Abstract
Background
Although current guidelines suggest that 16 or more lymph nodes (LNs) are required for the appropriate staging of gastric cancer, the effect that the minimum number of examined LNs (eLNs) in the different types of gastrectomy has on survival remains unclear.
Methods
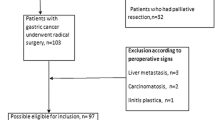
This study retrospectively analyzed 2662 patients who underwent curative gastrectomy with D2 lymphadenectomy for gastric cancer at Fujian Medical University Union Hospital from January 2000 to December 2010 and randomly divided them into development (70 %, n = 1863) and validation (30 %, n = 799) data sets. An additional external validation was performed using the data set (n = 285) collected during the same period from the Sun Yat-sen University Cancer Center in Guangzhou, China. A hypothetical tumor-node-metastasis (TNM) classification (hTNM) was proposed based on eLNs and survival.
Results
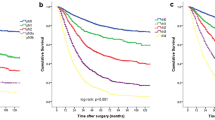
The mean numbers of nodes removed during radical distal and total gastrectomy were respectively 26 ± 9.6 and 29 ± 10.7 (p < 0.01). The optimal LN-count thresholds were determined to be 16 for patients who underwent curative distal gastrectomy and 21 for patients who underwent total gastrectomy. The hTNM staging system had higher linear trend and likelihood ratio χ 2 scores and lower Akaike information criterion (AIC) values than the seventh American Joint Committee on Cancer (AJCC) TNM classification. Thus, the hTNM staging system exhibited superior prognostic stratification. Similar results were found in the two validation data sets.
Conclusion
A harvest of at least 21 LNs may represent a superior threshold for radical total gastrectomy (RTG) and could yield a better prognosis. For patients undergoing RTG, the hTNM staging system may predict survival more accurately and discriminatively. However, a validation from a Western institution is warranted.


Similar content being viewed by others
References
Jemal A, Bray F, Center MM, et al. Global cancer statistics, CA Cancer J Clin. 2011;61:134.
Morgan JW, Ji L, Friedman G, et al. The role of the cancer center when using lymph node count as a quality measure for gastric cancer surgery. JAMA Surg. 2015;150:37–43.
Deutsch GB, O’Connor V, Sim M-S, et al. Incorporating surgical quality into the AJCC 7th edition improves staging accuracy in gastric cancer. Ann Surg Oncol. 2015;22:11–6.
Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A (eds). AJCC cancer staging manual. 7th ed. Springer, New York, 2010.
Lee HK, Yang HK, Kim WH, et al. Influence of the number of lymph nodes examined on staging of gastric cancer. Br J Surg. 2001;88:1408–12.
Ichikura T, Ogawa T, Chochi K, et al. Minimum number of lymph nodes that should be examined for the International Union Against Cancer/American Joint Committee on Cancer TNM classification of gastric carcinoma. World J Surg. 2003;27:330–3.
Baiocchi GL, Tiberio GA, Minicozzi AM, et al. A multicentric Western analysis of prognostic factors in advanced, node-negative gastric cancer patients. Ann Surg. 2010;252:70–3.
Smith DD, Schwarz RR, Schwarz RE. Impact of total lymph node count on staging and survival after gastrectomy for gastric cancer: data form a large US-population database. J Clin Oncol. 2005;23:7114–24.
Bouvier A-M, Haas O, Piard F, et al. How many nodes must be examined to accurately stage gastric carcinomas? Results from a population-based study. Cancer. 2002;94:2862–6.
Lin JX, Huang CM, Zheng CH, et al. Evaluation of laparoscopic total gastrectomy for advanced gastric cancer: results of a comparison with laparoscopic distal gastrectomy. Surg Endosc. 2016;30:1988–98.
Chen H-N, Chen X-Z, Zhang W-H, et al. Necessity of harvesting at least 25 lymph nodes in patients with stage N2–N3 resectable gastric cancer: a 10-year, single-institution cohort study. Medicine. 2015;94:e620.
Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2010 (ver. 3). Gastric Cancer. 2011;14:113–23.
Sobin LH, Gospodarowicz MK, Wittekind C, et al. TNM classification of malignant tumours. 7th ed. Wiley, Chichester, NJ, 2010.
