Abstract
Background
Current standard management for intraductal papilloma (IDP) diagnosed at biopsy indicates complete surgical resection, but there are increasing controversies over whether and when routine excision is indeed necessary.
Objective
The aim of this study was to determine the carcinoma upgrade rate and identify the associated predictive factors for IDP diagnosed at biopsy by meta-analysis.
Methods
We searched the PubMed and EMBASE databases for studies published from 2009 to 2020 that investigated the upgrade rate and predictive factors of IDP diagnosed at biopsy.
Results
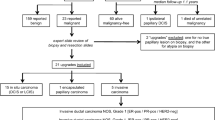
A total of 7016 IDP cases diagnosed at biopsy and histologically examined after surgical excision were pooled from 44 original studies. The pooled prevalence of IDP in breast biopsy findings was 4.6% [95% confidence interval (CI) 4.4–4.7%] and the majority of IDP tumors were benign. The pooled upgrade rates to carcinoma for benign IDP and atypical IDP were 5.0% (95% CI 4.4–5.5%) and 36.0% (95% CI 32.7–39.2%), respectively. In addition, we identified 10 predictive upgrade factors for benign IDP, including Breast Imaging Reporting and Data System (BI-RADS) 5, BI-RADS 4C, mass and calcification in the mammographic finding, bloody nipple discharge, imaging–histological discordance, peripheral IDP, palpable mass, BI-RADS 4B, microcalcification, and lesion size ≥ 1 cm. The upgrade rates associated with these predictive factors ranged from 7.3 to 31.1%.
Conclusion
Surgical excision appears a reasonable recommendation for atypical IDP. Patients with benign IDP exhibiting one or more predictive factors might benefit from surgical excision, while patients with asymptomatic benign IDP without these predictive factors can be managed by imaging surveillance.



Similar content being viewed by others
References
Ueng S-H, Mezzetti T, Tavassoli FA. Papillary neoplasms of the breast: a review. Arch Pathol Lab Med. 2009;133(6):893–907.
Foley NM, Racz JM, Al-Hilli Z, et al. An international multicenter review of the malignancy rate of excised papillomatous breast lesions. Ann Surg Oncol. 2015;22(Suppl 3):385–90.
Kuehner G, Darbinian J, Habel L, et al. Benign papillary breast mass lesions: favorable outcomes with surgical excision or imaging surveillance. Ann Surg Oncol. 2019;26(6):1695–703.
Pareja F, Corben AD, Brennan SB, et al. Breast intraductal papillomas without atypia in radiologic-pathologic concordant core-needle biopsies: rate of upgrade to carcinoma at excision. Cancer. 2016;122(18):2819–27.
Jaffer S, Nagi C, Bleiweiss IJ. Excision is indicated for intraductal papilloma of the breast diagnosed on core needle biopsy. Cancer. 2009;115(13):2837–43.
Kim MJ, Kim S-I, Youk JH, et al. The diagnosis of non-malignant papillary lesions of the breast: comparison of ultrasound-guided automated gun biopsy and vacuum-assisted removal. Clin Radiol. 2011;66(6):530–5.
Rizzo M, Linebarger J, Lowe MC, et al. Management of papillary breast lesions diagnosed on core-needle biopsy: clinical pathologic and radiologic analysis of 276 cases with surgical follow-up. J Am Coll Surg. 2012;214(3):280–7.
Destounis S, Seifert P, Somerville P, et al. Underestimation of papillary breast lesions by core biopsy: correlation to surgical excision. Breast Cancer. 2014;21(2):128–34.
Moynihan A, Quinn EM, Smith CS, et al. Benign breast papilloma: is surgical excision necessary? Breast J. 2020;26(4):705–10.
Genco IS, Tugertimur B, Manolas PA, et al. Upgrade rate of intraductal papilloma without atypia on breast core needle biopsy: a clinical, radiological and pathological correlation study. Am J Surg. 2020;220(3):677–81.
MacColl C, Salehi A, Parpia S, et al. Benign breast papillary lesions diagnosed on core biopsy: upgrade rate and risk factors associated with malignancy on surgical excision. Virchows Arch. 2019;475(6):701–7.
