Abstract
Background
Approximately 14% of women undergoing breast-conserving surgery (BCS) require re-excision to achieve negative margins following the Society of Surgical Oncology (SSO) and American Society for Radiation Oncology (ASTRO) margin guidelines, which may influence patient-reported outcomes (PROs). Few studies have assessed the impact of re-excision on PROs following BCS.
Patients and Methods
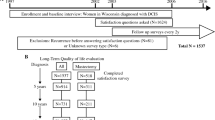
Women with stage 0–III breast cancer undergoing BCS who completed a BREAST-Q PRO measure from 2010 to 2016 were identified from a prospective database. Baseline characteristics were compared between women who underwent one BCS and those who underwent ≥ 1 re-excision surgery for positive margins (R-BCS). Linear mixed models were used to analyze associations between number of excisions and BREAST-Q scores over time.
Results
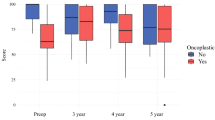
Of 2543 eligible women, 1979 (78%) had one BCS and 564 (22%) had R-BCS. Younger age, lower BMI, surgery pre-SSO Invasive Guidelines issuance, ductal carcinoma in situ (DCIS), multifocal disease, radiation therapy receipt, and endocrine therapy omission were more common in the R-BCS group. Breast satisfaction and sexual well-being were lower in the R-BCS group 2 years postoperatively. There were no differences in psychosocial well-being between groups over 5 years. On multivariable analysis, re-excision was associated with lower breast satisfaction and sexual well-being (p= 0.007 and p= 0.049, respectively), but there was no difference in psychosocial well-being (p= 0.250).
Conclusions
Women with R-BCS had lower breast satisfaction and sexual well-being 2 years postoperatively, but this difference did not remain long term. Psychosocial well-being in women who underwent one BCS were largely comparable over time to the R-BCS group. These findings may help in counseling women who are concerned about satisfaction and quality-of-life outcomes with BCS if re-excision is necessary.

Similar content being viewed by others
References
Blichert-Toft M, Nielsen M, Düring M, et al. Long-term results of breast conserving surgery vs. mastectomy for early stage invasive breast cancer: 20-year follow-up of the Danish randomized DBCG-82TM protocol. Acta Oncol. 2008;47(4):672–81.
Christiansen P, Carstensen SL, Ejlertsen B, et al. Breast conserving surgery versus mastectomy: overall and relative survival-a population based study by the Danish Breast Cancer Cooperative Group (DBCG). Acta Oncol. 2018;57(1):19–25.
Darby S, McGale P, Correa C, et al. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet. 2011;378(9804):1707–16.
Fisher B, Anderson S, Bryant J, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med. 2002;347(16):1233–41.
Poggi MM, Danforth DN, Sciuto LC, et al. Eighteen-year results in the treatment of early breast carcinoma with mastectomy versus breast conservation therapy: the National Cancer Institute Randomized Trial. Cancer. 2003;98(4):697–702.
Veronesi U, Cascinelli N, Mariani L, et al. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med. 2002;347(16):1227–32.
Kummerow KL, Du L, Penson DF, Shyr Y, Hooks MA. Nationwide trends in mastectomy for early-stage breast cancer. JAMA Surg. 2015;150(1):9–16.
Nelson JA, Rubenstein RN, Haglich K, et al. Analysis of a trend reversal in US lumpectomy rates from 2005 through 2017 using 3 nationwide data sets. JAMA Surg. 2022;157(8):702–11.
Havel L, Naik H, Ramirez L, Morrow M, Landercasper J. Impact of the SSO-ASTRO margin guideline on rates of re-excision after lumpectomy for breast cancer: a meta-analysis. Ann Surg Oncol. 2019;26(5):1238–44.
Kuritzky A, Reyna C, McGuire KP, et al. Evaluation of 2014 margin guidelines on re-excision and recurrence rates after breast conserving surgery: a multi-institution retrospective study. Breast. 2020;51:29–33.
Monaghan A, Chapinal N, Hughes L, Baliski C. Impact of SSO-ASTRO margin guidelines on reoperation rates following breast-conserving surgery. Am J Surg. 2019;217(5):862–7.
Klassen AF, Pusic AL, Scott A, Klok J, Cano SJ. Satisfaction and quality of life in women who undergo breast surgery: a qualitative study. BMC Womens Health. 2009;9:11.
Norris D, Julian TB. Update on the NSABP B-39/RTOG 0413 clinical trial. Oncol Issues. 2008;23:20–1.
Olivotto IA, Whelan TJ, Parpia S, et al. Interim cosmetic and toxicity results from RAPID: a randomized trial of accelerated partial breast irradiation using three-dimensional conformal external beam radiation therapy. J Clin Oncol. 2013;31(32):4038–45.
Troidl H, Kusche J, Vestweber KH, Eypasch E, Koeppen L, Bouillon B. Quality of life: an important endpoint both in surgical practice and research. J Chronic Dis. 1987;40(6):523–8.
Al-Ghazal SK, Fallowfield L, Blamey RW. Does cosmetic outcome from treatment of primary breast cancer influence psychosocial morbidity? Eur J Surg Oncol. 1999;25(6):571–3.
