Summary
Synopsis
Nimodipine is a dihydropyridine calcium antagonist which has been shown to dilate cerebral arterioles and increase cerebral blood flow in animals and humans. It has potential in the treatment of a range of cerebrovascular disorders. Major interest to date, however, has focused on its use in the prevention and treatment of the delayed ischaemic neurological deficits that frequently occur in patients with subarachnoid haemorrhages as a result of sustained cerebral vasospasm.
Initial studies in which patients were treated with an intravenous infusion of nimodipine for up to 2 weeks, followed by oral treatment for 7 days, indicated that a higher proportion of patients than would normally be expected recovered with little or no permanent neurological damage. In a number of controlled studies oral nimodipine treatment for 3 weeks significantly decreased mortality rates and increased the number of patients who had a ‘good’ neurological outcome as compared with placebo treatment. In some of these trials fewer of the nimodipine-treated patients developed neurological deficits during the treatment period, but in none was there a significant effect on the incidence of angiographic vasospasm. It would seem that other pharmacological actions, such as increasing collateral blood flow to underperfused regions or a direct anti-ischaemic effect at the cellular level, may contribute to the clinical benefits obtained with nimodipine treatment. Preliminary results suggest that nimodipine is potentially useful in other cerebrovascular disorders, particularly ischaemic stroke.
To date, nimodipine has been well-tolerated, the only adverse effects of any significance being reductions in the blood pressure of some patients and reversible increases in liver enzymes during intravenous therapy. Thus, nimodipine has significant potential in the treatment of patients with subarachnoid haemorrhage. Wider clinical use should confirm its value as a significant addition to the very limited range of therapeutic choices currently available for patients with this disorder.
Pharmacodynamic Studies
Nimodipine is a dihydropyridine calcium antagonist which relaxes arterial smooth muscle in the presence of agonist-induced increased tone. In in vitro preparations it demonstrates a marked specificity for cerebral vessels. Following intravenous and intraperitoneal doses of nimodipine, dilation of cerebral arterioles has been demonstrated in vivo in animals, and similar results have been reported following the topical application of a nimodipine solution to exposed vessels. Several studies have shown that there is a preferential effect of nimodipine on arterioles with a diameter < 70 to 100μm. Direct observations of cerebral arteriole dilation have also been made in patients undergoing cranial surgery who received nimodipine 10 μg/kg as an intravenous infusion over 10 minutes. In animal studies intravenous or intracortical doses of nimodipine up to 0.1 μg/kg/min increased cerebral blood flow (CBF) by between 18 and 170% without significantly decreasing arterial blood pressure, although it would seem that this effect is only seen when cerebrovascular resistance is raised. Oral doses of nimodipine 40 to 80mg and intravenous doses of 15 to 30 μg/kg increased CBF by up to 18% in patients with subarachnoid haemorrhage (SAH), with no evidence of a ‘cerebral steal’ syndrome where blood flow is diverted to healthy tissue at the expense of ischaemic regions.
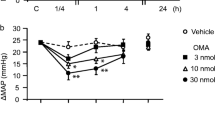
In patients with SAH infusion of nimodipine 1 mg/h, increased to 2 mg/h after 2 hours, had no significant effects on blood pressure or heart rate when given for up to 14 days, except in patients who were hypertensive before the start of treatment. However, if the infusion was started at the higher rate of 2 mg/h, systolic and diastolic blood pressures decreased over 3 to 4 hours by about 30 and 20mm Hg, respectively, partially recovered and then remained stable at this level for the duration of treatment.
When tested in non-primate animal models where experimental SAH was produced by injection of blood into the subarachnoid space, intrathecal administration of nimodipine was found to reverse both acute and delayed vasospasms of cerebral arteries. However, neither intrathecal nor intravenous doses of nimodipine up to 12 mg/kg 3 times daily had any effect on the occurrence of vasospasm or neurological deficits in primates subjected to experimental SAH by the surgical implantation of an autologous haematoma into the subarachnoid space. In animal models of total or partial cerebral ischaemia pretreatment with nimodipine increased post-ischaemic CBF values, reduced the extent of ischaemic damage, and improved neurological recovery in most studies, whereas only half the investigations where treatment was just given in the post-ischaemic stage were able to demonstrate any beneficial effects of nimodipine.
In healthy volunteers single oral doses up to 60mg produced modest improvements in self-rated alertness, and doses of 40 or 60mg given to elderly patients with mild cerebrovascular insufficiency tended to stabilise EEG determinants of vigilance.
Pharmacokinetic Properties
Intravenous infusions of nimodipine at rates of approximately 2 mg/h have resulted in mean steady-state plasma concentrations of 27 to 53 μg/L in patients with SAH, while single oral 60mg doses (in tablet form) given to healthy volunteers have produced maximum plasma concentrations of up to 31 μg/L within 1 hour of administration. Mean AUC values following 60mg oral doses have ranged from 42 to 125 μg/L · h, and other studies in volunteers showed reasonable linearity between oral dosage of nimodipine (up to 80mg) and both maximum plasma concentrations and AUC values. Despite the fact that nimodipine is well absorbed from the alimentary tract, considerable first-pass metabolism reduces the oral bioavailability to between 5 and 13% in volunteers and between 3 and 28% in patients with SAH.
