Abstract
Menopause, regardless of age at onset, is associated with a marked increase in coronary heart disease (CHD) risk. On the basis of epidemiological studies that demonstrated mainly positive effects of postmenopausal hormone therapy on CHD as well as on risk markers of CHD, it has been suggested that CHD could be prevented in postmenopausal women with long-term hormone therapy. However, since the publications of the Heart and Estrogen/progestin Replacement Study and the Women’s Health Initiative trial, prescription of hormone therapy for the prevention of CHD has become controversial.
Major efforts have been made to identify alternatives for hormone therapy. Compounds suggested have included selective estrogen receptor modulators (SERMs), which represent a class with a growing number of compounds that act as either estrogen receptor agonists or antagonists in a tissue-specific manner. This pharmacological profile may offer the opportunity to dissociate favourable estrogenic effects on the bone and cardiovascular system from unfavourable stimulatory effects on the breast and endometrium. Two SERMs presently on the market are tamoxifen and raloxifene. The only data available regarding the effects of tamoxifen on cardiovascular events in postmenopausal women are from breast cancer trials. These trials found fewer fatal myocardial events in women randomly assigned to tamoxifen compared with women assigned to placebo.
Raloxifene is a second-generation SERM that has been shown to prevent osteoporotic fractures, is safe for the endometrium and holds high promise for the prevention of breast cancer. The effect of raloxifene on CHD is still uncertain. On the basis of the MORE (Multiple Outcomes of Raloxifene Evaluation) trial, raloxifene may offer some protection to women with CHD or to those who are at high risk of CHD. Proof that raloxifene reduces the risk of CHD requires a clinical trial with hard clinical endpoints. Such a study is currently underway.
Next-generation SERMs taken into clinical development include idoxifene, droloxifene, ospemifene, arzoxifene, acolbifene/EM-800, levormeloxifene, lasofoxifene, bazedoxifene and HMR 3339. The aim is to find a compound with the ideal profile, that is, alleviation of climacteric symptoms and prevention of osteoporotic fractures, but without an adverse effect on the breast and endometrium, and no negative effect or even a beneficial effect on the cardiovascular system and the brain. Currently, limited data are available with regard to these next-generation SERMs and CHD. Nevertheless, some of these novel agents provide arguments for continuing the search for an ideal SERM.











Similar content being viewed by others
References
Barrett-Connor E, Bush TL. Estrogen and coronary artery disease in women. JAMA 1991; 265: 1861–7
Maxwell SR. Women and heart disease. Basic Res Cardiol 1998; 93 Suppl. 2: 79–84
Kannel WB, Hjortland MC, McNamara PM, et al. Menopause and risk of cardiovascular disease: the Framingham study. Ann Intern Med 1976; 85: 447–52
Gaspard UJ, Gottal JM, van den Brule FA. Postmenopausal changes of lipid and glucose metabolism: a review of their main aspects. Maturitas 1995; 21: 171–8
Scanu AM, Lawn RM, Berg K. Lipoprotein(a) and atherosclerosis. Ann Intern Med 1991; 115: 209–18
Maher VM, Brown BG. Lipoprotein (a) and coronary heart disease. Curr Opin Lipid 1995; 6: 229–35
Spencer CP, Godsland IF, Stevenson JC. Is there a menopausal metabolic syndrome? Gynecol Endocrinol 1997; 11: 341–55
Wouters MG, Moorrees MT, van der Mooren MJ, et al. Plasma homocysteine and menopausal status. Eur J Clin Invest 1995; 25: 801–5
Hak AE, Polderman KH, Westendorp IC, et al. Increased plasma homocysteine after menopause. Atherosclerosis 2000; 149: 163–8
Mijatovic V, van der Mooren MJ, Stehouwer CDA, et al. Postmenopausal hormone replacement, risk estimators for coronary artery disease and cardiovascular protection. Gynecol Endocrinol 1999; 13: 130–44
Stampfer MJ, Colditz GA, Willett WC, et al. Postmenopausal estrogen therapy and cardiovascular disease: ten year follow-up from the Nurses’ Health Study. N Engl J Med 1991; 325: 756–62
Stampfer MJ, Colditz GA. Estrogen replacement therapy and coronary heart disease: a quantitative assessment of the epidemiologic evidence. Prev Med 1991; 20: 47–63
Grady D, Rubin SM, Petitti DB, et al. Hormone therapy to prevent disease and prolong life in postmenopausal women. Ann Intern Med 1992; 117: 1016–37
Barrett-Connor E, Grady D. Hormone replacement therapy, heart disease, and other considerations. Annu Rev Public Health 1998; 19: 55–72
Hulley S, Grady D, Bush T, et al. Randomized trial of estrogen plus progestin for secondary prevention of coronary heart disease in postmenopausal women. JAMA 1998; 280: 605–13
