Abstract
Introduction
Up to 25% of colorectal cancer patients present with synchronous liver metastases that can be treated with two operations or a single ‘simultaneous’ operation. Morbidity and mortality appear similar between approaches, however changes in health-related quality-of-life following simultaneous resection are not well reported.
Methods
A prospective, feasibility trial for simultaneous resection of synchronous colorectal liver metastases was conducted. Patients completed the European Organization for Research and Treatment of Cancer QLQ-C30 and LMC21 at baseline (preoperatively), and 4 and 12 weeks postoperatively. Week 4 and 12 scores were compared with baseline using t-tests. Minimally important clinical differences were considered as a 10-point difference from baseline.
Results
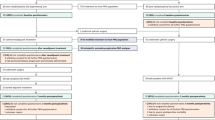
C30 and QLQ-LMC21 were completed at baseline, 4 weeks, and 12 weeks by 39 (95%), 35 (85%) and 34 (83%) patients, and 39 (95%), 33 (80%) and 33 (80%) patients, respectively; 79% and 75% had at least one MICD according to QLQ-C30 at 4 and 12 weeks. At 4 weeks, physical functioning (mean difference (MD) − 11.9%, p = 0.002), role functioning (MD − 23.6, p = 0.007), and pain (MD + 19.7, p = 0.017) had significant worsening from baseline. At 12 weeks postoperatively, role functioning (MD − 19.7, p = 0.011) and fatigue (MD + 14.3, p = 0.03) were the only domains that remained significantly worse. By 12 weeks, pain and physical functioning had returned to baseline. There were no major demographic differences among those with and without an MICD at 12 weeks.
Conclusions
Simultaneous resection of colorectal liver metastases led to clinically significant worsening fatigue and role functioning that persisted at 12 weeks post-surgery.


Similar content being viewed by others
References
Manfredi S, Lepage C, Hatem C, Coatmeur O, Faivre J, Bouvier A-M. Epidemiology and management of liver metastases from colorectal cancer. Ann Surgery. 2006;244(2):254–9.
Leporrier J, Maurel J, Chiche L, Bara S, Segol P, Launoy G. A population-based study of the incidence, management and prognosis of hepatic metastases from colorectal cancer. Br J Surgery. 2006;93(4):465–74.
Engstrand J, Nilsson H, Strömberg C, Jonas E, Freedman J. Colorectal cancer liver metastases - a population-based study on incidence, management and survival. BMC Cancer. 2018;18(1):78.
Aghayan DL, Kazaryan AM, Dagenborg VJ, et al. Long-term oncologic outcomes after laparoscopic versus open resection for colorectal liver metastases: A randomized trial. Ann Intern Med. 2021;174(2):175–82.
Abelson JS, Michelassi F, Sun T, et al. Simultaneous resection for synchronous colorectal liver metastasis: The new standard of care? J Gastrointest Surgery. 2017;21(6):975–82.
Vallance AE, van der Meulen J, Kuryba A, et al. The timing of liver resection in patients with colorectal cancer and synchronous liver metastases: a population-based study of current practice and survival. Colorectal Dis. 2018;20(6):486–95.
Griffiths C, Bogach J, Simunovic M, et al. Simultaneous resection of colorectal cancer with synchronous liver metastases; a practice survey. HPB (Oxford). 2020;22(5):728–34.
Howard C, Clements TW, Edwards JP, et al. Synchronous colorectal liver metastases: a national survey of surgeon opinions on simultaneous resection and multidisciplinary cooperation. Hepatobiliary Surgery Nutr. 2018;7(4):242–50.
Bogach J, Wang J, Griffiths C, et al. Simultaneous versus staged resection for synchronous colorectal liver metastases: A population-based cohort study. Int J Surgery. 2020;74:68–75.
Reddy SK, Pawlik TM, Zorzi D, et al. Simultaneous resections of colorectal cancer and synchronous liver metastases: a multi-institutional analysis. Ann Surg Oncol. 2007;14(12):3481–91.
Boudjema K, Locher C, Sabbagh C, et al. Simultaneous versus delayed resection for initially resectable synchronous colorectal cancer liver metastases: a prospective, open-label, randomized, controlled trial. Ann Surgery. 2021;273(1):49–56.
Church J. Quality of life and patient-reported outcomes. British Journal of Surgery. 2018;105(3):157–8.
Urbach DR. Measuring quality of life after surgery. Surg Innov. 2005;12(2):161–5.
