Abstract
Background
Wire-localized excision of nonpalpable breast cancer is imprecise, resulting in positive margins 25–30% of the time.
Methods
Patients underwent preoperative supine magnetic resonance imaging (MRI). A radiologist outlined the tumor edges on consecutive images, creating a three-dimensional (3D) view of its location. Using 3D printing, a bra-like plastic form (the Breast Cancer Locator [BCL]) was fabricated, with features that allowed a surgeon to (1) mark the edges of the tumor on the breast surface; (2) inject blue dye into the breast 1 cm from the tumor edges; and (3) place a wire in the tumor at the time of surgery.
Results
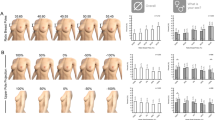
Nineteen patients with palpable cancers underwent partial mastectomy after placement of surgical cues using patient-specific BCLs. The cues were in place in <5 min and no adverse events occurred. The BCL accurately localized 18/19 cancers. In the 18 accurately localized cases, all 68 blue-dye injections were outside of the tumor edges. Median distance from the blue-dye center to the pathologic tumor edge was 1.4 cm, while distance from the blue dye to the tumor edge was <5 mm in 4% of injections, 0.5–2.0 cm in 72% of injections, and >2 cm in 24% of injections. Median distance from the tumor center to the BCL-localized wire and to the clip placed at the time of diagnosis was similar (0.49 vs. 0.73 cm) on specimen mammograms.
Conclusions
Information on breast cancer location and shape derived from a supine MRI can be transferred safely and accurately to patients in the operating room using a 3D-printed form.



Similar content being viewed by others
References
Barth R, Gibson G, Carney P, Mott LA, Becher RD, Poplack SP, et al. Detection of breast cancer on screening mammography allows patients to be treated with less toxic therapy. AJR Am J Roentgenol. 2005;184:324–9.
Wong J, Kaelin C, Troyan S, Gadd MA, Gelman R, Lester SC, et al. Prospective study of wide excision alone for DCIS of the breast. J Clin Oncol. 2006;24:1031–6.
Lovrics P, Goldsmith C, Hodgson N, McCready D, Gohla G, Boylan C, et al. A multicentered, randomized controlled trial comparing radioguided seed localization to standard wire localization for nonpalpable, invasive and in situ breast carcinomas. Ann Surg Oncol. 2011;18:3407–14.
Schnabel F, Boolbol S, Gittleman M, Karni T, Tafra L, Feldman S, et al. A randomized prospective study of lumpectomy margiin assessment with use of MarginProbe in patients with nonpalpable breast malignancies. Ann Surg Oncol. 2014;21:1589–95.
Chapgar A, Killelea B, Tsangaris T, Butler M, Stavris K, Li F, et al. A randomized controlled trial of cavity shave margins in breast cancer. N Engl J Med. 2015;373:503–10.
Heil J, Breitkruz K, Golatta M, Czink E, Dahlkamp J, Rom J, et al. Do reexcisions impair aesthetic outcome in breats conservation surgery? Exploratory analysis of a prospective study cohort. Ann Surg Oncol. 2012;19:541–7.
Abe S, Hill J, Han Y, Walsh K, Symanowski JT, Hadzikadic‐Gusic L, et al. Margin re-excision and local recurrence in invasive breast cancer. J Surg Oncol. 2015;112:443–8.
Berg WA, Gutierrez L, NessAiver MS, Carter WB, Bhargavan M, Lewis RS, et al. Diagnostic accuracy of mammography, clinical examination, US, and MR imaging in preoperative assessment of breast cancer. Radiology. 2004;233:830–49.
Manell J, Morris E, Dershaw D, Abramson AF, Brogi E, Liberman L, et al. Determination of the presence and extent of pure ductal carcinoma in situ by mammography and MRI. Breast J. 2005;11:382–90.
Hwang E, Kinkel K, Esserman L, Lu Y, Weidner N, Hylton NM, et al. MRI in patients diagnosed with DCIS: value in the diagnosis of residual disease, occult invasion and multicentricity. Ann Surg Oncol. 2003;10:381–8.
Kristoffersen Wiberg M, Aspelin P, Sylvan M, Bone B. Comparison of lesion size estimated by dynamic MR imaging, mammography and histopathology in breast neoplasms. Eur Radiol. 2003;13:1207–12.
Boetes C, Mus R, Holland R, Barentsz JO, Strijk SP, Wobbes T, et al. Breast tumors: comparative accuracy of MR imaging relative to mammography and US for demonstrating extent. Radiology. 1995;197:743–7.
Davis P, Staiger M, Harris K, Ganott MA, Klementaviciene J, McCarty KS, et al. Breast cancer measurements with MRI, ultrasonography and mammography. Breast Cancer Res. 1996;37:1–9.
Turnbull L, Brown S, Harvey I, Olivier C, Drew P, Napp V, et al. Comparative effectiveness of MRI in breast cancer (COMICE) trial: a randomised controlled trial. Lancet. 2010;375:563–71.
Sakakibara M, Nagashima T, Sangai T, Nakamura R, Fujimoto H, Arai M, et al. Breast-conserving surgery using projection and reproduction techniques of surgical-position breast MRI in patients with ductal carcinoma in situ of the breast. J Am Coll Surg. 2008;207:62–8.
Sakakibara M, Yokomizu J, Shima N, Kazama T, Nakamura R, Fujimoto R, et al. MRI guided quadrantectomy in patients with DCIS detected pre-operatively by mammographic calcifications. J Am Coll Surg. 2014;219:295–302.
Pallone M, Poplack S, Avutu H, Paulsen KD, Barth RJ. Supine breast MRI and 3D optical scanning: a novel approach to improve tumor localization for breast conserving surgery. Ann Surg Oncol. 2014;21:2203–08.
Gibson G, Lesnikoski B, Yoo J, Mott LA, Cady B, Barth RJ, et al. A comparison of ink directed and traditional whole cavity re-excision for breast lumpectomy specimens with positive margins. Ann Surg Oncol. 2001;8:693–704.
Krekel N, Haloua M, Lopes Cardozo A, de Wit RH, Bosch AM, de widt-Levert LM, et al. Intra-op US guidance for palpable breast cancer excision (COBALT trial): a multicenter randomized controlled trial. Lancet Oncol. 2103; 14: 448–54.
Moore M, Whitney L, Cerilli L, Imbrie JZ, Bunch M, Simpson VB, et al. Intra-operative US is associated with clear lumpectomy margins for palpable intraductal breast cancer. Ann Surg. 2001;233:761–8.
Disclosure
Drs. Barth, Krishnaswamy and Paulsen have ownership interest in CairnSurgical LLC. This work was supported by National Institutes of Health/National Cancer Institute (NIH/NCI) Grant R43 CA210810 to CairnSurgical LLC, and a Synergy Clinician Entrepreneur Fellowship to Richard J. Barth. Timothy B. Rooney, Wendy A. Wells, Elizabeth Rizzo, Christina V. Angeles, Jonathan D. Marotti, Rebecca A. Zuurbier, and Candice C. Black have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Barth, R.J., Krishnaswamy, V., Paulsen, K.D. et al. A Patient-Specific 3D-Printed Form Accurately Transfers Supine MRI-Derived Tumor Localization Information to Guide Breast-Conserving Surgery. Ann Surg Oncol 24, 2950–2956 (2017). https://doi.org/10.1245/s10434-017-5979-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-5979-z