Abstract
Objectives
To assess the association between consumption of ultra-processed foods and obesity in the Canadian population.
Methods
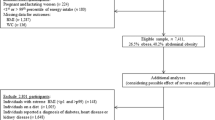
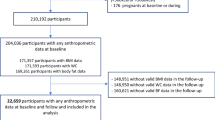
Cross-sectional study including 19,363 adults aged 18 years or more from the 2004 Canadian Community Health Survey, cycle 2.2. Ultra-processed food intake was estimated using daily relative energy intake of ultra-processed food (% of total energy intake) from data obtained by 24-h food recalls. Obesity was assessed using body mass index (BMI ≥ 30 kg/m2). Univariate and multivariate linear regressions were performed to describe ultra-processed food consumption according to socio-economic and demographic variables, and multivariate logistic regression was performed to verify the association between ultra-processed food consumption and obesity, adjusting for potential confounders, including socio-demographic factors, physical activity, smoking, immigrant status, residential location, and measured vs self-reported weight and height.
Results
Ultra-processed foods make up almost half (45%) of the daily calories consumed by Canadian adults. Consumption of these foods is higher among men, younger adults, those with fewer years of formal education, smokers, those physically inactive, and Canadian-born individuals. Ultra-processed food consumption is positively associated with obesity. After adjusting for confounding factors, individuals in the highest quintile of ultra-processed food consumption were 32% more likely of having obesity compared to individuals in the first quintile (predicted OR = e0.005 × 56 = 1.32; 95% CI = 1.05–1.57).
Conclusion
Canadians would benefit from reducing consumption of ultra-processed foods and beverages and increasing consumption of freshly prepared dishes made from unprocessed or minimally processed foods.
Résumé
Objectifs
Cette étude vise à évaluer l’association entre la consommation d’aliments ultra-transformés et l’obésité.
Méthodes
Étude transversale comprenant 19 363 adultes âgés de 18 ans ou plus qui ont participé à l’Enquête sur la santé dans les collectivités canadiennes, 2004, cycle 2.2. La consommation d’aliments ultra-transformés est estimée en utilisant l’apport énergétique relatif provenant des aliments ultra-transformés du rappel alimentaire de 24 heures. L’obésité est déterminée en utilisant l’indice de masse corporelle (IMC) ≥ 30 kg/m2. Les régressions linéaires univariée et multivariée ont été réalisées pour décrire la consommation d’aliments ultra-transformés selon différents groupes socioéconomiques et démographiques, et la régression logistique multivariée a été réalisée pour évaluer l’association entre la consommation de ces aliments et l’obésité, avec ajustement selon diverses variables de contrôle, incluant les facteurs sociodémographiques, l’activité physique, le tabagisme, le statut migratoire, la zone résidentielle et le type de mesure de l’IMC.
Résultats
Les aliments ultra-transformés sont largement consommés au Canada. La consommation de ces aliments est plus élevée chez les hommes, les jeunes adultes, les personnes avec moins d’années d’études, les fumeurs, les personnes physiquement inactives, et celles nées au Canada. La consommation d’aliments ultra-transformés est associée à l’obésité. Les individus du quintile supérieur de consommation d’aliments ultra-transformée ont 32 % plus de risque d’être obèses comparés aux individus du premier quintile (OR = e0.005 × 56 = 1,32; 95% CI = 1,05–1,57).
Conclusion
Les Canadiens pourraient bénéficier d’une réduction de la consommation de produits ultra-transformés et d’une augmentation de mets cuisinés sur place à base d’aliments peu ou pas transformés.

Similar content being viewed by others
References
Fardet, A. (2016). Minimally processed foods are more satiating and less hyperglycemic than ultra-processed foods: A preliminary study with 98 ready-to-eat foods. Food & Function, 7(5), 2338–2346.
Fiolet, T., Srour, B., Sellem, L., et al. (2018). Consumption of ultra-processed foods and cancer risk: Results from NutriNet-Santé prospective cohort. BMJ, 360, k322.