Yu Y, Salisbury E, Gordon-Thomson D, et al. Management of papillary lesions without atypia of the breast diagnosed on needle biopsy. ANZ J Surg. 2019;89(5):524–8.
Li X, Aho M, Newell MS, et al. Papilloma diagnosed on core biopsies has a low upgrade rate. Clin Imaging. 2019;60(1):67–74.
Liu C, Sidhu R, Ostry A, et al. Risk of malignancy in papillary neoplasms of the breast. Breast Cancer Res Treat. 2019;178(1):87–94.
Leithner D, Kaltenbach B, Hödl P, et al. Intraductal papilloma without atypia on image- guided breast biopsy: upgrade rates to carcinoma at surgical excision. Breast Care. 2018;13(5):364–8.
Chang JM, Moon WK, Cho N, et al. Management of ultrasonographically detected benign papillomas of the breast at core needle biopsy. Am J Roentgenol. 2011;196(3):723–9.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Batohi B, Fang C, Michell MJ, et al. An audit of mammographic screen detected lesions of uncertain malignant potential (B3) diagnosed on initial image guided needle biopsy: how has our practice changed over 10 years? Clin Radiol. 2019;74(8):653.e19-653.e25.
Kiran S, Jeong YJ, Nelson ME, et al. Are we overtreating intraductal papillomas? J Surg Res. 2018;231:387–94.
Kim S-Y, Kim E-K, Lee HS, et al. Asymptomatic benign papilloma without atypia diagnosed at ultrasonography-guided 14-gauge core needle biopsy: which subgroup can be managed by observation? Ann Surg Oncol. 2016;23(6):1860–6.
Han S-H, Kim M, Chung YR, et al. Benign intraductal papilloma without atypia on core needle biopsy has a low rate of upgrading to malignancy after excision. J Breast Cancer. 2018;21(1):80–6.
Seely JM, Verma R, Kielar A, et al. Benign papillomas of the breast diagnosed on large-gauge vacuum biopsy compared with 14 gauge core needle biopsy—do they require surgical excision? Breast J. 2017;23(2):146–53.
Nasehi L, Sturgis CD, Sharma N, et al. Breast cancer risk associated with benign intraductal papillomas initially diagnosed on core needle biopsy. Clin Breast Cancer. 2018;18(6):468–73.
Park S-Y, Ko S, Yoon CS, et al. Factors associated with disease upgrading in patients with papillary breast lesion in core-needle biopsy. Gland Surg. 2020;9(4):919–24.
Shouhed D, Amersi FF, Spurrier R, et al. Intraductal papillary lesions of the breast: clinical and pathological correlation. Am Surg. 2012;78(10):1161–5.
Tatarian T, Sokas C, Rufail M, et al. Intraductal papilloma with benign pathology on breast core biopsy: to excise or not? Ann Surg Oncol. 2016;23(8):2501–7.
Richter-Ehrenstein C, Tombokan F, Fallenberg E-M, et al. Intraductal papillomas of the breast: diagnosis and management of 151 patients. Breast. 2011;20(6):501–4.
Swapp RE, Glazebrook KN, Jones KN, et al. Management of benign intraductal solitary papilloma diagnosed on core needle biopsy. Ann Surg Oncol. 2013;20(6):1900–5.
Ahn SK, Han W, Moon H-G, et al. Management of benign papilloma without atypia diagnosed at ultrasound-guided core needle biopsy: scoring system for predicting malignancy. Eur J Surg Oncol. 2018;44(1):53–8.
Shamonki J, Chung A, Huynh KT, et al. Management of papillary lesions of the breast: can larger core needle biopsy samples identify patients who may avoid surgical excision? Ann Surg Oncol. 2013;20(13):4137–44.
Li X, Weaver O, Desouki MM, et al. Microcalcification Is an important factor in the management of breast intraductal papillomas diagnosed on core biopsy. Am J Clin Pathol. 2012;138(6):789–95.
Asirvatham JR, Jorns JM, Zhao L, et al. Outcomes of benign intraductal papillomas diagnosed on core biopsy: a review of 104 cases with subsequent excision from a single institution. Virchows Arch. 2018;473(6):679–86.