Following intravenous administration there is an initial rapid distribution of nimodipine into the central compartment (half-life = 7 minutes, initial volume of distribution = 0.43 L/kg), presumably followed by a slower distribution into tissue sites. The volume of distribution at steady-state has been estimated at between 0.94 and 2.3 L/kg following intravenous administration. Only a small proportion of circulating nimodipine passes into the cerebrospinal fluid — a CSF concentration of 0.3 μg/L corresponded to a plasma concentration of 77 μg/L in SAH patients — reflecting the fact that nimodipine is extensively (about 98%) bound by plasma proteins.
The primary stages in the metabolism of nimodipine are demethylation and dehydrogenation of the dihydropyridine nucleus to produce an inactive pyridine analogue which is then further metabolised to a variety of plasma and urinary species. Approximately 50% of an oral dose is excreted as metabolites in the urine within 4 days. The elimination half-life of nimodipine following intravenous administration was 0.9 to 1.5 hours, while oral studies in volunteers produced longer values of between 1.7 and 7.2 hours.
Patients with liver disease have impaired clearance of nimodipine (mean total clearances of 158 to 217 L/h vs 420 to 519 L/h in healthy controls) but this only produced a noticeable increase in elimination half-life when nimodipine was given sublingually (18 vs 6.2 hours in controls). Similarly, the elimination half-life was much longer in elderly patients with renal failure (22 hours) compared with younger volunteers (3 hours), but it is not known whether this is due to impaired renal function or the effects of increasing age.
Therapeutic Trials
In non-comparative studies of patients with SAH who, in addition to standard treatment, received intravenous nimodipine 1 to 2 mg/h for 7 to 14 days, followed by oral treatment of 45 to 60mg every 4 hours for up to 7 days, overall neurological outcome (assessed at the end of treatment or after up to 3 years) was considered good in 60 to 78% of patients and mortality rates were 2 to 13%. In other, independent series of patients who underwent standard therapeutic procedures only, good recovery was obtained in 42 to 56% of those studied and 28 to 39% of patients died. A limited number of double-blind randomised trials have compared the effects of oral treatment with nimodipine 0.35 mg/kg to 90mg every 4 hours for 21 days with those of placebo treatment. Some of these assessed overall neurological outcome in all patients at 3 months and it was reported that there was a significant reduction in mortality (4 vs 24%; p < 0.01) or an increase in the percentage of patients who had little or no permanent neurological damage (29 vs 10%; p < 0.01) in the groups who received nimodipine. Furthermore, in 1 study fewer patients receiving nimodipine developed delayed neurological deficits during the treatment period (8% vs 29% for placebo). In the largest such trial to date (n = 554), nimodipine reduced the incidence of cerebral infarction by 34% (p < 0.005) and of poor outcomes by 40% (p < 0.001) versus placebo. The other studies concentrated on those patients who developed vasospasm-related neurological deficits during treatment; in 1 of these trials nimodipine reduced the incidence of deficits, the severity of neurological impairment was consistently reduced, and in 1 study there was a slight decrease in mortality. Similar results have been obtained with intravenous administration. In none of the comparative studies did nimodipine treatment actually reduce the incidence of angiographic cerebral vasospasm, and it is possible that the clinical benefits of nimodipine are the result of increased collateral blood supply to ischaemic tissues or a direct antiischaemic effect at the cellular level.
Preliminary studies have shown that oral treatment with nimodipine 120 mg/day for 28 days significantly reduced mortality and improved neurological recovery of patients who had suffered an acute ischaemic stroke. Additionally, the results of a number of small scale trials indicate that prophylactic treatment with nimodipine 120 mg/day reduces the frequency of migraine attacks in patients with common or classical disease, and may also lessen the duration and severity of attacks.
Adverse Effects
Nimodipine is generally well-tolerated, with hypotension being the only adverse effect reported more frequently than with placebo treatment. The incidence of hypotension in studies of patients with SAH was 4.7 to 8%, while a total of 21% of patients who received nimodipine noted adverse effects of any type, compared with 25% of patients who received placebo in 1 double-blind comparative study. Increased serum concentrations of liver enzymes have been observed in patients during intravenous treatment with nimodipine; these have always been reversible and are thought to be produced by ethanol in the intravenous formulation rather than nimodipine per se. There have been single reports of confusion with psychosis and possible myocardial ischaemia during nimodipine treatment.
Dosage and Administration
Treatment of patients with SAH should be started as soon after the initial haemorrhage or the development of neurological deficit as possible. Oral treatment can be given at a dosage of 60mg every 4 hours for 21 days. Alternatively, treatment can initially be an intravenous infusion of 1 mg/h. Provided that blood pressure remains stable this can be increased after 2 hours to 2 mg/h, then continued for 5 to 14 days, and followed by oral treatment of 60mg every 4 hours for up to 7 days. If treatment is started prior to surgery it should be continued for at least 5 days after the operation. For patients with low bodyweight, unstable blood pressure or impaired liver function a lower starting dose of intravenous nimodipine 0.5 mg/h (or 30mg orally every 4 hours) may be more suitable. Renal function should be monitored in patients known to have kidney disease.
