Abstract
Background
An estimated 5–10% of breast and ovarian cancers are due to hereditary causes such as hereditary breast and ovarian cancer (HBOC) syndrome. Medicare, the third-party payer that covers 44 million patients in the United States, has implemented a set of clinical criteria to determine coverage for the testing of the BRCA1 and BRCA2 genes. These criteria, developed to identify carriers of BRCA1/2 variants, have not been evaluated in the panel testing era. This study investigated a series of Medicare patients undergoing genetic testing for HBOC to determine the efficacy of genetic testing criteria in identifying patients with hereditary risk.
Methods
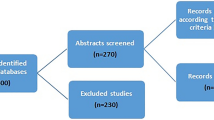
This study retrospectively examined de-identified data from a consecutive series of Medicare patients undergoing genetic testing based on personal and family history of breast and gynecologic cancer. Ordering clinicians indicated whether patients did or did not meet established criteria for BRCA1/2 genetic testing. The genetic test results were compared between the group that met the criteria and the group that did not. Patients in families with known pathogenic (P) or likely pathogenic (LP) variants were excluded from the primary analysis.
Results
Among 4196 unique Medicare patients, the rate of P/LP variants for the patients who met the criteria for genetic testing was 10.5%, and for those who did not, the rate was 9% (p = 0.26).
Conclusions
The results of this study indicate that a substantial number of Medicare patients with clinically actionable genetic variants are being missed by current testing criteria and suggest the need for significant expansion and simplification of the testing criteria for HBOC.

Similar content being viewed by others
References
American Cancer Society: Breast Cancer Facts & Figures 2017–2018. American Cancer Society, Atlanta, GA. 2017. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/breast-cancer-facts-and-figures/breast-cancer-facts-and-figures-2017-2018.pdf. Accessed April 2018.
Norquist BM, Harrell MI, Brady MF, et al. Inherited mutations in women with ovarian carcinoma. JAMA Oncol. 2016;2(4):482–90.
Drohan B, Roche CA, Cusack Jr JC, Hughes KS. Hereditary breast and ovarian cancer and other hereditary syndromes: using technology to identify carriers. Ann Surg Oncol. 2012;19(6):1732–7.
Levy-Lahad E, Lahad A, King M-C. Precision medicine meets public health: population screening for BRCA1 and BRCA2. J Natl Cancer Inst. 2015;107(1):420.
Childers CP, Childers KK, Maggard-Gibbons M, Macinko J. National estimates of genetic testing in women with a history of breast or ovarian cancer. J Clin Oncol. 2017;35(34):3800–6.
Guo F, Hirth JM, Lin Y-L, et al. Use of BRCA mutation test in the US, 2004–2014. Am J Prev Med. 2017;52(6):702–9.
Evans DGR, Ingham SL, Baildam A, et al. Contralateral mastectomy improves survival in women with BRCA1/2-associated breast cancer. Breast Cancer Res Treat. 2013;140(1):135–42.
Robson M, Im S-A, Senkus E, et al. Olaparib for metastatic breast cancer in patients with a germline BRCA mutation. N Engl J Med. 2017;377(6):523–33.
Local coverage determination: MolDx BRCA1 and BRCA2 genetic testing. Noridian Medicare. https://med.noridianmedicare.com/documents/10546/6990981/MolDX+BRCA1+and+BRCA2+Genetic+Testing+LCD/220c55c8-8bc8-4319-80a1-66c4a1d51dd8. Accessed April 2018.
O’Leary E, Iacoboni D, Holle J, et al. Expanded gene panel use for women with breast cancer: identification and intervention beyond breast cancer risk. Ann Surg Oncol. 2017;24(10):3060–6.
Lincoln SE, Kobayashi Y, Anderson MJ, et al. A systematic comparison of traditional and multigene panel testing for hereditary breast and ovarian cancer genes in more than 1000 patients. J Mol Diagn. 2015;17(5):533–44.
Nykamp K, Anderson M, Powers M, et al. Sherloc: a comprehensive refinement of the ACMG–AMP variant classification criteria. Genet Med. 2017;19:1105.
Grindedal EM, Heramb C, Karsrud I, et al. Current guidelines for BRCA testing of breast cancer patients are insufficient to detect all mutation carriers. BMC Cancer. 2017;17(1):438.
Tung N, Lin NU, Kidd J, et al. Frequency of germline mutations in 25 cancer-susceptibility genes in a sequential series of patients with breast cancer. J Clin Oncol. 2016;34(13):1460–8.
Tung N, Battelli C, Allen B, et al. Frequency of mutations in individuals with breast cancer referred for BRCA1 and BRCA2 testing using next-generation sequencing with a 25-gene panel. Cancer. 2015;121(1):25–33.
Desmond A, Kurian AW, Gabree M, et al. Clinical actionability of multigene panel testing for hereditary breast and ovarian cancer risk assessment. JAMA Oncol. 2015;1(7):943–51.
Hauke J, Horvath J, Groß E, et al. Gene panel testing of 5589 BRCA1/2-negative index patients with breast cancer in a routine diagnostic setting: results of the German Consortium for Hereditary Breast and Ovarian Cancer. Cancer Med. 2018;7(4):1349–58.
CHEK2 Breast Cancer Case-Control Consortium. CHEK2*1100delC and susceptibility to breast cancer: a collaborative analysis involving 10,860 breast cancer cases and 9065 controls from 10 studies. Am J Hum Genet. 2004;74(6):1175–82.
Chen S, Parmigiani G. Meta-analysis of BRCA1 and BRCA2 penetrance. J Clin Oncol. 2007;25(11):1329–33.
Acknowledgment
We appreciate the manuscript editing assistance of Nancy Jacoby and graphic design assistance of Carole Leung and Alla Zarifyan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yang, S., Axilbund, J.E., O’Leary, E. et al. Underdiagnosis of Hereditary Breast and Ovarian Cancer in Medicare Patients: Genetic Testing Criteria Miss the Mark. Ann Surg Oncol 25, 2925–2931 (2018). https://doi.org/10.1245/s10434-018-6621-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-018-6621-4