Abstract
Background
Platelets play a crucial role in the pathogenesis of acute coronary syndromes (ACS). The efficacy of antiplatelet treatment is pivotal in the success of percutaneous coronary intervention (PCI) performed in patients with ACS.
Objective
The aim of the study was to investigate the effects of clopidogrel with or without abciximab on the expression of platelet surface receptors and platelet function in patients with ST-segment elevation myocardial infarction (STEMI) undergoing PCI.
Materials and methods
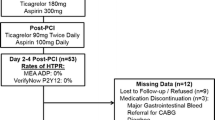
Thirty patients with STEMI were included in the study. During acute primary coronary intervention, patients received aspirin (acetylsalicylic acid) and clopidogrel in a loading dose of 300mg. Clopidogrel was the only antiplatelet therapy used by nine patients (group B). Twenty-one patients (group A) received additional abciximab. Blood samples were collected and analyzed twice: before and up to 22 hours after administration of antiplatelet therapy. The platelet aggregation was established as primary platelet-related hemostasis (closure time [CT] assessed using the PFA100 system). The absolute number of platelet surface antigens as CD41a, CD42a, CD42b, CD61, and CD62P were determined by flow cytometry analysis.
Results
The study revealed a statistically significant increase in CT induced by adenosine diphosphate and adrenaline (epinephrine) +130 seconds (p < 0.0001) and +94 seconds (p < 0.0001), respectively, in group A patients post-therapy. While in group B the parameters of CT did not change after treatment. In addition, the absolute number of CD41a antigens (glycoprotein [GP] IIb/IIIa) increased significantly after treatment in group A. No significant changes were observed after treatment in the expression of CD62P (P-selectin) antigens in either treatment group. There was a significant reduction in the percentage of CD62P-positive platelets in group B after antiplatelet therapy.
Conclusions
The absolute number of GP IIb/IIIa receptors increases and platelets are not activated up to 12 hours after cessation of abciximab therapy. Treatment of STEMI patients undergoing PCI with a loading dose of clopidogrel reduces the percentage of active platelets but does not influence the CT.








Similar content being viewed by others
Notes
The use of trade names is for product identification only and does not imply indorsement.
References
Gurbel PA, O’Connor CM, Cummings CC, et al. Clopidogrel: the future choice for preventing platelet activation during coronary stenting? Pharmacol Res 1999; 40: 107–11.
Caplain H, Donat F, Gaud C, et al. Pharmacokinetics of clopidogrel. Semin Thromb Hemost 1999; 25 Suppl. 2: 25–8.
Gurbel PA, Cummings CC, Bell CR, et al. Onset and extent of platelet inhibition by clopidogrel loading in patients undergoing elective coronary stenting: the Plavix Reduction Of New Thrombus Occurrence (PRONTO) trial. Am Heart J 2003; 145: 239–47.
Cadroy Y, Bossavy J-P, Thalamas C, et al. Early potent antithrombotic effect with combined aspirin and a loading dose of clopidogrel on experimental arterial thrombogenesis in humans. Circulation 2000; 101: 2823–8.
Lepantalo A, Virtanen KS, Heikkila J, et al. Limited early antiplatelet effect of 300mg clopidogrel in patients with aspirin therapy undergoing percutaneous coronary intervention. Eur Heart J 2004; 25: 476–83.
Brener SJ, Barr LA, Burchenal JEB, et al. Randomised, placebo-controlled trial of platelet glycoprotein IIb/IIIa blockade with primary angioplasty for acute myocardial infarction. Circulation 1998; 98: 734–41.
Neumann FJ, Kastrati A, Schmit C, et al. Effect of glycoprotein IIb/IIIa receptor blockade with abciximab on clinical and angiografic restenosis rate after the placement of coronary stents following acute myocardial infarction. J Am Coll Cardiol 2000; 35: 915–21.
Tcheng JE, Kandzari DE, Grines CL, et al. Benefit and risk of abciximab use in primary angioplasty for acute myocardial infarction: the controlled abciximab and device investigation to lower late angioplasty complications (CADILLAC) Trial. Circulation 2003; 108: 1316–23.
de Queiroz Fernandes Araujo JO, Veloso HH, Braga De Paiva JM et al. Efficacy and safety of abciximab on acute myocardial infarction treated with percutaneous coronary interventions: a meta-analysis of randomised, controlled trials. Am Heart J 2004; 148: 937–43.
Silber S, Albertsson P, Aviles FF, et al. Guidelines for percutaneous coronary intervention: the task force for percutaneous coronary interventions of the European Society of Cardiology. Eur Heart J 2005; 26: 804–47.
The RESTORE Investigators. Effects of platelet glycoprotein IIb/IIIa blockade with tirofiban on adverse cardiac events in patients with unstable angina or acute myocardial infarction undergoing coronary angioplasty. Circulation 1997; 96: 1445–53.
Lee DP, Herity NA, Hiatt BL, et al. Adjunctive platelet glycoprotein IIb/IIIa receptor inhibition with tirofiban before primary angioplasty improves aniografic outcomes: results of the TIrofiban Given in the Emergency Room before Primary Angioplasty (TIGER-PA) pilot trial. Circulation 2003; 107: 1497–501.
Rosove MH. Platelet glycoprotein IIb/IIIa inhibitors. Best Pract Res Clin Haematol 2004; 1: 65–76.
Gurbel PA, Malinin AI, Callahan KP, et al. Effect of loading with clopidogrel at the time of coronary stenting on platelet aggregation and glycoprotein IIb/IIIa expression and platelet-leukocyte aggregate formation. Am J Cardiol 2002; 90: 312–5.
Hezard N, Metz D, Nazeyrollas P, et al. Free and total glycoprotein IIb/IIIa measurement in whole blood by quantitative flow cytometry during and after infusion of c7E3 Fab in patients undergoing PTCA. Thrombosis Haemostasis 1999; 81: 869–73.
Matzdorff AC, Kühnel G, Kemkes-Matthes B, et al. Effect of glycoprotein IIb/IIIa inhibitors on CD62P expression, platelet aggregates and microparticles in vitro. J Lab Clin Med 2000; 135: 247–55.
Acknowledgments
This study was financially supported as a statute project of the Institute of Cardiology, Coronary Care Unit in Warsaw, Poland (study number 2.21/III/02). The authors have no conflicts of interest that are directly relevant to the content of this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Professor Ewa Zdebska died unexpectedly on the 28th of July 2007. She was an outstanding Polish Biochemist who worked for many years at the Department of Biochemistry in the Institute of Haematology and Blood Transfusion in Warsaw, Poland. Professor Zdebska had many scientific publications to her credit. Her main research interest was the biochemistry of blood cell membranes with expertise in glycoconjugates. She was involved in the investigation of various glycolization processes of proteins, lipids, and enzymes associated with erythrocytes, leukocytes, and platelets.
Rights and permissions
About this article
Cite this article
Konopka, A., Spychalska, J., Sitkiewicz, D. et al. Expression of Platelet Surface Receptors and Early Changes in Platelet Function in Patients with STEMI Treated with Abciximab and Clopidogrel versus Clopidogrel Alone. Am J Cardiovasc Drugs 7, 433–439 (2007). https://doi.org/10.2165/00129784-200707060-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00129784-200707060-00006