Similar content being viewed by others
References
Allen GS, Ahn HS, Preziosi TJ, Battye R, Boone SC, et al. Cerebral arterial spasm: a controlled trial of nimodipine in patients with subarachnoid hemorrhage. New England Journal of Medicine 308: 619–624, 1983
Alps BJ, Calder C, Hass WK, Wilson AD. Comparative protective effects of nicardipine, flunarizine, lidoflazine and nimodipine against ischaemic injury in the hippocampus of the mongolian gerbil. British Journal of Pharmacology 93: 877–883, 1988
Altura BM, Altura BT, Gelbrewold A. Comparative microvascular actions of Ca2+antagonists. In Merril & Weiss (Eds) Ca2+entry blockers, adenosine and neurohumors, pp. 155–175, Urban & Schwarzenberg, Baltimore, 1983
Andersson K-E, Edvinsson L, MacKenzie ET, Skärby T, Young AR. Influence of extracellular calcium and calcium antagonists on contractions induced by potassium and prostaglandin F2αin isolated cerebral and mesenteric arteries of the cat. British Journal of Pharmacology 79: 135–140, 1983
Auer LM. Pial arterial and venous reaction to intravenous infusion of nimodipine in cats. Journal of Neurosurgical Science 26: 213–218, 1982
Auer LM. Acute operation and preventive nimodipine improve outcome in patients with ruptured cerebral aneurysms. Neurosurgery 15: 57–66, 1984
Auer LM, Brandt L, Ebeling U, Gilsbach J, Groeger U, et al. Nimodipine and early aneurysm operation in good condition SAH patients. Acta Neurochirurgica 82: 7–13, 1986
Auer LM, Mokry M. Effect of topical nimodipine versus its ethanol-containing vehicle on cat pial arteries. Stroke 17: 225–228, 1985
Auer LM, Oberbauer RW, Schalk HV. Human pial vascular reactions to intravenous nimodipine infusion during EC-IC bypass surgery. Stroke 14: 210–213, 1983
Auer LM, Reulen HJ, Gilsbach J, Oppel F, Gröger U, et al. Prevention of brain infarction from arterial spasm by acute aneurysm surgery and preventive nimodipine treatment in patients with subarachnoid hemorrhage. In Betz et al. (Eds) Nimodipine. Pharmacological and Clinical Properties, pp. 398–408, Schattauer Verlag, Stuttgart, 1985
Auer LM, Suzuki A, Yasui N, Ito Z. Intraoperative topical nimodipine after aneurysm clipping. Neurochirurgia 27: 36–38, 1984
Baethmann A, Jansen M. Possible role of calcium entry blockers in brain protection. European Neurology 25 (Suppl. 1): 102–114, 1986
Barnett GH, Bose B, Little JR, Jones SC, Friel HT. Effects of nimodipine on acute focal cerebral ischaemia. Stroke 17: 884–890, 1986
Battye R. Plasma and cerebrospinal fluid levels after oral doses of nimodipine. In Battye R. (Ed.) Calcium antagonists: possible therapeutic use in neurosurgery. Proceedings of a Workshop, Dorado Beach, Puerto Rico, June 10–11, 1983, pp. 62–64, 1984
Bianchi AP, Viglianesi MS. Hemorrheological effects of dihydropyridine calcium entry blockers. Naunyn Scheideberg’s Archives of Pharmacology (abstract no. 154) 330: 87, 1985
Boldt J, Bormann B, Kling D, Ratthey K, Hempelmann G. Influence of nimodipine and nifedipine on intrapulmonary shunting: a comparison to other vasoactive drugs. Intensive Care Medicine 13: 52–56, 1987
Bormann B, Boldt J, Kling D, Mulch J, Weidler B, et al. Influence of nimodipine on cardiovascular parameters during coronary surgery. Neurochirurgia 28: 79–83, 1985
Brandt L, Andersson K-E, Edvinsson L, Ljunggren B. Effects of extracellular calcium and of calcium antagonists on the contractile responses of isolated human pial and mesenteric arteries. Journal of Cerebral Blood Flow and Metabolism 1: 339–347, 1981
Brandt L, Ljunggren B, Säveland H, Andersson K-A, Vinge E. Cerebral vasospasm and calcium channel blockade. Acta Pharmacologica 58 (Suppl. 2): 151–155, 1986
Bunnel OS, Louis TM, Saldanha RL, Kopelman AE. Protective actions of the calcium antagonists, flunarizine and nimodipine, on cerebral ischaemia. Medical Science Research 15: 1513–1514, 1987
Bussone G, Baldini S, O’Andrea G, Cananzi A, Frediani F, et al. Nimodipine versus flunarizine in common migraine; a controlled pilot trial. Headache 27: 76–79, 1987
Cauvin C, Loutzenhiser R, van Breemen C. Mechanisms of calcium antagonist-induced vasodilation. Annual Review on Pharmacology and Toxicology 23: 373–396, 1983
Dompert WU, Traber J. Binding sites for dihydropyridine calcium antagonists. Perspectives in Cardiovascular Research 9: 175–179, 1984
