Abstract
Purpose
This study aimed to examine the differential impact of body mass index and the feature of metabolic syndrome (MetS; obesity, hypertension, diabetes mellitus, and dyslipidemia) on biochemical recurrence (BCR) following radical prostatectomy (RP) treatment for prostate cancer using different surgical procedures.
Methods
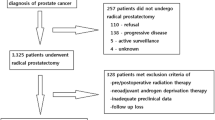
This study included 283 Japanese patients with clinically localized prostate cancer who were treated with RP between 2008 and 2012. The prognostic significance of overweight and the feature of MetS were analyzed according to surgical procedures.
Results
BCR occurred in 68/283 (24.0%) men. Overweight and the feature of MetS were predictors of BCR in patients who had undergone open RP (ORP), but not in those treated with laparoscopic surgery. Multivariate analyses incorporating preoperative and postoperative risk factors revealed that overweight and the feature of MetS were independent BCR risk factors when treated with ORP.
Conclusions
In Japanese men, overweight and the feature of MetS were associated with worse outcomes following RP, particularly ORP, compared with those following laparoscopic surgery. These results suggest that laparoscopic surgery can overcome the surgical challenges associated with abdominal obesity.


Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015;65(1):5–29.
Faria EF, Chapin BF, Muller RL, Machado RD, Reis RB, Matin SF. Radical prostatectomy for locally advanced prostate cancer: current status. Urology. 2015;86(1):10–5.
Pound CR, Partin AW, Eisenberger MA, Chan DW, Pearson JD, Walsh PC. Natural history of progression after PSA elevation following radical prostatectomy. JAMA. 1999;281(17):1591–7.
Simmons MN, Stephenson AJ, Klein EA. Natural history of biochemical recurrence after radical prostatectomy: risk assessment for secondary therapy. Eur Urol. 2007;51(5):1175–84.
Han M, Partin AW, Zahurak M, Piantadosi S, Epstein JI, Walsh PC. Biochemical (prostate specific antigen) recurrence probability following radical prostatectomy for clinically localized prostate cancer. J Urol. 2003;169(2):517–23.
Hsing AW, Tsao L, Devesa SS. International trends and patterns of prostate cancer incidence and mortality. Int J Cancer. 2000;85(1):60–7.
Cleeman JI. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA. 2001;285:2486–97.
Mozumdar A, Liguori G. Persistent increase of prevalence of metabolic syndrome among U.S. adults: NHANES III to NHANES 1999–2006. Diabetes Care. 2011;34(1):216–9.
Arai H, Yamamoto A, Matsuzawa Y, Saito Y, Yamada N, Oikawa S, et al. Prevalence of metabolic syndrome in the general Japanese population in 2000. J Atheroscler Thromb. 2006;13(4):202–8.
Rhee H, Vela I, Chung E. Metabolic syndrome and prostate cancer: a review of complex interplay amongst various endocrine factors in the pathophysiology and progression of prostate cancer. Horm Cancer. 2016;7(2):75–83.
Laukkanen JA, Laaksonen DE, Niskanen L, Pukkala E, Hakkarainen A, Salonen JT. Metabolic syndrome and the risk of prostate cancer in Finnish men: a population-based study. Cancer Epidemiol Biomark Prev. 2004;13(10):1646–50.
Castillejos-Molina R, Rodríguez-Covarrubias F, Sotomayor M, Gómez-Alvarado MO, Villalobos-Gollás M, Gabilondo F, et al. Impact of metabolic syndrome on biochemical recurrence of prostate cancer after radical prostatectomy. Urol Int. 2011;87(3):270–5.
Häggström C, Stocks T, Ulmert D, Bjørge T, Ulmer H, Hallmans G, et al. Prospective study on metabolic factors and risk of prostate cancer. Cancer. 2012;118(24):6199–206.
Shiota M, Yokomizo A, Takeuchi A, Imada K, Kiyoshima K, Inokuchi J, et al. The feature of metabolic syndrome is a risk factor for biochemical recurrence after radical prostatectomy. J Surg Oncol. 2014;110(4):476–81.