Fu C-Y, Chen T-W, Hong Z-J, et al. Papillary breast lesions diagnosed by core biopsy require complete excision. Eur J Surg Oncol. 2012;38(11):1029–35.
Chang JM, Han W, Moon WK, et al. Papillary lesions initially diagnosed at ultrasound-guided vacuum-assisted breast biopsy: rate of malignancy based on subsequent surgical excision. Ann Surg Oncol. 2011;18(9):2506–14.
Khan S, Diaz A, Archer KJ, et al. Papillary lesions of the breast: to excise or observe? Breast J. 2018;24(3):350–5.
Brennan SB, Corben A, Liberman L, et al. Papilloma diagnosed at MRI-guided vacuum-assisted breast biopsy: is surgical excision still warranted? Am J Roentgenol. 2012;199(4):W512–9.
Nakhlis F, Ahmadiyeh N, Lester S, et al. Papilloma on core biopsy: excision vs observation. Ann Surg Oncol. 2015;22(5):1479–82.
Glenn ME, Throckmorton AD, Thomison JB, Bienkowski RS. Papillomas of the breast 15 mm or smaller: 4-year experience in a community-based dedicated breast imaging clinic. Ann Surg Oncol. 2015;22(4):1133–9.
Holley SO, Appleton CM, Farria DM, et al. Pathologic outcomes of nonmalignant papillary breast lesions diagnosed at imaging-guided core needle biopsy. Radiology. 2012;265(2):379–84.
Hong YR, Song BJ, Jung SS, et al. Predictive factors for upgrading patients with benign breast papillary lesions using a core needle biopsy. J Breast Cancer. 2016;19(4):410–6.
Lu Q, Tan EY, Ho B, et al. Surgical excision of intraductal breast papilloma diagnosed on core biopsy. Anz J Surg. 2012;82(3):168–72.
Ko D, Kang E, Park SY, et al. The management strategy of benign solitary intraductal papilloma on breast core biopsy. Clin Breast Cancer. 2017;17(5):367–72.
Armes JE, Galbraith C, Gray J, Taylor K. The outcome of papillary lesions of the breast diagnosed by standard core needle biopsy within a BreastScreen Australia service. Pathology. 2017;49(3):267–70.
Chen P, Zhou D, Wang C, et al. Treatment and outcome of 341 papillary breast lesions. World J Surg. 2019;43(10):2477–82.
Wiratkapun C, Keeratitragoon T, Lertsithichai P, Chanplakorn N. Upgrading rate of papillary breast lesions diagnosed by core-needle biopsy. Diagn Interv Radiol. 2013;19(5):371–6.
Kibil W, Hodorowicz-Zaniewska D, Popiela TJ, Kulig J. Vacuum-assisted core biopsy in diagnosis and treatment of intraductal papillomas. Clin Breast Cancer. 2013;13(2):129–32.
Renshaw AA, Derhagopian RP, Tizol-Blanco DM, Gould EW. Papillomas and atypical papillomas in breast core needle biopsy specimens: risk of carcinoma in subsequent excision. Am J Clin Pathol. 2004;122(2):217–21.
Muttarak M, Lerttumnongtum P, Chaiwun B, Peh WCG. Spectrum of papillary lesions of the breast: clinical, imaging, and pathologic correlation. Am J Roentgenol. 2008;191(3):700–7.
Author information
Authors and Affiliations
Contributions
FL conceptualized and designed the study; XZ and WL performed the data acquisition and analysis; and XZ and TH interpreted the findings and drafted the initial manuscript. All authors approved the final manuscript and agree to be accountable for this work.
Corresponding author
Ethics declarations
Disclosure
Xiaoli Zhang, Wenqing Liu, Tao Hai, and Fei Li declare no potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, X., Liu, W., Hai, T. et al. Upgrade Rate and Predictive Factors for Breast Benign Intraductal Papilloma Diagnosed at Biopsy: A Meta-Analysis. Ann Surg Oncol 28, 8643–8650 (2021). https://doi.org/10.1245/s10434-021-10188-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-10188-7