Summary
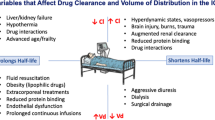
Brain death protocols facilitate early recognition of death in patients on life support systems. When the clinical situation has deteriorated to a level where brain death is to be considered, it is essential that the effects of drugs be excluded. Most centrally acting drugs depress respiration and would be expected to affect apnoea testing of brain stem function. However, the pharmacodynamic and pharmacokinetic properties of drugs are altered when patients are critically ill, so projections made from data derived from less ill patients or normal volunteers are inappropriate. The entry of drugs into the brain is also altered in some disease states, but there are few data relating to the effects of central depressant drugs in the situation of a disrupted blood-brain barrier or brain damage. Drug screens can assist in determining whether drugs are present, but correct interpretation of the results depends on close liaison between the clinical and laboratory staff. It is in the patient’s interests to avoid termination of life support if any centrally active drug is present, unless there are other categorical factors consistent with irreversible brain death, such as demonstrated lack of cerebral blood flow.
Similar content being viewed by others
References
Hutchesson P, Watson B, Schockett W, editors. The All England Law Reports. Airedale NHS Trust vs Bland. 1993 Mar; Pt 10: 821
Brierley JB, Adams JH, Graham DI, et al. Neocortical death after cardiac arrest. Lancet 1971; ii: 560–5
Ad Hoc Committee of the Harvard Medical School to Examine the Definition of Brain Death. A definition of irreversible coma. JAMA 1968; 205(6): 337–40
Diagnosis of brainv death. Statement by the honorary secretary of the Conference of Medical Royal Colleges and their Faculties in the United Kingdom. BMJ 1976; 2: 1187–8
Special Communication. Guidelines for the determination of Death. JAMA 1981; 246(19): 2185–6
Searle J, Collins C. A brain-death protocol. Lancet 1980; i: 641–3
Black PM. Brain death: part I. N Engl J Med 1978; 299(8): 338–44
Black PM. Brain death: part II. N Engl J Med 1978; 299(8): 393–401
Pallis C. ABC of brain stem death: reappraising death. BMJ (Clin Res Ed) 1982; 285: 1409–12
Pallis C. ABC of brain stem death: from brain death to brain stem death. BMJ 1982; 285: 1487–90
Pallis C. ABC of brain stem death: diagnosis of brain stem death −1. BMJ 1982; 285: 1558–60
Pallis C. ABC of brain stem death: diagnosis of brain stem death −2. BMJ 1982; 285: 1643–4
Pallis C. ABC of brain stem death: pitfalls and safeguards. BMJ 1982; 285: 1720–2
Australian and New Zealand Intensive Care Society. Statement and guidelines on brain death and organ donation. Carlton (Vic): Australian and New Zealand Intensive Care Society, 1993
Dobb GJ, Weekes JW. Clinical confirmation of brain death. Anaesth Intensive Care 1995; 23: 37–43
Osternol J. Testing for drugs of abuse: pharmacokinetic considerations for cocaine in urine. Clin Pharmacokinet 1993; 24(5): 255–61
Heinemeyer G. Clinical pharmacokinetic considerations in the treatment of increased intracranial pressure. Clin Pharmacokinet 1987; 13: 1–25
Bodenham A, Shelly M, Park G. The altered pharmacokinetics and pharmacodynamics of drugs commonly used in critically ill patients. Clin Pharmacokinet 1988; 14: 347–73
Bass J, Miles MV, Tennison MB, et al. Effects of enterai tube feeding on the absorption and pharmacokinetic profile of carbamazepine suspension. Epilepsia 1989; 30: 364–9
Randall C, Tett S. Phenytoin pharmacokinetics after intravenous administration to patients receiving enterai tube feeding. Pharm World Sci 1994; 16(4) 217–24
Cumming JF. The effect of arterial oxygen tension on antipyrine half-time in plasma. Clin Pharmacol Ther 1976; 19: 468–71
Perkins MW, Dasta JF, DeHaven B. Physiologic implications of mechanical ventilation on pharmacokinetics. Ann Pharmacother 1989; 23: 316–23
Milne RW, Nation RL, Somogyi AA, et al. The influence of renal function on the renal clearance of morphine and its glucuronide metabolites in intensive care patients. Br J Clin Pharmacol 1992; 34: 53–9
Boucher BA, Khul DA, Fabian TC, et al. The effect of neurotrauma on hepatic drug clearance. Clin Pharmacol Ther 1991; 5(1): 487–97
De Boer AG, Breimer DD. The blood-brain barrier: implications for drug delivery to the brain. J R Coll Physicians Lond 1994; 28(6): 502–6
