Abstract
Background
According to the JCOG0802 study, there were many non-cancer-related deaths in the lobectomy group. Meanwhile, the median age of the enrolled patients in the JCOG0802 study was 67 years old. Whether this difference in perioperative outcomes and survival outcomes is related to age remains unknown. We aim to investigate whether the sublobectomy was comparable to lobectomy in elderly (≥ 75 years old) patients with peripheral solid-dominant [50% ≤ consolidation tumor ratio (CTR) ≤ 1] and diameter ≤ 2 cm non-small cell lung cancer (NSCLC).
Methods
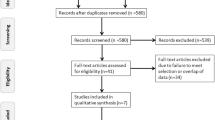
We retrospectively included 10,830 patients who underwent surgery treatment at two large-volume medical centers, Taizhou Hospital of Zhejiang Province and Shanghai Chest Hospital, from January 2016 to January 2018. Of these, 164 patients aged ≥ 75 years, tumor ≤ 2 cm, and 50% ≤ CTR ≤ 1 who received lobectomy or sublobectomy were included in our study. The perioperative outcomes, survival analyses, analysis of death patterns, tumor recurrence patterns, and Cox regression analyses were performed.
Results
On perioperative outcomes, sublobectomy was associated with a shorter operation time (p < 0.001), and in terms of survival outcomes, the 5-year overall survival (OS, p = 0.85) and 5-year disease-free surivial (DFS, p = 0.58) did not differ significantly between the two groups. The Cox regression analyses showed that CTR value, visceral pleural infiltration, and smoking were independent risk factors for worse OS. Furthermore, tumor recurrence pattern and death patterns between the two groups did not differ significantly.
Conclusions
Sublobectomy could achieve superior perioperative outcomes and equivalent oncological efficacy in comparison with lobectomy in elderly patients (≥ 75 years old) with peripheral solid-dominant and diameter ≤ 2 cm NSCLC.




Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68:394–424.
Brooks ED, Sun B, Zhao L, et al. Stereotactic ablative radiation therapy is highly safe and effective for elderly patients with early-stage non-small cell lung cancer. Int J Radiat Oncol Biol Phys. 2017;98:900–7.
Clérigo V, Hasmucrai D, Teixeira E, et al. Characterization and management of elderly and very elderly patients with non-small cell lung cancer. Clin Respir J. 2020;14:683–6.
Schellevis FG, van der Velden J, van de Lisdonk E, et al. Comorbidity of chronic diseases in general practice. J Clin Epidemiol. 1993;46:469–73.
Mannino DM, Buist AS. Global burden of COPD: risk factors, prevalence, and future trends. Lancet (London, England). 2007;370:765–73.
Pennathur A, Brunelli A, Criner GJ, et al. Definition and assessment of high risk in patients considered for lobectomy for stage I non-small cell lung cancer: the American Association for Thoracic Surgery expert panel consensus document. J Thorac Cardiovasc Surg 2021;162.
Gu Y, Zhang J, Zhou Z, et al. Metastasis patterns and prognosis of octogenarians with NSCLC: a population-based study. Aging Dis. 2020;11:82–92.
Ginsberg RJ, Rubinstein LV. Randomized trial of lobectomy versus limited resection for T1 N0 non-small cell lung cancer. Lung Cancer Study Group. Ann Thorac Surg 1995;60:615-22; discussion 22–3.
Saji H, Okada M, Tsuboi M, et al. Segmentectomy versus lobectomy in small-sized peripheral non-small-cell lung cancer (JCOG0802/WJOG4607L): a multicentre, open-label, phase 3, randomised, controlled, non-inferiority trial. Lancet. 2022;399:1607–17.
Aberle DR, DeMello S, Berg CD, et al. Results of the two incidence screenings in the National Lung Screening Trial. N Engl J Med. 2013;369:920–31.
Miao XH, Yao YW, Yuan DM, et al. Prognostic value of the ratio of ground glass opacity on computed tomography in small lung adenocarcinoma: a meta-analysis. J Thorac Dis. 2012;4:265–71.
Huang TW, Lin KH, Huang HK, et al. The role of the ground-glass opacity ratio in resected lung adenocarcinoma. Eur J Cardiothorac Surg. 2018;54:229–34.
Moon Y, Lee KY, Moon SW, et al. Sublobar resection margin width does not affect recurrence of clinical N0 non-small cell lung cancer presenting as GGO-predominant nodule of 3 cm or less. World J Surg. 2017;41:472–9.
Acknowledgement
The authors thank Taizhou Hospital of Zhejiang Province affiliated to Wenzhou Medical University and Shanghai Chest Hospital, Shanghai Jiao Tong University School of Medicine for providing the research environment.
Funding
This study was supported by Grants from the National Natural Science Foundation of China (NSFC) (Grant No. 82002420), the National Natural Science Foundation of China (Grant No.82272679), Shanghai Talent Development Fund (Grant No.2019073), and the Natural Science Foundation of Zhejiang Province (Grant No. LY19H160018).
Author information
Authors and Affiliations
Contributions
S.W., Z.W., and J.S. drafted the manuscript. S.W., Z.J., S.R., and B.H. made and processed the figures and tables. W.C., H.W., and C.Z. revised the manuscript. T.C. and J.S. administrated this project. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Disclosure
The authors declare no potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, S., Wang, Z., Sun, J. et al. Survival Outcomes of Sublobectomy and Lobectomy in Elderly Patients with Peripheral Solid-Dominant Non-small Cell Lung Cancer. Ann Surg Oncol 30, 1522–1529 (2023). https://doi.org/10.1245/s10434-022-12909-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12909-y