Abstract
Background
Invasive fungal infections in neutropenic patients treated for haematological malignancies are associated with a high mortality rate and, therefore, require early treatment. As the diagnosis of invasive fungal infections is difficult, effective antifungal prophylaxis is desirable. So far, fluconazole has been the most commonly used.
Objective
To assess the cost effectiveness of itraconazole compared with both fluconazole and no prophylaxis for the prevention of invasive fungal infections in haematological patients, mean age 51 years, in Germany and The Netherlands.
Study design
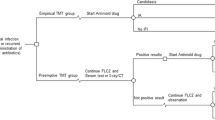
We designed a probabilistic decision model to fully incorporate the uncertainty associated with the risk estimates of acquiring an invasive fungal infection. These risk estimates were extracted from two meta-analyses, evaluating the effectiveness of fluconazole and itraconazole and no prophylaxis. The perspective of the analysis was that of the healthcare sector; only medical costs were taken into account. All costs were reported in €, year 2004 values.
Cost effectiveness was expressed as net costs per invasive fungal infection averted. No discounting was performed, as the model followed patients during their neutropenic period, which was assumed to be less than 1 year.
Results
According to our probabilistic decision model, the monetary benefits of averted healthcare exceed the costs of itraconazole prophylaxis under baseline assumptions (95% CI: from cost-saving to €5000 per invasive fungal infection averted). Compared with fluconazole, itraconazole is estimated to be both more effective and more economically favourable, with a probability of almost 98%.
Conclusions
In specific groups of neutropenic patients treated for haematological malignancies, itraconazole prophylaxis could potentially reduce overall healthcare expenditure, without harming effectiveness, in settings where fluconazole is common practice in the prophylaxis of invasive fungal infections.








Similar content being viewed by others
Notes
The use of trade names is for product identification purposes only and does not imply endorsement.
References
McNeil MM, Nash SL, Hajjeh RA, et al. Trends in mortality due to invasive mycotic diseases in the United States, 1980–1997. Clin Infect Dis 2001; 33: 641–647
Garber G. An overview of fungal infections. Drugs 2001; 61 Suppl. 1: 1–12
Prentice HG, Kibbler CC, Prentice AG. Towards a targeted, risk-based, antifungal strategy in neutropenic patients. Br J Haematol 2000; 100: 273–284
Uzun O, Anaisse EJ. Antifungal prophylaxis in patients with hematologic malignancies: a reappraisal. Blood 1995; 86: 2063–2072
Lin SJ, Schranz J, Teutsch SM. Aspergillosis case-fatality rate: systematic review of the literature. Clin Infect Dis 2001; 32: 358–366
Rinaldi MG. Problems in the diagnosis of invasive fungal diseases. Rev Infect Dis 1991; 13: 493–495
Kanda Y, Yamamoto R, Chizuka A, et al. Prophylactic action of oral fluconazole against fungal infection of neutropenic patients: a meta-analysis of 16 randomized, controlled trials. Cancer 2000; 89: 1611–1625
Glasmacher A, Prentice A, Gorschliiter M, et al. Itraconazole prevents invasive fungal infections in neutropenic patients treated for hematologic malignancies: evidence from a metaanalysis of3,597 patients. J Clin Oncol 2003; 21 (24): 4615–4626
Sutton AJ, Abrams KR, Jones DR, et al. Methods for meta-analysis in medical research. Chichester: John Wiley & Sons Ltd, 2000
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials 1986; 7: 177–188
Goodman JL, Winston DJ, Greenfield RA, et al. A controlled trial of fluconazole to prevent fungal infections in patients undergoing bone marrow transplantation. N Engl J Med 1992; 326: 845–851
Winston DJ, Chandrasekar PH, Lazarus HM, et al. Fluconazole prophylaxis of fungal infections in patients with acute leukemia: results of a randomized placebo-controlled, double blind, multi-center trial. Ann Intern Med 1993; 118: 495–503
Chandrasekar PH, Gatny CM. Effect of fluconazole prophylaxis on fever and use of amphotericin in neutropenic cancer patients: the Bone Marrow Transplantation Team. Chemotherapy 1994; 40: 136–143
Chandrasekar PH, Gathy CM. The effect of fluconazole prophylaxis on fungal colonization in neutropenic cancer patients: the Bone Marrow Transplantation Team. J Antimicrob Chemother 1994; 33: 309–318
Schafftier A, Schaffner M. Effect of prophylactic fluconazole on the frequency of fungal infections, amphotericin B use, and health care costs in patients undergoing intensive chemotherapy for hematologic neoplasias. J Infect Dis 1995; 172: 1035–1041
Slavin MA, Osborne B, Adams R, et al. Efficacy and safety of fluconazole prophylaxis for fungal infections after bone marrow transplantation: a prospective, randomised, double-blind study. J Infect Dis 1995; 171: 1545–1552