Flagg, L. A., Sen, B., Kilgore, M., et al. (2014). The influence of gender, age, education and household size on meal preparation and food shopping responsibilities. Public Health Nutrition, 17(9), 2061–2070.
Garriguet, D. (2007). Canadians’ eating habits. Health Reports, 18(2), 17–32.
Garriguet, D. (2008). Impact of identifying plausible respondents on the under-reporting of energy intake in the Canadian Community Health Survey. Health Reports, 19(4), 47–55.
Gorber, S. C., Shields, M., Tremblay, M. S., et al. (2008). The feasibility of establishing correction factors to adjust self-reported estimates of obesity. Health Reports, 19(3), 71–82.
Health Canada (2006). Canadian Community Health Survey, Cycle 2.2, Nutrition (2004): A guide to accessing and interpreting the data. Accessed 16 Nov 2016. Available at: http://www.hc-sc.gc.ca/fn-an/surveill/nutrition/commun/cchs_guide_escc-eng.php. Accessed 16 Nov 2016.
Jessri, M., Lou, W. Y., & L’Abbé, M. R. (2016). Evaluation of different methods to handle misreporting in obesity research: Evidence from the Canadian national nutrition survey. The British Journal of Nutrition, 115(1), 147–159.
Juul, F., Martinez-Steele, E., Parekh, N., et al. (2018). Ultra-processed food consumption and excess weight among US adults. The British Journal of Nutrition, 120(1), 90–100.
Lam, M. C. L., & Adams, J. (2017). Association between home food preparation skills and behaviour, and consumption of ultra-processed foods: Cross-sectional analysis of the UK National Diet and nutrition survey (2008–2009). International Journal of Behavioral Nutrition and Physical Activity, 14(1), 68.
Lavigne-Robichaud, M., Moubarac, J.-C., Lantagne-Lopez, S., et al. (2017). Diet quality indices in relation to metabolic syndrome in an indigenous Cree (Eeyouch) population in northern Québec, Canada. Public Health Nutrition, 21(1), 172–180.
Louzada, M. L. C., Baraldi, L. G., Steele, E. M., et al. (2015). Consumption of ultra-processed foods and obesity in Brazilian adolescents and adults. Preventive Medicine, 81, 9–15.
Louzada, M. L. d. C., Ricardo, C. Z., Steele, E. M., et al. (2017). The share of ultra-processed foods determines the overall nutritional quality of diets in Brazil. Public Health Nutrition, 21(1), 94–102.
McEntee, J. (2009). Highlighting food inadequacies: Does the food desert metaphor help this cause? British Food Journal, 111(4), 349–363.
Mendonça, R. D., Lopes, A. C. S., Pimenta, A. M., et al. (2016a). Ultra-processed food consumption and the incidence of hypertension in a Mediterranean cohort: The Seguimiento Universidad de Navarra Project. American Journal of Hypertension, 30(4), 358–366.
Mendonça, R. D., Pimenta, A. M., Gea, A., et al. (2016b). Ultraprocessed food consumption and risk of overweight and obesity: the University of Navarra Follow-Up (SUN) cohort study. The American Journal of Clinical Nutrition, 104(5), 1433–1440.
Monteiro, C. A., Cannon, G., Moubarac, J.-C., et al. (2017a). The UN decade of nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutrition, 21(1), 5–17.
Monteiro, C. A., Moubarac, J.-C., Levy, R. B., et al. (2017b). Household availability of ultra-processed foods and obesity in nineteen European countries. Public Health Nutrition, 21(1), 18–26.
Moubarac JC (2017). Ultra-processed foods in Canada: consumption, impact on diet quality and policy implications. Montréal: TRANSNUT, University of Montreal. Available at: http://www.heartandstroke.ca/-/media/pdf-files/canada/media-centre/hs-report-upp-moubarac-dec-5-2017.ashx.
Moubarac, J.-C., Parra, D. C., Cannon, G., et al. (2014). Food classification systems based on food processing: Significance and implications for policies and actions: A systematic literature review and assessment. Current Obesity Reports, 3(2), 256–272.
