan RFA, Devlin HB, et al. Incidence of and mortality from acute upper gastrointestinal haemorrhage in the United Kingdom. BMJ 1995 Jul 22; 311 (6999): 222–6
Kapsoritakis AN, Ntounas EA, Makrigiannis EA, et al. Acute upper gastrointestinal bleeding in central Greece: the role of clinical and endoscopic variables in bleeding outcome. Dig Dis Sci 2009 Feb; 54 (2): 333–41
de Leest H, van Dieten H, van Tulder M, et al. Costs of treating bleeding and perforated peptic ulcers in the Netherlands. J Rheumatol 2004 Apr; 31 (4): 788–91
Sörngård H, Sverdén-Eklund SE, Söderlund C, et al. Hospital costs for treatment of patients with peptic ulcer bleed (PUB) in Sweden: data from the KPP (cost per patient) database [abstract no. PG19 plus poster]. 13th Annual European Congress of the International Society for Phar-macoeconomics and Outcomes Research; 2010 Nov 6–9; Prague
Sung JJY, Barkun A, Kuipers EJ, et al. Intravenous esomeprazole for prevention of recurrent peptic ulcer bleeding: a randomized trial. Ann Intern Med 2009 Apr 7; 150 (7): 455–64
Barkun AN, Adam V, Sung JJY, et al. Cost effectiveness of high-dose intravenous esomeprazole for peptic ulcer bleeding. Pharmacoeconomics 2010; 28 (3): 217–30
Kuipers EJ, Sung JJ, Barkun A, et al. Safety and tolerability of high-dose intravenous esomeprazole for prevention of peptic ulcer rebleeding. Adv Ther 2011 Feb; 28 (2): 150–9
Borrill J, Edwards SJ, Gray J. Cost-effectiveness of highdose intravenous proton pump inhibitors (IV PPI) for the prevention of gastric or duodenal ulcer rebleeding after therapeutic endoscopy [abstract no. PG18]. Value Health 2009 Oct; 12 (7): A347. Plus poster presented at the 12th Annual European Congress of the International Society for Pharmacoeconomics and Outcomes Research; 2009 Oct 24–27; Paris
Edwards SJ, Gray J, Borrill J, et al. Intravenous (IV) proton pump inhibitors (PPIs) for the treatment of peptic ulcer bleeding [abstract no. PG13]. Value Health 2009 Oct; 12 (7): A346. Plus poster presented at the 12th Annual European Congress of the International Society for Pharmacoeconomics and Outcomes Research; 2009 Oct 24–27; Paris
Groeneveld PW, Lieu TA, Fendrick AM, et al. Quality of life measurement clarifies the cost-effectiveness of Helicobacter pylori eradication in peptic ulcer disease and uninvestigated dyspepsia. Am J Gastroenterol 2001 Feb; 96 (2): 338–47
Lau JYW, Sung JJY, Lee KKC, et al. Effect of intravenous omeprazole on recurrent bleeding after endoscopic treatment of bleeding peptic ulcers. N Engl J Med 2000 Aug 3;343 (5): 310–6
Lin H-J, Lo W-C, Lee F-Y, et al. A prospective randomized comparative trial showing that omeprazole prevents rebleeding in patients with bleeding peptic ulcer after successful endoscopic therapy. Arch Intern Med 1998 Jan 12; 158(1): 54–8
Canadian Agency for Drug Technologies in Health. Indirect evidence: indirect treatment comparisons in meta-analysis [online]. Available from URL: http://www.cadth.ca/media/pdf/H0462_itc_tr_e.pdf [Accessed 2011 Mar 24]
Laine L, Peterson WL. Bleeding peptic ulcer. N Engl J Med 1994 Sep 15; 331 (11): 717–27
Leontiadis GI, Sharma VK, Howden CW. Proton pump inhibitor therapy for peptic ulcer bleeding: Cochrane collaboration meta-analysis of randomized controlled trials. Mayo Clin Proc 2007 Mar; 82 (3): 286–96
Khuroo MS, Khuroo MS, Farahat KLC, et al. Treatment with proton pump inhibitors in acute non-variceal upper gastrointestinal bleeding: a meta-analysis. J Gastroenterol Hepatol 2005 Jan; 20 (1): 11–25
Leontiadis GI, Sreedharan A, Dorward S, et al. Systematic review of the clinical effectiveness and cost-effectiveness of proton pump inhibitors in acute upper gastrointestinal bleeding. Health Technol Assess 2007; 11 (51): iii–iiv, 1–164
Barkun A, Bardou M, Marshall JK. Consensus recommendations for managing patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med 2003 Nov 18; 139(10): 843–57
Barkun AN, Herba K, Adam V, et al. High-dose intravenous proton pump inhibition following endoscopic therapy in the acute management of patients with bleeding peptic ulcers in the USA and Canada: a cost-effectiveness analysis. Aliment Pharmacol Ther 2004 Mar 1; 19 (5): 591–600
Lee KKC, You JHS, Wong ICK, et al. Cost-effectiveness analysis of high-dose omeprazole infusion as adjuvant therapy to endoscopic treatment of bleeding peptic ulcer. Gastrointest Endosc 2003 Feb; 57 (2): 160–4
Spiegel BMR, Ofman JJ, Woods K, et al. Minimizing recurrent peptic ulcer hemorrhage after endoscopic hemos-tasis: the cost-effectiveness of competing strategies. Am J Gastroenterol 2003 Jan; 98 (1): 86–97
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Keating, G.M. Intravenous Esomeprazole. Pharmacoeconomics 29, 535–543 (2011). https://doi.org/10.2165/11207430-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11207430-000000000-00000