Abstract
Introduction
Evidence from the American College of Surgeons Oncology Group (ACOSOG) Z0011 trial suggests completion axillary lymph node dissection (cALND) after positive sentinel lymph node biopsy (+SLNB) does not improve outcomes in select patients, leading to practice variation. A multidisciplinary group of surgeons, oncologists, and pathologists developed a regional guideline for cALND which was disseminated in August 2012. We assessed the impact of Z0011 and the regional guideline on cALND rates.
Methods
Consecutive invasive breast cancer cases undergoing SLNB were reviewed at 12 hospitals. Patient, tumor, and process measures were collected for three time periods: TP1, before publication of Z0011 (May 2009–August 2010); TP2, after publication of Z0011 (March 2011–June 2012); and TP3, after guideline dissemination (January 2013–April 2014). Cases were categorized by whether they met the guideline criteria for cALND (i.e. ≤50 years, mastectomy, T3 tumor, three or more positive sentinel lymph nodes [SLNs]) or not (e.g. age > 50 years, breast-conserving surgery, T1/T2 tumor, and one to two positive SLNs).
Results
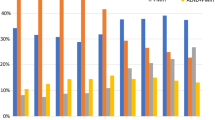
The SLNB rate increased from 56 % (n = 620), to 70 % (n = 774), to 78 % (n = 844) in TP1, TP2, and TP3, respectively. Among cases not recommended for cALND using the guideline criteria, cALND rates decreased significantly over time (TP1, 71 %; TP2, 43 %; TP3, 17 %) [p < 0.001]. The cALND rate also decreased over time among cases recommended to have cALND using the guideline criteria (TP1, 92 %; TP2, 69 %; TP3, 58 %) [p < 0.001]. Based on multivariable analysis, age and nodal factors appeared to be significant factors for cALND decision making.
Conclusion
Publication of ACOSOG Z0011 and regional guideline dissemination were associated with a marked decrease in cALND after +SLNB, even among several cases in which the guideline recommended cALND.
Similar content being viewed by others
References
Krag DN, Anderson SJ, Julian TB, et al. Sentinel-lymph-node resection compared with conventional axillary lymph node dissection in clinically node-negative patients with breast cancer: overall survival findings from the NSABP B-32 randomized phase 3 trial. Lancet Oncol. 2010;11:927–33.
Purushotham AD, Upponi S, Klevesath MB, et al. Morbidity after sentinel lymph node biopsy in primary breast cancer: results from a randomized controlled trial. J Clin Oncol. 2005;23(19):4312–21.
The American Society of Breast Surgeons Board of Directors. Position statement on management of the axilla in patients with invasive breast cancer. https://www.breastsurgeons.org/statements/index.php. Accessed 22 June 2016.
Lyman GH, Giuliano AE, Omerfield MR, et al. American Society of Clinical Oncology guideline recommendations for sentinel lymph node biopsy in early-stage breast cancer. J Clin Oncol. 2005;23:7703–20.
George R, Quan ML, McCready D, et al. Expert panel on SLNB in breast cancer. Sentinel lymph node biopsy in early-stage breast cancer. Toronto, ON: Cancer Care Ontario, Jul 14 2009. Program in Evidence-Based Care Evidence-Based Series No.: 17–5. https://www.cancercare.on.ca/common/pages/UserFile.aspx?fileId=45870. Accessed 22 June 2016.
Anampa J, Makower D, Sparano JA. Progress in adjuvant chemotherapy for breast cancer: an overview. BMC Med. 2015;13:195.
Giuliano AE, Hunt KK, Ballman KV, et al. Axillary dissection vs no axillary dissection in women with invasive breast cancer and sentinel node metastasis: a randomized clinical trial. JAMA. 2011;305:569–75.
Caudle AS, Hunt KK, Kuerer HM, et al. Multidisciplinary considerations in the implementation of the findings from the American College of Surgeons Oncology Group (ACOSOG) Z0011 study: a practice-changing trial. Ann Surg Oncol. 2011;18(9):2407–12.
Barry JM, Weber WP, Sacchini V. The evolving role of axillary lymph node dissection in the modern era of breast cancer management. Surg Oncol. 2012;21:143–5.