Moubarac, J.-C., Batal, M., Louzada, M. L., et al. (2016). Consumption of ultra-processed foods predicts diet quality in Canada. Appetite, 108, 512–520.
Nasreddine, L., Tamim, H., Itani, L., et al. (2018). A minimally processed dietary pattern is associated with lower odds of metabolic syndrome among Lebanese adults. Public Health Nutrition, 21(1), 160–171.
Ogilvie, K.K., Eggleton, A. (2016). Obesity in Canada. A whole-of-society approach for a healthier Canada. Report of the standing senate committee on social affairs, science and technology. Standing senate committee on social affairs, Science and Technology. Available at: www.senate-senat.ca/social.asp.
PAHO. (2015). Ultra-processed food and drink products in Latin America: trends, impact on obesity, policy implications. Washington D.C.: Pan American Health Organization Available at: http://www.paho.org/hq/index.php?option=com_content&view=article&id=11153%3Aultra-processed-food-and-drink-products&catid=4999%3Adocuments&Itemid=0&lang=en. Accessed 15 Aug 2016.
PHAC. (2011). Obesity in Canada - healthy living - Public Health Agency of Canada. Public Health Agency of Canada. Available at: http://www.phac-aspc.gc.ca/hp-ps/hl-mvs/oic-oac/index-eng.php. Accessed 10 Aug 2016.
Rauber, F., Campagnolo, P. D. B., Hoffman, D. J., et al. (2015). Consumption of ultra-processed food products and its effects on children’s lipid profiles: A longitudinal study. Nutrition, Metabolism, and Cardiovascular Diseases, 25(1), 116–122.
Sanou, D., O’Reilly, E., Ngnie-Teta, I., et al. (2014). Acculturation and nutritional health of immigrants in Canada: A scoping review. Journal of Immigrant and Minority Health, 16(1), 24–34.
Statistics Canada (2008). Canadian Community Health Survey (CCHS) Cycle 2.2, 2004. Nutrition - General Health (including vitamins & mineral supplements) & 24-hour dietary recall, Master and Shared files - Derived variables documentation. Available at: http://www23.statcan.gc.ca/imdb-bmdi/pub/document/5049_D24_T9_V1-eng.pdf.
Steele, E. M., & Monteiro, C. A. (2017). Association between dietary share of ultra-processed foods and urinary concentrations of phytoestrogens in the US. Nutrients, 9(3). https://doi.org/10.3390/nu9030209.
Steele, E. M., Popkin, B. M., Swinburn, B., et al. (2017). The share of ultra-processed foods and the overall nutritional quality of diets in the US: Evidence from a nationally representative cross-sectional study. Population Health Metrics, 15(1), 6.
Tavares, L. F., Fonseca, S. C., Garcia Rosa, M. L., et al. (2012). Relationship between ultra-processed foods and metabolic syndrome in adolescents from a Brazilian Family Doctor Program. Public Health Nutrition, 15(1), 82–87.
Vandevijvere, S., Monteiro, C. A., Krebs-Smith, S. M., et al. (2013). Monitoring and benchmarking population diet quality globally: A step-wise approach. Obesity Reviews, 14(Suppl 1), 135–149.
Wolfson, J. A., & Bleich, S. N. (2015). Is cooking at home associated with better diet quality or weight-loss intention? Public Health Nutrition, 18(8), 1397–1406.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study complies with current research ethics standards and was approved by the Health Research Ethics Board of the University of Montreal (17-017-CERES-D). Data access was granted by Statistics Canada, under contract (no. 13-SSH-MTL-3475) and data were analyzed at the Québec interUniversity Centre for Social Statistics in Montreal.
Electronic supplementary material
ESM 1
(DOCX 30 kb)
Rights and permissions
About this article
Cite this article
Nardocci, M., Leclerc, BS., Louzada, ML. et al. Consumption of ultra-processed foods and obesity in Canada. Can J Public Health 110, 4–14 (2019). https://doi.org/10.17269/s41997-018-0130-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.17269/s41997-018-0130-x