Abstract
Background
A diagnosis of breast cancer (BC) can result in multifactorial stress. If not addressed, distress can have a negative impact on outcomes. The experience of patients with newly diagnosed BC has not been sufficiently investigated. This study characterizes distress among new patients in a multidisciplinary care (MDC) clinic. The study aimed to determine the degree of distress at presentation, to characterize the sources, and to evaluate the impact of an MDC visit.
Methods
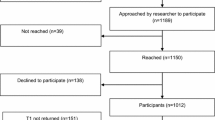
A retrospective review was performed from January 2015 to November 2017. Charts were accessed for demographics, tumor characteristics, and treatment data. Distress scores (DS) and problems as captured using the National Comprehensive Cancer Network (NCCN) Distress Thermometer were completed before evaluation and in a subgroup after an MDC visit. Predictors of severe distress (DS ≥4) were investigated using multivariable logistic regression. The paired t test was used to determine the impact of an MDC visit.
Results
The mean initial DS (n = 474) was 4.98. The top four sources of distress were worry, anxiety, fears, and sadness. Age younger than 65 years was significantly associated with a higher DS at presentation (p < 0.003). Among the patients queried before and after MDC (n = 137), a significant reduction in distress was identified (5.58–2.94; p < 0.0005).
Conclusions
Severe distress was found in 66 % of the patients with a recent diagnosis of BC, with younger age related to higher distress scores at presentation. Emotional stressors were the predominant factors accounting for distress. A same-day MDC visit was associated with a significant reduction in DS. These data indicate the importance and feasibility of proactively screening patients. Our research lends support to the value of multidisciplinary evaluation in this setting.
Similar content being viewed by others
References
SEER Cancer Stat Facts: Female Breast Cancer. National Cancer Institute, Bethesda MD, 2019.
Choi EK, Kim IR, Chang O, et al. Impact of chemotherapy-induced alopecia distress on body image, psychosocial well-being, and depression in breast cancer patients. Psychooncology. 2014;23:1103–10.
Antoni MH, Wimberly SR, Lechner SC, et al. Reduction of cancer-specific thought intrusions and anxiety symptoms with a stress management intervention among women undergoing treatment for breast cancer. Am J Psychiatry. 2006;163:1791–7.
Wenzel JA, Griffith KA, Shang J, et al. Impact of a home-based walking intervention on outcomes of sleep quality, emotional distress, and fatigue in patients undergoing treatment for solid tumors. Oncologist. 2013;18:476–84.
Hegel MT, Collins ED, Kearing S, et al. Sensitivity and specificity of the Distress Thermometer for depression in newly diagnosed breast cancer patients. Psychooncology. 2008;17:556–60.
Golden-Kreutz DM, Thornton LM, Wells-Di Gregorio S, et al. Traumatic stress, perceived global stress, and life events: prospectively predicting quality of life in breast cancer patients. Health Psychol. 2005;24:288–96.
Hartl K, Engel J, Herschbach P, et al. Personality traits and psychosocial stress: quality of life over 2 years following breast cancer diagnosis and psychological impact factors. Psychooncology. 2010;19:160–9.
Palesh O, Butler LD, Koopman C, et al. Stress history and breast cancer recurrence. J Psychosom Res. 2007;63:233–9.
Lazenby M, Ercolano E, Grant M, et al. Supporting commission on cancer-mandated psychosocial distress screening with implementation strategies. J Oncol Pract. 2015;11:e413–20.
Zebrack B, Kayser K, Bybee D, et al. A practice-based evaluation of distress screening protocol adherence and medical service utilization. J Natl Compr Cancer Netw. 2017;15:903–12.
Jacobsen PB, Donovan KA, Trask PC, et al. Screening for psychologic distress in ambulatory cancer patients. Cancer. 2005;103:1494–502.
Mitchell AJ. Short screening tools for cancer-related distress: a review and diagnostic validity meta-analysis. J Natl Compr Cancer Netw. 2010; 8: 487–494.
Thalen-Lindstrom A, Larsson G, Hellbom M, et al. Validation of the Distress Thermometer in a Swedish population of oncology patients; accuracy of changes during six months. Eur J Oncol Nurs. 2013;17:625–31.
National Comprehensive Network Cancer Network. NCCN clinical practice guidelines in oncology: distress management V.2. 2013. www.nccn.org. Accessed 5 Apr 2019.
Stafford L, Judd F, Gibson P, et al. Screening for depression and anxiety in women with breast and gynaecologic cancer: course and prevalence of morbidity over 12 months. Psychooncology. 2013;22:2071–8.
Chiang AC, Buia Amport S, Corjulo D, et al. Incorporating patient-reported outcomes to improve emotional distress screening and assessment in an ambulatory oncology clinic. J Oncol Pract. 2015;11:219–22.
Acquati C, Kayser K. Predictors of psychological distress among cancer patients receiving care at a safety-net institution: the role of younger age and psychosocial problems. Support Care Cancer. 2017;25:2305–12.
Jorgensen L, Laursen BS, Garne JP, et al. Prevalence and predictors of distress in women taking part in surgical continuity of care for breast cancer: a cohort study. Eur J Oncol Nurs. 2016;22:30–6.
Agarwal J, Powers K, Pappas L, et al. Correlates of elevated Distress Thermometer scores in breast cancer patients. Support Care Cancer. 2013;21:2125–36.
McFarland DC, Shaffer KM, Polizzi H, et al. Prevalence of physical problems detected by the Distress Thermometer and problem list in patients with myeloproliferative disorders. J Natl Compr Cancer Netw. 2017;15:1503–8.
Mertz BG, Bistrup PE, Johansen C, Dalton SO, Deltour I, Kehlet H. Psychological distress among women with newly diagnosed breast cancer. Eur J Oncol Nurs. 2012;16:439–43.
Avis NE, Crawford S, Manuel J. Psychosocial problems among younger women with breast cancer. Psychooncology. 2004;13:295–308.
Castellon S, Ganz PA. Neuropsychological studies in breast cancer: in search of chemobrain. Breast Cancer Res Treat. 2009;116:125–7.
Robbeson C, Hugenholtz-Wamsteker W, Meeus M, et al. Screening of physical distress in breast cancer survivors: concurrent validity of the Distress Thermometer and problem list. Eur J Cancer Care Engl. 2019; 28:e12880.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
There are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ciambella, C.C., Taneja, C., Dizon, D.S. et al. Distress: Characterizing What Causes the Thermometer to Shift in Patients with Newly Diagnosed Breast Cancer Attending a Multidisciplinary Clinic. Ann Surg Oncol 26, 3204–3209 (2019). https://doi.org/10.1245/s10434-019-07544-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-07544-z