Abstract
Background
There is limited previous research examining the healthcare costs of neovascular age-related macular degeneration (NV-AMD), which constrains our understanding of the economic impact of this condition. With aging populations, this leading cause of rapid vision loss in Western countries is expected to become a pressing health predicament, requiring decision makers to evaluate alternative treatment strategies for AMD.
Objective
To document the economic burden of bilateral NV-AMD, the late stage of AMD, in elderly patients, from a societal perspective.
Study design, setting and participants: A cross-sectional, observational study surveyed 401 patients with bilateral NV-AMD and 471 non-AMD subjects in Canada, France, Germany, Spain and the UK. Physicians’ records and subjects’ standardized telephone interviews were used to record medical resource utilization, assistance with daily living and social benefits. Annual bilateral NV-AMDrelated socioeconomic costs were calculated in €, year 2005 values. Main outcome measures: Societal costs including direct vision-related medical costs (e.g. treatment of AMD and vision-related equipment), direct non-vision-related medical costs (e.g. medications) and direct non-medical-related costs (e.g. home healthcare and social services) were the main outcome measures.
Results
The demographic profile of NV-AMD patients was similar across countries; however, co-morbid condition profiles varied. NV-AMD patients reported substantial health-related problems and associated health resource utilization (HRU). In the previous 12 months, 12–22% of patients fell, and half of these patients required medical treatments. More than 20% (range 21–59%) of patients were prescribed vision-enhancing equipment. More than half of the patients (54–81%) were living with a spouse or family member and 19–41% reported receiving assistance for activities of daily living.
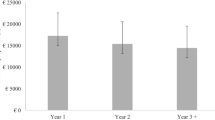
The average annual societal cost per bilateral NV-AMD patient treated was estimated to be €7879 in Canada, €7349 in France, €12 445 in Germany, €5732 in Spain and €5300 in the UK, and direct vision-related medical costs accounted for 23–63% of the total cost. Half of the patients were diagnosed with bilateral NV-AMD for <1 year, with an average length of 5 months; there were no statistically significant differences in total annual costs per patient between these patients and those who were diagnosed with bilateral disease for ≥1 year. Estimated annual societal costs of bilateral NV-AMD patients in these countries ranged from €268 to €1311 million. Estimated annual societal costs of all NV-AMD patients in these countries ranged from €671 to €3278 million.
Conclusions
Bilateral NV-AMD imposes significant functional impairment on patients, leading to increased HRU and a high societal cost burden. Differences in national healthcare systems and NV-AMD treatment patterns were reflected in the wide variation of NV-AMD costs across the five surveyed countries. Even though the prevalence rates and per-patient costs varied by country, the societal costs of NV-AMD patients were substantial in each country. Earlier intervention with effective therapies is expected to reduce disease burden and disability associated with NV-AMD and, thus, decrease the overall societal cost.








Similar content being viewed by others
References
Ambati J, Ambati BK, Yoo SH, et al. Age-related macular degeneration: etiology, pathogenesis, and therapeutic strategies. Surv Ophthalmol 2003 May-Jun; 48 (3): 257–293
Verma L, Das T, Binder S, et al. New approaches in the management of choroidal neovascular membrane in age-related macular degeneration. Indian J Ophthalmol 2000 Dec; 48 (4): 263–278
Desai M, Pratt LA, Lentzner H, et al Trends in vision and hearing among older Americans: aging trends no. 2. Hyatts-ville (MD): National Center for Health Statistics, 2001
Dargent-Molina P, Favier F, Grandjean H, et al. Fall-related factors and risk of hip fracture: the EPIDOS prospective study. Lancet 1996 Jul 20; 348 (9021): 145–149
Lee HK, Scudds RJ. Comparison of balance in older people with and without visual impairment. Age Ageing 2003 Nov; 32 (6): 643–649
Ivers RQ, Cumming RG, Mitchell P, et al. Visual impairment and falls in older adults: the Blue Mountain Eye Study. J Am Geriatr Soc 1998 Jan; 46 (1): 58–64
Bonastre J, Le Pen C, Soubrane G, et al. The burden of age-related macular degeneration: results of a cohort study in two French referral centres. Pharmacoeconomics 2003; 21 (3): 181–190
Sharma S, Bakal J, Brown G, et al. Economic resources utilized in a cohort of patients with age-related macular degeneration [abstract no. 1410]. Annual Meeting of the Association for Research in Vision and Ophthalmology; 2004 Apr 25-29; Fort Lauderdale (FL)
Rizzo JA, Friedkin R, Williams CS, et al. Health care utilization and costs in a Medicare population by fall status. Med Care 1998 Aug; 36 (8): 1174–1188