Espinosa F, Weir B, Overton T, Castor W, Grace M, et al. A randomized placebo-controlled double-blind trial of nimodipine after SAH in monkeys. Journal of Neurosurgery 60: 1167–1175, 1984
Fleckenstein-Grün G, Frey M, Makita Y, Byon YK. New pharmacological aspects of various dihydropyridine calcium antagonists with regard to smooth muscle relaxation. In Lichtlen PR (Ed.) Recent aspects in calcium antagonism, pp. 29–46, Schattauer Verlag, Stuttgart, 1985
Forsman M, Fleischer JE, Milde JH, Steen PA, Michenfelder JD. The effects of nimodipine on cerebral blood flow and metabolism. Journal of Cerebral Blood Flow and Metabolism 6: 763–767, 1986
Fujisawa A, Matsumoto M, Matsuyama T, Ueda H, Wanaka A, et al. The effect of the calcium antagonist nimodipine on the gerbil model of experimental cerebral ischaemia. Stroke 17: 748–752, 1986
Gaab MR, Haubitz I, Brawanski A, Korn A, Czech Th. Acute effects of nimodipine on the cerebral floow flow and intracranial pressure. Neurochirurgia 28: 93–99, 1985
Gawel M. A double-blind, crossover study of nimodipine versus pizotyline in common and classical migraine. Cephalalgia 7 (Suppl. 6): 453–454, 1987
Gelmers HJ. Effect of nimodipine (Bay e 9736) on postischaemic cerebrovascular reactivity, as revealed by measuring regional cerebral blood flow (rCBF). Acta Neurochirurgica 63: 283–290, 1982
Gelmers HJ. Nimodipine, a new calcium antagonist in the prophylactic treatment of migraine. Headache 23: 106–109, 1983
Gelmers HJ. The effects of nimodipine on the clinical course of patients with acute ischaemic stroke. Acta Neurologica Scandinavica 69: 232–239, 1984
Gelmers HJ, Gorter K, de Weerdt CJ, Weizer HAJ. A controlled trial of nimodipine in acute ischaemic stroke. New England Journal of Medicine 318: 203–207, 1988
Gengo FM, Fagan SC, Krol G, Bernhard H. Nimodipine disposition and haemodynamic effects in patients with cirrhosis and age-matched controls. British Journal of Clinical Pharmacology 23: 47–53, 1987
Germano IM, Bartkowski HM, Cassel ME, Pitts LH. The therapeutic value of nimodipine in experimental focal cerebral ischaemia. Journal of Neurosurgery 67: 81–87, 1987
Gioia AE, White RP, Bakhtian B, Robertson JT. Evaluation of the efficacy of intrathecal nimodipine in canine models of chronic cerebral vasospasm. Journal of Neurosurgery 62: 721–728, 1985
Glossmann H, Go UA, Rombusch M, Ferry DR. Molecular pharmacology of Ca2+channels: receptor binding studies. In Betz et al. (Eds) Nimodipine: pharmacological and clinical properties, pp. 147–161, Schattauer Verlag, Stuttgart, 1985
Gotoh O, Mohamed AA, McCulloch J, Graham DJ, Harper AM, et al. Nimodipine and the haemodynamic and histopathological consequences of middle cerebral artery occlusion in the rat. Journal of Cerebral Blood Flow and Metabolism 6: 321–331, 1986
Gould RJ, Murphy KMM, Snyder SH. A simple sensitive radio-receptor assay for calcium antagonist drugs. Life Sciences 33: 2665–2672, 1983
Grabowski M, Johansson BB. Nifedipine and nimodipine: effect on blood pressure and regional cerebral blood flow in conscious normotensive and hypertensive rats. Journal of Cardiovascular Pharmacology 7: 1127–1133, 1985
Hakim AM. Cerebral acidosis in focal ischaemia II: nimodipine and verapamil normalize cerebral pH following middle cerebral artery occlusion in the rat. Journal of Cerebral Blood Flow and Metabolism 6: 676–683, 1986
Harper AM, Craigen L, Kazda S. Effect of the calcium antagonist, nimodipine, on cerebral blood flow and metabolism in the primate. Journal of Cerebral Blood Flow and Metabolism 1: 349–356, 1981
Harris RJ, Branston NM, Symon L, Bayhan M, Watson A. The effects of a calcium antagonist, nimodipine, upon physiological responses of the cerebral vasculature and its possible influence upon focal cerebral ischaemia. Stroke 13: 759–766, 1982
Havanka-Kanniaianen H, Hokkanen E, Myllylä VV. Efficacy of nimodipine in the prophylaxis of migraine. Cephalalgia 5: 39–43, 1985a
Havanka-Kanniainen H, Hokkanen E, Myllylä V. Efficacy of nimodipine in comparison with pizotifen (Sandomigrin) in the prophylaxis of migraine. Cephalalgia 5 (Suppl. 3): 530–531, 1985b
Haws CW, Gourley JK, Heistad DD. Effects of nimodipine on cerebral blood flow. Journal of Pharmacology and Experimental Therapeutics 225: 24–48, 1983
Haws CW, Heistad DD. Effects of nimodipine on cerebral vasoconstrictor responses. American Journal of Physiology 247: H170–H176, 1984
