Abstract
Background
Basosquamous carcinoma (BSC) is a relatively rare type of neoplasm originating from basal cell carcinoma with features of squamous differentiation. BSC has an aggressive local behaviour with a tendency for recurrence and a less frequent metastatic potential
Objectives
The primary objective was to describe the dermatoscopic features of the tumour. Secondary goals were to detect the morphological features of the tumour along with patients’ characteristics and to evaluate possible dermatoscopic and histopathological correlations
Materials & Methods
Twenty-two patients with 25 BSCs were enrolled. All tumours were surgically excised and diagnosis was based on histopathology. Clinical and dermatoscopic images were evaluated by two investigators based on pre-defined criteria, and a statistical analysis was performed
Results
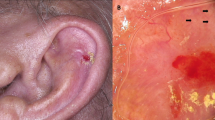
The median age of the patients was 78 years old (range: 52–88) and the male/female ratio was 2.14. All patients reported history of either occupational (50%) or recreational (50%) intensive sun exposure and 72.73% had signs of actinic keratosis. The most common anatomical site of the tumours was the head/neck area (72%). Clinically, nodular (64%), ulcerated (88%) and non-pigmented (76%) lesions prevailed. Dermatoscopically, 92% had prominent vasculature and monomorphous arborizing vessels with a diffuse arrangement, representing the most frequently observed type. Ulceration (88%), SCC dermatoscopic criteria (56%), white strands/blotches (56%) and features of pigmentation (40%) were also detected
Conclusion
We suggest that the most common prototype of BSC is an ulcerated, facial nodule in elderly males with photo-damaged skin, dermatoscopically displaying combined features of mostly nodular BCC and, to a less extent, SCC
Similar content being viewed by others
References
Elder DJ, Massi S, Scolyer RA, Willemze R. WHO classification of skin tumors. Lyon: IARC, 2018.
Leibovitch I, Huilgol SC, Selva D, et al. Basosquamous carcinoma: treatment with Mohs micrographic surgery. Cancer 2005; 104: 170–5.
Maloney ML. What is basosquamous carcinoma? Dermatol Surg 2000; 26: 505–6.
Peris K, Fargnoli MC, Garbe C, et al. Diagnosis and treatment of basal cell carcinoma: European consensus-based interdisciplinary guidelines. Eur J Cancer 2019; 118: 10–34.
Cameron MC, Lee E, Hibler BP, et al. Basal cell carcinoma. Contemporary approaches to diagnosis, treatment, and prevention. J Am Acad Dermatol 2019; 80: 321–40.
Tan KZ, Rieger KE, Sarin KY. Basosquamous carcinoma: controversy, advances and future directions. Dermatol Surg 2017; 43: 23–31.
Volkenstein S, Wohlschlaeger J, Liebau J, et al. Basosquamous carcinoma-a rare but aggressive skin malignancy. J Plast Reconstr Aesth Surg 2010; 63: 304–6.
Kittler H, Rosendahl C, Cameron A, Tschandl P. Dermatoscopy: an algorithmic method based on pattern analysis. Vienna: Facultas.wuv Universitäts, 2016.
Lallas A, Apalla Z, Argenziano G, et al. The dermatoscopic universe of basal cell carcinoma. Dermatol Pract Concept 2013; 4: 11–24.
Giacomel J, Zalaudek I. Pink lesions. Dermatol Clin 2013; 31: 649–78.
Lallas A, Apalla Z, Ioannides D, et al. Dermoscopy in the diagnosis and management of basal cell carcinoma. Future Oncol 2015;11:2975–84.
Suppa M, Micantonio T, Di Stefano A, et al. Dermoscopic variability of basal cell carcinoma according to clinical type and anatomic location. J Eur Acad Dermatol Venereol 2015; 29: 1732–41.
Yélamos O, Braun RP, Liopyris K, et al. Dermoscopy and dermatopathology correlates of cutaneous neoplasms. J Am Acad Dermatol 2019; 80: 341–64.