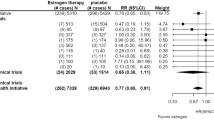
Manson JE, Hsia J, Johnson KC, et al. Estrogen plus progestin and the risk of coronary heart disease. N Engl J Med 2003; 349: 523–34
Anderson GL, Limacher M, Assaf AR, et al. Effects of conjugated equine estrogen in postmenopausal women with hysterectomy: the Women’s Health Initiative randomized controlled trial. JAMA 2004; 291: 1701–12
Peverill RE. Hormone therapy and venous thromboembolism. Best Pract Res Clin Endocrinol Metab 2003; 17: 149–64
Fisher B, Costantino JP, Wickerham DL, et al. Tamoxifen for prevention of breast cancer: report of the National Surgical Adjuvant Breast and Bowel Project P-1 Study. J Natl Cancer Inst 1998; 90: 1371–88
Cummings SR, Eckert S, Krueger KA, et al. The effect of raloxifene on risk of breast cancer in postmenopausal women: results from the MORE randomized trial. JAMA 1999; 281: 2189–97
Walsh BW, Kuller LH, Wild RA, et al. Effects of raloxifene on serum lipids and coagulation factors in healthy postmenopausal women. JAMA 1998; 279: 1445–51
Brzozowski AM, Pike AC, Dauter Z, et al. Molecular basis of agonism and antagonism in the oestrogen receptor. Nature 1997; 389: 753–8
Kenemans P. Estrogens and antiestrogens: basic and clinical aspects. A book review. N Engl J Med 1998; 338: 1079
Yang NN, Venugopalan M, Hardikar S, et al. Identification of an estrogen response element activated by metabolites of 17beta-estradiol and raloxifene. Science 1996; 273: 1222–5
Systemic treatment of early breast cancer by hormonal, cytotoxic, or immune therapy. 133 randomised trials involving 31,000 recurrences and 24,000 deaths among 75,000 women. Early Breast Cancer Trialists’ Collaborative Group.Lancet 1992; 339: 71–85
Tamoxifen for early breast cancer: an overview of the randomised trials. Early Breast Cancer Trialists’ Collaborative Group. Lancet 1998; 351: 1451–67
Wysowski DK, Honig SF, Beitz J. Uterine sarcoma associated with tamoxifen use. N Engl J Med 2002; 346: 1832–3
Veronesi U, Maisonneuve P, Costa A, et al. Prevention of breast cancer with tamoxifen: preliminary findings from the Italian randomised trial among hysterectomised women. Italian Tamoxifen Prevention Study. Lancet 1998; 352: 93–7
Powles T, Eeles R, Ashley S, et al. Interim analysis of the incidence of breast cancer in the Royal Marsden Hospital tamoxifen randomised chemoprevention trial. Lancet 1998; 352: 98–101
Cuzick J, Forbes J, Edwards R, et al. First results from the International Breast Cancer Intervention Study (IBIS-I): a randomised prevention trial. Lancet 2002; 360: 817–24
Veronesi U, Maisonneuve P, Sacchini V, et al. Tamoxifen for breast cancer among hysterectomised women. Lancet 2002; 359: 1122–4
Veronesi U, Maisonneuve P, Rotmensz N, et al. Italian randomized trial among women with hysterectomy: tamoxifen and hormone-dependent breast cancer in high-risk women. J Natl Cancer Inst 2003; 95: 160–5
Cuzick J, Powles T, Veronesi U, et al. Overview of the main outcomes in breast-cancer prevention trials. Lancet 2003; 361: 296–300
Love RR, Mazess RB, Barden HS, et al. Effects of tamoxifen on bone mineral density in postmenopausal women with breast cancer. N Engl J Med 1992; 326: 852–6
Love RR, Barden HS, Mazess RB, et al. Effect of tamoxifen on lumbar spine bone mineral density in postmenopausal women after 5 years. Arch Intern Med 1994; 154: 2585–8
Powles TJ, Hickish T, Kanis JA, et al. Effect of tamoxifen on bone mineral density measured by dual-energy x-ray absorptiometry in healthy premenopausal and postmenopausal women. J Clin Oncol 1996; 14: 78–84
Cushman M, Costantino JP, Tracy RP, et al. Tamoxifen and cardiac risk factors in healthy women: suggestion of an anti-inflammatory effect. Arterioscler Thromb Vasc Biol 2001; 21: 255–61
Cattaneo M, Baglietto L, Zighetti ML, et al. Tamoxifen reduces plasma homocysteine levels in healthy women. Br J Cancer 1998; 77: 2264–6
Love RR, Newcomb PA, Wiebe DA, et al. Effects of tamoxifen therapy on lipid and lipoprotein levels in postmenopausal patients with node-negative breast cancer. J Natl Cancer Inst 1990; 82: 1327–32
Love RR, Wiebe DA, Newcomb PA, et al. Effects of tamoxifen on cardiovascular risk factors in postmenopausal women. Ann Intern Med 1991; 115: 860–4
Love RR, Surawicz TS, Williams EC. Antithrombin III level, fibrinogen level, and platelet count changes with adjuvant tamoxifen therapy. Arch Intern Med 1992; 152: 317–20
Love RR, Anker G, Yang Y, et al. Serum homocysteine levels in postmenopausal breast cancer patients treated with tamoxifen. Cancer Lett 1999; 145: 73–7
Love RR, Wiebe DA, Feyzi JM, et al. Effects of tamoxifen on cardiovascular risk factors in postmenopausal women after 5 years of treatment. J Natl Cancer Inst 1994; 86: 1534–9
