Abstract
Introduction
The revision of the N descriptor in non-small-cell lung cancer has been widely discussed in the past few years. Many different subclassification methods based on number or location of lymph nodes have been proposed for better distinguishing different N patients. This study aimed to systematically collect them and provide a comprehensive comparison among different subclassification methods in a large cohort.
Method
Pathological N1 or N2 non-small-cell lung cancer patients undergoing surgical resection between 2005 and 2016 in the Western China Lung Cancer Database were retrospectively reviewed. A literature review was conducted to collect previous subclassification methods. Kaplan-Meier and multivariable Cox analyses were used to examine the prognostic performance of subclassification methods. Decision curve analysis, Akaike’s information criterion, and area under the receiver operating curve concordance were also performed to evaluate the standardized net benefit of the subclassification methods.
Results
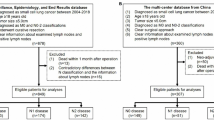
A total of 1625 patients were identified in our cohort. Eight subclassification methods were collected from previous articles and further grouped into subclassification based on number categories (node number or station number), location categories (lymph node zone or chain) or combination of number and location categories. Subclassification based on combination of lymph node location and number tended to have better discrimination ability in multivariable Cox analysis. No significant superiority among the different subclassification methods was observed in the three statistical models.
Conclusion
Subclassification based on the combination of location and number could be used to provide a more accurate prognostic stratification in surgically resected NSCLC and is worth further validation.



Similar content being viewed by others
References
Goldstraw P, Chansky K, Crowley J, et al. The IASLC lung cancer staging project: proposals for revision of the TNM stage groupings in the forthcoming (Eighth) edition of the TNM classification for lung cancer. J Thorac Oncol. 2016;11(1):39–51.
Rusch VW, Crowley J, Giroux DJ, et al. The IASLC lung cancer staging project: proposals for the Revision of the N descriptors in the forthcoming seventh edition of the TNM classification for lung cancer. J Thorac Oncol. 2007;2(7):603–12.
Asamura H, Chansky K, Crowley J, et al. The international association for the study of lung cancer lung cancer staging project. J Thorac Oncol. 2015;10(12):1675–84.
Park BJ, Kim TH, Shin S, et al. Recommended change in the N descriptor proposed by the international association for the study of lung cancer: a validation study. J Thorac Oncol. 2019;14(11):1962–9.
Chiappetta M, Lococo F, Leuzzi G, et al. External validation of the N descriptor in the proposed tumour-node-metastasis subclassification for lung cancer: the crucial role of histological type, number of resected nodes and adjuvant therapy. Eur J Cardiothorac Surg. 2020;58(6):1236–44.
Chen W, Zhang C, Wang G, Yu Z, Liu H. Feasibility of nodal classification for non-small cell lung cancer by merging current N categories with the number of involved lymph node stations. Thorac Cancer. 2019;10(7):1533–43.
Yun JK, Lee GD, Choi S, et al. Comparison between lymph node station- and zone-based classification for the future revision of node descriptors proposed by the international association for the study of lung cancer in surgically resected patients with non-small-cell lung cancer. Eur J Cardiothorac Surg. 2019;56(5):849–57.
Yu Y, Zhang P, Yao R, et al. Prognostic value of log odds of positive lymph nodes in node-positive lung squamous cell carcinoma patients after surgery: a SEER population-based study. Transl Lung Cancer Res. 2020;9(4):1285–301.
Tsitsias T, Okiror L, Veres L, et al. New N1/N2 classification and lobe specific lymphatic drainage: Impact on survival in patients with non-small cell lung cancer treated with surgery. Lung Cancer. 2021;151:84–90.
Xu L, Su H, She Y, et al. Which N descriptor is more predictive of prognosis in resected non-small cell lung cancer: the number of involved nodal stations or the location-based pathological N stage? Chest. 2021;159(6):2458–69.
Rusch VW, Asamura H, Watanabe H, Giroux DJ, Rami-Porta R, Goldstraw P. The IASLC lung cancer staging project: a proposal for a new international lymph node map in the forthcoming seventh edition of the TNM classification for lung cancer. J Thorac Oncol. 2009;4(5):568–77.
Liu C, Wei S, Guo C, Mei J, Pu Q, Liu L. Clinical significance of station 3A lymph node dissection in patients with right-side non-small-cell lung cancer: a retrospective propensity-matched analysis. Annal Surg Oncol. 2021;28(1):194–202.
Aksoy Y, Çıtak N, Obuz Ç, Metin M, Sayar A. Does anatomical location-based metastatic lymph node density affect prognosis in lung cancer patients? Interact Cardiovasc Thorac Surg. 2021;33(4):541–9.
Bertoglio P, Ricciardi S, Alì G, et al. N2 lung cancer is not all the same: an analysis of different prognostic groups. Interact CardioVascular Thorac Surg. 2018;27(5):720–6.
