Abstract
Background
Postoperative changes in skeletal muscle and their influence on outcomes after esophagectomy for patients with esophageal cancer have not been fully investigated. This study aimed to confirm that postoperative skeletal muscle decrease influences long-term patient outcomes.
Methods
Data were collected from 218 patients who underwent curative esophagectomy for esophageal cancer whose data were available before and 6 months after surgery. The skeletal muscle index (SMI) was measured at the level of the L3 vertebrae, and the postoperative change in the SMI compared with preoperative values was calculated as the delta SMI.
Results
The mean SMI value was − 11.64%, and the median delta SMI value was − 11.88%. The first and third quartiles were defined as cutoffs, and 218 patients were classified as the mild-loss group (54 patients), moderate-loss group (110 patients), and severe-loss group (54 patients). The patients with a more severely reduced SMI had a worse prognosis (5-year overall survival rates: mild loss, 66.6%; moderate loss, 58.8%; and severe loss, 48.5%; p = 0.0314). This correlation between reduced SMI and prognosis also was observed for the patients with preoperative sarcopenia (p < 0.0001), but not for those without preoperative sarcopenia.
Conclusions
Postoperative reduced SMI and worse prognosis were significantly associated in esophageal cancer patients.



Similar content being viewed by others
References
Ferlay J, Soerjomataram I, Dikshit R, et al. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359–86.
Nakashima Y, Saeki H, Yukaya T, et al. Blood flow assessment with indocyanine green fluorescence angiography for pedicled omental flap on cervical esophagogastric anastomosis after esophagectomy. J Am Coll Surg. 2016;222:e67–9.
Saeki H, Nakashima Y, Hirose K, et al. “Energy-less technique” with mini-clips for recurrent laryngeal nerve lymph node dissection in prone thoracoscopic esophagectomy for esophageal cancer. Am J Surg. 2018;216:1212–4.
Nakashima Y, Saeki H, Hu Q, et al. Neoadjuvant chemotherapy versus chemoradiotherapy for patients with esophageal squamous cell carcinoma. Anticancer Res. 2018;38:6809–14.
Martin L, Lagergren P. Long-term weight change after oesophageal cancer surgery. Br J Surg. 2009;96:1308–14.
Baker M, Halliday V, Williams RN, Bowrey DJ. A systematic review of the nutritional consequences of esophagectomy. Clin Nutr. 2016;35:987–94.
Rosenberg IH. Sarcopenia: origins and clinical relevance. J Nutr. 1997;127(5 Suppl):990S–91S.
Harimoto N, Yoshizumi T, Shimokawa M, et al. Sarcopenia is a poor prognostic factor following hepatic resection in patients aged 70 years and older with hepatocellular carcinoma. Hepatol Res. 2016;46:1247–55.
Itoh S, Shirabe K, Matsumoto Y, et al. Effect of body composition on outcomes after hepatic resection for hepatocellular carcinoma. Ann Surg Oncol. 2014;21:3063–8.
Nakashima Y, Saeki H, Nakanishi R, et al. Assessment of sarcopenia as a predictor of poor outcomes after esophagectomy in elderly patients with esophageal cancer. Ann Surg. 2018;267:1100–4.
Ida S, Watanabe M, Yoshida N, et al. Sarcopenia is a predictor of postoperative respiratory complications in patients with esophageal cancer. Ann Surg Oncol. 2015;22:4432–7.
Japan Esophageal Society. Japanese classification of esophageal cancer, tenth edition: part I. Esophagus. 2009;6:1–25.
Japan Esophageal Society. Japanese classification of esophageal cancer, tenth edition: parts II and III. Esophagus. 2009;6:71–94.
Miyazaki T, Sakai M, Sohda M, et al. Prognostic significance of inflammatory and nutritional parameters in patients with esophageal cancer. Anticancer Res. 2016;36:6557–62.
Ignacio de Ulíbarri J, González-Madroño A, de Villar NGP, et al. CONUT: a tool for controlling nutritional status: first validation in a hospital population. Nutr Hosp. 20:38–45.
D’Journo XB, Ouattara M, Loundou A, et al. Prognostic impact of weight loss in 1-year survivors after transthoracic esophagectomy for cancer. Dis Esophagus. 2012;25:527–34.
Park SY, Yoon J-K, Lee SJ, Haam S, Jung J. Postoperative change of the psoas muscle area as a predictor of survival in surgically treated esophageal cancer patients. J Thorac Dis. 2017;9:355–61.
Mayanagi S, Tsubosa Y, Omae K, et al. Negative impact of skeletal muscle wasting after neoadjuvant chemotherapy followed by surgery on survival for patients with thoracic esophageal cancer. Ann Surg Oncol. 2017;24:3741–7.
Ballard-Barbash R, Friedenreich CM, Courneya KS, Siddiqi SM, McTiernan A, Alfano CM. Physical activity, biomarkers, and disease outcomes in cancer survivors: a systematic review. J Natl Cancer Inst. 2012;104:815–40.
Aoi W, Naito Y, Takagi T, et al. A novel myokine, secreted protein acidic and rich in cysteine (SPARC), suppresses colon tumorigenesis via regular exercise. Gut. 2013;62:882–9.
Ryan AM, Reynolds JV, Healy L, et al. Enteral nutrition enriched with eicosapentaenoic acid (EPA) preserves lean body mass following esophageal cancer surgery: results of a double-blinded randomized controlled trial. Ann Surg. 2009;249:355–63.
Kudou K, Saeki H, Nakashima Y, et al. Postoperative skeletal muscle loss predicts poor prognosis of adenocarcinoma of upper stomach and esophagogastric junction. World J Surg. 2019;43:1068–75.
Yamaoka Y, Fujitani K, Tsujinaka T, et al. Skeletal muscle loss after total gastrectomy, exacerbated by adjuvant chemotherapy. Gastric Cancer. 2015;18:382–9.
Okada G, Matsumoto Y, Nakamura Y, et al. Nutritional changes and factors contributing to postoperative weight recovery after esophagectomy. Esophagus. 2017;14:343–50.
Kobayashi A, Kaido T, Hamaguchi Y, et al. Impact of postoperative changes in sarcopenic factors on outcomes after hepatectomy for hepatocellular carcinoma. J Hepatobiliary Pancreat Sci. 2016;23:57–64.
Acknowledgment
This work was not supported by any grant support or funding. This work was supported in part by a Grant-in-Aid from the Ministry of Education.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
There are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
10434_2019_7850_MOESM2_ESM.tif
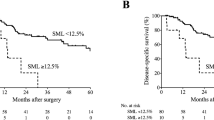
Figure S1. Kaplan–Meier DSS curves for patients with different degrees of skeletal muscle loss in the preoperative non-sarcopenia cohort (a) and preoperative sarcopenia cohort (b). Supplementary material 2 (TIFF 99 kb)
Rights and permissions
About this article
Cite this article
Nakashima, Y., Saeki, H., Hu, Q. et al. Skeletal Muscle Loss After Esophagectomy Is an Independent Risk Factor for Patients with Esophageal Cancer. Ann Surg Oncol 27, 492–498 (2020). https://doi.org/10.1245/s10434-019-07850-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-07850-6