Anker G, Lonning PE, Ueland PM, et al. Plasma levels of the atherogenic amino acid homocysteine in post-menopausal women with breast cancer treated with tamoxifen. Int J Cancer 1995; 60: 365–8
Bertelli G, Pronzato P, Amoroso D, et al. Adjuvant tamoxifen in primary breast cancer: influence on plasma lipids and antithrombin III levels. Breast Cancer Res Treat 1988; 12: 307–10
Simon T, Boutouyrie P, Simon JM, et al. Influence of tamoxifen on carotid intima-media thickness in postmenopausal women. Circulation 2002; 106: 2925–9
Genc S, Tanrikulu-Kilic F, Gurdol F, et al. Effect of tamoxifen on fibrinogen, D-dimer, lipid and lipoprotein concentrations in breast cancer patients. Clin Chim Acta 2003; 337: 177–9
Stamatelopoulos KS, Lekakis JP, Poulakaki NA, et al. Tamoxifen improves endothelial function and reduces carotid intimamedia thickness in postmenopausal women. Am Heart J 2004; 147: 1093–9
Mannucci PM, Bettega D, Chantarangkul V, et al. Effect of tamoxifen on measurements of hemostasis in healthy women. Arch Intern Med 1996; 156: 1806–10
McDonald CC, Stewart HJ. Fatal myocardial infarction in the Scottish adjuvant tamoxifen trial. The Scottish Breast Cancer Committee. BMJ 1991; 303: 435–7
McDonald CC, Alexander FE, Whyte BW, et al. Cardiac and vascular morbidity in women receiving adjuvant tamoxifen for breast cancer in a randomised trial: the Scottish Cancer Trials Breast Group. BMJ 1995; 311: 977–80
Rutqvist LE, Mattsson A. Cardiac and thromboembolic morbidity among postmenopausal women with early-stage breast cancer in a randomized trial of adjuvant tamoxifen: the Stockholm Breast Cancer Study Group. J Natl Cancer Inst 1993; 85: 1398–406
Stampfer MJ, Malinow MR, Willett WC, et al. A prospective study of plasma homocyst(e)ine and risk of myocardial infarction in US physicians. JAMA 1992; 268: 877–81
Boushey CJ, Beresford SA, Omenn GS, et al. A quantitative assessment of plasma homocysteine as a risk factor for vascular disease: probable benefits of increasing folic acid intakes. JAMA 1995; 274: 1049–57
Mijatovic V, van der Mooren MJ. Homocysteine in postmenopausal women and the importance of hormone replacement therapy. Clin Chem Lab Med 2001; 39: 764–7
Peterson JC, Spence JD. Vitamins and progression of atherosclerosis in hyper-homocyst(e)inaemia [letter]. Lancet 1998; 351: 263
Rimm EB, Willett WC, Hu FB, et al. Folate and vitamin B6 from diet and supplements in relation to risk of coronary heart disease among women. JAMA 1998; 279: 359–64
Ridker PM, Hennekens CH, Buring JE, et al. C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med 2000; 342: 836–43
Van Baal WM, Kenemans P, van der Mooren MJ, et al. Increased C-reactive protein levels during short-term hormone replacement therapy in healthy postmenopausal women. Thromb Haemost 1999; 81: 925–8
Cushman M, Legault C, Barrett-Connor E, et al. Effect of postmenopausal hormones on inflammation-sensitive proteins: the Postmenopausal Estrogen/Progestin Interventions (PEPI) Study. Circulation 1999; 100: 717–22
Post MS, van der Mooren MJ, Stehouwer CD A, et al. Effects of transdermal and oral oestrogen replacement therapy on C-reactive protein levels in postmenopausal women: a randomised, placebo-controlled study. Thromb Haemost 2002; 88: 605–10
Lacut K, Oger E, Le Gal G, et al. Differential effects of oral and transdermal postmenopausal estrogen replacement therapies on C-reactive protein. Thromb Haemost 2003; 90: 124–31
Prestwood KM, Unson C, Kulldorff M, et al. The effect of different doses of micronized 17beta-estradiol on C-reactive protein, interleukin-6, and lipids in older women. J Gerontol A Biol Sci Med Sci 2004; 59: 827–32
Costantino JP, Kuller LH, Ives DG, et al. Coronary heart disease mortality and adjuvant tamoxifen therapy. J Natl Cancer Inst 1997; 89: 776–82
Reis SE, Costantino JP, Wickerham DL, et al. Cardiovascular effects of tamoxifen in women with and without heart disease: breast cancer prevention trial. National Surgical Adjuvant Breast and Bowel Project Breast Cancer Prevention Trial Investigators. J Natl Cancer Inst 2001; 93: 16–21
Buzdar AU, Marcus C, Holmes F, et al. Phase II evaluation of Lyl56758 in metastatic breast cancer. Oncology 1988; 45: 344–5
Delmas PD, Bjarnason NH, Mitlak BH, et al. Effects of raloxifene on bone mineral density, serum cholesterol concentrations, and uterine endometrium in postmenopausal women. N Engl J Med 1997; 337: 1641–7
Rohatgi N, Blau R, Lower EE. Raloxifene is associated with less side effects than tamoxifen in women with early breast cancer: a questionnaire study from one physician’s practice. J Womens Health Gend Based Med 2002; 11: 291–301
Martino S, Cauley JA, Barrett-Connor E, et al. Continuing outcomes relevant to Evista: breast cancer incidence in postmenopausal osteoporotic women in a randomized trial of raloxifene. J Natl Cancer Inst 2004; 96: 1751–61
