Summary
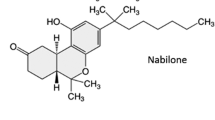
Synopsis: Nabilone1 is a new orally active cannabinoid for the treatment of severe gastrointestinal toxicity associated with cancer chemotherapy. The pharmacological profile of nabilone suggests that it acts primarily by preventing emesis controlled by the medulla oblongata, although its secondary mild anxiolytic activity may contribute to the overall efficacy. Nabilone 2mg twice daily starting 12 hours prior to, and continued for the duration of, chemotherapy produces significant reduction in the severity and duration of nausea and the frequency of vomiting in about 50 to 70% of patients with severe symptoms refractory to conventional therapy. Nabilone has proven to be more effective in controlling symptoms and preferred by more patients than prochlorperazine 10mg 2 to 4 times daily in a limited number of studies, despite a higher incidence of side effects. Comparative trials against other new antiemetic agents, such as high dose metoclopramide, and use of nabilone in combination with other antiemetics remain to be undertaken. The incidence of side effects is high with nabilone; drowsiness, dizziness and/or vertigo occur in 60 to 70% of patients, but rarely lead to drug withdrawal, although more troublesome effects, such as postural hypotension, ataxia, vision disturbance and toxic psychoses, may cause discontinuation of therapy. Thus, nabilone offers an effective alternative to the treatment options available in a difficult therapeutic area — those patients with severe gastrointestinal side effects from cancer chemotherapy who are refractory to conventional therapy.
Pharmacodynamic Studies: The antiemetic activity of nabilone has been demonstrated in anaesthetised and unanaesthetised cats. Nabilone was more potent than prochlorperazine in preventing emesis due to intravenous cisplatin (cis-diamminedichloroplatinum), nitrosureas. mechlorethamine and other emetogenic agents. Less activity was seen against apomorphine-induced emesis and no activity was seen against intravenous nicotine-induced emesis, suggesting these effects of nabilone may occur at the level of the vomiting control mechanism in the medulla oblongata. Nabilone usually produces marked reduction in blood pressure in cats, rabbits and rats (but not in monkeys or dogs). However, there is some evidence that cardiovascular and behavioural effects are intimately linked, and that repeated administration is associated with tolerance to the cardiovascular effects of nabilone. Mild anxiolytic activity has been seen with ‘lower’ doses both in animal models and in man, and at high doses nabilone is associated with locomotor disturbance and sedation. Nabilone possesses little or no opiate-like activity, does not induce development of a withdrawal syndrome and may be associated with a lower incidence of euphoria than Δ9-tetrahydrocannabinol, although evidence of abuse potential for nabilone has been demonstrated.
Pharmacokinetic Studies: Only very limited data are available on the disposition of nabilone in man. Oral doses are rapidly absorbed and the bioavailability is about 96%. Nabilone has an elimination half-life of about 2 hours and is extensively metabolised to a mixture of isomeric alcohols, with extended half-lives (up to 35 hours). Toxicity in dogs led to a withdrawal of nabilone from clinical trials until it was discovered that metabolism of the drug in dogs was different to that in man and other species.
Therapeutic Trials: Nabilone has been used as an oral antiemetic agent in the treatment of gastrointestinal toxicity in patients undergoing cancer chemotherapy. Significant reduction of the duration and severity of nausea and frequency of vomiting is usually seen after nabilone 2mg 2 or 3 times daily in about 50 to 70% of patients, many of whom have been refractory to conventional antiemetics. In a limited number of comparative studies, nabilone has produced significantly greater reduction of symptoms than prochlorperazine, and reduced the necessity for supplemental parenteral therapy. Despite a higher incidence of side effects, nabilone has also been preferred to prochlorperazine as treatment of choice in the majority of cases (40 to 75% vs 15 to 23%), although in 2 of 3 placebo-controlled studies less than 20% of patients elected to continue with nabilone therapy. Patients with more severe symptoms [induced by cisplatin, doxorubicin (adriamycin), cyclophosphamide] appear to respond equally well as those with less severe symptoms, and thus comprise the preferred treatment group for therapy with nabilone. Further therapeutic studies are needed with nabilone, particularly to clarify its efficacy compared with high dose metoclopramide and other antiemetic agents, and its use in combination with other antiemetic agents.
