Summary
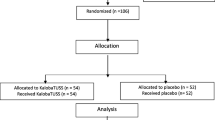
In a double-blind, randomised, clinical trial involving 191 elderly patients of either gender affected by nonproductive cough, the therapeutic efficacy and tolerability of oral levodropropizine and Clobutinol (60mg three times daily for 3 days, for both agents) were evaluated. Efficacy was assessed by analysing cough intensity, the number of coughing spells in the 5 hours post-treatment, and night awakenings due to cough; tolerability was evaluated by analysing laboratory data, vital signs, dyspnoea and any adverse event occurring during the clinical trial, including the presence or absence of somnolence.
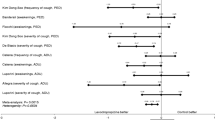
Independent of the underlying pathology, cough intensity was significantly (p < 0.01) reduced by both drugs at the end of the treatment period; moreover, the number of coughing spells was significantly (p < 0.01) reduced by both drugs after the first day of treatment. In addition to the relief of cough, the number of night awakenings was significantly decreased (p < 0.01) by both treatments. No changes in laboratory data were considered clinically relevant; vital signs were not clinically affected by either study drug. Mild somnolence was reported for a low percentage of patients (< 15%) with both drugs; the percentage of patients experiencing this adverse effect was about 50% lower with levodropropizine (6.5%) than with Clobutinol (14.6%), although this difference was not statistically significant. Dyspnoea also improved throughout the treatment period.
These data indicate that both levodropropizine and Clobutinol have antitussive efficacy and are free of bronchopulmonary adverse effects in elderly patients, although a central effect such as somnolence was experienced with a certain frequency, especially with Clobutinol.
Similar content being viewed by others
References
National Health Survey. Vital and Health Statistics. Office visits to internists: The National ambulatory medical care survey. United States 1975, Series 13, No. 36, Department of Health, Education and Welfare Publication No. 79-1786 (Public Health Service) 1978; 4–29
Irwin RS, Curley FJ, Bennet FM. Appropriate use of antitussives and protussives. A practical review. Drugs 1993; 46: 80–91
Zervanos NJ, Shute KM. Acute, dysruptive cough. Postgrad Med 1994; 95: 153–68
Daffonchio L, Clavenna G, Fedele G, et al. Levodropropizine. Drugs Today 1995; 31: 299–305
Guffanti EE. Drugs with direct peripheral action. In: Braga PC, Allegra L, editors. Cough. New York: Raven Press, 1989: 198–214
Shams H, Daffonchio L, Scheid P. Effects of levodropropizine on vagal afferent C-fibres in the cat. Br J Pharmacol 1996; 117: 853–8
Bossi R, Braga PC, Centanni S, et al. Antitussive activity and respiratory system effects of levodropropizine in man. Arzneimittel Forschung 1988; 38: 1159–62
Clobutinol hydrochloride. In: Reynolds JEF, editor. Martindale. The Extra Pharmacopoeia. London: The Royal Pharmaceutical Society, 31st edition, 1996: 1065
Guffanti EE. Centrally acting nonopioid drugs. In: Braga PC, Allegra L, editors. Cough. New York: Raven Press, 1989: 167–77
Banner AS. Cough: physiology, evaluation and treatment. Lung 1986; 164: 79–92
Yoshida S, Hukushima Y, Kitamura S, et al. Antitussive effect of 1-p-chlorophenyl-2,3-dimethyl-4-dimethylaminobutanol-(2)-hydrochloride. Arzneimittel Forschung 1967; 17: 1515–8
Bickerman HA. Antitussive drugs. In: Modell W, editor. Drugs of choice. St Louis, Mo: The C.V. Mosby Co., 1969: 419–32
Manning HL, Schwartzstein RM. Pathophysiology of dyspnea. N Engl J Med 1995; 333: 1547–53
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Pontiroli, A.E., Daffonchio, L. Efficacy and Tolerability of Levodropropizine and Clobutinol in Elderly Patients with Nonproductive Cough. Clin. Drug Invest. 14, 175–182 (1997). https://doi.org/10.2165/00044011-199714030-00003
Published:
Issue Date:
DOI: https://doi.org/10.2165/00044011-199714030-00003