Ettinger B, Black DM, Mitlak BH, et al. Reduction of vertebral fracture risk in postmenopausal women with osteoporosis treated with raloxifene: results from a 3-year randomized clinical trial. Multiple Outcomes of Raloxifene Evaluation (MORE) Investigators. JAMA 1999; 282: 637–45
Delmas PD, Ensrud KE, Adachi JD, et al. Efficacy of raloxifene on vertebral fracture risk reduction in postmenopausal women with osteoporosis: four-year results from a randomized clinical trial. J Clin Endocrinol Metab 2002; 87: 3609–17
Cauley JA, Norton L, Lippman ME, et al. Continued breast cancer risk reduction in postmenopausal women treated with raloxifene: 4-year results from the MORE trial. Multiple outcomes of raloxifene evaluation. Breast Cancer Res Treat 2001; 65: 125–34
Draper MW, Flowers DE, Huster WJ, et al. A controlled trial of raloxifene (LY139481) HC1: impact on bone turnover and serum lipid profile in healthy postmenopausal women. J Bone Miner Res 1996; 11: 835–42
Walsh BW, Paul S, Wild RA, et al. The effects of hormone replacement therapy and raloxifene on C-reactive protein and homocysteine in healthy postmenopausal women: a randomized, controlled trial. J Clin Endocrinol Metab 2000; 85: 214–8
De Valk-de Roo GW, Stehouwer CDA, Meijer P, et al. Both raloxifene and estrogen reduce major cardiovascular risk factors in healthy postmenopausal women: a 2-year, placebo-controlled study. Arterioscler Thromb Vasc Biol 1999; 19: 2993–3000
Mijatovic V, Netelenbos JC, van der Mooren MJ, et al. Randomized, double-blind, placebo-controlled study of the effects of raloxifene and conjugated equine estrogens on plasma homocysteine levels in healthy postmenopausal women. Fertil Steril 1998; 70: 1085–9
Mijatovic V, van der Mooren MJ, Kenemans P, et al. Raloxifene lowers serum lipoprotein (a) in healthy postmenopausal women: a randomized, double-blind, placebo-controlled comparison with conjugated equine estrogens. Menopause 1999; 6: 134–7
Vogelvang TE, Mijatovic V, Kamp O, et al. Neither long-term treatment with raloxifene nor hormone replacement therapy modulate cardiac function in healthy postmenopausal women: two randomized, placebo-controlled, 2-year studies. Am J Obstet Gynecol 2002; 186: 729–36
De Leo V, La Marca A, Morgante G, et al. Randomized control study of the effects of raloxifene on serum lipids and homocysteine in older women. Am J Obstet Gynecol 2001; 184: 350–3
Smolders RG, Vogelvang TE, Mijatovic V, et al. A 2-year, randomized, comparative, placebo-controlled study on the effects of raloxifene on lipoprotein(a) and homocysteine. Maturitas 2002; 41: 105–14
Vogelvang TE, Leurs JR, van der Mooren MJ, et al. Raloxifene reduces procarboxypeptidase U, an antifibrinolytic marker: a 2-year randomized, placebo-controlled study in healthy early postmenopausal women. Menopause 2004; 11: 110–5
Vogelvang TE, van der Mooren MJ, Mijatovic V. Hormone replacement therapy, selective estrogen receptor modulators, and tissue-specific compounds: cardiovascular effects and clinical implications. Treat Endocrinol 2004; 3: 105–15
Barrett-Connor E, Grady D, Sashegyi A, et al. Raloxifene and cardiovascular events in osteoporotic postmenopausal women: four-year results from the MORE (Multiple Outcomes of Raloxifene Evaluation) randomized trial. JAMA 2002; 287: 847–57
Vogelvang TE, Mijatovic V, Kenemans P, et al. HMR 3339, a novel selective estrogen receptor modulator, reduces total cholesterol, low-density lipoprotein cholesterol, and homocysteine in healthy postmenopausal women. Fertil Steril 2004; 82: 1540–9
Grey AB, Stapleton JP, Evans MC, et al. The effect of the antiestrogen tamoxifen on bone mineral density in normal late postmenopausal women. Am J Med 1995; 99: 636–41
Applebaum-Bowden D, McLean P, Steinmetz A, et al. Lipoprotein, apolipoprotein, and lipolytic enzyme changes following estrogen administration in postmenopausal women. J Lipid Res 1989; 30: 1895–906
Vogelvang TE, Mijatovic V, Kenemans P, et al. The effects of 12 weeks of HMR 3339, a novel selective estrogen receptor modulator, on markers of coagulation and fibrinolysis: a randomized, placebo-controlled, double-blind, dose-ranging study in healthy postmenopausal women. Am J Obstet Gynecol 2005; 193: 1384–94
Kannel WB, Wolf PA, Castelli WP, et al. Fibrinogen and risk of cardiovascular disease: the Frammingham Study. JAMA 1987; 258: 1183–6
Azevedo GD, Franco RF, Baggio MS, et al. Effects of raloxifene therapy on the anticoagulant system in postmenopausal women. Climacteric 2003; 6: 140–5
Thögersen AM, Jansson JH, Boman K, et al. High plasminogen activator inhibitor and tissue plasminogen activator levels in plasma precede a first acute myocardial infarction in both men and women: evidence for the fibrinolytic system as an independent primary risk factor. Circulation 1998; 98: 2241–7
