Abstract
Proton-pump inhibitor (PPI) failure in gastro-oesophageal reflux disease (GORD) patients has become the main reason for referral of these patients to gastroenterology specialists. It is estimated that 30% of GORD patients requiring a PPI once daily will experience treatment failure. Patients with non-erosive reflux disease are the most common GORD-related group in which once-daily PPI therapy fails. Various mechanisms have been suggested to underlie PPI failure in GORD patients. The most pertinent include weakly acidic reflux, duodenogastro-oesophageal reflux, visceral hyperalgesia, delayed gastric emptying, psychological co-morbidity and concomitant functional bowel disorders, as well as others. Because of the importance of PPI failure as a target for future drug development, further understanding of the most relevant underlying mechanisms is needed.
Similar content being viewed by others
References
Locke GR 3rd, Talley NJ, Fett SL, et al. Prevalence and clinical spectrum of gastroesophageal reflux: a population-based study in Olmsted County, Minnesota. Gastroenterology 1997 May; 112(5): 1448–56
Inadomi JM, McIntyre L, Bernard L, et al. Step-down from multiple- to single-dose proton pump inhibitors (PPIs): a prospective study of patients with heartburn or acid regurgitation completed relieved with PPIs. Am J Gastroenterol 2003; 98(9): 1940–4
Carlsson R, Dent J, Watts R, et al. Gastro-oesophageal reflux disease in primary care: an international study of 56 treatment strategies with omeprazole. International GORD Study Group. Eur J Gastroenterol Hepatol 1998; 10(2): 119–24
Fass R, Shapiro M, Dekel R, et al. Proton pump inhibitor failure in reflux disease: where next? Aliment Pharmacol Ther 2005; 22(2): 79–94
Vaezi MF. ‘Refractory GERD’: acid, nonacid, or not GERD? Am J Gastroenterol 2004; 99(6): 989–90
Richter JE, Bochenek W. Pantoprazole US GERD Study Group. Oral pantoprazole for erosive esophagitis: a placebo-controlled randomized clinical trial. Am J Gastroenterol 2000; 95(11): 3071–80
Johnson DA, Lauritsen K, Junghard O, et al. Evaluation of symptoms is an unreliable predictor of relapse of erosive esophagitis in patients receiving maintenance PPI therapy [abstract no. T1646]. Gastroenterology 2003; 124 (4 Suppl.): A540
Fass R, Thomas S, Traxler D, et al. Patient reported outcome of heartburn improvement: doubling the proton pump inhibitor (PPI) dose in patient who failed standard dose PPI versus switching to a different PPI [abstract no. 326]. Gastroenterology 2004; 146 (4 Suppl. 2): A37
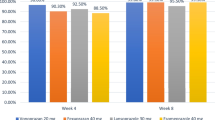
Fass R, Murthy U, Hayden CW, et al. Omeprazole 40mg once a day is equally effective as lansoprazole 30mg twice a day in symptom control of patients with gastro-oesophageal reflux disease (GERD) who are resistant to conventional-dose lansoprazole therapy: a prospective, randomized, multi-centre study. Aliment Pharmacol Ther 2000; 14(12): 1595–603
Dean BB, Gano AD Jr, Knight K, et al. Effectiveness of proton pump inhibitors in nonerosive reflux disease. Clin Gastroenterol Hepatol 2004; 2(8): 656–64
Lind T, Havelund T, Carlsson R, et al. Heartburn without oesophagitis: efficacy of omeprazole therapy and features determining therapeutic response. Scand J Gastroenterol 1997; 32(10): 974–9
Fass R, Tougas G. Functional heartburn: the stimulus, the pain, and the brain. Gut 2002; 51(6): 885–92
Bardhan KD, Hawkey CJ, Long RG, et al. Lansoprazole versus ranitidine for the treatment of reflux oesophagitis. UK Lansoprazole Clinical Research Group. Aliment Pharmacol Ther 1995; 9(2): 145–51
Castell DO, Richter JE, Robinson R, et al. Efficacy and safety of lansoprazole in the treatment of erosive reflux esophagitis. The Lansoprazole Group. Am J Gastroenterol 1996; 91(9): 1749–57
Sharma VK, Leontiadis GI, Howden CW. Meta-analysis of randomized controlled trials comparing standard clinical doses of omeprazole and lansoprazole in erosive oesophagitis. Aliment Pharmacol Ther 2001; 15(2): 227–31
Richter JE, Kahrilas PJ, Johanson J, et al. Efficacy and safety of esomeprazole compared to omeprazole in GERD patients with erosive esophagitis: a randomized controlled trial. Am J Gastroenterol 2001; 96(3): 656–65