Hess P, Lansman JB, Tsien RW. Different modes of Ca channel gating behaviour favoured by dihydropyridine Ca agonists and antagonists. Nature 311: 538–544, 1984
Hoffmeister F, Benz U, Heise A, Krause HP, Neuser V. Behavioural effects of nimodipine in animals. Arzneimittel-Forschung 32: 347–360, 1982
Hunt WE, Hess RH. Surgical risk as related to time of intervention in the repair of intracranial aneurysms. Journal of Neurosurgery 28: 14–20, 1968
Itil TM, Itil KZ. The comparative CNS pharmacology of nimodipine in humans. In Betz et al. (Eds) Nimodipine: pharmacological and clinical properties, pp. 185–202, Schattauer Verlag, Stuttgart, 1985
Itil TM, Michael ST, Hoffmeister F, Kunitz A, Eral E. Nimodipine, a calcium antagonist vasodilator with psychotropic properties (a controlled quantitative pharmaco-EEG study). Current Therapeutic Research 35: 405–422, 1984
Jakobsen P, Lederballe Pederson O, Mikkelson E. Gas Chromatographic determination of nifedipine and one of its metabolites using electron capture detection. Journal of Chromatography 162: 81–87, 1979
Jakobsen P, Mikkelsen EO, Laursen J, Jensen F. Determination of nimodipine by gas chromatography using electron-capture detection; external factors influencing nimodipine concentrations during intravenous administration. Journal of Chromatography 374: 383–387, 1986
James IM, Savage IT. Nimodipine on cerebral blood flow and alertness in man. In Lechner & Ladurner (Eds) Progress in pathophysiology, diagnosis and therapy of cerebrovascular diseases, pp. 142–149, Excerpta Medica, 1984
Jan M, Buchheit F, Tremoulet M. Therapeutic trial of intravenous nimodipine in patients with established cerebral vaso-spasms after rupture of intracranial aneurysms. Neurosurgery 23: 154–157, 1988
Janis RA, Krol GJ, Noe AJ, Pan M. Radioreceptor and high-performance liquid Chromatographic assays for the calcium channel antagonist nitrendipine in serum. Journal of Clinical Pharmacology 23: 266–273, 1983
Janis RA, Triggle DJ. 1,4-dihydropyridine Ca2+channel antagonists and activators: a comparison of binding characteristics with pharmacology. Drug Development Research 4: 257–274, 1984
Jansen I, Edvinsson L. Effects of extracellular calcium and of the calcium entry blockers flunarizine and nimodipine on contractile responses in human temporal arteries. Cephalalgia 6: 235–240, 1986
Jennet B, Bond M. Assessment of outcome after severe brain damage. Lancet 1: 480–484, 1975
Kamath B, Lettieri J, Krol G, Raemusch K, Yeh S, et al. Pharmacokinetics and metabolism of radiolabeled nimodipine. Pharmacological Research 4 (Suppl. 2): S80, 1987
Kanda K, Flaim SF. Effects of nimodipine on cerebral blood flow in conscious rat. Journal of Pharmacology and Experimental Therapeutics 236: 41–47, 1986
Kassell NF. The natural history and treatment outcome of SAH: comments derived from the National Cooperative Aneurysm Study. In Battye R (Ed.) Calcium antagonists: possible therapeutic use in neurosurgery. Proceedings of a Workshop, Dorado Beach, Puerto Rico, June 10–11, 1983, pp. 62–64, 1984
Kazda S. Garthoff B, Krause HP, Schloβmann K. Cerebrovascular effects of the calcium antagonistic dihydropyridine derivative nimodipine in animal experiments. Arzneimittel-Forschung 32: 331–338, 1982
Kazda S, Garthoff B, Luckhaus G. Calcium antagonists prevent brain damage in stroke-prone spontaneously hypertensive rats independent of their effect on blood pressure. Journal of Cerebral Blood Flow and Metabolism 3 (Suppl. 1): S526–S527, 1983a
Kazda S, Hoffmeister F, Garthoff B, Towart R. Prevention of the postischaemic impaired reperfusion of the brain by nimodipine (Bay e 9736). Acta Neurologica Scandinavica 60 (Suppl. 72): 302–303, 1979
Kazda S, Knorr A, Towart R. Common properties and differences between various calcium antagonists. Progress in Pharmacology 5: 83–116, 1983b
Kazner F, Sprung CL, Adelt D, Ammerer HP, Karnick R, et al. Clinical experience with nimodipine in the prophylaxis of neurological deficits after subarachnoid haemorrhage. Neurochirurgia 28 (Suppl. 1): 110–113, 1985
Kieswetter H, Jung F, Radtke H, Roggenkamp G, Schneider R. Investigation of the Theological effectiveness of nimodipine in comparison to other established rheologica with an in vitrostress model with calcium. In Betz et al. (Eds) Nimodipine. Pharmacological and Clinical Properties, pp. 127–135, Schattauer Verlag, Stuttgart, 1985
