Abstract
Background
The high incidence of early recurrence after hepatectomy for intrahepatic cholangiocarcinoma (ICC) has a detrimental effect on overall survival (OS). Machine-learning models may improve the accuracy of outcome prediction for malignancies.
Methods
Patients who underwent curative-intent hepatectomy for ICC were identified using an international database. Three machine-learning models were trained to predict early recurrence (< 12 months after hepatectomy) using 14 clinicopathologic characteristics. The area under the receiver operating curve (AUC) was used to assess their discrimination ability.
Results
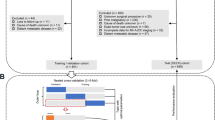
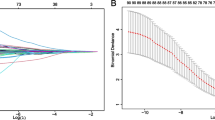
In this study, 536 patients were randomly assigned to training (n = 376, 70.1%) and testing (n = 160, 29.9%) cohorts. Overall, 270 (50.4%) patients experienced early recurrence (training: n = 150 [50.3%] vs testing: n = 81 [50.6%]), with a median tumor burden score (TBS) of 5.6 (training: 5.8 [interquartile range {IQR}, 4.1–8.1] vs testing: 5.5 [IQR, 3.7–7.9]) and metastatic/undetermined nodes (N1/NX) in the majority of the patients (training: n = 282 [75.0%] vs testing n = 118 [73.8%]). Among the three different machine-learning algorithms, random forest (RF) demonstrated the highest discrimination in the training/testing cohorts (RF [AUC, 0.904/0.779] vs support vector machine [AUC, 0.671/0.746] vs logistic regression [AUC, 0.668/0.745]). The five most influential variables in the final model were TBS, perineural invasion, microvascular invasion, CA 19-9 lower than 200 U/mL, and N1/NX disease. The RF model successfully stratified OS relative to the risk of early recurrence.
Conclusions
Machine-learning prediction of early recurrence after ICC resection may inform tailored counseling, treatment, and recommendations. An easy-to-use calculator based on the RF model was developed and made available online.




Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Tsilimigras DI, Sahara K, Wu L, et al. Very early recurrence after liver resection for intrahepatic cholangiocarcinoma: considering alternative treatment approaches. JAMA Surg. 2020;155:823–31.
Spolverato G, Glavas D, Hewitt DB, et al. Advances in pharmacotherapy for cholangiocarcinoma: from conventional therapies to targeted drugs. Expert Opin Pharmacother. 2022;23:473–81.
Choi WJ, Williams PJ, Claasen M, et al. Systematic review and meta-analysis of prognostic factors for early recurrence in intrahepatic cholangiocarcinoma after curative-intent resection. Ann Surg Oncol. 2022;29:4337–53.
Tsilimigras DI, Mehta R, Moris D, et al. A machine-based approach to preoperatively identify patients with the most and least benefit associated with resection for intrahepatic cholangiocarcinoma: an international multi-institutional analysis of 1146 patients. Ann Surg Oncol. 2020;27:1110–9.
Li M, Du M, Cong H, et al. Characterization of hepatitis B virus DNA integration patterns in intrahepatic cholangiocarcinoma. Hepatol Res. 2021;51:102–15.
Wu ZY, Shen W, Yue JQ, et al. Combining immunoscore with clinicopathologic features in cholangiocarcinoma: an influential prognostic nomogram. Onco Targets Ther. 2020;13:11359–76.
Cheng Z, Lei Z, Jin X, et al. Postoperative adjuvant transarterial chemoembolization for intrahepatic cholangiocarcinoma patients with microvascular invasion: a propensity score analysis. J Gastrointest Oncol. 2021;12:819–30.
Kaibori M, Yoshii K, Kashiwabara K, et al. Impact of hepatitis C virus on survival in patients undergoing resection of intrahepatic cholangiocarcinoma: report of a Japanese nationwide survey. Hepatol Res. 2021;51:890–901.
Krenzien F, Nevermann N, Krombholz A, et al. Treatment of intrahepatic cholangiocarcinoma: a multidisciplinary approach. Cancers Basel. 2022;14:362.
Wei T, Zhang XF, He J, et al. Prognostic impact of perineural invasion in intrahepatic cholangiocarcinoma: multicentre study. Br J Surg. 2022;109:610–6.
Buettner S, Galjart B, van Vugt JLA, et al. Performance of prognostic scores and staging systems in predicting long-term survival outcomes after surgery for intrahepatic cholangiocarcinoma. J Surg Oncol. 2017;116:1085–95.
Langella S, Russolillo N, Ossola P, et al. Recurrence after curative resection for intrahepatic cholangiocarcinoma: how to predict the chance of repeat hepatectomy. J Clin Med. 2021;10:2820.
Alaimo L, Moazzam Z, Brown ZJ, et al. Application of hazard function to investigate recurrence of intrahepatic cholangiocarcinoma after curative-intent liver resection: a novel approach to characterize recurrence. Ann Surg Oncol. 2022;30:1340–9.
