Abstract
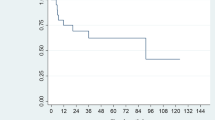
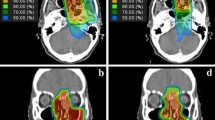
Thirty-two patients with nasal NK/T-cell lymphoma and disseminated disease (lung, skin, and bone marrow) were treated with an intensive combined therapy that consisted of three cycles of CMED (cyclophosphamide 2 g/m2, metothrexate 200 mg/m2, etoposide 600 mg/m2, and dexamethasone 80 mg/m2 with leucovorin rescue administered 24 h after) every 14 d, following high-dose radiotherapy: 55 Gy in 20 sesions to centrofacial region and three cycles more of the same chemotherapy regimen. To ameliorate the presence of severe granulocytopenia, granulocyte colony-stimulating factor, 5 µg/kg, daily for 14 d, begun on d 2 after chemotherapy, was administered. Complete response was achieved in 21 cases (65%); failure or progression was observed in 11 cases (35%). With a median follow-up of 69.1 mo, relapse has not been observed; thus, actuarial curves at 5 yr showed that event-free survival (EFS) is 100% in 21 patients and overall survival (OS) is 65%. Granulocytopenia grade IV was observed in 15% cycles, Nonhematological toxicity was mild and well tolerated. Radiotherapy was well tolerated; only mild mucositis was observed. Nasal NK/T-cell lymphoma is an rare presentation of maligant lymphoma (<1% of all cases) with a worse prognosis; less than 5% patients are alive free of disease at 1 yr. The use of intensive more specific chemotherapy and high dose of local radiotherapy, appear to be an excellent therapeutic approach with improvement in EFS and OS.
Similar content being viewed by others
References
Avilés, A., et al. (1991). Angiocentric T-cell lymphoma of the nose, paranasal sinuses and hard palate. Hematol. Oncol. 10:141–147.
Kwong, Y.L., et al. (1997). CD56 + NK lymphomas. Clinicopathological features and prognosis. Br. J. Haematol. 97:821–829.
Cheong, M.M.C., et al. (1998). Primary non-Hodgkin’s lymphoma of the nose and nasopharynx. Clinical features, tumor immunophenotype and treatment outcome in 253 patients. J. Clin. Oncol. 16:70–77.
Avilés A., et al. (1994). Combined therapy for angioimmunoproliferative lesions. Eur. J. Cancer Oral Oncol. 32B:302–304.
Shikamura, N., et al. (2001). Localized aggressive non-Hodgkin’s of the nasal cavity: a survey by the Japan Lymphoma Radiation Therapy Group. Int. J. Radiat. Oncol. Biol. Phys. 51:1228–1233.
Liang, R. (2000). Diagnosis and management of primary nasal lymphoma of T-cell or NK cell origin. Clin. Lymphoma 1:33–37.
Marz-Gerhard, R. et al. (2001). Natural killer/natural killer like T cell lymphoma CD 56+, presenting in the skin. J. Clin. Oncol. 19:2179–2181.
Chang, J.K.C., et al. (1988). Angiocentric T-cell lymphoma of the skin. Am. J. Clin. Pathol. 12:861–876.
Chang, J.K.C., et al. (1997). Lymphoma of nasal cavity and paranasal sinuses. Improved outcome and altered prognostic factors with combined therapy. Cancer 80:477–485.
Avilés, A., et al. (2000). Angiocentric nasal T/natural killer cell lymphoma. A single centre study of prognostic factors in 108 patients. Clin. Lab. Haematol. 22:215–220.
Sobrevilla, C.P., et al. (1993). Radiotherapy compared to chemotherapy as initial treatment of angiocentric centrofacial lymphoma (polymorphic reticulosis). Acta Oncol. 32:69–72.
Loni, L., et al. (2001). Pharmacogenetics of anticance drugs in non-Hodgkin’s lymphoma. Br. J. Cancer. 85:1425–1431.
Avilés, A., et al. (1990). Linfomas no-hodgkinianos. Resultados de la quimioterapia alterna frente a la quimioterapia secuencial. Sangre (Barc.) 35:245–249.
Ribrag, V., et al. (2001). Early locoregional high dose radiotherapy is associated with long-term disease control in localized primary angiocentric lymphoma of the nose and nasopharynx. Leukemia 15:1123–1126.
Kim, C.E., et al. (2000). Angiocentric lymphoma of the head and neck. Patterns of systemic failure after radiation therapy. J. Clin. Oncol. 18:54–63.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Avilés, A., Neri, N., Fernández, R. et al. Nasal NK/T-cell lymphoma with disseminated disease treated with aggressive combined therapy. Med Oncol 20, 13–17 (2003). https://doi.org/10.1385/MO:20:1:13
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1385/MO:20:1:13