Abstract
Objective
To assess the cost effectiveness of palivizumab (a preventative treatment against severe respiratory syncytial virus [RSV] infection) in children at high risk of hospitalisation, i.e. preterm infants ≤35 weeks gestation, children with bronchopulmonary dysplasia (BPD) and children with congenital heart disease (CHD).
Methods
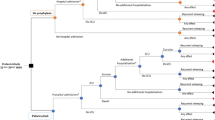
A decision tree model was developed employing data sources from the published literature, palivizumab clinical trials, official UK price/tariff lists and national population statistics. The comparator was no prophylaxis. The primary perspective of the study was that of the UK NHS. In a societal perspective scenario analysis, the future lost productivity of a child resulting from RSV-related mortality (indirect costs) was also included. The cost of administration of palivizumab, hospital care for RSV infections and the cost of asthma treatment were included.
The analysis was based on a lifetime follow-up period in order to capture the impact of palivizumab on long-term morbidity and mortality resulting from an RSV infection. The primary efficacy outcome in the palivizumab clinical trials was the number of RSV hospitalisations avoided, which was extrapolated to effectiveness outcomes, i.e. number of life-years gained and number of QALYs. Costs and effects were discounted by 3.5%.
Results
In preterm infants and children with BPD, prophylaxis with palivizumab compared with no prophylaxis had an incremental cost-effectiveness ratio (ICER) of £7042/QALY without discounting outcomes, increasing to £16 720/QALY after discounting. In babies with CHD, the use of palivizumab resulted in an ICER of £2427/QALY without discounting outcomes and £6664/QALY after discounting. One-way sensitivity analyses and probabilistic sensitivity analyses confirmed the robustness of the model. A scenario analysis showed that the inclusion of indirect costs leads to further improvement in the cost-effectiveness outcomes for palivizumab.
Conclusion
This study suggests that palivizumab prophylaxis against severe RSV infection in children at high risk may be cost effective from the NHS perspective (vs no prophylaxis), and that the positive clinical and economic benefits may persist beyond one RSV season.














Similar content being viewed by others
References
Hall C. Respiratory syncytial virus. In: Feigin R, Cherry J, editors. Infectious diseases. Philadelphia (PA): W.B. Saunders, 1998
Allport T, Davies E, Wells C, et al. Ribavarin and bronchiolitis: variation in use in the UK [letter]. Arch Dis Child 1997; 76: 385
Canfield S, Simoes E. Prevention of respiratory syncytial virus (RSV) infection: RSV immune globulin intravenous and palivizumab. Ped Ann 1999; 28: 507–514
Public Health Laboratory Service. Seasonal diseases: winter infections. Respiratory syncytial virus (RSV) infections [online]. Available from URL: http://www.phls.co.uk/seasonal/ rsv/RSV13.htm [Accessed 2005 Jun 15]
Clark S, Beresford M, Subhedar N, et al. Respiratory syncytial virus infection in high risk infants and the potential impact of prophylaxis in a United Kingdom cohort. Arch Dis Child 2000; 83: 313–316
Sampalis JS. Morbidity and mortality after RSV-associated hospitalizations among premature Canadian infants. J Pediatr 2003 Nov; 143 (5 Suppl.): S150–S156
Bont L, van Aalderen W, Kimpen J. Long term consequences of respiratory syncytial virus (RSV) bronchiolitis. Paediatr Respir Rev 2000; 1: 221–227
Sigurs N, Bjarnason R, Sigurbergsson F, et al. Asthma and immunoglobulin E antibodies after respiratory syncytial virus bronchiolitis: a prospective cohort study with matched controls. Pediatrics 1995; 95: 500–505
American Academy of Pediatrics Committee on Infectious Diseases and Committee of Fetus and Newborn. Prevention of respiratory syncytial virus infections: indications for the use of palivizumab and update on the use of RSV-IGIV. Pediatrics 1998 Nov; 102 (5): 1211–1216
IMpact study group. Palivizumab, a humanised respiratory syncytial virus monoclonal antibody, reduces hospitalisation from respiratory syncytial virus infection in high risk infants. Pediatrics 1998; 102: 531–537
Feltes TF, Cabalka AK, Meissner HC, et al. Palivizumab prophylaxis reduces hospitalization due to respiratory syncytial virus in young children with hemodynamically significant congenital heart disease: Cardiac Synagis Study Group. J Pediatr 2003; 143: 532–540
NICE. Guidance for manufacturers and sponsors: technology appraisals No. 5, 2001 [online]. Available from URL: http:// www.nice.org.uk/page.aspx?o 201974 [Accessed 2005 Jun 15]
Personal Social Services Research Unit. Unit costs of health and social care 2003 [online]. Available from URL: http://www.p ssru.ac.uk/pdf/uc2003/uc2003_inflation.pdf [Accessed 2005 Jun 1]
Nuijten MJC. Data management in modelling studies: the selection of data sources. PharmacoEconomics 1998; 3 (3): 305–316
Groothuis JR, Simoes EA, Levin MJ, et al. Prophylactic administration of respiratory syncytial virus immune globulin to high-risk infants and young children: Respiratory Syncytial Virus Immune Globulin Study Group. N Engl J Med 1993; 329: 1524–1530
PREVENT Study Group. Reduction of RSV hospitalisation among premature infants and infants with bronchopulmonary dysplasia using respiratory syncytial virus immune globulin prophylaxis. Pediatrics 1997; 99: 93–99