Nakamura S. Axillary lymph node dissection in sentinel node positive breast cancer: is it necessary? Curr Opin Obstet Gynecol. 2013. doi:10.1097/GCO.0b013e32834f3608.
Latosinsky S, Berrand TS, Cutter CS, et al. Axillary dissection versus no axillary dissection in women with invasive breast cancer and sentinel node metastasis. Can J Surg. 2012;55:66–69.
Giuliano AE, Morrow M, Duggal S, et al. Should ACOSOG Z0011 change practice with respect to axillary lymph node dissection for a positive sentinel lymph node biopsy in breast cancer? Clin Exp Metastasis. 2012;29:687–92.
Voutsadakis IA, Spadafora S. Axillary lymph node management in breast cancer with positive sentinel lymph node biopsy. World J Clin Oncol. 2015;6(1):1–6.
Galimberti V, Chifu C, Perez SR, et al. Positive axillary sentinel lymph node: is axillary dissection always necessary? Breast. 2011;20(Suppl 3):S96–8.
Morrow M, Giuliano AE. To cut is to cure: can we really apply Z11 in practice? Ann Surg Oncol. 2011;18:2413–5.
Cody HS III, Houssami N. Axillary management in breast cancer: what’s new for 2012? Breast. 2012;21(3):411–5.
Caudle AS, Hunt KK, Tucker SL, et al. American College of Surgeons Oncology Group (ACOSOG) Z0011: impact on surgeon practice patterns. Ann Surg Oncol. 2012;19(10):3144–51.
Joyce DP, Lowery AJ, McGrath-Soo LB, et al. Management of the axilla: has Z0011 had an impact? Ir J Med Sci. 2016;185(1):145–9.
Wright GP, Mater ME, Sobel HL, et al. Measuring the impact of the American College of Surgeons Oncology Group Z0011 trial on breast cancer surgery in a community healthy system. Am J Surg. 2015;209:240–5.
Jamtvedt G, Young JM, Kristoffersen DT, et al. Does telling people what they have been doing change what they do? A systematic review of the effects of audit and feedback. Qual Saf Health Care. 2006;15:433–6.
Grimshaw J, Eccles M, Walter A, et al. Changing physician’s behaviour; what works and thoughts on getting more things to work. J Cont Educ Health Prof. 2002;22:237–43.
Flodgren G, Parmelli E, Doumit G, et al. Local opinion leaders: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2011. doi:10.1002/14651858.CD000125.pub4.
Forsetlund L, Bjorndal A, Rashidian A, et al. Continuing education meetings and workshops: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2009. doi:10.1002/14651858.CD003030.pub2.
O’Brien MA, Oxman AD, Davis DA, et al. Educational outreach visits: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2007;(2):CD000409.
American Society of Breast Surgeons. Performance and practice guidelines for axillary lymph node dissection in breast cancer patients—Nov. 2014. https://www.breastsurgeons.org/new_layout/about/statements/PDF_Statements/PerformancePracticeGuidelines_ALND.pdf. Accessed Dec 2015.
Lyman GH, Temin S, Edge S, et al. Sentinel lymph node biopsy for patients with early-stage breast cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2014;32:1365–86.
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology V3.2015. www.consensocancermamario.com/guias/NCCN_2015.pdf. Accessed 23 June 2016.
Lovrics PJ, Hodgson N, O’Brien MA, et al. Results of a surgeon-directed quality improvement project on breast cancer surgery outcomes in South-Central Ontario. Ann Surg Oncol. 2014;21:2181–7.
Tsao MW, Cornacchi SD, Lovrics PJ, et al. Factors affecting the implementation of a regional guideline for completion axillary lymph node dissection: a qualitative study of physician opinions. Canadian Centre for Applied Research in Cancer Control (ARCC) Conference 2016, Toronto, ON. 2016. http://cc-arcc.ca/wpcontent/uploads/2015/12/Final-Web-ARCC-Program.pdf. Accessed 22 June 2016.
Fisher B, Redmond C, Fisher ER, et al. Ten-year results of a randomized clinical trial comparing radical mastectomy and total mastectomy with or without radiation. N Engl J Med. 1985;312(11):674–81.