Post JM, Beebe-Dimmer JL, Morgenstern H, Neslund-Dudas C, Bock CH, Nock N, et al. The metabolic syndrome and biochemical recurrence following radical prostatectomy. Prostate Cancer. 2011;2011:245642.
Jaggers JR, Sui X, Hooker SP, LaMonte MJ, Matthews CE, Hand GA, et al. Metabolic syndrome and risk of cancer mortality in men. Eur J Cancer. 2009;45(10):1831–8.
Martin RM, Vatten L, Gunnell D, Romundstad P, Nilsen TI. Components of the metabolic syndrome and risk of prostate cancer: the HUNT 2 cohort, Norway. Cancer Causes Control. 2009;20(7):1181–92.
D’Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA, et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA. 1998;280(11):969–74.
Naito S, Kuroiwa K, Kinukawa N, Goto K, Koga H, Ogawa O, et al. Validation of Partin tables and development of a preoperative nomogram for Japanese patients with clinically localized prostate cancer using 2005 International Society of Urological Pathology consensus on Gleason grading: data from the Clinicopathological Research Group for Localized Prostate Cancer. J Urol. 2008;180(3):904–9.
Freedland SJ, Grubb KA, Yiu SK, Humphreys EB, Nielsen ME, Mangold LA, et al. Obesity and risk of biochemical progression following radical prostatectomy at a tertiary care referral center. J Urol. 2005;174(3):919–22.
Komaru A, Kamiya N, Suzuki H, Endo T, Takano M, Yano M, et al. Implications of body mass index in Japanese patients with prostate cancer who had undergone radical prostatectomy. Jpn J Clin Oncol. 2010;40(4):353–9.
Cao Y, Ma J. Body mass index, prostate cancer-specific mortality, and biochemical recurrence: a systematic review and meta-analysis. Cancer Prev Res. 2011;4(4):486–501.
Amling CL, Riffenburgh RH, Sun L, Moul JW, Lance RS, Kusuda L, et al. Pathologic variables and recurrence rates as related to obesity and race in men with prostate cancer undergoing radical prostatectomy. J Clin Oncol. 2004;22(3):439–45.
Kheterpal E, Sammon JD, Diaz M, Bhandari A, Trinh QD, Pokala N, et al. Effect of metabolic syndrome on pathologic features of prostate cancer. Urol Oncol. 2013;31(7):1054–9.
Freedland SJ, Grubb KA, Yiu SK, Nielsen ME, Mangold LA, Isaacs WB, et al. Obesity and capsular incision at the time of open retropubic radical prostatectomy. J Urol. 2005;174(5):1798–801.
Park SW, Readal N, Jeong BC, Humphreys EB, Epstein JI, Partin AW, et al. Risk factors for intraprostatic incision into malignant glands at radical prostatectomy. Eur Urol. 2015;68(2):311–6.
Freedland SJ, Aronson WJ, Kane CJ, Presti JC Jr, Amling CL, Elashoff D, et al. Impact of obesity on biochemical control after radical prostatectomy for clinically localized prostate cancer: a report by the Shared Equal Access Regional Cancer Hospital database study group. J Clin Oncol. 2004;22(3):446–53.
Freedland SJ, Bañez LL, Sun LL, Fitzsimons NJ, Moul JW. Obese men have higher-grade and larger tumors: an analysis of the duke prostate center database. Prostate Cancer Prostatic Dis. 2009;12(3):259–63.
Jayachandran J, Aronson WJ, Terris MK, Presti JC Jr, Amling CL, Kane CJ, et al. Obesity and positive surgical margins by anatomic location after radical prostatectomy: results from the Shared Equal Access Regional Cancer Hospital database. BJU Int. 2008;102(8):964–8.
Moskovic DJ, Lavery HJ, Rehman J, Nabizada-Pace F, Brajtbord J, Samadi DB. High body mass index does not affect outcomes following robotic assisted laparoscopic prostatectomy. Can J Urol. 2010;17(4):5291–8.