Side Effects: Nabilone is associated with a high incidence of mild or moderate side effects, the most common being drowsiness, dizziness and vertigo (60 to 70%), and dry mouth (29%). More severe effects such as postural hypotension, ataxia, visual disturbance and some toxic psychoses are occasionally seen, and may necessitate treatment withdrawal. Nabilone produces a higher incidence of side effects than prochlorperazine, but they may lessen in severity during continued therapy.
Dosage and Administration: The usual therapeutic dose of nabilone for use as an antiemetic agent in patients undergoing cancer chemotherapy is 2mg twice daily commencing 12 hours prior to, and continuing until one dose after, chemotherapy.
Similar content being viewed by others
References
Ahmedzai, S.; Carlyle, I.T. and Moran, F.: Anti-emetic efficacy and toxicity of nabilone, a synthetic cannabinoid, in lung cancer chemotherapy. British Journal of Cancer 48: 657–663 (1983).
Archer, R.A.; Fukuda, D.S.; Kossoy, A.D. and Abbott, B.J.: Microbiological transformations of nabilone, a synthetic cannabinoid. Applied and Environmental Microbiology 37: 965–971 (1979).
Archer, R.A.; Hanasono, G.K.; Lemburger, L. and Sullivan, H.R.: Update of nabilone research: The relationship of metabolism to toxicity in dogs; in Poster et al. (Eds) Treatment of Cancer Chemotherapy Induced Nausea and Vomiting, pp. 119–127 (Masson, New York 1981).
Cone, L.A.; Greene, D.S. and Helm, N.A.: Use of nabilone in the treatment of chemotherapy-induced vomiting in an outpatient setting. Cancer Treatment Reviews 9(Suppl. B): 63–70 (1982).
Cornbleet, M.A.; Hamilton, D.A.; Christian, P. and Smyth, J.F.: Evaluation of nabilone as an anti-emetic. British Journal of Cancer 46: 492–493 (1982).
Craigmill, A.: Cannabinoids and handling-induced convulsions. Research Communications in Psychology, Psychiatry and Behaviour 4: 51–63 (1979).
Desante, K.; Wolen, K.; Bergstrom, R.; Hatcher, B.; Spradlin, C. and Lemberger, L.: Determination of the bioavailability and dose proportionality of nabilone using stable isotope technology. Proceedings of the 2nd World Conference on Clinical Pharmacology and Therapeutics, p. 48 (Washington, 1983).
Doherty, P.A.; McCarthy, L.E. and Borison, H.L.: Respiratory and cardiovascular depressant effects of nabilone, N-methyllevonantradol and Δ9-tetrahydrocannabinol in anaesthetised cats. Journal of Pharmacology and Experimental Therapeutics 227: 508–516 (1983).
Einhorn, L.: Nabilone: An effective antiemetic agent in patients receiving cancer chemotherapy. Cancer Treatment Reviews 9(Suppl. B): 55–61 (1982).
Einhorn, L.H.; Nagy, C; Furnas, B. and Williams, S.D.: Nabilone: An effective anti-emetic in patients receiving cancer chemotherapy. Journal of Clinical Pharmacology 21: 64S–69S (1981).
Fabre, L.F. and McLendon, D.: The efficacy and safety of nabilone (a synthetic cannabinoid) in the treatment of anxiety. Journal of Clinical Pharmacology 21: 377S–382S (1981).
Fabre, L.F.; McLendon, D.M. and Stark, P.D.: Nabilone, and cannabinoid, in the treatment of anxiety: An open-label and double-blind study. Current Therapeutic Research 24: 161–169 (1978).
George, M.; Pejovic, M.H.; Thuaire, M.; Kramar, A. and Wolff, J.P.: Essai comparatif randomisé d’un nouvel anti-émétique: La nabilone, chez des maladies cancéreuses traitées par le cisplatinum. Biomedicine and Pharmacotherapy 37: 24–27 (1983).
Gilbert, P.E.: A comparison of THC, nantradol, nabilone and morphine in the chronic spinal dog. Journal of Clinical Pharmacology 21: 311S:319S (1981).
Glass, R.M.; Uhlenhuth, E.H.; Hartel, F.W.; Schuster, L.R. and Fischman, M.W.: A single dose study of nabilone, a synthetic cannabinoid. Psychopharmacology 71: 137–142 (1980).
Glass, R.M.; Uhlenhuth, E.H.; Hartel, F.W.; Shuster, CR. and Fischman, M.W.: Single-dose study of nabilone in anxious volunteers. Journal of Clinical Pharmacology 21: 383–396 (1981).
