Abstract
Uveitis refers to inflammation involving the uvea or middle coat of the eye. This condition occurs uncommonly, particularly in persons aged ≤16 years. However, pediatric uveitis deserves special consideration for reasons that include the relatively poor prognosis, unique systemic associations, and various age-related treatment considerations.
Accurate diagnosis requires history from both patient and parents, a complete ophthalmic examination that may require general anesthesia, and carefully selected investigations. Infections and masquerade syndromes, such as leukemia and retinoblastoma, must be excluded before treatment is commenced with immunosuppressive agents.
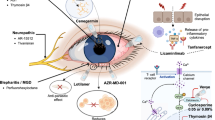
Noninfectious anterior uveitis generally responds to topical corticosteroid and mydriatic therapy. Although used frequently in adults with posterior uveitis, periocular corticosteroid injections may require a general anesthetic, and systemic corticosteroids may cause serious adverse effects, including growth retardation, in pediatric patients. Consequently, in children, one or more corticosteroid-sparing immunosuppressive drugs are usually employed for vision-threatening noninfectious posterior eye inflammation. Methotrexate is the most commonly used systemic immunosuppressive agent for pediatric uveitis. It is effective in small retrospective clinical series, generally well tolerated, easy to administer, and inexpensive. Cyclosporin has also been used successfully in children with uveitis, being associated with a low risk of renal toxicity when used at standard doses. Although prescribed for severe ocular inflammation in adults, alkylating agents are generally contraindicated in children owing to risks including secondary malignancy, sterility and bone marrow suppression. Drugs that inhibit tumor necrosis factor-α have recently been used successfully to treat children with uveitis; however, in some patients there may be a risk of potentiating the ocular inflammation. Randomized clinical trials would provide valuable information about the relative efficacy of the various available treatment options.
Similar content being viewed by others
References
Bloch-Michel E, Nussenblatt RB. International Uveitis Study Group recommendations for the evaluation of intraocular inflammatory disease. Am J Ophthalmol 1987; 103: 234–5
Paivonsalo-Hietanen T, Tuominen J, Saari KM. Uveitis in children: population-based study in Finland. Acta Ophthalmol Scand 2000; 78: 84–8
Darreil RW, Wagener HP, Kurland LT. Epidemiology of uveitis: incidence and prevalence in a small urban community. Arch Ophthalmol 1962; 68: 502–14
Dandona L, Dandona R, John RK, et al. Population based assessment of uveitis in an urban population in Southern India. Br J Ophthalmol 2000; 84: 706–9
Cunningham ET. Uveitis in children. Ocul Immunol Inflamm 2000; 8: 251–61
Shetty AK, Gedalia A. Sarcoidosis: a pediatric perspective. Clin Pediatr 1998; 37: 707–18
Tabbara KH, Chavis PS, Freeman WR. Vogt-Koyanagi-Harada syndrome in children compared to adults. Acta Ophthalmol Scand 1998; 76: 723–6
Rodriguez A, Calonge M, Pedroza-Seres M. Referral patterns of uveitis in a tertiary eye care center. Arch Ophthalmol 1996; 114: 593–9
Stoffel PB, Sauvain MJ, Von Vigier RO, et al. Non-infectious causes of uveitis in 70 Swiss children. Acta Paediatr 2000; 89: 955–8
Pivetti-Pezzi P. Uveitis in children. Eur J Ophthalmol 1996; 6: 293–8
Kanski JJ, Shun-Shun GA. Systemic uveitis syndromes in childhood: an analysis of 340 cases. Ophthalmology 1984; 91: 1247–52
Okada AA, Foster CS. Posterior uveitis in the pediatric population. Int Ophthalmol Clin 1992; 32: 121–52
