Abstract
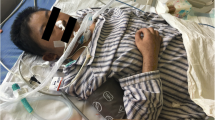
We report a case of a 64-year-old woman treated with meglumine antimoniate (Glucantime®). On day 20, she developed fever, a pruriginous skin rash and myalgia. The blood tests showed eosinophilia and hepatic cytolysis. The clinico-biological picture improved gradually and the symptoms disappeared 4 weeks after the drug withdrawal. Six weeks later, intradermal tests to Glucantime® were performed and were positive at 48 hour-reading. This clinical picture suggests DRESS induced by meglumine antimoniate. To the best of our knowledge, only one case of meglumine antimoniate-induced DRESS has been reported in the literature and we are the first to report a case confirmed by skin tests.
Similar content being viewed by others
References
Barbaud A. 2014. Skin testing and patch testing in non-IgE-mediated drug allergy. Current Allergy and Asthma Reports,14, 442. DOI: 10.1007/s11882-014-0442-8
Ben Salah A., Ben Messaoud N., Guedri E., Zaatour A., Ben Alaya N., Bettaieb J. et al. 2013. Topical paromomycin with or without gentamicin for cutaneous leishmaniasis. The New England Journal of Medicine, 1, 368–524. DOI: 10.1056/NEJMoa1202657
Brasileiro A., Martín-Ezquerra G., García-Martinez P., Pujol R.M., Giménez-Arnau A.M. 2017. Allergic reactions to meglumine antimoniate while treating cutaneous leish-maniasis. Journal of the European Academy of Dermatology and Venereology, 1, 31–59. DOI: 10.1111/ jdv.13726
Cordoba S., Gandolfo Cano M., Aguado M., Huerta-Brogera M., Romero A., Martinez-Moran C. et al. 2012. Delayed allergic skin reactions due to intralesional meglumine anti-moniate therapy for cutaneous leishmaniasis. Allergy, 1, 67–1609. DOI: 10.1111/all.12050
Esfandiarpour I., Farajzadeh S., Rahnama Z., Fathabadi E.A., Heshmatkhah A. 2012. Adverse effects of intralesional meglumine antimoniate and its influence on clinical laboratory parameters in the treatment of cutaneous leishmaniasis. International Journal of Dermatology, 51, 1221. DOI: 10.1111/j.1365-4632.2012.05460.x
Jeddi F., Caumes E., Thellier M., Jauréguiberry S., Mazier D., Buffet P.A. 2009. Case report: Drug hypersensitivity syndrome induced by meglumine antimoniate. The American Journal Of Tropical Medicine And Hygiene, 1, 80–939
Kardaun S.H., Sidoroff A., Allanore V., Halevy S., Davidovici B.B., Mockenhaupt M., et al. 2007. Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist? The British Journal of Dermatology, 1, 156–609. DOI: 10.1111/j.1365-2133.2006.07704.x
Masmoudi A., Hariz W., Marrekchi S., Amouri M., Turki H. 2013. Old world cutaneous leishmaniasis: diagnosis and treatment. Journal of Dermatological Case Reports, 1, 7–31. DOI: 10.3315/jdcr.2013.1135
Naranjo C.A., Busto U., Sellers E.M., Sandor P., Ruiz I., Roberts E.A., et al. 1981. A method for estimating the probability of adverse drug reactions. Clinical Pharmacology and Therapeutics, 1, 30–239
Wongkitisophon P., Chanprapaph K., Rattanakaemakorn P., Vachiramon V. 2012. Six-year retrospective review of drug reaction with eosinophilia and systemic symptoms. Acta Dermato-Venereologica, 1, 92–200. DOI: 10.2340/00015555-1222
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chaabane, A., Romdhane, H.B., Brahim, H.B. et al. Meglumine antimoniate-induced DRESS: original case with a positive skin test. Acta Parasit. 63, 845–847 (2018). https://doi.org/10.1515/ap-2018-0104
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1515/ap-2018-0104