Schmier JK, Jones ML, Halpern MT. The burden of age-related macular degeneration. Pharmacoeconomics 2006; 24 (4): 319–334
Soubrane G, Cruess A, Lotery A, et al. Burden and resource utilization of neovascular AMD: findings of a multicountry study. Arch Ophthalmol 2007; 125 (9): 1249–1254
Organisation for Economic Co-operation and Development (OECD). Purchasing power parities (PPP) [online]. Available from URL: http://www.oecd.org/document/47/0,2340,en_2649_34357_36202863_l_l_l_l,00.html [Accessed 2006 Jan 31]
French National Authority for Health. Common classification for medical services. Version 2, 2005 [online]. Available from URL: http://www.ccam.sante.fr/ [Accessed 2006 Jan 27]
National Association of Sickness Fund Physicians. Uniform value scale (2005) [online]. Available from URL: http://www.kbv.de/ebm2000plus/EBMGesamt.htm [Accessed 2004 Oct 28]
Canadian Institute for Health and Information. Analysis of 2003 data from the Canadian MIS Database (CMDB) [online]. Available from URL: http://secure.cihi.ca/cihiweb/dispPage.jsp?cw_page=spend_canmis_e [Accessed 2006 May 17]
Centre for Studies in Health Economics and Social Policy (Centre d’Estudis En Economia’ e La Salut I De La Politic a Social SL, SOIKOS). Database for Spanish Health Costs. Version 2.2 [database on CD-ROM]. Barcelona: SOIKOS, 2005
Curtis L, Netten A. Unit costs of health and social services 2004. Kent: Personal Social Services Research Unit (PSSRU), University of Kent, 2004
Technical Agency for Information on Hospitalization. Program of medicalization of information systems, 2005 [online]. Available from URL: https://www.epmsi.atih.sante.fr/ [Accessed 2006 Jan 27]
University Clinic, Miinster, Westphalia Wilhelms University Minister. German Diagnosis-Related Group Webgrouper 2005 [online]. Available from URL: http://drg.uni-muenster.de/index.html [Accessed 2005 Oct 28]
Ministry of Health and Long-Term Care. Ontario drug benefit formulary/comparative drug index, edition 38, 2004 [online]. Available from URL: http://www.health.gov.on.ca/english/providers/program/drugs/odbf_mn.html [Accessed 2005 Jun 14]
Vidal, 2005 [online]. Available from URL: http://www.vidalpro.net [Accessed 2006 Jan]
Rote Liste, 2005 [online]. Available from URL: http://www.rote-liste.de [Accessed 2005 Oct 28]
British National Formulary 2005 (BNF). Available from URL: http://www.bnf.org [Accessed 2005 Jul 1]
Mattson Jack Group. Epidemiology of age-related macular degeneration. St Louis (MO): Mattson Jack Group, 2003. (Data on file)
Augood CA, Vingerling JR, de Jong PT, et al. Prevalence of age-related maculopathy in older Europeans: the European Eye Study (EUREYE). Arch Ophthalmol 2006 Apr; 124 (94): 529–535
Wang JJ, Mitchell P, Smith W, et al. Bilateral involvement by age related maculopathy lesions in a population. Br J Ophthalmol 1998 Jul; 82 (7): 743–747
Organisation for Economic Co-operation and Development (OECD). Health data 2006 [online]. Available from URL: http://www.oecd.org [Accessed 2006 Aug 17]
Bonastre J, Le Pen C, Anderson P, et al. The epidemiology, economics and quality of life burden of age-related macular degeneration in France, Germany, Italy and the United Kingdom. Eur J Health Econ 2002; 3 (2): 94–102
Brown DM, Kaiser PK, Michels M, et al. Ranibizumab versus verteporfin for neovascular age-related macular degeneration. N Engl J Med 2006 Oct 5; 355 (14): 1432–1444
Rosenfeld PJ, Brown DM, Heier JS, et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med 2006 Oct 5; 355 (14): 1419–1431
Chakravarthy U, Adamis AP, Cunningham Jr ET, et al. Year 2 efficacy results of 2 randomized controlled clinical trials of pegaptanib for neovascular age-related macular degeneration. Ophthalmology 2006 Sep; 113 (9): 1508–1521
Gragoudas ES, Adamis AP, Cunningham Jr ET, et al. Pegaptanib for neovascular age-related macular degeneration. N Engl J Med 2004 Dec 30; 351 (27): 2805–2816
Acknowledgements
Gisèle Soubrane, Daniel Pauleikhoff, Andrew Lotery and Jordi Mones have acted as consultants for and received honoraria from Pfizer Inc. This study was funded by Pfizer Inc. Alan F. Cruess has acted as a consultant for and received honoraria from Pfizer and Novartis. Gergana Zlateva and Ronald Buggage are employees of Pfizer Inc. Xiao Xu, Caroline Schaefer, Tyler Knight and Thomas F. Goss are full-time consultants at Covance and provide ongoing consulting and research services to numerous biopharmaceutical manufacturers. Editorial support, including revising the paper based on author feedback and styling the paper for journal submission, was provided by Dr Jane G. Murphy of Zola Associates and funded by Pfizer Inc.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Cruess, A.F., Zlateva, G., Xu, X. et al. Economic Burden of Bilateral Neovascular Age-Related Macular Degeneration. Pharmacoeconomics 26, 57–73 (2008). https://doi.org/10.2165/00019053-200826010-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200826010-00006