Rosenbaum JT. Selection and interpretation of laboratory tests for patients with uveitis. Int Ophthalmol Clin 1990; 30: 238–43
Jabs DA, Rosenbaum JT, Foster CS, et al. Guidelines for the use of immunosuppressive drugs in patients with ocular inflammatory disorders: recommendations of an expert panel. Am J Ophthalmol 2000; 130: 492–513
McCombs CC, DeShazo RD. Immune system disorders. In: Speight TM, Holford NHG, editors. Avery’s drug treatment. Auckland: Adis International, 1997: 1295–345
Stanbury RM, Graham EM. Systemic corticosteroid therapy: side effects and their management. Br J Ophthalmol 1998; 82: 704–8
Nussenblatt RB, Palestine AG, editors. Uveitis: fundamentals and clinical practice. Chicago (IL): Year Book Medical Publishers, 1989
BenEzra B, Cohen E. Cataract surgery in children with chronic uveitis. Ophthalmology 2000; 107: 1255–60
Yoshikawa K, Kotake S, Ichiishi A, et al. Posterior sub-tenon injections of repository corticosteroids in uveitis patients with cystoid macular edema. Jpn J Ophthalmol 1995; 39: 71–6
Riordan-Eva P, Lightman S. Orbital floor steroid injections in the treatment of uveitis. Eye 1994; 8: 66–9
Freeman G. Cystoid macular oedema in uveitis: an unresolved problem. Eye 2001; 15: 12–7
O’Connor GR. Periocular corticosteroid injections: uses and abuses. Eye, Ear, Nose Throat J 1976; 55(2): 26–33
Smith JR, George RK, Rosenbaum JT. Lower lid herniation of orbital fat may complicate periocular corticosteroid injection. Am J Opthalmol. In press
Anglade E, Whitcup SM. The diagnosis and management of uveitis. Drugs 1995; 49: 213–23
Dick AD, Azim M, Forrester JV. Immunosuppressive therapy for chronic uveitis: optimising therapy with steroids and cyclosporin A. Br J Ophthalmol 1997; 81: 1107–12
Smith JR, Rosenbaum JT. Management of immune-mediated uveitis. Biodrugs 2000; 13: 9–20
Wakefield D, McCluskey P, Penny R. Intravenous pulse methylprednisolone therapy in severe inflammatory eye disease. Arch Ophthalmol 1986; 104: 847–51
Hemady R, Tauber J, Foster CS. Immunosuppressive drugs in immune and inflammatory ocular disease. Surv Ophthalmol 1991; 35: 369–85
Cassidy JT. Medical management of children with juvenile rheumatoid arthritis. Drugs 1999; 58: 831–50
Weiss AH, Wallace CA, Sherry DD. Methotrexate for resistant chronic uveitis in children with juvenile rheumatoid arthritis. J Pediatr 1998; 133: 266–8
Shetty AK, Zganjar BE, Ellis GS, et al. Low-dose methotrexate in the treatment of severe juvenile rheumatoid arthritis and sarcoid iritis. J Pediatr Ophthalmol Strabismus 1999; 36: 125–8
Hemady RK, Baer JC, Foster CS. Immunosuppressive drugs in the management of progressive, corticosteroid-resistant uveitis associated with juvenile rheumatoid arthritis. Int Ophthalmol Clin 1992; 32: 241–52
Foster CS, Barrett F. Cataract development and cataract surgery in patients with juvenile rheumatoid arthritis-associated iridocyclitis. Ophthalmology 1993; 100: 809–17
Gion N, Stavrou P, Foster CS. Immunomodulatory therapy for chronic tubulo-interstitial nephritis-associated uveitis. Am J Ophthalmol 2000; 129: 764–8
Kremer JM, Alarcon GS, Lightfoot RW, et al. Methotrexate for rheumatoid arthritis: suggested guidelines for monitoring liver toxicity. Arthritis Rheum 1994; 37: 316–28
Larkin G, Lightman S. Mycophenolate mofetil: a useful immunosuppressive in inflammatory eye disease. Ophthalmology 1999; 106: 370–4
Kilmartin DJ, Fletcher ZJ, Almeida JA, et al. CD69 expression on peripheral CD4+ T cells parallels disease activity and is reduced by mycophenolate mofetil therapy in uveitis. Invest Ophthalmol Vis Sci 2001; 42: 1285–92
