Summary
There is no specific treatment for terminal liver failure apart from liver transplantation. Fulminant hepatitis is the most acute expression of liver failure. Transplantation for fulminant hepatitis has its limits: 15% of patients die, principally of cerebral oedema, before transplantation can be performed, and the survival rate after transplantation is lower than that after chronic liver disease, principally because of poorer patient status and emergency use of ABO-incompatible or steatotic grafts. There is therefore a need for treatment that will slow the evolution of the hepatitis and control the cerebral oedema in patients awaiting liver transplantation.
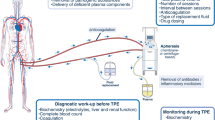
Artificial liver support systems derived from artificial kidneys have not proven suitable and bioartificial matrixes containing hepatocytes are under development. The systems under development are based upon extracorporeal circulation of the patients’s blood, or plasma, across a capillary filter containing hepatocytes in the extracapillary spaces. The hepatocytes may be human, originating from a hepatoblastoma tumour cell line, since culture of normal human hepatocytes is not yet possible, or they may be porcine. In the plasmapheresis system used at our hospital as an investigational protocol, plasma isolated from the patient is passed first across a carbon filter, and then through a capillary filter where the extracapillary spaces contain porcine hepatocytes on a matrix of dextran and collagen fibres, before being returned to the patient. In our centre, 8 patients have had 1 to 3 sessions of 6 hours each on the artificial liver while awaiting liver transplantation. Improvement in neurological status was the most significant change noted during the treatment, which was well tolerated. All patients could be transplanted; 1 died during the immediate postoperative course and another of sepsis 7 months after the operation.
In conclusion, the artificial liver support systems presently under development utilise pig hepatocytes in the extracapillary space of a semipermeable membrane. Preliminary results are encouraging, and future improvements in these systems will doubtless lead to wider applications in liver failure.
Similar content being viewed by others
Références
Bismuth H, Samuel D, Castaing D, et al. Orthotopic liver transplantation in fulminant and subfulminant hepatitis. The Paul Brousse experience. Ann Surg 1995; 222: 109–19
Farges O, Kalil A, Samuel D, et al. The use of ABO-incompatible grafts in liver transplantation: a life saving procedure in highly selected patients. Transplantation 1995; 59: 1124–33
Adam R, Reynes M, Johann M, et al. The outcome of steatotic grafts in liver transplantation. Transplant Proc 1991; 23: 1538–40
Chari RS, Collins BH, Magee JC, et al. Brief report: treatment of hepatic failure with ex vivo pig-liver perfusion followed by liver transplantation. N Engl J Med 1994; 331(4): 234–7
Sussman NL, Chong MG, Koyssayer T, et al. Reversal of fulminant hepatic failure using an extracorporeal liver assist device. Hepatology 1992; 16: 60–5
Rozga J, Williams F, Ro MS, et al. Development of a bioartificial liver: properties and function of a hollow-fiber module inoculated with liver cells. Hepatology 1993; 17: 258–65
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Samuel, D. Les systèmes de support hépatique artificiels. BioDrugs 8 (Suppl 1), 26–28 (1997). https://doi.org/10.2165/00063030-199700081-00011
Published:
Issue Date:
DOI: https://doi.org/10.2165/00063030-199700081-00011