Cooper BT, Neumann CS, Cox MA, et al. Continuous treatment with omeprazole 20mg daily for up to 6 years in Barrett’s oesophagus. Aliment Pharmacol Ther 1998; 12(9): 893–7
Fass R, Sampliner RE, Malagon IB, et al. Failure of oesophageal acid control in candidates for Barrett’s oesophagus reversal on a very high dose of proton pump inhibitor. Aliment Pharmacol Ther 2000; 14(5): 597–602
Sampliner RE. Effect of up to 3 years of high-dose lansoprazole on Barrett’s esophagus. Am J Gastroenterol 1994; 89(10): 1844–8
Malesci A, Savarino V, Zentilin P, et al. Partial regression of Barrett’s esophagus by long-term therapy with high-dose omeprazole. Gastrointest Endosc 1996; 44(6): 700–5
Gallup Study of Consumers’ use of Stomach Relief Products. Princeton (NJ): The Gallup Organization, 2000
Vela M, Camacho-Lobato L, Srinivasan R, et al. Simultaneous intraesophageal impedance and pH measurement of acid and nonacid gastroesophageal reflux: effect of omeprazole. Gastroenterology 2001; 120(7): 1599–606
Bredenoord A, Weusten B, Curvers W, et al. Determinants of perception of heartburn and regurgitation. Gut 2006; 55: 313–8
Mainie I, Tutuian R, Shay S, et al. Acid and non-acid reflux in patients with persistent symptoms despite acid suppressive therapy: a multicentre study using combined ambulatory impedance-pH monitoring. Gut 2006 Oct; 55(10): 1398–402
Frazzoni M, De Micheli E, Zentilin P, et al. Pathophysiological characteristics of patients with non-erosive reflux disease differ from those of patients with functional heartburn. Aliment Pharmacol Ther 2004; 20(1): 81–8
Martinez SD, Malagon IB, Garewal HS, et al. Non-erosive reflux disease (NERD): acid reflux and symptom patterns. Aliment Pharmacol Ther 2003; 17(4): 537–45
Watson RG, Tham TC, Johnston BT, et al. Double blind crossover placebo controlled study of omeprazole in the treatment of patients with reflux symptoms and physiological levels of acid reflux: the “sensitive oesophagus”. Gut 1997; 40(5): 587–90
Fass R, Ofman JJ. Gastroesophageal reflux disease: should we adopt a new conceptual framework? Am J Gastroenterol 2002; 97(8): 1901–9
Hobson AR, Matthews P, Furlong P, et al. The role of esophageal afferent pathway sensitivity in non-erosive reflux disease [abstract no. 128]. Gastroenterology 2004; 126 (4 Suppl. 2): A18
Shapiro M, Green C, Bautista J, et al. Functional heartburn patients demonstrate traits of functional bowel disorder but lack a uniform increase of chemoreceptor sensitivity to acid. Am J Gastroenterol 2006 May; 101(5): 1084–91
Vaezi MF. Duodenogastroesophageal reflux. In: Castro D, Richter J, editors. The oesophagus. Philadelphia (PA): Lippincott Williams & Wilkins, 2004: 1553–8
Netzer P, Gut A, Brundler R, et al. Influence of pantoprazole on oesophageal motility, and bile and acid reflux in patients with oesophagitis. Aliment Pharmacol Ther 2001; 15(9): 1375–84
Marshall RE, Anggiansah A, Manifold DK, et al. Effect of omeprazole 20mg twice daily on duodenogastric and gastro-oesophageal bile reflux in Barrett’s oesophagus. Gut 1998; 43(5): 603–6
Tack J, Koek G, Demedts I, et al. Gastroesophageal reflux disease poorly responsive to single-dose proton pump inhibitors in patients without Barrett’s esophagus: acid reflux, bile reflux, or both? Am J Gastroenterol 2004; 99(6): 981–8
Siddiqui A, Rodriguez-Stanley S, Zubaidi S, et al. Esophageal visceral sensitivity to bile salts in patients with functional heartburn and in healthy control subjects. Dig Dis Sci 2005; 50(1): 81–5
Kudara N, Chiba T, Orii S, et al. Gastric emptying of patients with persistent reflux symptoms and erosive esophagitis under PPI therapy [abstract no 23]. Neurogastroenterol Motil 2004; 16(5): 654
Sotoudehmanesh R, Ali Asgari A, Ansari R, et al. Endoscopic findings in end-stage renal disease. Endoscopy 2003; 35(6): 502–5
Cucchiara S, Minella R, Campanozzi A, et al. Effects of omeprazole on mechanisms of gastroesophageal reflux in childhood. Dig Dis Sci 1997; 42(2): 293–9
Liacouras CA, Campbell C, Ruchelli E, et al. Eosinophilic esophagitis: a 10-year experience in 381 children. Clin Gastroenterol Hepatol 2005; 3: 1198–206