Reiter O, Mimouni I, Gdalevich M, et al. The diagnostic accuracy of dermoscopy for basal cell carcinoma: a systematic review and metaanalysis. J Am Acad Dermatol 2019; 80: 1380–8.
Giacomel J, Lallas A, Argenziano G, et al. Dermoscopy of basosquamous carcinoma. Br J Dermatol 2013; 169: 358–64.
Akay BN, Saral S, Heper AO, Erdem C, Rosendahl C. Basosquamous carcinoma: dermoscopic clues to diagnosis. J Dermatol 2017; 44: 127–34.
Cunceen TS, Yong JL, Benger R. Lung metastases in a case of metatypical basal cell carcinoma of the eyelid: an illustrative case and literature review to heighten vigilance of its metastatic potential. Clin Exp Opthalmol 2008; 36: 475–7.
Wermker K, Roknic N, Goessling K, Klein M, Schulze HJ, Hallermann C. Basosquamous carcinoma of the head and neck: clinical and histologic characteristics and their impact on disease progression. Neoplasia 2015;17:301–5.
Oldbury J, Wain R, Abas S, Dobson C, Iyer S. Basosquamous carcinoma: a single centre clinicopathological evaluation and proposal of an evidence-based protocol. J Skin Cancer 2018; 2018: 6061395.
Tarallo M, Cigna E, Frati R, et al. Metatypical basal cell carcinoma: a clinical review. J Exp Clin Cancer Res 2008; 27: 65.
Garcia C, Poletti E, Neil Crowson A. Basosquamous carcinoma. J Am Acad Dermatol 2009; 60: 137–43.
Cigna E, Tarallo M, Servillo S, Piperno A, Scuderi N. Metatypical carcinoma of the head: a review of 312 cases. Eur Rev Med Pharmacol Sci 2012;16:1915–8.
Moon HR, Park TJ, Ro KW, et al. Pigmentation of basal cell carcinoma is inversely associated with tumor aggressiveness in Asian patients. J Am Acad Dermatol 2019; 80: 1755–7.
Conforti C, Pizzichetta MA, Vichi S, et al. Sclerodermiform basal cell carcinomas vs. other histotypes: analysis of specific demographic, clinical and dermatoscopic features. J Eur Acad Dermatol Venereol 2021; 35: 79–87.
Pampena R, Parisi G, Benati M, et al. Clinical and dermoscopic factors for the identification of aggressive histologic subtypes of basal cell carcinoma. Front Oncol 2021; 10: 630458.
Navarette-Dechent C, Bajaj S, Marchetti M, Rabinovitz H, Dusza S, Marghoob A. Association of shiny white blotches and strands with nonpigmented basal cell carcinoma. JAMA Dermatol 2016; 152: 546–52.
Navarette-Dechent C, Liopyris K, Rishpon A, et al. Association of multiple aggregated yellow-white globules with nonpigmented Basal Cell Carcinoma. JAMA Dermatol 2020; 156: 882–90.
Balagula Y, Braun RP, Rabinovitz HS, et al. The significance of crystalline/chrysalis structures in the diagnosis of melanocytic and nonmelanocytic lesions. J Am Acad Dermatol 2012; 67: 194e1–8.
Rosendahl C, Cameron A, Argenziano G, Zalaudek I, Tschandl P, Kittler H. Dermoscopy of squamous cell carcinoma and keratoacanthoma. Arch Dermatol 2012; 148: 1386–92.
Acknowledgements and disclosures
Acknowledgements: the patients in this manuscript have given written informed consent to publication of their case details.
Funding sources: none.
Conflicts of interest: none.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Sgouros, D., Apalla, Z., Theofili, M. et al. How to spot a basosquamous carcinoma: a study on demographics, clinical-dermatoscopic features and histopathological correlations. Eur J Dermatol 31, 779–784 (2021). https://doi.org/10.1684/ejd.2021.4178
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2021.4178