Summary
Patients with essential arterial hypertension demonstrate abnormal vasodilator capacity either during increased cardiac metabolic demand or during pharmacological vasodilation. Structural and functional damage to the coronary microcirculation has been proposed as one of the major causes of impaired coronary reserve in this disease.
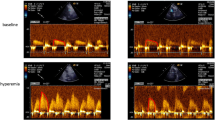
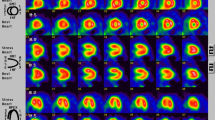
To assess the role of microvascular impairment in regional myocardial blood flow (MBF), 27 patients with essential hypertension were evaluated by dynamic positron emission tomography (PET) at rest, during atrial pacing and after dipyridamole infusion and compared with 13 healthy subjects. All patients had normal coronary arteries, 17 had moderate to severe hypertension and 10 had mild hypertension. Baseline mean MBF of 0.97 ± 0.25 ml/min/g was significantly increased to 1.60 ± 0.38 during atrial pacing and 2.35 ± 0.95 after dipyridamole infusion (p < 0.01); however, mean flow during atrial pacing and after dipyridamole infusion was significantly lower than in healthy subjects (2.15 ± 0.73 and 3.71 ± 0.86 ml/min/g, p < 0.05 and p < 0.01, respectively). The MBF response to atrial pacing and dipyridamole infusion was similarly depressed in patients with mild and severe hypertension.
The study was repeated after 6 months of antihypertensive treatment with the calcium antagonist verapamil or the angiotensin converting enzyme (ACE) inhibitor enalapril in a subgroup of 20 patients as part of a randomised, single-blind clinical trial. This study is still in progress; the initial 16 patients treated with verapamil or enalapril showed an obvious improvement in MBF values during atrial pacing and after dipyridamole infusion after 6 months of therapy (mean MBF: 2.10 ± 0.64 and 2.99 ± 1.63 ml/min/g. respectively, p < 0.05 vs pretreatment values).
In conclusion, obvious impairment of MBF during atrial pacing and after dipyridamole infusion was observed in hypertensive patients with normal coronary arteries and this appeared unrelated to the severity of hypertension. Therapy with verapamil or enalapril improved coronary reserve and MBF response to an increase in myocardial oxygen demand.
Similar content being viewed by others
References
Bache RJ, Vrobel TR, Ring SW, Emery RW, Andersen RW. Regional myocardial blood flow during exercise in dogs with chronic left ventricular hypertrophy. Circulation Research 48: 76–87, 1981
Bellina CR, Parodi O, Camici P, Salvadori PA, Taddei L, et al. Simultaneous in vitro and in vivo validation of nitrogen-13-ammonia for the assessment of regional myocardial blood flow. Journal of Nuclear Medicine 31: 1335–1343, 1990
Cuocolo A, Sax FL, Brush JE, Maron BJ, Bacharach SL, et al. Left ventricular hypertrophy and impaired diastolic filling in essential hypertension. Diastolic mechanisms for systolic dysfunction during exercise. Circulation 81: 978–986, 1990
Daly P, Rouleau JL, Cousineau JL, Burgess JH. Acute effects of captopril on the coronary circulation of patients with hypertension and angina. American Journal of Medicine 76: 111–115, 1984
De Marco T, Daly PA, Liu M, Kayser S, Parmley WW, et al. Enalaprilat: a new parenteral angiotensin-converting enzyme inhibitor: rapid changes in systemic and coronary hemodynamics and humoral profile in chronic heart failure. Journal of the American College of Cardiology 9: 1131–1138, 1987
Devereux RD, Alonso DR, Lutas EN, et al. Echocardiographic assessment of left ventricular hypertrophy: comparison with necropsy finding. American Journal of Cardiology 57: 540–548, 1986
Eighorn P, Grimm J, Koch R, Hess O, Carroll J, et al. Left ventricular relaxation in patients with left ventricular hypertrophy secondary to aortic valve disease. Circulation 65: 1395–1404, 1982