Reudink M, Molenaar CJL, Bonhof CS, Janssen L, Mols F, Slooter GD. Evaluating the longitudinal effect of colorectal surgery on health-related quality of life in patients with colorectal cancer. J Surg Oncol. 2022;125(2):217–26.
Wee IJY, Syn N, Lee LS, Tan SS, Chiow AKH. A systematic review and meta-analysis on the quality of life after hepatic resection. HPB (Oxford). 2020;22(2):177–86.
Kang BM, Lee YS, Kim JH, et al. Quality of life and patient satisfaction after single- and multiport laparoscopic surgery in colon cancer: a multicentre randomised controlled trial (SIMPLE Trial). Surg Endosc. 2021;35(11):6278–90.
Studer P, Horn T, Haynes A, Candinas D, Banz VM. Quality of life after hepatic resection. Br J Surg. 2018;105(3):237–43.
Serrano PE, Parpia S, Karanicolas P, et al. Simultaneous resection for synchronous colorectal cancer liver metastases: a feasibility clinical trial. J Surg Oncol. 2022;125(4):671–7.
Serrano PE, Gafni A, Parpia S, et al. Simultaneous resection of colorectal cancer with synchronous liver metastases (RESECT), a pilot study. Int J Surg Protoc. 2018;8:1–6.
Strasberg SM. Nomenclature of hepatic anatomy and resections: a review of the Brisbane 2000 system. J Hepatobiliary Pancreat Surg. 2005;12(5):351–5.
Dindo D, Demartines N, Clavien P-A. Classification of surgical complications. Ann Surgery. 2004;240(2):205–13.
Groenvold M, Klee MC, Sprangers MA, Aaronson NK. Validation of the EORTC QLQ-C30 quality of life questionnaire through combined qualitative and quantitative assessment of patient-observer agreement. J Clin Epidemiol. 1997;50(4):441–50.
Blazeby JM, Fayers P, Conroy T, et al. Validation of the European organization for research and treatment of cancer QLQ-LMC21 questionnaire for assessment of patient-reported outcomes during treatment of colorectal liver metastases. Br J Surgery. 2009;96(3):291–8.
Ringash J, O’Sullivan B, Bezjak A, Redelmeier DA. Interpreting clinically significant changes in patient-reported outcomes. Cancer. 2007;110(1):196–202.
RStudio: integrated development for R [computer program]. Boston, MA: PBC; 2020.
King PM, Blazeby JM, Ewings P, et al. The influence of an enhanced recovery programme on clinical outcomes, costs and quality of life after surgery for colorectal cancer. Colorectal Dis. 2006;8(6):506–13.
Janson M, Lindholm E, Anderberg B, Haglind E. Randomized trial of health-related quality of life after open and laparoscopic surgery for colon cancer. Surg Endosc. 2007;21(5):747–53.
Eaton AA, Gonen M, Karanicolas P, et al. Health-related quality of life after pancreatectomy: Results from a randomized controlled trial. Ann Surg Oncol. 2016;23(7):2137–45.
Serrano PE, Herman JM, Griffith KA, et al. Quality of life in a prospective, multicenter phase 2 trial of neoadjuvant full-dose gemcitabine, oxaliplatin, and radiation in patients with resectable or borderline resectable pancreatic adenocarcinoma. Int J Radiat Oncol Biol Phys. 2014;90(2):270–7.
Domati F, Luppi G, Reggiani-Bonetti L, et al. The perception of health-related quality of life in colon cancer patients during chemotherapy: differences between men and women. Intern Emerg Med. 2015;10(4):423–9.
Moaven O, Votanopoulos KI, Shen P, et al. Health-related quality of life after cytoreductive surgery/HIPEC for mucinous appendiceal cancer: Results of a multicenter randomized trial comparing oxaliplatin and mitomycin. Ann Surg Oncol. 2020;27(3):772–80.
Cheng KKF, Clark AM. Qualitative methods and patient-reported outcomes: Measures development and adaptation. Int J Qual Methods. 2017;16(1):1609406917702983.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Griffiths, C.D., Karanicolas, P., Gallinger, S. et al. Health-Related Quality of Life Following Simultaneous Resection for Synchronous Colorectal Cancer Liver Metastases. Ann Surg Oncol 30, 1331–1338 (2023). https://doi.org/10.1245/s10434-022-12696-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12696-6