Palmer RG, Kanski JJ, Ansell BM. Chlorambucil in the treatment of intractable uveitis associated with juvenile chronic arthritis. J Rheumatol 1985; 12: 967–70
Godfrey WA, Epstein WV, O’Connor GR, et al. The use of chlorambucil in intractable idiopathic uveitis. Am J Ophthalmol 1974; 78: 415–28
Mehra R, Moore TL, Catalano D, et al. Chlorambucil in the treatment of iridocyclitis in juvenile rheumatoid arthritis. J Rheumatol 1981; 8: 141–4
Kilmartin DJ, Forrester JV, Dick AD. Cyclosporin A therapy in refractory noninfectious childhood uveitis. Br J Ophthalmol 1998; 82: 737–42
Walton RC, Nussenblatt RB, Whitcup SM. Cyclosporine therapy for severe sight-threatening uveitis in children and adolescents. Ophthalmology 1998; 105: 2028–34
De Vos AF, Van Haren MA, Verhagen C, et al. Kinetics of intraocular tumor necrosis factor and interleukin-6 in endotoxin-induced uveitis. Invest Ophthalmol Vis Sci 1994; 35: 1100–6
Planck SR, Huang X-N, Robertson JE, et al. Cytokine mRNA levels in rat tissues after systemic endotoxin treatment. Invest Ophthalmol Vis Sci 1994; 35: 924–30
Smith JR, Hart PH, Coster DJ, et al. Mice deficient in TNFR p55 and p75, IL-4 or iNOS are susceptible to endotoxin-induced uveitis. Invest Ophthalmol Vis Sci 1998; 39: 658–61
Lovell DJ, Giannini EH, Reiff A, et al. Etanercept in children with polyarticular juvenile rheumatoid arthritis. Pediatric Rheumatology Collaborative Study Group. N Engl J Med 2000; 342: 763–9
Van den Bosch F, Kruithof E, Baeten D, et al. Effects of a loading dose regimen of three infusions of chimeric monoclonal antibody to tumour necrosis factor alpha (infliximab) in spondyloarthropathy: an open pilot study. Ann Rheum Dis 2000; 59: 428–33
Targan SR, Hanauer SB, van Deventer SJ, et al. A short-term study of chimeric monoclonal antibody cA2 to tumor necrosis factor alpha for Crohn’s disease. N Engl J Med 1997; 37: 1029–35
Mikuls TR, Moreland LW. TNF blockade in the treatment of rheumatoid arthritis: infliximab versus etanercept. Expert Opin Pharmacother 2001; 2: 75–84
Reiff A, Takei S, Sadeghi S, et al. Etanercept therapy in children with treatment-resistant uveitis. Arthritis Rheum 2001; 44: 1411–5
Smith JR, Levinson RD, Holland GN, et al. Differential efficacy of tumor necrosis factor inhibition in the management of inflammatory eye disease and associated rheumatic disease. Arthritis Rheum 2001; 45: 252–7
Brooks PM. NSAIDs. In: Klippel JH, Dieppe PA, editors. Rheumatology. 2nd ed. London: Mosby, 1998: 3.5.1–6
Nguyen QD, Foster CS. Saving the vision of children with juvenile rheumatoid arthritis-associated uveitis. JAMA 1998; 280: 1133–4
Olson NY, Lindsley CB, Godfrey WA. Nonsteroidal anti-inflammatory drug therapy in chronic childhood iridocyclitis. Am J Dis Child 1988; 142: 1289–92
Sand BB, Krogh E. Topical indomethacin, a prostaglandin inhibitor, in acute anterior uveitis: a controlled clinical trial of non-steroid versus steroid anti-inflammatory treatment. Acta Ophthalmol 1991; 69: 145–8
Acknowledgements
The preparation of this manuscript was supported in part by a Career Development Award from Research to Prevent Blindness. The author was a co-investigator on studies with Centocor (to investigate infliximab for the treatment of uveitis) and Buasch and Lomb (to investigate fluocinolone acetonide implants for the treatment of uveitis).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smith, J.R. Management of Uveitis in Pediatric Patients. Pediatr-Drugs 4, 183–189 (2002). https://doi.org/10.2165/00128072-200204030-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00128072-200204030-00005