Lindahl TL, Ohlsson PI, Wiman B. The mechanism of the reaction between human plasminogen-activator inhibitor 1 and tissue plasminogen activator. Biochem J 1990; 265: 109–13
Hendriks DF, Scharpe SS, van Sande M, et al. Characterisation of a carboxypeptidase in human serum distinct from carboxypeptidase N. J Clin Chem Clin Biochem 1989; 27: 277–85
Wang W, Boffa MB, Bajzar L, et al. A study of the mechanism of inhibition of fibrinolysis by activated thrombin-activable fibrinolysis inhibitor. J Biol Chem 1998; 273: 27176–81
Leurs J, Wissing BM, Nerme V, et al. Different mechanisms contribute to the biphasic pattern of carboxypeptidase U (TAFIa) generation during in vitro clot lysis in human plasma. Thromb Haemost 2003; 89: 264–71
Van Tilburg NH, Rosendaal FR, Bertina RM. Thrombin activatable fibrinolysis inhibitor and the risk for deep vein thrombosis. Blood 2000; 95: 2855–9
Silveira A, Schatteman KA, Goossens FJ, et al. Plasma procarboxypeptidase U in men with symptomatic coronary artery disease. Thromb Haemost 2000; 84: 364–8
Morange PE, Juhan-Vague I, Scarabin PY, et al. Association between TAFI antigen and Ala 147Thr polymorphism of the TAFI gene and the angina pectoris incidence. The PRIME study. Thromb Haemost 2003; 89: 554–60
Santamaria A, Oliver A, Borrell M, et al. Risk of ischemic stroke associated with functional thrombin-activatable fibrinolysis inhibitor plasma levels. Stroke 2003; 34: 2387–91
Schatteman KA, Goossens FJ, Scharpé SS, et al. Assay of procarboxypeptidase U, a novel determinant of the fibrinolytic cascade, in human plasma. Clin Chem 1999; 45: 807–13
Juhan-Vague I, Renucci JF, Grimaux M, et al. Thrombin-activatable fibrinolysis inhibitor antigen levels and cardiovascular risk factors. Arterioscler Thromb Vasc Biol 2000; 20: 2156–61
Chetaille P, Alessi MC, Kouassi D, et al. Plasma TAFI antigen variations in healthy subjects. Thromb Haemost 2000; 83: 902–5
Post MS, Hendriks DF, van der Mooren MJ, et al. Oral oestradiol/trimegestone replacement reduces procarboxypeptidase U (TAFI): a randomized placebo-controlled 12-week study in early postmenopausal women. J Intern Med 2002; 251: 245–51
Bladbjerg EM, Madsen JS, Kristensen SR, et al. Effect of long-term hormone replacement therapy on tissue factor pathway inhibitor and thrombin activatable fibrinolysis inhibitor in healthy postmenopausal women: a randomized controlled study. J Thromb Haemost 2003; 1: 1208–14
Vogelvang TE, Leurs JR, Mijatovic V, et al. HMR 3339, a novel estrogen receptor modulator, reduces concentrations of procarboxypeptidase U, an inhibitor of fibrinolysis: arandomized, placebo-controlled study in postmenopausal women. J Thromb Haemost 2005; 3: 1090–2
Post MS, Leurs JR, van der Mooren MJ, et al. Different effects of low-dose transdermal and oral oestrogen therapy on procarboxy-peptidase U, an inhibitor of fibrinolysis, in healthy postmenopausal women: a randomised, placebo-controlled study. Thromb Haemost 2005; 93: 620–2
Vogelvang TE, Mijatovic V, Kenemans P, et al. Effect of HMR 3339, a novel selective estrogen receptor modulator, on C-reactive protein levels in healthy postmenopausal women. Am J Cardiol 2004; 94: 1205–8
Lerman A, Edwards BS, Hallett JW, et al. Circulating and tissue endothelin immunoreactivity in advanced atherosclerosis. N Engl J Med 1991; 325: 997–1001
Mikkola T, Viinikka L, Ylikorkala O, et al. Estrogen and postmenopausal estrogen/progestin therapy: effect on endothelium-dependent prostacyclin, nitric oxide and endothelin-1 production. Eur J Obstet Gynecol Reprod Biol 1998; 79: 75–82
Van Baal WM, Kenemans P, Emeis JJ, et al. Long-term effects of combined hormone replacement therapy on markers of endothelial function and inflammatory activity in healthy postmenopausal women. Fertil Steril 1999; 71: 663–70
Van Baal WM, Emeis JJ, Kenemans P, et al. Short-term hormone replacement therapy: reduced plasma levels of soluble adhesion molecules. Eur J Clin Invest 1999; 29: 913–21
Saitta A, Altavilla D, Cucinotta D, et al. Randomized, double-blind, placebo-controlled study on effects of raloxifene and hormone replacement therapy on plasma NO concentrations, endothelin-1 levels, and endothelium-dependent vasodilation in postmenopausal women. Arterioscler Thromb Vasc Biol 2001; 21: 1512–9
Christodoulakos G, Panoulis C, Kouskouni E, et al. Effects of estrogen-progestin and raloxifene therapy on nitric oxide, prostacyclin and endothelin-1 synthesis. Gynecol Endocrinol 2002; 16: 9–17
Pines A, Fisman EZ, Shemesh J, et al. Menopause related changes in left ventricular function in healthy women. Cardiology 1992; 80: 413–6