Bradbury MWB. The blood-brain barrier. Exp Physiol 1993; 78: 453–72
Reese TS, Karnovsky MJ. Fine structural localisation of a blood-brain barrier to exogenous peroxidase. J Cell Biol 1967; 34: 207–17
Bonati M, Kanto J, Tognoni G. Clinical pharmacokinetics of cerebrospinal fluid. Clin Pharmacokinet 1982; 7: 312–35
Brodie B, Kurtz H, Schanker L. The importance of dissociation constant and lipid solubility in influencing the passage of drugs into the cerebrospinal fluid. J Pharmacol Exp Ther 1960; 130: 20–5
Crone C. The permeability of brain capillaries to non-electrolytes. Acta Physiol Scand 1965; 64: 407–17
Van Bree JBM, DeBoer AG, Danhof M, et al. Characterisation of an ‘in vitro’ blood brain barrier: effects of molecular size and lipophilicity on cerebrovascular endothelial transport rates of drugs. J Pharmacol Exp Ther 1988; 247(3): 1233–9
Joo F, Klatzo I. Role of cerebral endothelium in brain oedema. Neurol Res 1989; 11: 67–75
Bullock R, Fujisawa H. The role of glutamate antagonists for the treatment of CNS injury. J Neurotrauma 1992; 9 Suppl. 2: 443–61
Benzel EC, Gross CD, Hadden TA, et al. The apnea test for determination of brain death. J Neurosurg 1989; 71: 191–4
Berger AJ, Mitchell RA, Severingham JW. Regulation of respiration: part I. N Engl J Med 1977; 297(2): 92–7
Berger AJ, Mitchell RA, Severingham JW. Regulation of respiration: part II. N Engl J Med 1977; 297(3): 138–43
Berger AJ, Mitchell RA, Severingham JW. Regulation of respiration: part III. N Engl J Med 1977; 297(4): 194–201
Nunn JF. Control of breathing. Nunn’s applied respiratory physiology. 4th ed. London: Butterworth, 1993 90–116
Cohn MA. Hypnotics and the control of breathing: a review. Br J Clin Pharm 1983: 16 Suppl.: 245–50
Olson KR, Pentel PR, Kelley MT. Physical assessment and differential diagnosis of the poisoned patient. Med Toxicol 1987; 2: 52–81
Lipton SA, Rosenberg PA. Excitatory amino acids as a final common pathway for neurological disorders. N Engl J Med 1994; 330(9): 613–20
Mandema JW, Danhof M. Electroencephalogram effect measures and relationship between pharmacokinetics and pharmacodynamics of centrally acting drugs. Clin Pharmacokinet 1992; 23(3): 191–215
Powner DJ. Drug associated isoelectric EEGs: a hazard in braindeath certification. JAMA 1976; 236: 1123
Setzer N. Brain death: physiologic definitions. Crit Care Clin 1985; 1(2): 375–96
Taylor MJ, Houston BD, Lowry NJ. Recovery of auditory brainstem responses after a severe hypoxic ischaemic insult. N Engl J Med 1983; 309: 1169–70
Levine SR, Brust JCM, Furtell N, et al. Cerebrovascular complications of the use of the ‘crack’ form of alkaloidal cocaine. N Engl J Med. 1990; 323: 699–704
Bucthal F, Svensmark O, Schiller PJ. Clinical and electroen-cephalographic correlation with serum levels of diphenylhydantoin. Arch Neurol 1960; 2: 624–30
Lund L. Anticonvulsant effect of diphenylhydantoin relative to plasma levels. Arch Neurol 1974; 31(5): 289–94
Ingelfinger JA, Isakson G, Shine D, et al. Reliability of the toxic screen in overdose. Clin Pharmacol Ther 1981; 29(5) 570–95
Spiechler VR, O’Donnell CM, Gokhale DV. Confirmation and certainty in toxicology screening. Clin Chem 1988; 34(8) 1535–9
Op de Coul AAW, Lambregts PCLA, Koeman J, et al. Neuromuscular complications in patients given Pavulon® (pancuronium bromide) during artificial ventilation. Clin Neurol Neurosurg 1985; 87(1): 17–22
Belaesky M, Kalwans HI. Prolonged neuromuscular blockade with pancuronium bromide in a young healthy woman. Anaesthesiology 1971; 40(3): 295–6
Segredo V, Caldwell JE, Marthay MA, et al. Persistent paralysis in critically ill patients after long-term administration of vecuronium. N Engl J Med 1992; 327: 524–8
Tyson RN. Simulation of cerebral death by succinylcholine sensitivity. Arch Neurol 1974; 30: 409–11
Shapiro HM. Barbiturates in brain ischaemia. Br J Anaesth 1985; 57: 82–95
Scatton B, Carter C, Benavides J, et al. N-Methyl-D-Aspartate receptor antagonists: a novel therapeutic perspective for the treatment of ischaemic brain injury. Cerebrovasc Dis 1991; 1: 121–35
Fitzpatrick AJ, Crawford M, Allan RM, et al. Aconite poisoning managed with a ventricular assist device. Anaesth Intensive Care 1994; 22: 714–7
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kennedy, M., Kiloh, N. Drugs and Brain Death. Drug-Safety 14, 171–180 (1996). https://doi.org/10.2165/00002018-199614030-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/00002018-199614030-00004