Foult JM, Tavolaro O, Antony I, Nitenberg A. Direct myocardial and coronary effects of enalaprilat in patients with dilated cardiomyopathy: assessment by a bilateral intracoronary infusion technique. Circulation 77: 337–344, 1988
Gwatmey JK, Morgan JP. Altered calcium handling in experimental pressure-overload hypertrophy in the ferret. Circulation Research 57: 836–843, 1985
Halperin JL, Faxon DP, Creager MA, Bass TA, Melidossian CD, et al. Coronary hemodynamic effects of angiotensin inhibition by captopril and teprotide in patients with congestive heart failure. American Journal of Cardiology 50: 967–972, 1982
Hanrath P, Mathey DG, Siegert R, Bleifeld W. Left ventricular relaxation and filling pattern in different forms of left ventricular hypertrophy: an echocardiographic study. American Journal of Cardiology 45: 15–23, 1980
Inouye IK, Massie BM, Loge D, Simpson P, Tubau JF. Failure of antihypertensive therapy with diuretic, beta-blocking and calcium channel-blocking drugs to consistently reverse left ventricular diastolic filling abnormalities. American Journal of Cardiology 53: 1583–1587, 1984
Magrini F, Reggiani P, Roberts N, Meazza R, Ciulla M, et al. Effects of angiotensin and angiotensin blockade on coronary circulation and coronary reserve. American Journal of Medicine 84: 55–60, 1988
Marcus M, Doty DB, Hiratzka LF, Wright CB, Eastham CL. Decreased coronary reserve: a mechanism for angina pectoris in patients with aortic stenosis and normal coronary arteries. New England Journal of Medicine 307: 1362–1367, 1982
McLaurin LP, Rolett EL, Grossman W. Impaired left ventricular relaxation during pacing induced ischemia. American Journal of Cardiology 32: 751–757, 1973
Opherk D, Mall G, Zebe H, Schwartz F, Wehle E, et al. Reduction of coronary reserve: a mechanism for angina pectoris in patients with arterial hypertension and normal coronary arteries. Circulation 69: 1–7, 1984
Parodi O, Simonetti I, Michelassi C, Carpeggiani C, Biagini A, et al. Comparison of verapamil and propranolol in rest angina pectoris. A randomized multiple cross-over trial in the coronary care unit. American Journal of Cardiology 57: 899–906, 1986
Paulus WJ, Serizawa T, Grossman W. Altered left ventricular diastolic properties during pacing induced ischemia in dogs with coronary stenoses: potentiation by caffeine. Circulation Research 40: 218–227, 1982
Pichard AD, Gorlin R, Smith H, Ambrose J, Meller J. Coronary flow studies in patients with left ventricular hypertrophy of the hypertensive type. American Journal of Cardiology 47: 547–554, 1981
Shapiro LM, McKenna WJ. Left ventricular hypertrophy. Relation of structure to diastolic function in hypertension. British Heart Journal 51: 637–642, 1984
Sordahl LA, McCollum WB, Wood WG, Schwartz A. Mitochondria and sarcoplasmic reticulum function in cardiac hypertrophy and failure. American Journal of Physiology 224: 497–502, 1978
Strauer BE. Ventricular function and coronary hemodynamics in hypertensive heart disease. American Journal of Cardiology 44: 999–1006, 1979
Tomaneck RJ. Response of the coronary vascolature to myocardial hypertrophy. Journal of the American College of Cardiology 15: 528–533, 1990
Vatner SF, Shannon R, Hittinger L. Reduced subendocardial coronary reserve. A potential mechanism for impaired diastolic function in the hypertrophied and failing heart. Circulation 81(Suppl. III): 8–14, 1990
Yamori Y, Yagawa T, Tagami M, Kanbe T, Nara Y, et al. Humoral trophic influence on cardiovascular structural changes in hypertension. Hypertension 6(Suppl. III): 27–38, 1984
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Parodi, O., Neglia, D., Sambuceti, G. et al. Regional Myocardial Blood Flow and Coronary Reserve in Hypertensive Patients. Drugs 44 (Suppl 1), 48–55 (1992). https://doi.org/10.2165/00003495-199200441-00009
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199200441-00009