Abstract
Background
The American Society of Clinical Oncology (ASCO) guidelines include incorporation of fertility preservation guidelines in the care of breast oncology patients. This study aimed to examine the baseline knowledge and preferences concerning fertility preservation among women of childbearing age with newly diagnosed breast cancer at the time of their initial visit to Memorial Sloan Kettering Cancer Center (MSKCC).
Methods
A questionnaire on reproductive history, fertility knowledge, and preservation options was administered to women 18–45 years of age with newly diagnosed breast cancer at MSKCC between May and September 2011.
Results
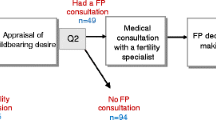
The inclusion criteria were met by 60 women eligible for analysis who had a median age of 40 years (range 20–45 years). The findings showed that 50 % of the women either desired children in the future or were unsure whether they wanted children, with 9 % reporting that they received information about fertility preservation options before their MSKCC visit. Women who had never been pregnant were more likely than those with prior pregnancies to consider having children in the future (p = 0.001) and to contemplate fertility preservation options both before (p = 0.001) and after (p = 0.0002) cancer treatment.
Conclusion
Early referral allows patients to take advantage of fertility preservation options while preventing delay in the initiation of systemic therapy. Referral by the breast surgical oncologist at the time of the initial visit has the potential to increase fertility knowledge because it appears that many women have not yet received fertility information at this early treatment stage.
Similar content being viewed by others
References
Department of Health and Human Services, Centers for Disease Control and Prevention, and the National Cancer Institute. U.S. Cancer Statistics Working Group. United States Cancer Statistics: 1999–2011 Incidence and Mortality Web-Based Report, Atlanta, GA, 2014.
Ferlay J, Soerjomataram I, Dikshit R, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359–86.
Bao T, Davidson NE. Gene expression profiling of breast cancer. Adv Surg. 2008;42:249–60.
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015;65:5–29.
Toi M, Iwata H, Yamanaka T, et al. Clinical significance of the 21-gene signature (oncotype DX) in hormone receptor-positive early stage primary breast cancer in the Japanese population. Cancer. 2010;116:3112–8.
Cooke A, Mills TA, Lavender T. “Informed and uninformed decision making”: women’s reasoning, experiences and perceptions with regard to advanced maternal age and delayed childbearing: a meta-synthesis. Int J Nurs Stud. 2010;47:1317–29.
Benzies K, Tough S, Tofflemire K, et al. Factors influencing women’s decisions about timing of motherhood. J Obstet Gynecol Neonatal Nurs. 2006;35:625–33.
Mathews TJHB. First Births to Older Women Continue to Rise. NCHS data brief, no 152. National Center for Health Statistics, Hyattsville, MD, 2014.
Trivers KF, Fink AK, Partridge AH, et al. Estimates of young breast cancer survivors at risk for infertility in the U.S. Oncologist. 2014;19:814–22.
Ben-Aharon I, Shalgi R. What lies behind chemotherapy-induced ovarian toxicity? Reproduction. 2012;144:153–63.
Tham YL, Sexton K, Weiss H, et al. The rates of chemotherapy-induced amenorrhea in patients treated with adjuvant doxorubicin and cyclophosphamide followed by a taxane. Am J Clin Oncol. 2007;30:126–32.
Moore HC, Unger JM, Phillips KA, et al. Goserelin for ovarian protection during breast-cancer adjuvant chemotherapy. N Engl J Med. 2015;372:923–32.
Anderson RA, Wallace WH. Antimullerian hormone, the assessment of the ovarian reserve, and the reproductive outcome of the young patient with cancer. Fertil Steril. 2013;99:1469–75.
Rosendahl M, Andersen CY, la Cour Freiesleben N, et al. Dynamics and mechanisms of chemotherapy-induced ovarian follicular depletion in women of fertile age. Fertil Steril. 2010;94:156–66.
Partridge AH, Gelber S, Peppercorn J, et al. Web-based survey of fertility issues in young women with breast cancer. J Clin Oncol. 2004;22:4174–83.
Ruddy KJ, Gelber SI, Tamimi RM, et al. Prospective study of fertility concerns and preservation strategies in young women with breast cancer. J Clin Oncol. 2014;32:1151–6.
Schover LR, Rybicki LA, Martin BA, et al. Having children after cancer: a pilot survey of survivors’ attitudes and experiences. Cancer. 1999;86:697–709.
Peate M, Meiser B, Friedlander M, et al. It’s now or never: fertility-related knowledge, decision-making preferences, and treatment intentions in young women with breast cancer: an Australian fertility decision aid collaborative group study. J Clin Oncol. 2011;29:1670–7.
Jukkala AM, Azuero A, McNees P, et al. Self-assessed knowledge of treatment and fertility preservation in young women with breast cancer. Fertil Steril. 2010;94:2396–8.
Vadaparampil ST, Christie J, Quinn GP, et al. A pilot study to examine patient awareness and provider discussion of the impact of cancer treatment on fertility in a registry-based sample of African American women with breast cancer. Support Care Cancer. 2012;20:2559–64.
Kasum M, Beketic-Oreskovic L, Peddi PF, et al. Fertility after breast cancer treatment. Eur J Obstet Gynecol Reprod Biol. 2014;173:13–8.
Gorman JR, Su HI, Roberts SC, et al. Experiencing reproductive concerns as a female cancer survivor is associated with depression. Cancer. 2015;121:935–42.
Letourneau JM, Ebbel EE, Katz PP, et al. Pretreatment fertility counseling and fertility preservation improve quality of life in reproductive age women with cancer. Cancer. 2012;118:1710–7.
Peate M, Meiser B, Cheah BC, et al. Making hard choices easier: a prospective, multicentre study to assess the efficacy of a fertility-related decision aid in young women with early-stage breast cancer. Br J Cancer. 2012;106:1053–61.
Loren AW, Mangu PB, Beck LN, et al. Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013;31:2500–10.
Quinn GP, Vadaparampil ST, Lee JH, et al. Physician referral for fertility preservation in oncology patients: a national study of practice behaviors. J Clin Oncol. 2009;27:5952–7.
Canada AL, Schover LR. The psychosocial impact of interrupted childbearing in long-term female cancer survivors. Psychooncology. 2012;21:134–43.
Baynosa J, Westphal LM, Madrigrano A, et al. Timing of breast cancer treatments with oocyte retrieval and embryo cryopreservation. J Am Coll Surg. 2009;209:603–7.
Lee S, Ozkavukcu S, Heytens E, et al. Value of early referral to fertility preservation in young women with breast cancer. J Clin Oncol. 2010;28:4683–6.
Avis NE, Levine B, Naughton MJ, et al. Age-related longitudinal changes in depressive symptoms following breast cancer diagnosis and treatment. Breast Cancer Res Treat. 2013;139:199–206.
Acknowledgment
This study was funded in part through NIH/NCI Cancer Center Support Grant P30 CA008748.
Disclosures
The authors have no disclosures to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goldfarb, S.B., Kamer, S.A., Oppong, B.A. et al. Fertility Preservation for the Young Breast Cancer Patient. Ann Surg Oncol 23, 1530–1536 (2016). https://doi.org/10.1245/s10434-015-5036-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-5036-8