Remedios M, Campbell C, Jones DM, et al. Eosinophilic esophagitis in adults: clinical, endoscopie, histologie findings, and response to treatment with fluticasone proprionate. Gastrointest Endosc 2006; 63: 3–12
Straumann A, Spichtin H-P, Grize L, et al. Natural history of primary eosinophilic esophagitis: a follow-up of 30 adult patients for up to 11.5 years. Gastroenterology 2003; 125: 1660–9
Croese J, Fairley SK, Masson JW, et al. Clinical and endoscopic features of eosinophilic esophagitis in adults. Gastrointest Endosc 2003; 58: 516–22
Potter JW, Saeian K, Staff D, et al. Eosinophilic esophagitis in adults: an emerging problem with unique eseophageal features. Gastrointest Endosc 2004; 59: 355–61
Zimmerman SL, Levine MS, Rubesin SE, et al. Idiopathic eosinophilic esophagitis in adults: the ringed esophagus. Radiology 2005; 236: 159–65
Johnston BT, Lewis S, Collins J, et al. Acid perception in gastro-oesophageal reflux disease is dependent on psychosocial factors. Scand J Gastroenterol 1995; 30: 1–5
Nojkov B, Chey W, Adlis S, et al. Predictors of response to PPI therapy in patients with GERD: the influence of co-morbid IBS and psychological disease [abstract]. Gastroenterology 2005; 128 (4 Suppl. 2): A61
Delhotal-Landes B, Cournot A, Vermerie N, et al. The effect of food and antacids on lansoprazole absorption and disposition. Eur J Drub Metab Pharmacokinet 1991; Spec No 3: 315–20
Dammann HG, Fuchs W, Richter G, et al. Lansoprazole versus omeprazole: influence on meal-stimulated gastric acid secretion. Aliment Pharmacol Ther 1997; 11(2): 359–64
Leite L, Lambrecht N, Sachs G, et al. Is omeprazole resistance due to mutations of cysteine 813 or 822 in the acid pump? [abstract]. Gastroenterology 1995; 108: A147
Furuta T, Shirai N, Watanabe F, et al. Effect of cytochrome P4502C19 genotypic differences on cure rates for gastroesophageal reflux disease by lansoprazole. Clin Pharmacol Ther 2002; 72(4): 453–60
Kawamura M, Ohara S, Koike T, et al. The effect of lansoprazole on erosive reflux esophagitis are influenced by CYP2C19 polymorphism. Aliment Pharmacol Ther 2003; 17: 965–73
Egan LJ, Myhre GM, Mays DC, et al. CYP2C19 pharmacogenetics in the clinical use of proton-pump inhibitors for gastro-oesophageal reflux disease: variant alleles predict gastric acid suppression, but not oesophageal acid exposure or reflux symptoms. Aliment Pharmacol Ther 2003; 17(12): 1521–8
Peghini PL, Katz PO, Bracy NA, et al. Nocturnal recovery of gastric acid secretion with twice-daily dosing of proton pump inhibitors. Am J Gastroenterol 1998; 93(5): 763–7
Ours TM, Fackler WK, Richter JE, et al. Nocturnal acid breakthrough: clinical significance and correlation with esophageal acid exposure. Am J Gastroenterol 2003; 98(3): 545–50
Fouad YM, Katz PO, Castell DO. Oesophageal motility defects associated with nocturnal gastro-oesophageal reflux on proton pump inhibitors. Aliment Pharmacol Ther 1999; 13(11): 1467–71
Nzeako UC, Murray JA. An evaluation of the clinical implications of acid breakthrough in patients on proton pump inhibitor therapy. Aliment Pharmacol Ther 2002; 16(7): 1309–16
Orr WC, Harnish MJ. The efficacy of omeprazole twice daily with supplemental H2 blockade at bedtime in the suppression of nocturnal oesophageal and gastric acidity. Aliment Pharmacol Ther 2003; 17(12): 1553–8
Verdu EF, Armstrong D, Fraser R, et al. Effect of Helicobacter pylori status on intragastric pH during treatment with omeprazole. Gut 1995; 36(4): 539–43
Vigneri S, Termini R, Savarino V, et al. Review article: is Helicobacter pylori status relevant to the management of GORD? Aliment Pharmacol Ther 2000; 14 Suppl. 3: 31–42
Holtmann G, Cain C, Malfertheiner P. Gastric Helicobacter pylori infection accelerates healing of reflux esophagitis during treatment with the proton pump inhibitor pantoprazole. Gastroenterology 1999; 117(1): 11–6
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fass, R. Proton-Pump Inhibitor Therapy in Patients with Gastro-Oesophageal Reflux Disease. Drugs 67, 1521–1530 (2007). https://doi.org/10.2165/00003495-200767110-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-200767110-00001