Abstract
Background
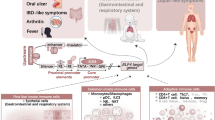
Erythropoietic protoporphyria (EPP) is a rare inherited disease associated with heme metabolism, characterized by severe life-long photosensitivity and liver involvement.
Objective
To provide epidemiological data of EPP in Italy.
Materials & Methods
Prospective/retrospective data of EPP patients were collected by an Italian network of porphyria specialist centres (Gruppo Italiano Porfiria, GrIP) over a 20-year period (1996–2017).
Results
In total, 179 patients (79 females) with a clinical and biochemical diagnosis of EPP were assessed, revealing a prevalence of 3.15 cases per million persons and an incidence of 0.13 cases per million persons/year. Incidence significantly increased after 2009 (due to the availability of alfa-melanotide, which effectively limits skin photosensitivity). Mean age at diagnosis was 28 years, with only 22 patients (12.2%) diagnosed ≤10 years old. Gene mutations were assessed in 173 (96.6%) patients; most (164; 91.3%) were FECH mutations on one allele in association with the hypomorphic variant, c.315–48C, on the other (classic EPP), and nine (5.2%) were ALAS2 mutations (X-linked EPP). Only one case of autosomal recessive EPP was observed. Of the 42 different FECH mutations, 15 are novel, three mutations collectively accounted for 45.9% (75/164) of the mutations (c.215dupT [27.2%], c.901_902delTG [11.5%] and c.67 + 5G > A [7.2%]), and frameshift mutations were prevalent (33.3%). A form of light protection was used by 109/179 (60.8%) patients, and 100 (56%) had at least one α-melanotide implant. Three cases of severe acute liver involvement, requiring OLT, were observed.
Conclusion
These data define, for the first time, the clinical and molecular epidemiology of EPP in Italy.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Cox TM. Protoporphyria. Kadish KM, Guilard R. San Diego: Academic Press, 2003.
Thunell S, Harper P, Brun A. Porphyrins, porphyrin metabolism and porphyrias. IV. Pathophysiology of erythyropoietic protoporphyriadiagnosis, care and monitoring of the patient. Scand J Clin Lab Invest 2000; 60: 581–604.
Holme SA, Anstey AV, Finlay AY, Elder GH, Badminton MN. Erythropoietic protoporphyria in the UK: clinical features and effect on quality of life. Br J Dermatol 2006; 155: 574–81.
Sood G, Anderson KE. Porphyrias. Crowther M, Ginsberg J, Schunemann H, et al. Hoboken: Wiley, 2008.
Wahlin S, Floderus Y, Stal P, Harper P. Erythropoietic protoporphyria in Sweden: demographic, clinical, biochemical and genetic characteristics. J Intern Med 2011; 269: 278–88.
Whatley SD, Mason NG, Holme SA, Anstey AV, Elder GH, Badminton MN. Molecular epidemiology of erythropoietic protoporphyria in the U.K. Br J Dermatol 2010; 162: 642–6.
Elder G, Harper P, Badminton M, Sandberg S, Deybach JC. The incidence of inherited porphyrias in Europe. J Inherit Metab Dis 2013; 36: 849–57.
Sarkany RP, Ross G, Willis F. Acquired erythropoietic protoporphyria as a result of myelodysplasia causing loss of chromosome 18. Br J Dermatol 2006; 155: 464–6.
Wiman A, Floderus Y, Harper P. Novel mutations and phenotypic effect of the splice site modulatori IVS3–48C in nine Swedish Families with erythropoietic protoporhyria. J Hum Genet 2003; 48: 70–6.
Gouya L, Puy H, Robreau AM, et al. The penetrance of dominant erythropoietic protoporphyria is modulated by expression of wildtype FECH. Nat Genet 2002; 30: 27–8.
Gouya L, Martin-Schmitt C, Robreau AM, et al. Contribution of a common single-nucleotide polymorphism to the genetic predisposition for erythropoietic protoporphyria. Am J Hum Genet 2006; 78: 2–14.
Sarkany RP, Cox TM. Autosomal recessive erythropoietic protoporphyria: a syndrome of severe photosensitivity and liver failure. QJM 1995; 88: 541–9.
Whatley SD, Ducamp S, Gouya L, et al. C-terminal deletions in the ALAS2 gene lead to gain of function and cause X-linked dominant protoporphyria without anemia or iron overload. Am J Hum Genet 2008; 83: 408–14.
Yien YY, Ducamp S, van der Vorm LN, et al. Mutation in human CLPX elevates levels of delta-aminolevulinate synthase and protoporphyrin IX to promote erythropoietic protoporphyria. Proc Natl Acad Sci USA 2017; 114: E8045–52.
Whitman JC, Paw BH, Chung J. The role of ClpX in erythropoietic protoporphyria. Hematol Transfus Cell Ther 2018; 40: 182–8.
Aurizi C, Schneider-Yin X, Sorge F, Macri A, Minder EI, Biolcati G. Heterogeneity of mutations in the ferrochelatase gene in Italian patients with erythropoietic protoporphyria. Mol Genet Metab 2007; 90: 402–7.
Deacon AC, Elder GH. ACP Best Practice No 165: front line tests for the investigation of suspected porphyria. J Clin Pathol 2001; 54: 500–7.
Sassaroli M, da Costa R, Vaananen H, Eisinger J, Poh-Fitzpatrick MB. Distribution of erythrocyte free porphyrin content in erythropoietic protoporphyria. J Lab Clin Med 1992; 120: 614–23.