Kirch W, Rämsch K-D, Dührsen U, Ohnhaus EE. Clinical pharmacokinetics of nimodipine in normal and impaired renal function. International Journal of Clinical Pharmaceutical Research 4: 381–384, 1984
Kistler JP, Ropper AH, Martin JB. Cerebrovascular diseases. In Braunwald et al. (Eds) Harrison’s principles of internal medicine, 11th ed., Vol. 2, pp. 1930–1960, McGraw-Hill, New York, 1987
Koos WT, Perneczky A, Auer LM, Böker DK, Graab M, et al. Nimodipine treatment of ischaemic neurological deficits due to cerebral vasospasm after subarachnoid haemorrhage. Neurochirurgia 28 (Suppl. 1): 114–117, 1985
Krol GJ, Noe AJ, Yeh SC, Raemsch KD. Gas and liquid Chromatographic analyses of nimodipine calcium antagonist in blood plasma and cerebrospinal fluid. Journal of Chromatography 305: 105–118, 1984
Laursen J, Jensen F, Mikkelsen E, Jakobsen P. Nimodipine treatment of subarachnoid hemorrhage. Clinical Neurology and Neurosurgery 90: 329–337, 1988
Lewis PJ, Weir BKA, Nosko MG, Tanabe T, Grace MG. Intrathecal nimodipine therapy in a primate model of chronic cerebral vasospasm. Neurosurgery 22: 492–500, 1988
Ljunggren B, Brandt L, Säveland H. Management of aneurysmal subarachnoid hemorrhage. In Vincent JL (Ed.) Update in intensive care and emergency medicine, pp. 179–184, Springer-Verlag, Berlin, 1985
Ljunggren BCA, Brandt JL, Säveland HG. Outcome in patients subjected to early aneurysm operation and intravenous nimodipine. Minerva Medica 77: 1087–1092, 1986
Ljunggren B, Brandt L, Säveland H, Nilsson P-E, Cronqvist S, et al. Outcome in 60 consecutive patients treated with early aneurysm operation and intravenous nimodipine. Journal of Neurosurgery 61: 864–873, 1984
Mabe H, Nagai H, Takagi T, Umemura S, Ohno M. Effect of nimodipine on cerebral function and metabolic recovery following ischaemia in the rat brain. Stroke 17: 501–505, 1986
Mannhold R. Calcium antagonists: basic chemical and pharmacological properties. Drugs of Today 20: 69–90, 1984
McCalden TA, Nath RG, Thiele K. The effects of a calcium antagonist (Nimodipine) on basal cerebral blood flow and reactivity to various agonists. Stroke 15: 527–530, 1984
Mee E, Dorrance D, Lowe D, Neil-Dwyer G. Controlled study of nimodipine in aneurysm patients treated early after subarachnoid haemorrhage. Neurosurgery 22: 484–491, 1988
Meyer H, Wehinger E, Bosserk F, Scherling D. Nimodipine: synthesis and metabolic pathway. Arzneimittel-Forschung 33(1): 106–112, 1983
Michenfelder JD, Milde JH. Nimodipine does not affect cerebral lactate levels following complete ischaemia in dogs. Journal of Cerebral Blood Flow and Metabolism 7: 619–624, 1987
Micieli G, Trucco M, Agostinis C, Mancuso A, Papalia F, et al. Nimodipine vs pizotifen in common migraine: result of a double-blind cross-over trial. Cephalalgia 5 (Suppl. 3): 532–533, 1985
Mohamed AA, Gotoh O, Graham DI, Osborne KA, McCulloch J, et al. Effect of pretreatment with the calcium antagonist nimodipine on local cerebral blood flow and histopathology after middle cerebral artery occlusion. Annals of Neurology 18: 705–711, 1985
Mohamed AA, McCulloch J, Mendelow AD, Teasdale GM, Harper AM. Effect of the calcium antagonist nimodipine on local cerebral blood flow: relationship to arterial pressure. Journal of Cerebral Blood Flow and Metabolism 4: 206–211, 1984
Müller-Schweinitzer E, Neumann P. In vitroeffects of calcium antagonists PN200-110, nifedipine, and nimodipine on human and canine cerebral arteries. Journal of Cerebral Blood Flow and Metabolism 3: 354–361, 1983
Newberg Milde L, Milde JH, Michenfelder JD. Delayed treatment with nimodipine improves cerebral blood flow after complete cerebral ischaemia in the dog. Journal of Cerebral Blood Flow and Metabolism 6: 332–337, 1986
Nosko M, Weir B, Krueger C, Cook D, Norris S, et al. Nimodipine and chronic vasospasm in monkeys. Part 1: clinical and radiological findings. Neurosurgery 16: 129–136, 1985
Ohman J, Heiskanen O. Effect of nimodipine on the outcome of patients after aneurysmal subarachnoid haemorrhage and surgery. Journal of Neurosurgery 69: 683–686, 1988
Onoda JM, Sloane BF, Honn KV. Antithrombogenic effects of calcium channel blockers: synergism with prostacyclin and thromboxane synthetase inhibitors. Thrombosis Research 34: 367–378, 1984
