Abstract
Although process measures of care have traditionally been used to assess the quality of healthcare, there is little evidence, for the majority of healthcare activities, to support a clear relationship between processes of care and resulting health gains. Outcomes monitoring is increasingly being advocated as a vital component of healthcare, particularly with the increasingly aging population. A consensus is emerging that routine systems of outcome monitoring are fundamental to rational clinical decision-making and public policy.
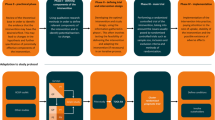
There are several issues that need to be considered when implementing a routine system of outcome monitoring; this article addresses these issues in older people within a UK community setting in the context of an innovative observational feasibility study (The North East Fife Outcomes Project). This project (i) determined which outcomes of health and social care are the most important to this patient group; and (ii) identified appropriate measures for relevant outcomes suitable for use in a community setting. Key patient characteristics and relevant clinical and social care process variables were then recorded, concomitant variables such as disease severity and comorbidities were taken into account and quality-of-life assessment measures recorded. For the success of any outcomes monitoring system, feedback to end-users is important. The North East Fife Project will assess the feasibility and value of feedback at the individual patient level and at the aggregate level.
More research, particularly from large observational studies, is needed to address reliability and validity issues, biases and inaccuracies with routinely collected data and to further determine the value of routine outcomes monitoring.




Similar content being viewed by others
References
Kennedy JW. Streptokinase for the treatment of acute myocardial infarction: a brief review of randomized trials. J Am Coll Cardiol 1987; 10 Suppl. 5 B: 28B–32B
Honan MB, Harrell FE, Reimer KA, et al. Cardiac rupture, mortality and the timing of thrombolytic therapy: a meta-analysis. J Am Coll Cardiol 1990; 16(2): 359–67
Treurniet HF, Essink-Bot M-L, Mackenbach JP, et al. Health-related quality of life: an indicator of quality of care? Qual Life Res 1997; 6: 363–9
Mooney G. Economics, medicine and health care. London: Harvester Wheatsheaf, 1992: 179
Gray A. Rationing and choice. In: B Davey, J Popay, editors. Dilemmas in health care. Milton Keynes: The Open University Press, 1993: 27–42
Department of Health (DoH). The new NHS modern dependable: a national framework for assessing performance. London: NHS Executive, 1998
Hennekens CH, Buring JE. Observational evidence: doing more good than harm — the evaluation of health care interventions. Ann NY Acad Sci 1994; 703: 22
Bowling A. The most important things in life — comparisons between older and younger population age groups by gender: results from a national survey of the public’s judgements. Int J Health Sciences 1995; 6(4): 169–75
Bowling A. What things are important in people’s lives? A survey of the public’s judgements to inform scales of health related quality of life. Soc Sci Med 1995; 41(10): 1447–62
Farquhar M. Elderly people’s definitions of quality of life. Soc Sci Med 1995; 41(10): 1439–46
Mahoney FI, Barthel DW. Functional evaluation: the Barthel index. Rehabilitation 1965: 61-5
Kahn RL, Goldfarb AI, Pollack M, et al. Brief objective measures for the determination of mental status in the aged. Am J Psychiatry 1960; 117: 326–8
Parkerson Jr GR, Broadhead WE, Tse C-KJ. The duke health profile: a 17-item measure of health and dysfunction. Med Care 1990; 28(11): 1056–69
Sherbourne CD, Stewart AL. The MOS social support survey. Soc Sci Med 1991; 32(6): 705–14
Hays RD, DiMatteo R. A short-form measure of loneliness. J Perspect Assess 1987; 51(1): 69–81
Downie WW, Leatham PA, Rhind VM, et al. Studies with pain rating scales. Ann Rheum Dis 1978; 37: 378–81
Horn SD, Buckle JM, Carver CM. Ambulatory severity index: development of an ambulatory case mix system. J Ambulatory Care Manage 1988; 11(4): 53–62
Greenfield S, Sullivan L, Dukes KA, et al. Development and testing of a new measure of case-mix for use in office practice. Med Care 1995; 33(4): AS47–AS55
Parkerson Jr GR, Broadhead E, Tse C-KJ. The Duke Severity of Illness Checklist (DUSOI) for measurement of severity and comorbidity. J Clin Epidemiol 1993; 46(4): 379–93
Eccles M, Steen N, Hutchinson A, et al. Severity measurement using a generic instrument. Eur J Public Health 1997; 7: 205–9
Havlik RJ, Yancik R, Long S, et al. The National Institute on Aging and the National Cancer Institute SEER collaborative study on comorbidity and early diagnosis of cancer in the elderly. Cancer 1994; 74(7): 2101–6
Newschaffer CJ, Bush TL, Penberthy LT. Comorbidity measurement in elderly female breast cancer patients with administrative and medical records data. J Clin Epidemiol 1997; 50(6): 725–33
Yancik R, Havlik RJ, Wesley MN, et al. Cancer and comorbidity in older patients: a descriptive profile. Ann Epidemiol 1996; 6(5): 399–412
Shah S, Vanclay F, Cooper B. Improving the sensitivity of the Barthel index for stroke rehabilitation. J Clin Epidemiol 1989; 42(8): 703–9
Lazar RB, Yarkoney GM, Ortolano D. Prediction of functional outcome by motor capability after spinal cord injury. Arch Phys Med Rehab 1989; 70: 819–22
Crombie IK, Davies HTO. Beyond health outcomes: the advantages of measuring process. J Eval Clin Pract 1998; 4: 31–8
Davies HTO, Crombie IK. Interpreting health outcomes. J Eval Clin Pract 1997; 4: 187–200
Naylor CD, Guyatt GH. Users’ guides to the medical literature: how to use an article reporting variations in the outcomes of health services. JAMA 1996; 275: 554–8
Acknowledgements
We gratefully acknowledge the help of all health and social work professionals and older people who participated in this study. The 3 year long outcomes project is funded by Perth & Kinross Healthcare Trust. We are also grateful for the helpful comments made by 2 anonymous referees on an earlier draft of this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kliempt, P., Ruta, D. Monitoring Outcomes of Care in Older People in a UK Community Setting. Dis-Manage-Health-Outcomes 7, 39–47 (2000). https://doi.org/10.2165/00115677-200007010-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00115677-200007010-00005