Kojima H, Terada Y, Yasuura Y, et al. Prognostic impact of the number of involved lymph node stations in patients with completely resected non-small cell lung cancer: a proposal for future revisions of the N classification. Gen Thorac Cardiovasc Surg. 2020;68(11):1298–304.
Baba T, Uramoto H, Kuwata T, et al. Survival impact of node zone classification in resected pathological N2 non-small cell lung cancer. Interact Cardiovasc Thorac Surg. 2012;14(6):760–4.
Demir A, Turna A, Kocaturk C, et al. Prognostic significance of surgical-pathologic N1 lymph node involvement in non-small cell lung cancer. Ann Thorac Surg. 2009;87(4):1014–22.
Eichhorn F, Klotz LV, Muley T, Kobinger S, Winter H, Eichhorn ME. Prognostic relevance of regional lymph-node distribution in patients with N1-positive non-small cell lung cancer: A retrospective single-center analysis. Lung Cancer. 2019;138:95–101.
Zheng H, Wang LM, Bao F, et al. Re-appraisal of N2 disease by lymphatic drainage pattern for non-small-cell lung cancers: by terms of nodal stations, zones, chains, and a composite. Lung Cancer. 2011;74(3):497–503.
Li S, Yan S, Lu F, et al. Validation of the 8th edition nodal staging and proposal of new nodal categories for future edition of the TNM classification of non-small cell lung cancer. Ann Surg Oncol. 2021;28(8):4510–6.
Ding X, Hui Z, Dai H, et al. A proposal for combination of lymph node ratio and anatomic location of involved lymph nodes for nodal classification in non-small cell lung cancer. J Thorac Oncol. 2016;11(9):1565–73.
Jonnalagadda S, Smith C, Mhango G, Wisnivesky JP. The number of lymph node metastases as a prognostic factor in patients with N1 non-small cell lung cancer. Chest. 2011;140(2):433–40.
Lee JG, Lee CY, Park IK, et al. Number of metastatic lymph nodes in resected non-small cell lung cancer predicts patient survival. Ann Thorac Surg. 2008;85(1):211–5.
Li F, Yuan L, Zhao Y, Wang S, Lv Z, Mao Y. Comparison of two proposed changes to the current nodal classification for non-small cell lung cancer based on the number and ratio of metastatic lymph nodes. Chest. 2021;160(4):1520–33.
Maniwa T, Ohmura A, Hiroshima T, et al. Number of metastatic lymph nodes and zones as prognostic factors in non-small-cell lung cancer. Interact Cardiovasc Thorac Surg. 2020;31(3):305–14.
Saji H, Tsuboi M, Shimada Y, et al. A proposal for combination of total number and anatomical location of involved lymph nodes for nodal classification in non-small cell lung cancer. Chest. 2013;143(6):1618–25.
Lee GD, Kim DK, Moon DH, et al. A comparison of the proposed classifications for the revision of N descriptors for non-small-cell lung cancer. Eur J Cardiothorac Surg. 2016;49(2):580–8.
Pawełczyk K, Marciniak M, Błasiak P. Evaluation of new classifications of N descriptor in non-small cell lung cancer (NSCLC) based on the number and the ratio of metastatic lymph nodes. J Cardiothorac Surg. 2016;11(1):68.
Deng W, Xu T, Wang Y, et al. Log odds of positive lymph nodes may predict survival benefit in patients with node-positive non-small cell lung cancer. Lung Cancer. 2018;122:60–6.
Dziedzic D, Piotr R, Langfort R, Orlowski T. Log odds of positive lymph nodes as a novel prognostic indicator in NSCLC staging. Surg Oncol. 2017;26(1):80–5.
Smeltzer MP, Faris NR, Ray MA, Osarogiagbon RU. Association of pathologic nodal staging quality with survival among patients with non-small cell lung cancer after resection with curative intent. JAMA Oncol. 2018;4(1):80.
Smeltzer MP, Faris N, Yu X, et al. Missed intrapulmonary lymph node metastasis and survival after resection of non-small cell lung cancer. Ann Thorac Surg. 2016;102(2):448–53.
Ramirez RA, Wang CG, Miller LE, et al. Incomplete intrapulmonary lymph node retrieval after routine pathologic examination of resected lung cancer. J Clin Oncol. 2012;30(23):2823–8.
Ray MA, Fehnel C, Akinbobola O, et al. Comparative effectiveness of a lymph node collection kit versus heightened awareness on lung cancer surgery quality and outcomes. J Thorac Oncol. 2021;16(5):774–83.
Funding
This study was supported by the 1.3.5 Project for Disciplines of Excellence ZYGD18021 to Lunxu Liu, West China Hospital, Sichuan University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors have declared no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Z., Yang, Z., Li, S. et al. A Comprehensive Comparison of Different Nodal Subclassification Methods in Surgically Resected Non-Small-Cell Lung Cancer Patients. Ann Surg Oncol 29, 8144–8153 (2022). https://doi.org/10.1245/s10434-022-12363-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12363-w