Peroutka SJ, Banghart SB, Allen GS. Relative potency and selectivity of calcium antagonists used in the treatment of migraine. Headache 24: 55–58, 1984
Petruk KC, West M, Mohr G, Weir BKA, Benoit BG, et al. Nimodipine treatment in poor-grade aneurysm patients. Journal of Neurosurgery 68: 505–517, 1988
Philippon J, Grob R, Dagreou F, Guggiari M, Rivierez M, et al. Prevention of vasospasm in subarachnoid haemorrhage: a controlled study with nimodipine. Acta Neurochirurgica 82: 110–114, 1986
Pickard JD, Murray GD, Illingworth R, Shaw MDM, Teasdale GM, et al. Effect of oral nimodipine on cerebral infarction and outcome after subarachnoid haemorrhage: British aneurysm nimodipine trial. British Medical Journal 298: 636–642, 1989
Rämsch K-D, Ahr G, Tettenborn D, Auer LM. Overview on pharmacokinetics of nimodipine in healthy volunteers and in patients with subarachnoid hemorrhage. Neurochirurgia 28: 74–78, 1985a
Rämsch K-D, Graefe K-H, Scherling D, Sommer J, Ziegler R. Pharmacokinetics and metabolism of calcium-blocking agents nifedipine, nitrendipine and nimodipine. American Journal of Nephrology 6: 73–80, 1986
Rämsch K-D, Graefe K-H, Sommer J. Pharmacokinetics and metabolism of nimodipine. In Betz et al. (Eds) Nimodipine: pharmacological and clinical properties, pp. 147–161, Schattauer Verlag, Stuttgart, 1985b
Rämsch K-D, Lücker PW, Wetzelsburger N. Pharmacokinetics of intravenously and orally administered nimodipine. Clinical Pharmacology and Therapeutics 41: 216, 1987
Rosenblum WI. Effects of calcium channel blockers on pial vascular responses to receptor mediated constrictors. Stroke 15: 284–287, 1984
Rosenwasser RH, Buchheit WA, Truex RC. Management of subarachnoid haemorrhage. Pennsylvania Medicine 87: 72–76, 1984
Saltiel E, Ellrodt AG, Monk JP, Langley MS. Feldopine: a review of its pharmacodynamic and pharmacokinetic properties, and therapeutic use in hypertension. Drugs 36: 387–428, 1988
Schmidli J, Santillan GG, Saeed M, Palmieri D, Bing RJ. The effect of nimodipine, a calcium antagonist, on intracortical arterioles in the cat brain. Current Therapeutic Research 38: 94–103, 1985
Schmunk GA, Lefer AM. Anti-aggregatory actions of calcium channel blockers in cat platelets. Research Communications in Chemical Pathology and Pharmacology 35: 179–187, 1982
Seiler RW, Grolimund P, Zurbruegg HR. Evaluation of the calcium antagonist nimodipine for the prevention of vasospasm after aneurysmal subarachnoid haemorrhage. Acta Neurochirurgica 85: 7–16, 1987
Smith M-J, Kågström E, Rosën I, Siesjö BK. Effect of the calcium antagonist nimodipine on the delayed hypoperfusion following incomplete ischaemia in the rat. Journal of Cerebral Blood Flow and Metabolism 3: 543–546, 1983
Spedding M, Cavero I. Calcium antagonists: a class of drugs with a bright future. Part II. Determination of basic pharmacological properties. Life Sciences 35: 575–587, 1984
Steen PA, Gisvold SE, Milde JH, Newberg LA, Scheithauer BW. Nimodipine improves outcome when given after complete cerebral ischaemia in primates. Anesthesiology 62: 406–414, 1985
Steen PA, Newberg LA, Milde JH, Michenfelder JD. Nimodipine improves cerebral blood flow and neurologic recovery after complete cerebral ischaemia in the dog. Journal of Cerebral Blood Flow and Metabolism 3: 38–43, 1983
Stewart DJ, Gelston A, Hakim A. Effect of prophylactic administration of nimodipine in patients with migraine. Headache 28: 260–262, 1988
Stullken EH, Balestrieri FJ, Prough DS, McWhorter JM. The haemodynamic effects of nimodipine in patients anaesthetized for cerebral aneurysm clipping. Anesthesiology 62: 346–348, 1985
Suwelack D, Weber H. Assessment of enterohepatic circulation of radioactivity following a single dose of [14C] nimodipine in the rat. European Journal of Drug Metabolism and Pharmacokinetics 10: 231–239, 1985
Suwelack D, Weber H, Maruhn D. Pharmacokinetics of nimodipine: II. Communication. Arzneimittel-Forschung 35(II): 1787–1794, 1985
Takayasu IM, Bassett JE, Dacey RG. Effects of calcium antagonists on intracerebral penetrating arterioles in the rat. Journal of Neurosurgery 69: 104–109, 1988
Tanaka K, Gotoh F, Muramatsu F, Fukuuchi Y, Amano T, et al. Effects of nimodipine (BAY e 9736) on cerebral circulation in cats. Arzneimittel-Forschung 30: 1494–1497, 1980