Simoes EA, Sondheimer HM, Top FH, et al. Respiratory syncytial virus immune globulin for prophylaxis against respiratory syncytial virus disease in infants and children with congenital heart disease: Cardiac study group. J Pediatr 1998 Oct; 133 (4): 492–499
Joffe S, Ray GT, Escobar GJ, et al. Cost-effectiveness of respiratory syncytial virus prophylaxis among preterm infants. Pediatrics 1999 Sept; 104 (3 pt 9): 419–427
MacDonald NE, Hall CB, Suffin SC, et al. Respiratory syncytial viral infection in infants with congenital heart disease. N Engl J Med 1982 Aug 12; 307 (7): 397–400
Rodriguez WJ, Parrott RH. Ribavirin aerosol treatment of serious respiratory syncytial virus infection in infants. Infect Dis Clin North Am 1987 Jun; 1 (2): 425–439
Wang EE, Law BJ, Stephens D. Pediatric investigators collaborative network on infections in Canada (PICNIC) prospective study of risk factors and outcomes in patients hospitalized with respiratory syncytial viral lower respiratory tract infection. J Pediatr 1995; 126: 212–219
Wang E, Tang NK. Immunoglobulin for preventing respiratory syncytial virus infection (Cochrane Review). Available in The Cochrane Library [database on disk and CD ROM]. Updated quarterly. The Cochrane Collaboration; issue 2. Chichester (UK): Oxford Update Software, 2004
Simoes E. Respiratory syncytial virus infection. Lancet 1999; 354: 847–852
National statistics [online]. Available from URL: http:// www.statistics.gov.uk [Accessed 2005 Jun 1]
Wren C, O’Sullivan JJ. Survival with congenital heart disease and need for follow up in adult life. Heart 2001; 85 (4): 438–443
Greenough A, Alexander J, Burgess S, et al. Health care utilisation of prematurely born, preschool children related to hospitalisation for RSV infection. Arch Dis Child 2004; 89 (7): 673–678
Netten A, Curtis L. Unit costs of health and social care 2000. Canterbury, UK: Personal Social Services Research Unit, University of Kent at Canterbury, 2000
Thomas M, Bedford-Russella A, Sharland M. Hospitalisation for RSV infection in expreterm infants: implications for use of RSV immune globulin. Arch Dis Child 2000; 83: 122–127
Greenough A, Cox S, Alexander J, et al. Health care utilisation of infants with chronic lung disease, related to hospitalisation for RSV Infection. Arch Dis Child 2001; 85: 463–468
Hospital Episode Statistics 1995–1999. London: Department of Health, 2000 [online]. Available from URL: http:// www.dh.gov.uk/publicationsandstatistics/statistics/hospitalepi sodestatistics/fs/en [Accessed 2005 Jun 15]
Simoes EAF, Carbonell-Estrany X, Kimpen J, et al. Palavizumab use decreases risk of recurrent wheezing in preterm children. Eur Respir J 2004; 24 Suppl. 48: 212s
International Labour Organization (ILO). Yearbook of Labour Statistics, 1998. Geneva: ILO, 1998
Organisation for Economic Cooperation and Development (OECD). OECD employment outlook: 2004 edition [online]. Available from URL: http://puck.sourceoecd.org/vl=4300666/ cl=14/nw=1/rpsv/ij/oecdthemes/99980045v2004n8/s1/p11 [Accessed 2006 Dec 1]
The Chartered Institute of Public Finance and Accountancy. The health service database 2003 (financial year 2002–3). London: CIPFA/HFM, IPF, 2003
Netten A, Curtis L. Unit costs of health and social care 2003. Canterbury, UK: Personal Social Services Research Unit, University of Kent at Canterbury, 2000
Devlin N, Parkin D. Does NICE have a cost-effectiveness threshold and what other factors influence its decisions? A binary choice analysis. Health Econ 2004; 13 (15): 437–452
Stevens TP, Sinkin RA, Hall CB, et al. Respiratory syncytial virus and premature infants born at 32 weeks’ gestation or earlier: hospitalization and economic implications of prophylaxis. Arch Pediatr Adolesc Med 2000 Jan; 154 (1): 55–61
Marchetti A, Lau H, Magar R, et al. Impact of palivizumab on expected costs of respiratory syncytial virus infection in preterm infants: potential for savings. Clin Ther 1999 Apr; 21 (4): 752–766
Rietveld E, Steyerberg E, Polder J, et al. Passive immunisation against respiratory syncytial virus: a cost-effectiveness analysis [thesis]. Enschede: Print Partners Ipscamp, 2003: 59–69
Rawlins MD, Culyer AJ. National Institute for Clinical Excellence and its value judgments. BMJ Jul 2004; 32: 224–227
Acknowledgements
This study was funded by Abbott GmbH &Co. KG, Ludwigshafen, Germany. The authors are grateful to Prof. Adrian Bagust, Economics Division, University of Liverpool, UK, for his support and input in the development of this study. MEDTAP received funding from Abbott GmbH &Co. KG, Ludwigshafen, Germany for the development of the model and writing of the manuscript. Wolfgang Wittenberg is an employee of Abbot GmbH and owns stock in the company. Maximilian Lebmeier was a contractor for Abbott Germany. All the authors contributed significantly to the intellectual content of the paper.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Nuijten, M.J.C., Wittenberg, W. & Lebmeier, M. Cost Effectiveness of Palivizumab for Respiratory Syncytial Virus Prophylaxis in High-Risk Children. Pharmacoeconomics 25, 55–71 (2007). https://doi.org/10.2165/00019053-200725010-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200725010-00006