Gong, H.; Tashkin, D.P. and Calvarese, B.: Comparison of bronchial effects of nabilone and terbutaline in healthy and asthmatic subjects. Journal of Clinical Pharmacology 23: 127–133 (1983).
Green, J.; Bigger, J.F.; Kim, K. et al.: Canabinoid action on the eye as mediated through the central nervous system and local adrenergic activity. Experimental Eye Research 24: 189–196 (1977).
Hepler, R.S.; Frank, I.M. and Ungerleider, J.T.: Pupillary constriction after maijuana smoking. American Journal of Ophthalmology 74: 1185–1190 (1972).
Herman, T.S.; Einhorn, L.H.; Jones, S.E.; Nagy, C; Chester, A.B. et al.: Superiority of nabilone over prochlorperazine as an antiemetic in patients receiving cancer chemotherapy. New England Journal of Medicine 300: 1295–1297 (1979).
Herman, T.S.; Jones, S.E.; Dean, J.; Leigh, S.; Dorr, R. et al.: Nabilone: A potent anti-emetic cannabinol with minimal euphoria. Biomedicine 27: 331–334 (1977).
Hogan, P.; Sharpe, M.; Smedley, H. and Sikora, K.: Cannabinoids and LCG levels in patients with testicular cancer. Lancet 2: 1144 (1983).
Ilaria, R.L.; Thornby, J.I. and Fann, W.E.: Nabilone, a cannabinol derivative, in the treatment of anxiety neurosis. Current Therapeutic Research 29: 943–949 (1981).
Johansson, R.; Kilkku, P. and Groenroos, M.: A double-blind, controlled study of nabilone vs prochlorperazine for refractory emesis induced by cancer chemotherapy. Cancer Treatment Research 9(Suppl. B): 25–33 (1982).
Johnson, R.E.; Jasinski, D.R.; Boren, J.J. and Kocher, T.R.: Abuse potential of nabilone. Proceedings of the 2nd World Conference on Clinical Pharmacology and Therapeutics, p. 90 (Washington, DC, Jul–Aug 1983).
Jones, S.E.; Durant, J.R.; Greco, F.A. and Robertone, A.: A multi-institutional phase III study of nabilone vs chemotherapy-induced nausea and vomiting. Cancer Treatment Reviews 9(Suppl. B): 45–48 (1982).
Lemberger, L. and Rowe, H.: Clinical pharmacology of nabilone, a cannabinol derivative. Clinical Pharmacology and Therapeutics 18: 720–726 (1975).
Lemberger, L.; Rubin, A.; Wolen, R.; DeSante, K.; Rowe, H. et al.: Pharmacokinetics, metabolism and drug-abuse potential of nabilone. Cancer Treatment Reviews 9(Suppl. B): 17–23 (1982).
Levitt, M.: Nabilone vs placebo in the treatment of chemotherapy-induced nausea and vomiting in cancer patients. Cancer Treatment Reviews 9(Suppl. B): 49–53 (1982).
London, S.W.; McCarthy, L.E. and Borison, H.L.: Suppression of cancer chemotherapy-induced vomiting in the cat by nabilone, a synthetic cannabinoid. Proceedings of the Society for Experimental Biology and Medicine 160: 437–440 (1979).
McCarthy, L.E. and Borison, H.L.: Antiemetic action of nabilone against apomorphine- and deslanoside-induced vomiting. Pharmacologist 19: 230 (1977).
McCarthy, L.E. and Borison, H.L.: Antiemetic activity of N-methyllevonantradol, and nabilone in cisplatin-treated cats. Journal of Clinical Pharmacology 21: 30S–37S (1981).
Markham, J.K.; Hanasono, G.K.; Adams, E.R. and Owen, N.V.: Reproduction studies on nabilone, a synthetic 9-ketocannabinoid. Toxicology and Applied Pharmacology 48: Al 19 (1979).
Mcndelson, J.H. and Mello, N.K.: Reinforcing properties of oral Δ9-tetrahydrocannabinol, smoked marijuana, and nabilone: Influence of previous marijuana use. Psychopharmacology 83: 351–356 (1984).
Meyer, B.R.; Reidenberg, M.M.; Drayer, D.E.; Pasmantier, M. and Lewin, M.: Initial trial of metoclopramide and nabilone combination anti-emetic therapy. Clinical Research 32: 688A (1984).
Moss, C.L.; Markham, J.K. and Hanasono, G.K.: Studies on the mechanism of neonatal toxicity in rats induced by nabilone, a synthetic 9-ketocannabinoid. Toxicology and Applied Pharmacology 48: A20 (1979).