Sassa S, Granick JL, Granick S, Kappas A, Levere RD. Studies in lead poisoning. I. Microanalysis of erythrocyte protoporphyrin levels by spectrophotometry in the detection of chronic lead intoxication in the subclinical range. Biochem Med 1973; 8: 135–48.
Brancaleoni V, Balwani M, Granata F, et al. X-chromosomal inactivation directly influences the phenotypic manifestation of X-linked protoporphyria. Clin Genet 2016; 89: 20–6.
Di Pierro E, Brancaleoni V, Besana V, Ausenda S, Drury S, Cappellini MD. A 10376 bp deletion of FECH gene responsible for erythropoietic protoporphyria. Blood Cells Mol Dis 2008; 40: 233–6.
Brancaleoni V, Granata F, Colancecco A, Tavazzi D, Cappellini MD, Di Pierro E. Seven novel genetic mutations within the 5′UTR and the housekeeping promoter of HMBS gene responsible for the non-erythroid form of acute intermittent porphyria. Blood Cells Mol Dis 2012; 49: 147–51.
Di Pierro E, Brancaleoni V, Besana V, Cappellini MD. Multiplex ligation-dependent probe amplification: a novel approach for genetic diagnosis of Porphyria. J Hum Genet 2009; 54: 479–87.
Chiara M, Primon I, Tarantini L, et al. Targeted resequencing of FECH locus reveals that a novel deep intronic pathogenic variant and eQTLs may cause erythropoietic protoporphyria (EPP) through a methylation-dependent mechanism. Genet Med 2020; 22: 35–43.
Lala SM, Naik H, Balwani M. Diagnostic delay in erythropoietic protoporphyria. J Pediatr 2018; 202: 320–3.e2.
Minder EI. Afamelanotide, an agonistic analog of alphamelanocyte-stimulating hormone, in dermal phototoxicity of erythropoietic protoporphyria. Expert Opin Investig Drugs 2010; 19: 1591–602.
Luger TA, Bohm M. An alpha-MSH analog in erythropoietic protoporphyria. J Invest Dermatol 2015; 135: 929–31.
Langendonk JG, Balwani M, Anderson KE, et al. Afamelanotide for erythropoietic protoporphyria. N Engl J Med 2015; 373: 48–59.
Parker M, Corrigall AV, Hift RJ, Meissner PN. Molecular characterization of erythropoietic protoporphyria in South Africa. Br J Dermatol 2008; 159: 182–91.
Risheg H, Chen FP, Bloomer JR. Genotypic determinants of phenotype in North American patients with erythropoietic protoporphyria. Mol Genet Metab 2003; 80: 196–206.
Balwani M. Erythropoietic protoporphyria and X-linked protoporphyria: pathophysiology, genetics, clinical manifestations, and management. Mol Genet Metab 2019; 128: 298–303.
Balwani M, Doheny D, Bishop DF, et al. Loss-of-function ferrochelatase and gain-of-function erythroid-specific 5-aminolevulinate synthase mutations causing erythropoietic protoporphyria and x-linked protoporphyria in North American patients reveal novel mutations and a high prevalence of X-linked protoporphyria. Mol Med 2013; 19: 26–35.
Balwani M, Naik H, Anderson KE, et al. Clinical, biochemical, and genetic characterization of North American patients with erythropoietic protoporphyria and X-linked protoporphyria. JAMA Dermatol 2017; 153: 789–96.
Berroeta L, Man I, Goudie DR, Whatley SD, Elder GH, Ibbotson SH. Late presentation of erythropoietic protoporphyria: case report and genetic analysis of family members. Br J Dermatol 2007; 157: 1030–1.
Schmitt C, Ducamp S, Gouya L, Deybach JC, Puy H. Inheritance in erythropoietic protoporphyria. Pathol Biol (Paris) 2010; 58: 372–80.
Langendonk JG. Treatment for erythropoietic protoporphyria. Br J Dermatol 2015; 172: 1481–2.
Singal AK, Parker C, Bowden C, Thapar M, Liu L, McGuire BM. Liver transplantation in the management of porphyria. Hepatology 2014; 60: 1082–9.
Gross U, Frank M, Doss MO. Hepatic complications of erythropoietic protoporphyria. Photodermatol Photoimmunol Photomed 1998; 14: 52–7.
Anstey AV, Hift RJ. Liver disease in erythropoietic protoporphyria: insights and implications for management. Postgrad Med J 2007; 83: 739–48.
McGuire BM, Bonkovsky HL, Carithers RL Jr., et al. Liver transplantation for erythropoietic protoporphyria liver disease. LiverTranspl 2005; 11: 1590–6.
Rand EB, Bunin N, Cochran W, Ruchelli E, Olthoff KM, Bloomer JR. Sequential liver and bone marrow transplantation for treatment of erythropoietic protoporphyria. Pediatrics 2006; 118: e1896–9.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Acknowledgments and disclosures
Acknowledgments: the authors are grateful to all patients, who donated samples for this study. We are grateful to Dr. Gigi Mori, PhD (ASST Spedali Civili di Brescia) and Prof. Leonardo Salviati, MD (Università degli studi di Padova) for genetic testing. Financial support: none. Conflicts of interest: Paolo Ventura and Maria Domenica Cappellini receivedfundsfor consultation and lecturing by Alnylam Pharmaceuticals and Recordati Rare Disease.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Ventura, P., Brancaleoni, V., Di Pierro, E. et al. Clinical and molecular epidemiology of erythropoietic protoporphyria in Italy. Eur J Dermatol 30, 532–540 (2020). https://doi.org/10.1684/ejd.2020.3880
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2020.3880