Pines A, Fisman EZ, Levo Y, et al. Menopause induced changes in left ventricular wall thickness. Am J Cardiol 1993; 72: 240–1
Pines A, Fisman EZ, Levo Y, et al. The effects of hormone replacement therapy in normal postmenopausal women: measurements of Doppler-derived parameters of aortic flow. Am J Obstet Gynecol 1991; 164: 806–12
Pines A, Fisman EZ, Ayalon D, et al. Long-term effects of hormone replacement therapy on Doppler-derived parameters of aortic flow in postmenopausal women. Chest 1992; 102: 1496–8
Voutilainen S, Hippelainen M, Hulkko S, et al. Left ventricular diastolic function by Doppler echocardiography in relation to hormonal replacement therapy in healthy postmenopausal women. Am J Cardiol 1993; 71: 614–7
Taskin O, Gokdeniz R, Muderrisoglu H, et al. The effects of hormone replacement therapy on echocardiographic basic cardiac functions in postmenopausal women. Hum Reprod 1998; 13: 2399–401
Fak AS, Erenus M, Tezcan H, et al. Effects of a single dose of oral estrogen on left ventricular diastolic function in hypertensive postmenopausal women with diastolic dysfunction. Fertil Steril 2000; 73: 66–71
Kamali P, Müller T, Lang U, et al. Cardiovascular responses of perimenopausal women to hormonal replacement therapy. Am J Obstet Gynecol 2000; 182: 17–22
Pines A, Fisman EZ, Averbuch M, et al. Left ventricular function during a short-term transdermal estradiol therapy in postmenopausal women: a double-blind placebo-controlled echocardiographic study. Eur Menopause J 1996; 3: 53–9
Snabes MC, Payne JP, Kopelen HA, et al. Physiologic estradiol replacement therapy and cardiac structure and function in normal postmenopausal women: a randomized, double-blind, placebo-controlled, crossover trial. Obstet Gynecol 1997; 89: 332–9
Lee M, Giardina EG, Homma S, et al. Lack of effect of estrogen on rest and treadmill exercise in postmenopausal women without known cardiac disease. Am J Cardiol 1997; 80: 793–7
Kessel H, Kamp O, Kenemans P, et al. Effects of 15 months 17β-estradiol/dydrogesterone on systolic cardiac function using quantitative and Doppler echocardiography in healthy postmenopausal women. Am J Obstet Gynecol 2001; 184: 910–6
Vogelvang TE, van der Mooren MJ, Kamp O, et al. Effects of oral and transdermal low-dose estrogen therapy on echocardiographic parameters of cardiac function. Fertil Steril 2003; 80: 546–53
Light K, Hinderliter A, West S, et al. Hormone replacement improves hemodynamic profile and left ventricular geometry in hypertensive and normotensive postmenopausal women. J Hypertens 2001; 19: 269–78
Johnell O, Cauley JA, Kulkarni PM, et al. Raloxifene reduces risk of vertebral fractures and breast cancer in postmenopausal women regardless of prior hormone therapy. J Fam Pract 2004; 53: 789–96
Mosca L, Barrett-Connor E, Wenger NK, et al. Design and methods of the Raloxifene Use for The Heart (RUTH) study. Am J Cardiol 2001; 88: 392–5
Wenger NK, Barrett-Connor E, Collins P, et al. Baseline characteristics of participants in the Raloxifene Use for The Heart (RUTH) trial. Am J Cardiol 2002; 90: 1204–10
Fleischer AC, Wheeler JE, Yeh IT, et al. Sonographic assessment of the endometrium in osteopenic postmenopausal women treated with idoxifene. J Ultrasound Med 1999; 18: 503–12
Chesnut C, Weiss S, Mulder H, et al. Idoxifene increases bone mineral density in osteopenic postmenopausal women [abstract]. Bone 1998; 23 Suppl.: S389
Van Rietbergen B, Majumdar S, Newitt D, et al. High-resolution MRI and micro-FE for the evaluation of changes in bone mechanical properties during longitudinal clinical trials: application to calcaneal bone in postmenopausal women after one year of idoxifene treatment. Clin Biomech (Bristol, Avon) 2002; 17: 81–8
Arpino G, Nair KM, Doval DC, et al. Idoxifene versus tamoxifen: a randomized comparison in postmenopausal patients with metastatic breast cancer. Ann Oncol 2003; 14: 233–41
Johnston SR, Gumbrell LA, Evans TR, et al. A cancer research (UK) randomized phase II study of idoxifene in patients with locally advanced/metastatic breast cancer resistant to tamoxifen. Cancer Chemother Pharmacol 2004; 53: 341–8
Herrington DM, Pusser BE, Riley WA, et al. Cardiovascular effects of droloxifene, a new selective estrogen receptor modulator, in healthy postmenopausal women. Arterioscler Thromb Vasc Biol 2000; 20: 1606–12
Herrington DM, Brosnihan KB, Pusser BE, et al. Differential effects of E and droloxifene on C-reactive protein and other markers of inflammation in healthy postmenopausal women. J Clin Endocrinol Metab 2001; 86: 4216–22
Buzdar A, Hayes D, El Khoudary A, et al. Phase III randomized trial of droloxifene and tamoxifen as first-line endocrine treatment of ER/PgR-positive advanced breast cancer. Breast Cancer Res Treat 2002; 73: 161–75