Nakano, S.; Gillespie, H.K. and Hollister, L.E.: A model for evaluation of antianxiety drugs with the use of experimentally induced stress: Comparison of nabilone and diazepam. Clinical Pharmacology and Therapeutics 23: 54–62 (1978).
Newell, F.W.; Stark, P.; Jay, W.M. and Schanzlin, D.J.: Nabilone: A pressure-reducing synthetic benzopyran in open-angle glaucoma. Ophthalmology 86: 156–160 (1979).
Niamatali, C; Fallon, S.D. and Egan, E.L.: Nabilone in the management of prochlorperazine resistant cancer chemotherapy induced emesis. Irish Medical Journal 77: 276–277 (1984).
Orzelek-O’Neil, R.M.; Goodman, F.R. and Forney, R.B.: The effects of Δ9tetrahydrocannabinol and nabilone on the isolated guinea pig bronchus. Toxicology and Applied Pharmacology 54: 493–500 (1980).
Rubin, A.; Lemberger, L.; Warrick, P.; Crabtree, R.E.; Sullivan, H. et al.: Physiologic disposition of nabilone, a cannabinol derivative, in man. Clin. Pharmacol. Therap. 22: 85–91 (1977).
Stark, P.: The pharmacologic profile of nabilone: A new antiemetic agent. Cancer Treatment Reviews 9(Suppl. B): 11–16 (1982a).
Stark, P.: Study design for the evaluation of the efficacy and safety of nabilone. Cancer Treatment Reviews 9(Suppl. B): 35–37 (1982b).
Stark, R and Dews, P.B.: Cannabinoids II. Cardiovascular Effects. Journal of Pharmacology and Experimental Therapeutics 214: 131–138 (1980a).
Stark, P. and Dews, P.B.: Cannabinoids I. Behavioural Effects. Journal of Pharmacology and Experimental Therapeutics 214: 124–130 (1980b).
Stark, P. and Henderson, J.K.: Increased reactivity in rats caused by septal lesions. International Journal of Neuropharmacology 5: 379–383 (1966).
Steele, N.; Gralla, R.J.; Braun, D.W. and Young, C.W.: Double-blind comparison of the anti-emetic effects of nabilone and prochlorperazine on chemotherapy-induced emesis. Cancer Treatment Reports 64: 219–224 (1980).
Wada, J.K.; Bogbon, D.L.; Gunnell, J.C.; Hum, G.J.; Gota, C.H. and Rieth, T.E.: Double-blind, randomized, crossover trial of nabilone vs placebo in cancer chemotherapy. Cancer Treatment Reviews 9(Suppl. B): 39–44 (1982).
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: O.E. Akwari, Department of Surgery, Duke University Medical Center, Durham, North Carolina, USA; D.N. Bateman, Department of Pharmacological Sciences, University of Newcastle upon Tyne, Newcastle upon Tyne, England; H.L. Borison, Department of Pharmacology and Toxicology, Dartmouth Medical School, Hanover, New Hampshire, USA; J.R.B.J. Brouwers, General Hospital de Tjongerschans, Heerenveen, The Netherlands; L.A. Cone, Eisenhower Medical Center, Rancho Mirage, California, USA; L.E. Einhorn, Indiana University Department of Medicine, Indianapolis, Indiana, USA; D. Greene, Eisenhower Medical Center, Rancho Mirage, California, USA; P.R. Jackson, Department of Therapeutics, Hallamshire Hospital, Sheffield, England; R. Johansson, Department of Radiotherapy and Oncology, University of Kuopio, Kuopio, Finland; S.E. Jones, Cancer Center, University of Arizona, Tucson, Arizona, USA; J. Laszlo, Duke University Medical Center, Durham, North Carolina, USA; M. Levitt, Manitoba Cancer Treatment and Research Foundation, Winnipeg, Canada; J.-R. Malagelada, Gastroenterology Unit, Saint Mary’s Hospital, Rochester, Minnesota, USA; E.E. Müller, Dipartimento di Farmacologia, Chemoterapia e Tossicologia Medica, Universita Degli Studi di Milano, Milan, Italy; G.L. Wampler, Division of Haematology and Oncology, Virginia Commonwealth University, Richmond, Virginia, USA.
‘Cesamet’ (Lilly).
Rights and permissions
About this article
Cite this article
Ward, A., Holmes, B. Nabilone. Drugs 30, 127–144 (1985). https://doi.org/10.2165/00003495-198530020-00002
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-198530020-00002