Abstract
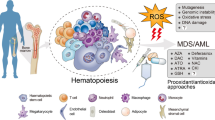
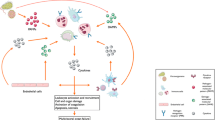
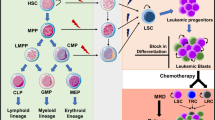
Proinflammation represents a pathophysiological state on the early stage of a number of diseases, especially the infectious and immunological ones. In recent years, proinflammation has attracted much attention, and the term “proinflammation factors” appears frequently in the literature. While investigating leukemia and leukemic cells from the angle of “proinflammation state”, we got some intriguing findings, e.g. we detected the significantly elevated expression of proinflammation factor IL-18 in patients with acute myeloid leukemia (AML), which could up-regulate matrix metalloproteinases (MMP) and specific tissue inhibitors (TIMPs). The increased MMP may play a role in the aggressiveness of myeloid leukemic cells, and be associated with a poor prognosis. This phenomenon reflects an ignored aspect of leukemia. Investigations from the angle of “proinflammation state” have broaden the fields of tumor and leukemia study.
Similar content being viewed by others
References
Wu, K. F., Zhu, Y. M., Rao, Q. et al., Expression of transforming growth factor-β, tumor necrosis factor-α and leukemia inhibitory factor mRNAs in rodent and human hematopoietic cells, Ann. N. Y. Acad. Sci., 1991, 628: 151–153.
Wu, K. F., Rao, Q., Zheng, G. G. et al., Enhancement of J6-1 human leukemic cell proliferation by cell-cell contact: Role of an M-CSF-like membrane-associated growth factor, Leuk. Res., 1994, 18: 843–849.
Wu, K. F., Zheng, G. G., Rao, Q. et al., Cellular macrophage colony-stimulating factor and its role, Hematologica, 1999, 84: 951–953.
Radisky, D., Hagios, C., Bissell, M. J., Tumors are unique organs defined by abnormal signaling and context, Semin. Cancer Biol., 2001, 11: 87–95.
Schuch, G., Machluf, M., Bartsch, G. Jr. et al., In vivo administration of vascular endothelial growth factor (VEGF) and its antagonist, soluble neuropilin predicts a role of VEGF in the progression of acute myloid leukemia in vivo, Blood, 2002, 100: 4622–4628.
Molica, S., Vacca, A., Ribatti, D. et al., Prognostic value of enhanced bone marrow angiogenesis early B-cell chronic lymphocytic leukemia, Blood, 2002, 100: 3344–3351.
Esch, T., Stefano, G. B., Proinflammation: A common denominator or initiator of different pathophysiological disease processes, Med. Sci. Monit, 2002, 8: 1–9. (http://www.MedSciMonit.com/pub/ vol_8/no_5/2686.pdf)
Ko, Y. G., Park, H., Kim, T. et al., A cofactor of tRNA synthetase, p43, is secreted to up-regulate proinflammatory genes, J. Biol. Chem., 2001, 276: 23028–23033.
Balkwill, F., Mantovani, A., Inflammation and cancer: back to Virchow? Lancet, 2001, 357: 539–545.
Coussens, L. M., Werb, Z., Inflammation and cancer, Nature, 2002, 420: 860–867.
Toi, M., Proinflammation in human tumor microenvironment: its status and implication, Med. Sci. Monit., 2002, 8: LE25–26.
Shen, W. H., Zhou, J. H., Suzanne, R. et al., Proinflammatory cytokines block growth of breast cancer cells by impairing signals from a growth factor receptor, Cancer Res., 2002, 62: 4746–4756.
Skinnider, B. F., Mak, T. W., The role of cytokines in classical Hodgkin lymphoma, Blood, 2002, 99: 4283–4297.
Wu, K. F., Luka, J., Joshiet, L. et al., Characterization of a Human Herpes Virus-6 (HHV-6) and Epstein-Barr Virus (EBV) associated leukemic cell line, J6-1, Chinese J. Cancer Res., 1994, 6: 157–167.
Wu, K. F., On bio-diversity, complexity of M-CSF and its receptor, Chinese Science Bulletin, 2000, 45: 1918–1920.
Cao, Z. Y., Wu, K. F., Li, G. et al., Enhancement of NIH3T3 cell’s proliferation by expressing M-CSF, Chinese J. Cancer Res., 2003, 15: 43–48.
Cao, Z. Y., Zhang, B., Rao, Q. et al., Effects of nuclear presenting M-CSF on the process of malignancy, Int. J. Hematol., 2003, 78: 87–89.
Wang, Y., Li, G., Zheng, G. G. et al., Detection and sequencing analysis of IL-18 expression in J6-1 leukemic cells, Leuk. Res., 2001, 25: 273–274.
Zhang, B., Ma, X. T., Zheng, G. G. et al., Expression of IL-18 and its receptor in human leukemia cells, Leuk. Res., 2003, 27: 813–822.
Zhang, B., Cao, Z. Y., Wu, K. F. et al., Expression and functional reconstitution of IL-18 receptor in K562 leukemia cells, Leuk. Res., 2003, 27: 971–972.
Zhang, B., Wang, Y., Zheng, G. G. et al., Clinical significance of IL-18 gene overexpression in acute myeloid leukemia, Leuk. Res., 2002, 26: 887–892.
Zhang, B., Rao, Q., Zheng, G. G. et al., Expression and significance of IL-18 in the bone marrow of patients with hematological diseases, Chin. Med. J., 2003, 116: 218–221.
Zhang, B., Wu, K. F., Cao, Z. Y. et al., IL-18 regulation of matrix metalloproteinases (MMPs) expression in HL-60 myeloid leukemia cells and its role in invasion, Leuk. Res., 2004, in press.
Yang, Y. H., Zheng, G. G., Li, G. et al., Expression of LL-37/hCAP18 gene in human leukemia cells, Leuk. Res., 2003, 27: 947–950.
Drexler, H. G., Matsuo, Y., MacLeod, R. A. F., Continuous hematopoietic cell lines as model systems for leukiemia-lymphoma research, Leuk. Res., 2000, 24: 881–911.
Medvinsky, A., Smith, A., Stem cells: Fusion brings down barriers, Nature, 2003, 422: 823–825.
Yanjie, Y. L., Isaacs, S. N., Willams, D. A. et al., Role of CXCR4 in cell-cell fusion and infection of monocyte derived macrophages by primary human immunodeficiency virus type 1 (HIV-1) strains: Two distinct mechanisms of HIV-1 dual tropism, J. Virol., 1999, 73: 7117–7125.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Wu, K., Ma, X. Viewpoints on the proinflammation state of leukemia. Chin.Sci.Bull. 48, 2519–2522 (2003). https://doi.org/10.1360/03wc0339
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1360/03wc0339