Abstract
Objectives
This study was designed to demonstrated the prognostic significance of lymphatic and vascular invasion in thoracic esophageal squamous cell carcinoma after curative surgery and establish their predictive role for lymph node metastasis and recurrence in early-stage disease.
Methods
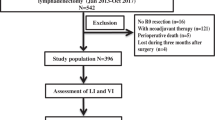
Clinical data of all patients from 2002 to 2014 who underwent curative surgery for thoracic squamous cell carcinoma were collected from a prospectively maintained database. The association of lymphatic invasion and vascular invasion with clinicopathological variables was illustrated respectively. The effect of lymphatic invasion and vascular invasion on the disease-free survival was determined by Kaplan–Meier analysis stratified by pathological stage. The predictive factors for lymph node metastasis in pT1 tumors and the predictive factors for recurrence in patients without lymph node involvement were analyzed with univariate and multivariate analyses respectively.
Results
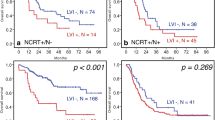
Both lymphatic invasion and vascular invasion significantly decreased stage-stratified, disease-free survival (p < 0.001). The independent predictive factors for lymph node metastasis in tumors limited in mucosa and submucosa were: submucosa invasion (p < 0.001, odds ratio [OR] 7.303), lymphatic invasion (p < 0.001, OR 5.031), and tumor differentiation (p = 0.008, OR 1.784). The independent predictive factors for decreased disease-free survival in patients with N0 disease involvement were: lymphatic invasion (p = 0.005, OR 4.326) and deeper tumor invasion (p = 0.001, OR 2.634).
Conclusions
Lymphatic invasion and vascular invasion are negative prognostic factors independent of tumor stage. Lymphatic invasion is a high-risk factor of lymph node metastasis in T1 tumors and a high-risk factor of recurrence in patients without lymph node involvement.


Similar content being viewed by others
References
Tanaka T, Matono S, Nagano T, et al. Esophagectomy with extended lymphadenectomy for submucosal esophageal cancer: long-term outcomes and prognostic factors. Ann Surg Oncol. 2011;19:750–6.
Kunisaki C, Makino H, Takagawa R, et al. Surgical outcomes in esophageal cancer patients with tumor recurrence after curative esophagectomy. J Gastrointest Surg. 2007;12:802–10.
Zafirellis K, Dolan K, Fountoulakis A, et al. Multivariable analysis of clinical, operative and pathologic features of esophageal cancer: who needs adjuvant therapy? Dis Esophagus. 2002;15:155–9.
Schoppmann SF, Jesch B, Zacherl J, Riegler MF, Friedrich J, Birner P. Lymphangiogenesis and lymphovascular invasion diminishes prognosis in esophageal cancer. Surgery. 2013;153:526–34.
Tanaka T, Matona S, Mori N, et al. T1 Squamous cell carcinoma of the esophagus: long-term outcomes and prognostic factors after esophagectomy. Ann Surg Oncol. 2014;21(3):932–8.
Bai B, Ma W, Wang K, et al. Detection of D2–40 monoclonal antibody-labeled lymphatic vessel invasion in esophageal squamous cell carcinoma and its clinicopathologic significance. Cancer Biol Med. 2013;10:81–5.
Waraich N, Rashid F, Jan A, et al. Vascular invasion is not a risk factor in oesophageal cancer recurrence. Int J Surg. 2011; 9:237–40.
Perry C, Soomro I, Kaye P, et al. Analysis of lymphatic and blood vessel invasion biomarkers in T1 esophagogastric adenocarcinomas for improved patient prognostication. Dis Esophagus. 2015;28(3):262–8.
Matsubara T, Ueda M, Abe T, et al. Unique distribution patterns of metastatic lymph nodes in patients with superficial carcinoma of the thoracic oesophagus. Br J Surg. 1999;86:669–73.
Endo M, Yoshino K, Kawano T, et al. Clinicopathologic analysis of lymph node metastasis in surgically resected superficial cancer of the thoracic esophagus. Dis Esophagus. 2000;13:125–9.
Eguchi T, Nakanishi Y, Shimoda T, et al. Histopathological criteria for additional treatment after endoscopic mucosal resection for esophageal cancer: analysis of 464 surgically resected cases. Mod Pathol. 2006;19:475–80.
Araki K, Ohno S, Egashira A, Saeki H, Kawaguchi H, Sugimachi K. Pathologic features of superficial esophageal squamous cell carcinoma with lymph node and distal metastasis. Cancer. 2002;94:570–5.
Fujita H, Sueyoshi S, Yamana H, et al. Optimum treatment strategy for superficial esophageal cancer: endoscopic mucosal resection versus radical esophagectomy. World J Surg. 2001;25:424–31.
Mitobe J, Ikogami M, Urashima M, et al. Clinicopathological investigation of lymph node metastasis predictors in superficial esophageal squamous cell carcinoma with a focus on evaluation of lympho-vascular invasion. Scand J Gastroenterol. 2013;48(10):1173–82.
Ando N, Iizuka T, Ide H, et al. Surgery plus chemotherapy compared with surgery alone for localized squamous cell carcinoma of the thoracic esophagus: a Japan Clinical Oncology Group Study–JCOG9204. J Clin Oncol. 2003;21(24):4592–6.
Lee J, Lee KE, Im YH, et al. Adjuvant chemotherapy with 5-fluorouracil and cisplatin in lymph node-positive thoracic esophageal squamous cell carcinoma. Ann Thorac Surg. 2005;80(4):1170–5.
Shiozaki A, Yamagishi H, Itoi H, et al. Long-term administration of low-dose cisplatin plus 5-fluorouracil prolongs the postoperative survival of patients with esophageal cancer. Oncol Rep 2005;13(4):667–72.
Huang Q, Luo K, Chen C, et al. Identification and validation of lymphovascular invasion as a prognostic and staging factor in node-negative esophageal squamous cell carcinoma. J Thorac Oncol. 2016;11(4):583–92.
Imamura Y, Watanabe M, Nagai Y, et al. Lymphatic vessel invasion detected by the D2-40 monoclonal antibody is an independent prognostic factor in node-negative esophageal squamous cell carcinoma. J Surg Oncol. 2012;105(3):277–83.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Additional information
Shaohua Wang and Xiaofeng Chen contribute equally to the article.
Rights and permissions
About this article
Cite this article
Wang, S., Chen, X., Fan, J. et al. Prognostic Significance of Lymphovascular Invasion for Thoracic Esophageal Squamous Cell Carcinoma. Ann Surg Oncol 23, 4101–4109 (2016). https://doi.org/10.1245/s10434-016-5416-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5416-8