Tanaka K, Gotoh F, Muramatsu F, Fukuuchi Y, Okayasu H, et al. Effect of nimodipine, a calcium antagonist, on cerebral vasospasm after subarachnoid hemorrhage in cats. Arzneimittel-Forschung 32: 1529–1534, 1982
Tettenborn D, Dycka J, Volberg E, Düdden P. Blood pressure and heart rate during treatment with nimodipine in patients with subarachnoid haemorrhage. Neurochirurgia 28: 84–86, 1985
Towart R. The selective inhibition of serotonin-induced contractions of rabbit cerebral vascular smooth muscle by calcium antagonistic dihydropyridines. Circulation Research 48: 650–657, 1981a
Towart R. Predilective relaxation by the calcium antagonist nimodipine (BAY e 9736) of isolated cerebral blood vessels, contracted with autologous blood. British Journal of Pharmacology 74: 268P-269P, 1981b
Towart R, Kazda S. Effects of calcium antagonist nimodipine on isolated cerebral vessels. In Betz et al. (Eds) Nimodipine: pharmacological and clinical properties, pp. 147–161, Schattauer Verlag, Stuttgart, 1985
Towart R, Perzborn E. Nimodipine inhibits carbocyclic throm-boxane-induced contractions of cerebral arteries. European Journal of Pharmacology 69: 213–215, 1981
Towart R, Wehinger E, Meyer H, Kazda S. The effects of nimodipine, its optical isomers and metabolites on isolated vascular smooth muscle. Arzneimittel-Forschung 32: 338–346, 1982
Ulrich G. Zur Wirkung von nimodipin auf die topische Verteilung der absoluten alpha-leistung im EEG sowie die aktuelle befindlichkeit gesunder probanden. Arzneimittel-Forschung 37: 541–544, 1987
Ulrich G, Stieglitz RD. Effect of nimodipine upon electroence-phalographic vigilance in elderly persons with minor impairment of brain functions. Arzneimittel-Forschung 38: 392–396, 1988
Van Reempts J, Haseldonck M, Van Deuren B, Wouters L, Borgers M. Structural damage of the ischaemic brain: involvement of calcium and effects of postischaemic treatment with calcium entry blockers. Drug Development Research 8: 387–395, 1986
van Zwieten PA. Differentiation of calcium entry blockers into calcium channel blockers and calcium overload blockers. European Neurology 25 (Suppl. 1): 57–67, 1986
Vermeulen M, van Gijn H, Hijdra A, Wijdicks EFM. Nimodipine for cerebral arterial spasm in subarachnoid hemorrhage. Correspondence. New England Journal of Medicine 309: 437, 1983
Vibulsresth S, Dietrich WD, Busto R, Ginsberg MD. Failure of nimodipine to prevent ischemic neuronal damage in rats. Stroke 18: 210–216, 1987
Vinge E, Andersson K-E, Brandt L, Ljunggren B, Nilsson L-G, et al. Pharmacokinetics of nimodipine in patients with aneurysmal subarachnoid haemorrhage. European Journal of Clinical Pharmacology 30: 421–425, 1986
Voldby B, Petersen OF, Buhl M, Jakobsen P, Østergaard R. Reversal of cerebral arterial spasm by intrathecal administration of a calcium antagonist (nimodipine). Acta Neurochirurgica 70: 243–254, 1984
White BC, Wiegenstein JG, Winegar CD. Brain ischaemic anoxia: mechanisms of injury. Journal of the American Medical Association 251: 1586–1590, 1984
Young WL, Josovitz K, Morales O, Chien S. The effect of nimodipine on post-ischaemic cerebral glucose utilization and blood flow in the rat. Anesthesiology 67: 54–59, 1987
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: M. Bhatt, Division of Neurology, University of British Columbia Health Sciences Center Hospital, Vancouver, British Columbia, Canada; D.B. Calne, Division of Neurology, University of British Columbia Health Sciences Center Hospital, Vancouver, British Columbia, Canada; L.B. Disney, Division of Neurosurgery, Faculty of Medicine, University of Alberta, Edmonton, Alberta, Canada; H.J. Gelmers, Department of Neurology, Streekziekenhuis Almelo, Almelo, The Netherlands; D.D. Heistad, Department of Internal Medicine, College of Medicine, The University of Iowa, Iowa City, Iowa, USA; J. Philippon, Service de Neurochirurgie, Hôpital de la Salpétrière, Paris, France; J.D. Pickard, Wessex Neurological Centre, Southampton General Hospital, Southampton, England; P. Turner, Department of Clinical Pharmacology, St Bartholomew’s Hospital Medical College, London, England; P.A. van Zwieten, Academic Medical Centre, University of Amsterdam, Amsterdam, The Netherlands.
Rights and permissions
About this article
Cite this article
Langley, M.S., Sorkin, E.M. Nimodipine. Drugs 37, 669–699 (1989). https://doi.org/10.2165/00003495-198937050-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-198937050-00004