Sundi D, Reese AC, Mettee LZ, Trock BJ, Pavlovich CP. Laparoscopic and robotic radical prostatectomy outcomes in obese and extremely obese men. Urology. 2013;82(3):600–5.
Després JP, Lemieux I. Abdominal obesity and metabolic syndrome. Nature. 2006;444(7121):881–7.
Froehner M, Litz R, Manseck A, Hakenberg OW, Leike S, Albrecht DM, et al. Relationship of comorbidity, age and perioperative complications in patients undergoing radical prostatectomy. Urol Int. 2001;67(4):283–8.
Kamerer A, Basler J, Thompson I. Novel technique of Vest suture vesicourethral anastomosis in morbidly obese patient undergoing radical retropubic prostatectomy. J Urol. 2003;170(1):174.
Berryhill R Jr, Jhaveri J, Yadav R, Leung R, Rao S, El-Hakim A, et al. Robotic prostatectomy: a review of outcomes compared with laparoscopic and open approaches. Urology. 2008;72(1):15–23.
Brown JA, Rodin DM, Lee B, Dahl DM. Laparoscopic radical prostatectomy and body mass index: an assessment of 151 sequential cases. J Urol. 2005;173(2):442–5.
Mikhail AA, Stockton BR, Orvieto MA, Chien GW, Gong EM, Zorn KC, et al. Robotic-assisted laparoscopic prostatectomy in overweight and obese patients. Urology. 2006;67(4):774–9.
Herman MP, Raman JD, Dong S, Samadi D, Scherr DS. Increasing body mass index negatively impacts outcomes following robotic radical prostatectomy. JSLS. 2007;11(4):438–42.
Boorjian SA, Crispen PL, Carlson RE, Rangel LJ, Karnes RJ, Frank I, et al. Impact of obesity on clinicopathologic outcomes after robot-assisted laparoscopic prostatectomy. J Endourol. 2008;22(7):1471–6.
Wiltz AL, Shikanov S, Eggener SE, Katz MH, Thong AE, Steinberg GD, et al. Robotic radical prostatectomy in overweight and obese patients: oncological and validated-functional outcomes. Urology. 2009;73(2):316–22.
Zilberman DE, Tsivian M, Yong D, Ferrandino MN, Albala DM. Does body mass index have an impact on the rate and location of positive surgical margins following robot assisted radical prostatectomy? Urol Oncol. 2012;30(6):790–3.
Lloyd JC, Bañez LL, Aronson WJ, Terris MK, Presti JC Jr, Amling CL, et al. Estimated blood loss as a predictor of PSA recurrence after radical prostatectomy: results from the SEARCH database. BJU Int. 2010;105(3):347–51.
Kang M, Jeong CW, Ku JH, Kwak C, Kim HH. Hypertriglyceridemia is a potential preoperative predictor for biochemical recurrence after radical prostatectomy. PLoS ONE. 2015;10(3):e0122438.
Pettersson A, Lis RT, Meisner A, Flavin R, Stack EC, Fiorentino M, et al. Modification of the association between obesity and lethal prostate cancer by TMPRSS2:ERG. J Natl Cancer Inst. 2013;105(24):1881–90.
Acknowledgement
The authors would like to thank the Edanz Group Japan for editorial assistance.
Funding
This work was supported by a Research Promotion Grant from the Daiwa Securities Health Foundation, Japan, and a Research Promotion Grant from the Smoking Research Foundation, Japan.
Disclosure
Masaki Shiota, Ario Takeuchi, Masaaki Sugimoto, Eiji Kashiwagi, Takashi Dejima, Keijiro Kiyoshima, Junichi Inokuchi, Katsunori Tatsugami, Akira Yokomizo, and Masatoshi Eto declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shiota, M., Takeuchi, A., Sugimoto, M. et al. The Differential Impact of Body Mass Index and the Feature of Metabolic Syndrome on Oncological Outcomes Following Different Surgical Procedures in Japanese Men with Prostate Cancer. Ann Surg Oncol 24, 1443–1450 (2017). https://doi.org/10.1245/s10434-016-5705-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5705-2