Abstract
Purpose
This study aims to investigate the effect of lymph node examination on overall survival (OS) and lung cancer-specific survival (LCSS) in stage I second primary lung cancer (SPLC) patients who underwent second pulmonary resection.
Patients and Methods
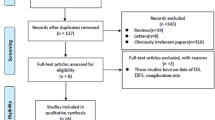
We conducted a retrospective study with the Surveillance, Epidemiology, and End Results (SEER) database to identify stage I SPLC patients who received surgery from 1998 to 2015. The Kaplan–Meier method with landmark analysis and multivariable Cox regression analysis were performed to evaluate the prognostic value of lymph node examination.
Results
A total of 842 patients from the SEER database with stage I SPLC who underwent a second surgical treatment were included. The 5-year survival rate was 54.8% for the whole cohort. Multivariable analysis revealed that the number of lymph nodes examined (LNE) was associated with better OS and LCSS in SPLC patients after 12 months postoperatively. Patients with contralateral SPLC had significantly more nodes removed than those with ipsilateral SPLC. For contralateral SPLC, more than 10 LNE was correlated with improved long-term survival outcomes. Ipsilateral SPLC patients benefited from 4 or more LNE. However, the current analysis did not show a significant survival benefit from lymph node examination within 12 months after surgery.
Conclusions
For stage I SPLC patients who received surgical treatment after initial resection, an adequate number of LNE would improve both OS and LCSS. We recommend more than 10 LNE for contralateral SPLC and at least 4 LNE for ipsilateral SPLC.




Similar content being viewed by others
References
Johnson BE. Second lung cancers in patients after treatment for an initial lung cancer. J Natl Cancer Inst. Sep 16 1998;90(18):1335–1345.
Thakur MK, Ruterbusch JJ, Schwartz AG, Gadgeel SM, Beebe-Dimmer JL, Wozniak AJ. Risk of second lung cancer in patients with previously treated lung cancer: analysis of Surveillance, Epidemiology, and End Results (SEER) data. J Thorac Oncol. 2018;13(1):46–53.
Finley DJ, Yoshizawa A, Travis W, et al. Predictors of outcomes after surgical treatment of synchronous primary lung cancers. J Thorac Oncol. 2010;5(2):197–205.
Bae MK, Byun CS, Lee CY, et al. The role of surgical treatment in second primary lung cancer. Ann Thorac Surg. 2011;92(1):256–262.
Hamaji M, Allen MS, Cassivi SD, et al. Surgical treatment of metachronous second primary lung cancer after complete resection of non-small cell lung cancer. J Thorac Cardiovasc Surg. 2013;145(3):683–690 (discussion 690-681).
Ludwig MS, Goodman M, Miller DL, Johnstone PA. Postoperative survival and the number of lymph nodes sampled during resection of node-negative non-small cell lung cancer. Chest. 2005;128(3):1545–1550.
Varlotto JM, Recht A, Nikolov M, Flickinger JC, Decamp MM. Extent of lymphadenectomy and outcome for patients with stage I nonsmall cell lung cancer. Cancer. 2009;115(4):851–858.
Krantz SB, Lutfi W, Kuchta K, Wang CH, Kim KW, Howington JA. Improved lymph node staging in early-stage lung cancer in the National Cancer Database. Ann Thorac Surg. 2017;104(6):1805–1814.
Dai J, Liu M, Yang Y, et al. Optimal lymph node examination and adjuvant chemotherapy for stage I lung cancer. J Thorac Oncol. 2019;14(7):1277–1285.
Goldstraw P, Chansky K, Crowley J, et al. The IASLC lung cancer staging project: proposals for revision of the TNM stage groupings in the forthcoming (Eighth) edition of the TNM classification for lung cancer. J Thorac Oncol. 2016;11(1):39–51.
Travis WD, Brambilla E, Nicholson AG, et al. The 2015 World Health Organization classification of lung tumors: impact of genetic, clinical and radiologic advances since the 2004 classification. J Thorac Oncol. 2015;10(9):1243–1260.
Martini N, Melamed MR. Multiple primary lung cancers. J Thorac Cardiovasc Surg. 1975;70(4):606–612.
Lee DS, LaChapelle C, Taioli E, et al. Second primary lung cancers demonstrate similar survival with wedge resection and lobectomy. Ann Thorac Surg. 2019;108(6):1724–1728.
Liang W, He J, Shen Y, et al. Impact of examined lymph node count on precise staging and long-term survival of resected non-small-cell lung cancer: a population study of the US SEER database and a Chinese multi-institutional registry. J Clin Oncol. 2017;35(11):1162–1170.
Osarogiagbon RU, Yu X. Nonexamination of lymph nodes and survival after resection of non-small cell lung cancer. Ann Thorac Surg. 2013;96(4):1178–1189.
David EA, Cooke DT, Chen Y, Nijar K, Canter RJ, Cress RD. Does lymph node count influence survival in surgically resected non-small cell lung cancer? Ann Thorac Surg. 2017;103(1):226–235.
Ou SH, Zell JA. Prognostic significance of the number of lymph nodes removed at lobectomy in stage IA non-small cell lung cancer. J Thorac Oncol. 2008;3(8):880–886.
Gulack BC, Yang CF, Speicher PJ, et al. The impact of tumor size on the association of the extent of lymph node resection and survival in clinical stage I non-small cell lung cancer. Lung Cancer (Amsterdam, Netherlands). 2015;90(3):554–560.
Allen MS, Darling GE, Pechet TT, et al. Morbidity and mortality of major pulmonary resections in patients with early-stage lung cancer: initial results of the randomized, prospective ACOSOG Z0030 trial. Ann Thorac Surg. 2006;81(3):1013–1019 (discussion 1019-1020).
Shapiro M, Mhango G, Kates M, et al. Extent of lymph node resection does not increase perioperative morbidity and mortality after surgery for stage I lung cancer in the elderly. Eur J Surg Oncol. 2012;38(6):516–522.
Harada H, Okada M, Sakamoto T, Matsuoka H, Tsubota N. Functional advantage after radical segmentectomy versus lobectomy for lung cancer. Ann Thorac Surg. 2005;80(6):2041–2045.
De Zoysa MK, Hamed D, Routledge T, Scarci M. Is limited pulmonary resection equivalent to lobectomy for surgical management of stage I non-small-cell lung cancer? Interact Cardiovasc Thorac Surg. 2012;14(6):816–820.
Zhang R, Wang G, Lin Y, et al. Extent of resection and lymph node evaluation in early stage metachronous second primary lung cancer: a population-based study. Transl Lung Cancer Res. 2020;9(1):33–44.
Acknowledgments
This study was supported by the National Natural Science Foundation of China (Grant No. 81972172), the Shanghai Municipal Health Commission (Grant No. 20174Y0111), the Shanghai Hospital Development Center (Grant No. SHDC12018122), and the Shanghai Science and Technology Committee (Grant No. 19XD1423200).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
There are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, Y., Zhang, J., Chen, L. et al. Lymph Node Examination for Stage I Second Primary Lung Cancer Patients Who Received Second Surgical Treatment. Ann Surg Oncol 28, 1810–1818 (2021). https://doi.org/10.1245/s10434-020-08975-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-020-08975-9