Voipio SK, Komi J, Kangas L, et al. Effects of ospemifene (FC-1271a) on uterine endometrium, vaginal maturation index, and hormonal status in healthy postmenopausal women. Maturitas 2002; 43: 207–14
Ylikorkala O, Cacciatore B, Halonen K, et al. Effects of ospemifene, a novel SERM, on vascular markers and function in healthy, postmenopausal women. Menopause 2003; 10: 440–7
Rutanen EM, Heikkinen J, Halonen K, et al. Effects of ospemifene, a novel SERM, on hormones, genital tract, climacteric symptoms, and quality of life in postmenopausal women: a double-blind, randomized trial. Menopause 2003; 10: 433–9
Komi J, Heikkinen J, Rutanen EM, et al. Effects of ospemifene, a novel SERM, on biochemical markers of bone turnover in healthy postmenopausal women. Gynecol Endocrinol 2004; 18: 152–8
Munster PN, Buzdar A, Dhingra K, et al. Phase I study of a third-generation selective estrogen receptor modulator, LY353381.HCL, in metastatic breast cancer. J Clin Oncol 2001; 19: 2002–9
Buzdar A, O’Shaughnessy JA, Booser DJ, et al. Phase II, randomized, double-blind study of two dose levels of arzoxifene in patients with locally advanced or metastatic breast cancer. J Clin Oncol 2003; 21: 1007–14
Baselga J, Llombart-Cussac A, Bellet M, et al. Randomized, double-blind, multicenter trial comparing two doses of arzoxifene (LY353381) in hormone-sensitive advanced or metastatic breast cancer patients. Ann Oncol 2003; 14: 1383–90
McMeekin DS, Gordon A, Fowler J, et al. A phase II trial of arzoxifene, a selective estrogen response modulator, in patients with recurrent or advanced endometrial cancer. Gynecol Oncol 2003; 90: 64–9
Labrie F, Champagne P, Labrie C, et al. Activity and safety of the antiestrogen EM-800, the orally active precursor of acolbifene, in tamoxifen-resistant breast cancer. J Clin Oncol 2004; 22: 864–71
Alexandersen P, Riis BJ, Stakkestad JA, et al. Efficacy of levormeloxifene in the prevention of postmenopausal bone loss and on the lipid profile compared to low dose hormone replacement therapy. J Clin Endocrinol Metab 2001; 86: 755–60
Goldstein SR, Nanavati N. Adverse events that are associated with the selective estrogen receptor modulator levormeloxifene in an aborted phase III osteoporosis treatment study. Am J Obstet Gynecol 2002; 187: 521–7
Bolognese M, Moffett Jr A, Lee A, et al. Lasofoxifene is superior to raloxifene in the prevention of bone loss in postmenopausal women: 1-year results [abstract]. Bone 2003; 32 Suppl. 5: S93
Pickar JH. Bazedoxifene [abstract]. Fourth Amsterdam Menopause Symposium; 2004 Oct 2–4; Amsterdam
Chander SK, McCague R, Luqmani Y, et al. Pyrrolidino-4-iodotamoxifen and 4-iodotamoxifen, new analogues of the antiestrogen tamoxifen for the treatment of breast cancer. Cancer Res 1991; 51: 5851–8
Coombes RC, Haynes BP, Dowsett M, et al. Idoxifene: report of a phase I study in patients with metastatic breast cancer. Cancer Res 1995; 55: 1070–4
Nuttall ME, Bradbeer JN, Stroup GB, et al. Idoxifene: a novel selective estrogen receptor modulator prevents bone loss and lowers cholesterol levels in ovariectomized rats and decreases uterine weight in intact rats. Endocrinology 1998; 139: 5224–34
Hasmann M, Rattel B, Loser R. Preclinical data for droloxifene. Cancer Lett 1994; 84: 101–16
Buzdar AU, Kau S, Hortobagyi GN, et al. Phase I trial of droloxifene in patients with metastatic breast cancer. Cancer Chemother Pharmacol 1994; 33: 313–6
Haarstad H, Gundersen S, Wist E, et al. Droloxifene: a new antiestrogen. A phase II study in advanced breast cancer. Acta Oncol 1992; 31: 425–8
Bruning PF. Droloxifene, a new anti-oestrogen in postmenopausal advanced breast cancer: preliminary results of a double-blind dose-finding phase II trial. Eur J Cancer 1992; 28A: 1404–7
Haarstad H, Lonning PE, Gundersen S, et al. Influence of droloxifene on metastatic breast cancer as first-line endocrine treatment. Acta Oncol 1998; 37: 365–8
Chen HK, Ke HZ, Lin CH, et al. Droloxifene inhibits cortical bone turnover associated with estrogen deficiency in rats. Bone 1995; 17: 175S–9S
Ke HZ, Chen HK, Qi H, et al. Effects of droloxifene on prevention of cancellous bone loss and bone turnover in the axial skeleton of aged, ovariectomized rats. Bone 1995; 17: 491–6
Qu Q, Zheng H, Dahllund J, et al. Selective estrogenic effects of a novel triphenylethylene compound, FC1271a, on bone, cholesterol level, and reproductive tissues in intact and ovariectomized rats. Endocrinology 2000; 141: 809–20
Hellmann-Blumberg U, Taras TL, Wurz GT, et al. Genotoxic effects of the novel mixed antiestrogen FC-1271a in comparison to tamoxifen and toremifene. Breast Cancer Res Treat 2000; 60: 63–70
DeGregorio MW, Wurz GT, Taras TL, et al. Pharmacokinetics of (deaminohydroxy)toremifene in humans: a new, selective estrogen-receptor modulator. Eur J Clin Pharmacol 2000; 56: 469–75