Heil J, Holl S, Golatta M, et al. Aesthetic and functional results after breast conserving surgery as correlates of quality of life measured by a German version of the Breast Cancer Treatment Outcome Scale (BCTOS). Breast. 2010;19(6):470–4.
Waljee JF, Hu ES, Ubel PA, Smith DM, Newman LA, Alderman AK. Effect of esthetic outcome after breast-conserving surgery on psychosocial functioning and quality of life. J Clin Oncol. 2008;26(20):3331–7.
Cardoso MJ, Cardoso J, Santos AC, et al. Factors determining esthetic outcome after breast cancer conservative treatment. Breast J. 2007;13(2):140–6.
Fedorcik GG, Sachs R, Goldfarb MA. Oncologic and aesthetic results following breast-conserving therapy with 0.5 cm margins in 100 consecutive patients. Breast J. 2006;12(3):208–11.
Taylor ME, Perez CA, Halverson KJ, et al. Factors influencing cosmetic results after conservation therapy for breast cancer. Int J Radiat Oncol Biol Phys. 1995;31(4):753–64.
Wang HT, Barone CM, Steigelman MB, et al. Aesthetic outcomes in breast conservation therapy. Aesthet Surg J. 2008;28(2):165–70.
Wazer DE, DiPetrillo T, Schmidt-Ullrich R, et al. Factors influencing cosmetic outcome and complication risk after conservative surgery and radiotherapy for early-stage breast carcinoma. J Clin Oncol. 1992;10(3):356–63.
Heil J, Breitkreuz K, Golatta M, et al. Do reexcisions impair aesthetic outcome in breast conservation surgery? Exploratory analysis of a prospective cohort study. Ann Surg Oncol. 2012;19(2):541–7.
O’Connell RL, DiMicco R, Khabra K, et al. Initial experience of the BREAST-Q breast-conserving therapy module. Breast Cancer Res Treat. 2016;160(1):79–89.
Stolpner I, Heil J, Riedel F, et al. Long-term patient satisfaction and quality of life after breast-conserving therapy: a prospective study using the BREAST-Q. Ann Surg Oncol. 2021;28(13):8742–51.
Klassen AF, Dominici L, Fuzesi S, et al. Development and validation of the BREAST-Q breast-conserving therapy module. Ann Surg Oncol. 2020;27(7):2238–47.
Baliski C, Bakos B. Patient reported outcomes following breast conserving surgery are improved by minimizing re-excisions and excessive breast tissue removal. Am J Surg. 2022;224(2):716–21.
Haloua MH, Volders JH, Krekel NM, et al. Intraoperative ultrasound guidance in breast-conserving surgery improves cosmetic outcomes and patient satisfaction: results of a multicenter randomized controlled trial (COBALT). Ann Surg Oncol. 2016;23(1):30–7.
Ojala K, Meretoja TJ, Leidenius MH. Aesthetic and functional outcome after breast conserving surgery - comparison between conventional and oncoplastic resection. Eur J Surg Oncol. 2017;43(4):658–64.
Volders JH, Negenborn VL, Haloua MH, et al. Breast-specific factors determine cosmetic outcome and patient satisfaction after breast-conserving therapy: results from the randomized COBALT study. J Surg Oncol. 2018;117(5):1001–8.
Chen CM, Cano SJ, Klassen AF, et al. Measuring quality of life in oncologic breast surgery: a systematic review of patient-reported outcome measures. Breast J. 2010;16(6):587–97.
BREAST-Q Website. https://qportfolio.org/breast-q/ (Accessed May 24, 2022).
Vrouwe SQ, Somogyi RB, Snell L, McMillan C, Vesprini D, Lipa JE. Patient-reported outcomes following breast conservation therapy and barriers to referral for partial breast reconstruction. Plast Reconstr Surg. 2018;141(1):1–9.
Lagendijk M, van Egdom LSE, van Veen FEE, et al. Patient-reported outcome measures may add value in breast cancer surgery. Ann Surg Oncol. 2018;25(12):3563–71.
Voineskos SH, Klassen AF, Cano SJ, Pusic AL, Gibbons CJ. Giving meaning to differences in BREAST-Q scores: minimal important difference for breast reconstruction patients. Plast Reconstr Surg. 2020;145(1):11e–20e.
Acknowledgment
The preparation of this study was supported in part by NIH/NCI Cancer Center Support Grant P30CA008748 to Memorial Sloan Kettering Cancer Center.
Funding
NIH/NCI Cancer Center Support Grant, P30CA008748.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
This study was presented in poster format at the 44th Annual San Antonio Breast Cancer Symposium, December 7-10, 2021, San Antonio, TX. All authors have no conflicts of interest or commercial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Matar-Ujvary, R., Haglich, K., Flanagan, M.R. et al. The Impact of Breast-Conserving Surgery Re-excision on Patient-Reported Outcomes Using the BREAST-Q. Ann Surg Oncol 30, 5341–5349 (2023). https://doi.org/10.1245/s10434-023-13592-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13592-3