Abstract
Background
Little is known about the long-term effects of surgical approach and type of anastomosis in the surgical treatment of esophageal cancer on patient-reported outcomes.
Methods
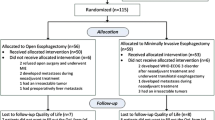
A Swedish nationwide, population-based cohort study included patients undergoing esophagectomy for esophageal cancer in 2001–2005. The predefined exposures included surgical approach (transhiatal or transthoracic) and anastomotic technique (hand-sewn or mechanical). The outcomes were esophageal-specific symptoms 3 years after the surgery. Symptoms were measured using the cancer-specific quality of life questionnaire, the QLQ-C30, supplemented by an esophageal cancer-specific module (QLQ-OES18), both developed by the European Organisation for Research and Treatment of Cancer. Logistic regression models were used to estimate relative risk, expressed as odds ratios (OR) with 95 % confidence intervals (CI), of experiencing symptoms as assessed by the questionnaires.
Results
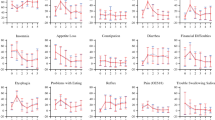
Among the 178 included patients, there was an 84 % participation rate. No statistically significant differences were found regarding surgical approach. However, point estimates indicate that patients operated on with a transhiatal approach had a lower risk for symptoms of nausea and vomiting (OR = 0.5, 95 % CI 0.1–1.9), diarrhea (OR = 0.5, 95 % CI 0.2–1.8), and trouble swallowing (OR = 0.4, 95 % CI 0–3), and a slightly higher risk for loss of appetite (OR = 2, 95 % CI 0.7–5.6) compared with patients operated on with a transthoracic approach. Anastomotic technique did not seem to influence the risk for any of the selected symptoms.
Conclusions
Surgical approach and type of anastomosis do not seem to influence the risk of general and esophageal-specific cancer symptoms 3 years after surgery for esophageal cancer.
Similar content being viewed by others
References
Mariette C, Piessen G, Triboulet JP. Therapeutic strategies in oesophageal carcinoma: role of surgery and other modalities. Lancet Oncol. 2007;8(6):545–53.
Sundelof M, et al. Improved survival in both histologic types of oesophageal cancer in Sweden. Int J Cancer. 2002;99(5):751–4.
Djarv T, Blazeby JM, Lagergren P. Predictors of postoperative quality of life after esophagectomy for cancer. J Clin Oncol. 2009;27(12):1963–8.
Omloo JM, et al. Extended transthoracic resection compared with limited transhiatal resection for adenocarcinoma of the mid/distal esophagus: five-year survival of a randomized clinical trial. Ann Surg. 2007;246(6):992–1000; discussion 1000-1.
Rutegard M, et al. Population-based study of surgical factors in relation to health-related quality of life after oesophageal cancer resection. Br J Surg. 2008;95(5):592–601.
Viklund P, et al. Quality of life and persisting symptoms after oesophageal cancer surgery. Eur J Cancer. 2006;42(10):1407–14.
Conroy T, Marchal F, Blazeby JM. Quality of life in patients with oesophageal and gastric cancer: an overview. Oncology. 2006;70(6):391–402.
Lagergren P, et al. Health-related quality of life among patients cured by surgery for esophageal cancer. Cancer. 2007;110(3):686–93.
Viklund P, et al. Risk factors for complications after esophageal cancer resection: a prospective population-based study in Sweden. Ann Surg. 2006;243(2):204–11.
Aaronson NK, et al. The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst. 1993;85(5):365–76.
Blazeby JM, et al. Clinical and psychometric validation of an EORTC questionnaire module, the EORTC QLQ-OES18, to assess quality of life in patients with oesophageal cancer. Eur J Cancer. 2003;39(10):1384–94.
Djarv T, Lagergren P. Six-month postoperative quality of life predicts long-term survival after oesophageal cancer surgery. Eur J Cancer. 2011;47(4):530–5.
Dresner SM, Griffin SM. Pattern of recurrence following radical oesophagectomy with two-field lymphadenectomy. Br J Surg. 2000;87(10):1426–33.
Lazarus RS. Coping theory and research: past, present, and future. Psychosom Med. 1993;55(3):234–47.
Sprangers MA, Schwartz CE. Integrating response shift into health-related quality of life research: a theoretical model. Soc Sci Med. 1999;48(11):1507–15.
Hulscher JB, et al. Extended transthoracic resection compared with limited transhiatal resection for adenocarcinoma of the esophagus. N Engl J Med. 2002;347(21):1662–9.
de Boer AG, et al. Quality of life after transhiatal compared with extended transthoracic resection for adenocarcinoma of the esophagus. J Clin Oncol. 2004;22(20):4202–8.
Markar SR, et al. Hand-sewn versus stapled oesophago-gastric anastomosis: systematic review and meta-analysis. J Gastrointest Surg. 2011;15(5):876–84.
Ercan S, et al. Does esophagogastric anastomotic technique influence the outcome of patients with esophageal cancer? J Thorac Cardiovasc Surg. 2005;129(3):623–31.
Blackmon SH, et al. Propensity-matched analysis of three techniques for intrathoracic esophagogastric anastomosis. Ann Thorac Surg. 2007;83(5):1805–13; discussion 1813.
Singh D, et al. Experience and technique of stapled mechanical cervical esophagogastric anastomosis. Ann Thorac Surg. 2001;71(2):419–24.
Parameswaran R, et al. The role of health-related quality of life outcomes in clinical decision making in surgery for esophageal cancer: a systematic review. Ann Surg Oncol. 2008;15(9):2372–9.
Acknowledgment
Funding was provided by the Swedish Cancer Society and the Swedish Research Council.
Conflict of interest
There are no conflicts of interest reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van der Schaaf, M., Rutegård, M. & Lagergren, P. The Influence of Surgical Factors on Persisting Symptoms 3 Years after Esophageal Cancer Surgery: A Population-Based Study in Sweden. Ann Surg Oncol 20, 1639–1645 (2013). https://doi.org/10.1245/s10434-012-2690-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2690-y