Kang M, Jeong CW, Kwak C, et al. The prognostic significance of the early postoperative neutrophil-to-lymphocyte ratio in patients with urothelial carcinoma of the bladder undergoing radical cystectomy. Ann Surg Oncol. 2015. DOI 10.1245/s10434-015-4708-8.
Hsu PK, Wu YC, Chou TY, et al. Comparison of the 6th and 7th editions of the American Joint Committee on Cancer tumor-node-metastasis staging system in patients with resected esophageal carcinoma. Ann Thorac Surg. 2010;89:1024–31.
Gholami S, Janson L, Worhunsky DJ, et al. Number of lymph nodes removed and survival after gastric cancer resection: an analysis from the US gastric cancer collaborative. J Am Coll Surg. 2015;221:291–9.
Schwarz RE I, Smith DD, et al. Clinical impact of lymphadenectomy extent in resectable gastric cancer of advanced stage. Ann Surg Oncol. 2006;14:317–8.
Xu D, Huang Y, Geng Q, et al. Effect of lymph node number on survival of patients with lymph node-negative gastric cancer according to the 7th edition UICC TNM system. PloS One. 2012;7:e38681.
Siewert JR, Böttcher K, Stein HJ, Roder JD. Relevant prognostic factors in gastric cancer: ten-year results of the German Gastric Cancer Study. Ann Surg. 1998;228:449–61.
Bouvier A-M, Haas O, Piard F, et al. How many nodes must be examined to accurately stage gastric carcinomas? Results from a population-based study. Cancer. 2002,94:2862–6.
Datta J, Lewis RS Jr, Mamtani R, et al. Implications of inadequate lymph node staging in resectable gastric cancer a contemporary analysis using the National Cancer Data Base. Cancer. 2014;120:2855–65.
Hundahl SA, Macdonald JS, Benedetti J, et al. Surgical treatment variation in a prospective, randomized trial of chemoradiotherapy in gastric cancer: the effect of undertreatment. Ann Surg Oncol. 2002;9:278–86.
Kong SH, Lee HJ, Ahn HS, et al. Stage migration effect on survival in gastric cancer surgery with extended lymphadenectomy: the reappraisal of positive lymph node ratio as a proper n-staging. Ann Surg. 2012;255:50–8.
Deng J, Zhang R, Zhang L, Liu Y, Hao X, Liang H. Negative node count improvement prognostic prediction of the seventh edition of the TNM classification for gastric cancer. PLoS One. 2013;8:e80082.
Kulig J, Sierzega M, Kolodziejczyk P, Popiela T, et al. Ratio of metastatic to resected lymph nodes for prediction of survival in patients with inadequately staged gastric cancer. Br J Surg. 2009;96:910–8.
Wang J, Dang P, Raut CP, et al. Comparison of a lymph node ratio-based staging system with the 7th AJCC system for gastric cancer: analysis of 18,043 patients from the SEER database. Ann Surg. 2012;255:478–85.
Kooby DA, Suriawinata A, Klimstra DS, et al. Biologic predictors of survival in node-negative gastric cancer. Ann Surg. 2003;237:828–35.
Wang X, Appleby, Zhang X, et al. Comparison of three lymph node staging schemes for predicting outcome in patients with gastric cancer. Br J Surg. 2013;100:505–14.
Smith DD, Nelson RA, Schwarz RE. A comparison of five competing lymph node staging schemes in a cohort of resectable gastric cancer patients. Ann Surg Oncol. 2014;21:875–82.
Sun Z, Wang ZN, Zhu Z, et al. Evaluation of the seventh edition of American Joint Committee on Cancer TNM staging system for gastric cancer: results from a Chinese monoinstitutional study. Ann Surg Oncol. 2012,19:1918–27.
Reim D, Loos M, Vogl F, et al. Prognostic implications of the seventh edition of the International Union Against Cancer classification for patients with gastric cancer: the Western experience of patients treated in a single-center European institution. J Clin Oncol. 2013;31:263–71.
Author information
Authors and Affiliations
Corresponding author
Additional information
Jun Lu and Wei Wang contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lu, J., Wang, W., Zheng, Ch. et al. Influence of Total Lymph Node Count on Staging and Survival After Gastrectomy for Gastric Cancer: An Analysis From a Two-Institution Database in China. Ann Surg Oncol 24, 486–493 (2017). https://doi.org/10.1245/s10434-016-5494-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5494-7