Kern W, Behre G, Rudolf T, et al. Failure of fluconazole prophylaxis to reduce mortality or the requirement of systemic amphotericin B therapy during treatment for refractory acute myeloid leukemia. Cancer 1998; 83: 289–301
Rotstein C, Bow EJ, Laverdiere M, et al. Randomized placebo-controlled trial of fluconazole prophylaxis for neutropenic cancer patients: benefit based on purpose and intensity of cytotoxic therapy. Clin Infect Dis 1999; 28: 331–340
Altaian DG. Practical statistics for medical research. Boca Raton (FL): CRC Press, 1999
Winston DJ, Maziarz RT, Chandrasekar PH, et al. Intravenous and oral itraconazole versus intravenous and oral fluconazole for long-term antifungal prophylaxis in allogeneic hematopoietic stem-cell transplant recipients: a multicenter, randomized trial. Ann Intern Med 2003; 138: 705–713
Marr KA, Crippa F, Leisenring W. Itraconazole versus fluconazole for prevention of fungal infections in patients receiving allogeneic stem cell transplants. Transplantation 2004; 103 (4): 1527–1533
Glasmacher A, Cornely O, Ullman AJ. An open-label randomized trial comparing itraconazole oral solution with fluconazole oral solution for primary prophylaxis of fungal infections in patents with haematological malignancy and profound neutropenia. J Antimicrob Chemother 2006; 57: 317–325
Prismant: National LMR information [online and further data specifically requested]. Available from URL: http://cognosserver.prismant.nl/cognos7/cgi-bin/ppdscgi.cgi?DC=Q&E=/Prisma-Landelijke-LMR/Landelij ke+LMR-informatie+-+Diagnosen [Accessed 2006 Jul 01]
Health Care Insurance Board. Dutch pharmacoeconomic guidelines 2004 [in Dutch]. Amstelveen: Health Care Insurance Board, 2003 [online]. Available from URL: http://www.fk.cvz.nl [Accessed 2006 Jul 01]
Oosterink JB, Bouwmans CAM, Koopmanschap MA, et al. Guideline for costing research, methods and standardized prices for economic evaluations in health care. Diemen: Health Care Insurance Board, 2004
Neilson AR, Moerer O, Burchardi H, et al. A new concept for DRG-based reimbursement of services in German intensive care units: results of a pilot study. Intensive Care Med 2004; 30 (6): 1220–1223
Landesamt fur Datenverarbeitung und Statistik Nordrhein-Westfalen [online]. Available from URL: http://www.lds.nrw.de/presse/pressemitteilungen/2005/pres_020_05.html [Accessed 2006 Jul 01]
Rote Liste®: arzneimittelinformationen fur Deutschland [online]. Available from URL: http://www.rote-liste.de [Accessed 2006 Jul 01]
Arztkosten [online]. Available from URL: http://www.e-bis.de/goae/defaultFrame.htm [Accessed 2006 Jul 01]
Briggs AH. Handling uncertainty in cost-effectiveness models. Pharmacoeconomics 2000; 17 (5): 479–500
Black WC. The CE plane: a graphic representation of cost-effectiveness. Med Decis Making 1990; 10 (3): 212–214
Bos JM, Postma MJ. Using pharmacoeconomics for policy making: is rational decision making enhanced by applying thresholds for cost-effectiveness? Expert Rev Pharmacoeconomics Outcomes Res 2004; 4 (3): 247–250
Wilson LS, Reyes CM, Stolpman M, et al. The direct cost and incidence of systematic fungal infections. Value Health 2002; 5 (1): 26–34
Torfs K. Economic aspects of treatment for fungal infections in cancer patients. Eur J Microbiol Infect Dis 1997; 16: 98–107
Menzin J, Lang KM, Friedman M, et al. Excess mortality, length of stay, and costs associated with serious fungal infections among elderly cancer patients: findings from linked SEER-Medicare data. Value Health 2005; 8 (2): 140–148
Gotzsche PC, Johansen HK. Meta-analysis of prophylactic or empirical antifungal treatment versus placebo or no treatment in patients with cancer complicated by neutropenia. BMJ 1997; 314: 1238–1244
Rentz AM, Halpern MT, Bowden R. The impact of candidemia on length of hospital stay, outcome, and overall cost of illness. Clin Infect Dis 1998; 27: 781–788
Jansen JP, Meis JF, Blijlevens NM, et al. Economic evaluation of voriconazole in the treatment of invasive fungal infections in the Netherlands. Curr Med Res Opin 2005; 12 (10): 1535–1546
Acknowledgements
This study was supported by a grant from Ortho Biotech. The co-authors from Ortho Biotech had an important contribution in conceiving and planning the project and in specific tasks (e.g. disseminating the questionnaire). The sponsor had no role in the data analysis and interpretation of the results. The authors from academic institutions retained the right to publish the data regardless of the outcomes. The sponsor did comment on various versions of the manuscripts, including the final version. Axel Glasmacher and Archie Prentice have previously received grants, honoraria and/or consultancy fees from Ortho Biotech and Pfizer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Vries, R., Daenen, S., Tolley, K. et al. Cost Effectiveness of Itraconazole in the Prophylaxis of Invasive Fungal Infections. Pharmacoeconomics 26, 75–90 (2008). https://doi.org/10.2165/00019053-200826010-00007
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200826010-00007