Gatzemeier W, Mann GB. Which sentinel lymph-node (SLN) positive breast cancer patient needs an axillary lymph-node dissection (ALND)—ACOSOG Z0011 results and beyond. Breast J. 2013;22(3):211–6.
Goyal A, Dodwell D, Reed MW, et al. Axillary treatment in women with one or two sentinel nodes with macrometastases: more evidence is needed to inform practice. J Clin Oncol. 2014;32:3902.
Doherty S. History of evidence-based medicine. Oranges, chloride of lime and leeches: barriers to teaching old dogs new tricks. Emerg Med Australas. 2005;17:314–21.
Langer I, Guller U, Berclaz G, et al. Morbidity of sentinel lymph node biopsy (SLN) alone versus SLN and completion axillary lymph node dissection after breast cancer surgery: a prospective Swiss multicenter study on 659 patients. Ann Surg. 2007;245(3):452–61.
Yi M, Giordano SH, Meric-Bernstam F, et al. Trends in and outcomes from sentinel lymph node biopsy (SLNB) alone vs. SLNB with axillary lymph node dissection for node-positive breast cancer patients: experience from the SEER database. Ann Surg Oncol. 2010;17:343–51.
Bilimoria KY, Bentrem DJ, Hansen NM, et al. Comparison of sentinel lymph node biopsy alone and completion axillary lymph node dissection for node-positive breast cancer. J Clin Oncol. 2009;27(18):2946–53.
Van Der Hage JA, Van de Velde JP, Tubiana-Hulin M, et al. Preoperative chemotherapy in primary operable breast cancer: results from the European Organization for Research and Treatment of Cancer trial 10902. J Clin Oncol. 2001;19:4224–37.
Donker M, Van Tienhoven G, Straver ME, et al. Radiotherapy or surgery of the axilla after a positive sentinel node in breast cancer (EORTC 10981-22023 AMAROS): a randomized, multicenter, open-label, phase 3 non-inferiority trial. Lancet Oncol. 2014;15(12):1303–10.
Li CZ, Zhang P, Li RW, et al. Axillary lymph node dissection versus sentinel lymph node biopsy alone for early breast cancer with sentinel node metastasis: a meta-analysis. Eur J Surg Oncol. 2015;41:958–66.
Wang J, Mittendorf EA, Sahin AA, et al. Outcomes of sentinel lymph node dissection alone vs. axillary lymph node dissection in early stage invasive lobular carcinoma: a retrospective study of the surveillance, epidemiology and end results (SEER) database. PLoS One. 2014;9:e89778.
Zakaria S, Degnim AC, Kleer CG, et al. Sentinel lymph node biopsy for breast cancer: how many nodes are enough? J Surg Oncol. 2007;96:554–9.
Lee MK, Varzi LA, Chung DU, et al. The effect of young age in hormone receptor positive breast cancer. Biomed Res Int. 2015;2015:325715.
Woolf SH, Grol R, Hutchinson A, et al. Clinical guidelines: potential benefits, limitations, and harms of clinical guidelines. BMJ. 1999;318:527–30.
Natsch S, van der Meer JWM. The role of clinical guidelines, policies and stewardship. J Hosp Infect. 2003;53(3):172–6.
Acknowledgment
The authors would like to thank Dyda Dao, Dominika Bhatia, and Olivia Lovrics for their assistance with data collection and management.
Funding
Funding was provided by the Hamilton Academic Health Sciences Organization (HAHSO) Innovation Grant, and by funds from the Department of Surgery, McMaster University and the McMaster Buffet Taylor Breast Cancer Research Chair, Department of Oncology, McMaster University. The funding sources played no role in the design, conduct, or reporting of this study.
Disclosure
Miriam W. Tsao, Sylvie D. Cornacchi, Nicole Hodgson, Marko Simunovic, Lehana Thabane, Ji Cheng, Mary Ann O’Brien, Barbara Strang, Som D. Mukherjee, and Peter J. Lovrics have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsao, M.W., Cornacchi, S.D., Hodgson, N. et al. A Population-Based Study of the Effects of a Regional Guideline for Completion Axillary Lymph Node Dissection on Axillary Surgery in Patients with Breast Cancer. Ann Surg Oncol 23, 3354–3364 (2016). https://doi.org/10.1245/s10434-016-5310-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5310-4