Gennari L. Ospemifene (Hormos). Curr Opin Investig Drugs 2004; 5: 448–55
Suh N, Glasebrook AL, Palkowitz AD, et al. Arzoxifene, a new selective estrogen receptor modulator for chemoprevention of experimental breast cancer. Cancer Res 2001; 61: 8412–5
Freddie CT, Larsen SS, Bartholomaeussen M, et al. The effect of the new SERM arzoxifene on growth and gene expression in MCF-7 breast cancer cells. Mol Cell Endocrinol 2004; 219: 27–36
Rossberg MI, Murphy SJ, Traystman RJ, et al. LY353381.HCl, a selective estrogen receptor modulator, and experimental stroke. Stroke 2000; 31: 3041–6
Sato M, Turner CH, Wang T, et al. LY353381.HCl: a novel raloxifene analog with improved SERM potency and efficacy in vivo. J Pharmacol Exp Ther 1998; 287: 1–7
Sato M, Zeng GQ, Rowley E, et al. LY353381 x HCl: an improved benzothiophene analog with bone efficacy complementary to parathyroid hormone-(1–34). Endocrinology 1998; 139: 4642–51
Ma YL, Bryant HU, Zeng Q, et al. Long-term dosing of arzoxifene lowers cholesterol, reduces bone turnover, and preserves bone quality in ovariectomized rats. J Bone Miner Res 2002; 17: 2256–64
Martel C, Provencher L, Li X, et al. Binding characteristics of novel nonsteroidal antiestrogens to the rat uterine estrogen receptors. J Steroid Biochem Mol Biol 1998; 64: 199–205
Labrie F, Labrie C, Belanger A, et al. EM-652 (SCH 57068), a third generation SERM acting as pure antiestrogen in the mammary gland and endometrium. J Steroid Biochem Mol Biol 1999; 69: 51–84
Martel C, Picard S, Richard V, et al. Prevention of bone loss by EM-800 and raloxifene in the ovariectomized rat. J Steroid Biochem Mol Biol 2000; 74: 45–56
Picard F, Deshaies Y, Lalonde J, et al. Effects of the estrogen antagonist EM-652.HCl on energy balance and lipid metabolism in ovariectomized rats. Int J Obes Relat Metab Disord 2000; 24: 830–40
Holm P, Shalmi M, Korsgaard N, et al. A partial estrogen receptor agonist with strong antiatherogenic properties without noticeable effect on reproductive tissue in cholesterol-fed female and male rabbits. Arterioscler Thromb Vasc Biol 1997; 17: 2264–72
Warming L, Christoffersen C, Riis BJ, et al. Adverse effects of a SERM (Levormeloxifene): safety parameters and bone mineral density 12 months after treatment withdrawal. Maturitas 2003; 44: 189–99
Ke HZ, Paralkar VM, Grasser WA, et al. Effects of CP-336,156, a new, nonsteroidal estrogen agonist/antagonist, on bone, serum cholesterol, uterus and body composition in rat models. Endocrinology 1998; 139: 2068–76
Rosati RL, Da Silva JP, Cameron KO, et al. Discovery and preclinical pharmacology of a novel, potent, nonsteroidal estrogen receptor agonist/antagonist, CP-336156, a diaryltetrahydronaphthalene. J Med Chem 1998; 41: 2928–31
Ke HZ, Qi H, Crawford DT, et al. Lasofoxifene (CP-336,156), a selective estrogen receptor modulator, prevents bone loss induced by aging and orchidectomy in the adult rat. Endocrinology 2000; 141: 1338–44
Ke HZ, Foley GL, Simmons HA, et al. Long-term treatment of lasofoxifene preserves bone mass and bone strength and does not adversely affect the uterus in ovariectomized rats. Endocrinology 2004; 145: 1996–2005
Miller CP, Collini MD, Tran BD, et al. Design, synthesis, and preclinical characterization of novel, highly selective indole estrogens. J Med Chem 2001; 44: 1654–7
Komm BS, Lyttle CR. Developing a SERM: stringent preclinical selection criteria leading to an acceptable candidate (WAY-140424) for clinical evaluation. Ann N Y Acad Sci 2001; 949: 317–26
Miller CP, Harris HA, Komm BS. Bazedoxifene acetate. Drugs Future 2002; 27: 117–21
Hoechst Marion Roussel R&D. HMR 3339: investigator’s brochure 1999. Report no.: 99/11161/GN [2nd ed]. Romainville, France: Hoechst Marion, Roussel R&D, 1999
Ammann P, Bourrin S, Brunner F, et al. A new selective estrogen receptor modulator HMR-3339 fully corrects bone alterations induced by ovariectomy in adult rats. Bone 2004; 35: 153–61
Van der Mooren MJ, Kenemans P. Postmenopausal hormone therapy: impact on menopause-related symptoms, chronic disease and quality of life. Drugs 2004; 64: 821–36
Stampfer MJ, Hu FB, Manson JE, et al. Primary prevention of coronary heart disease in women through diet and lifestyle. N Engl J Med 2000; 343: 16–22
Acknowledgements
No sources of funding were used to assist in the preparation of this review. The authors have no conflicts of interest that are directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vogelvang, T.E., van der Mooren, M.J., Mijatovic, V. et al. Emerging Selective Estrogen Receptor Modulators. Drugs 66, 191–221 (2006). https://doi.org/10.2165/00003495-200666020-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-200666020-00005