Li Q, Zhang J, Chen C, et al. A nomogram model to predict early recurrence of patients with intrahepatic cholangiocarcinoma for adjuvant chemotherapy guidance: a multi-institutional analysis. Front Oncol. 2022;12:896764.
Song Y, Cai M, Li Y, et al. The focus clinical research in intrahepatic cholangiocarcinoma. Eur J Med Res. 2022;27:116.
Tan YG, Fang AHS, Lim JKS, et al. Incorporating artificial intelligence in urology: supervised machine-learning algorithms demonstrate comparative advantage over nomograms in predicting biochemical recurrence after prostatectomy. Prostate. 2022;82:298–305.
Rahman SA, Walker RC, Maynard N, et al. The AUGIS survival predictor: prediction of long-term and conditional survival after esophagectomy using Random Survival Forests. Ann Surg. 2023;277(2):267–74.
Kudo SE, Ichimasa K, Villard B, et al. Artificial intelligence system to determine risk of T1 colorectal cancer metastasis to lymph node. Gastroenterology. 2021;160:1075-84.e2.
Ichimasa K, Kudo SE, Mori Y, et al. Artificial intelligence may help in predicting the need for additional surgery after endoscopic resection of T1 colorectal cancer. Endoscopy. 2018;50:230–40.
Amin MBES, Greene FL, et al. American Joint Committee on Cancer. Berlin: Springer; 2017.
Sasaki K, Morioka D, Conci S, et al. The tumor burden score: a new “metro-ticket” prognostic tool for colorectal liver metastases based on tumor size and number of tumors. Ann Surg. 2018;267:132–41.
Pang YY. The Brisbane 2000 terminology of liver anatomy and resections. HPB. 2000; 2:333–9. HPB Oxford. 2002;4:99; author reply 99–100.
Liang W, Xu L, Yang P, et al. Novel nomogram for preoperative prediction of early recurrence in intrahepatic cholangiocarcinoma. Front Oncol. 2018;8:360.
Moons KG, Altman DG, Reitsma JB, et al. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): explanation and elaboration. Ann Intern Med. 2015;162:W1-73.
Wilson A, Winner M, Yahanda A, et al. Factors associated with decisional regret among patients undergoing major thoracic and abdominal operations. Surgery. 2017;161:1058–66.
Winner M, Wilson A, Yahanda A, et al. Cancer surgeons’ attitudes and practices about discussing the chance of operative “cure.” Surgery. 2016;160:1619–27.
Bagante F, Spolverato G, Cucchetti A, et al. Defining when to offer operative treatment for intrahepatic cholangiocarcinoma: a regret-based decision curves analysis. Surgery. 2016;160:106–17.
Bridgewater J, Fletcher P, Palmer DH, et al. Long-term outcomes and exploratory analyses of the randomized phase III BILCAP study. J Clin Oncol. 2022;40:2048–57.
Akateh C, Ejaz AM, Pawlik TM, et al. Neoadjuvant treatment strategies for intrahepatic cholangiocarcinoma. World J Hepatol. 2020;12:693–708.
Buettner S, Koerkamp BG, Ejaz A, et al. The effect of preoperative chemotherapy treatment in surgically treated intrahepatic cholangiocarcinoma patients: a multi-institutional analysis. J Surg Oncol. 2017;115:312–8.
Li Z, Yuan L, Zhang C, et al. A novel prognostic scoring system of intrahepatic cholangiocarcinoma with machine learning basing on real-world data. Front Oncol. 2020;10:576901.
Li H, Liu R, Qiu H, et al. Tumor burden score stratifies prognosis of patients with intrahepatic cholangiocarcinoma after hepatic resection: a retrospective, multi-institutional study. Front Oncol. 2022;12:829407.
Zhang Z, Zhou Y, Hu K, et al. Perineural invasion as a prognostic factor for intrahepatic cholangiocarcinoma after curative resection and a potential indication for postoperative chemotherapy: a retrospective cohort study. BMC Cancer. 2020;20:270.
Nassar A, Tzedakis S, Sindayigaya R, et al. Factors of early recurrence after resection for intrahepatic cholangiocarcinoma. World J Surg. 2022;46:2459–67.
Zhang XF, Chakedis J, Bagante F, et al. Trends in use of lymphadenectomy in surgery with curative intent for intrahepatic cholangiocarcinoma. Br J Surg. 2018;105:857–66.
Acher AW, Paro A, Elfadaly A, et al. Intrahepatic cholangiocarcinoma: a summative review of biomarkers and targeted therapies. Cancers Basel. 2021;13:5169.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Dr. Hugo Marques has ownership of ophiomics precision medicine and is a consultant for JNJ and Roche. Dr. Guillaume Martel receives speaker’s honorarium from Incyte Biosciences. The remaining author have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alaimo, L., Lima, H.A., Moazzam, Z. et al. Development and Validation of a Machine-Learning Model to Predict Early Recurrence of Intrahepatic Cholangiocarcinoma. Ann Surg Oncol 30, 5406–5415 (2023). https://doi.org/10.1245/s10434-023-13636-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13636-8