Abstract
Background
The combination of acetaminophen, codeine, and caffeine (Tylenol 3, T3) is a standard postoperative analgesia after breast surgery despite the adverse effects and variable efficacy of narcotics. This study compared the efficacy of a nonnarcotic approach (acetaminophen and ibuprofen; AcIBU) to T3 after outpatient breast surgery.
Methods
This double-blind randomized equivalence trial involved patients undergoing outpatient breast surgery. Patients were randomized (stratified by procedure type) to receive AcIBU or T3 four times daily for 7 days, or until free of pain. Pain intensity, measured four times daily by the visual analog scale, was the primary outcome; secondary outcomes were pain relief with analgesic, days until freedom from pain, adverse effects, discontinuation of drug as a result of adverse effects, and patient satisfaction.
Results
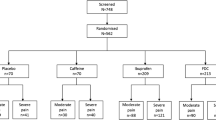
There were 71 patients randomized to AcIBU and 70 patients to T3. Repeated measures analysis showed no significant difference in average pain intensity over 7 days (AcIBU 19.9 mm vs. T3 20.6 mm; P = 0.78). Similarly, there was no significant difference in pain relief with analgesic (P = 0.46). Although no difference in the incidence of adverse effects was observed (P = 0.94), discontinuation of the study drug as a result of adverse effects was more common with T3 (19 % vs. 6 %; P = 0.018). No significant differences were identified in days until freedom from pain or patient satisfaction; 92 % of AcIBU and 89 % of T3 patients were satisfied with their pain control (P = 0.55).
Conclusions
AcIBU is a safe, effective method of pain control after outpatient breast surgery. Compared to T3, it provides at least equivalent analgesia and has a more tolerable adverse effect profile.



Similar content being viewed by others
References
Horner MJ, Ries LAG, Krapcho M, et al. SEER cancer statistics review, 1975–2006. Bethesda, MD: National Cancer Institute; 2009.
Canadian Cancer Society. Cancer statistics, 2010. November 2010. http://www.cancer.ca/canada-wide/about%20cancer/cancer%20statistics/~/media/CCS/Canada%20wide/Files%20List/English%20files%20heading/pdf%20not%20in%20publications%20section/Canadian20Cancer20Statistics2020102020English.ashx.
Veerbeek L, van der Geest L, Wouters M, et al. Enhancing the quality of care for patients with breast cancer: seven years of experience with a Dutch auditing system. Eur J Surg Oncol. 2011;37:714–8.
Bian J, Halpern MT. Trends in outpatient breast cancer surgery among Medicare fee-for-service patients in the United States from 1993 to 2002. Chin J Cancer. 2011;30:197–203.
Beauregard L, Pomp A, Choiniere M. Severity and impact of pain after day-surgery. Can J Anaesthes. 1998;45:304–11.
Zuckerman LA, Ferrante FM. Nonopioid and opioid analgesics. In: Ashburn MA, Rice LJ, editors. The management of pain. New York: Churchill Livingstone; 1998. p. 111–40.
Miller RD. Anesthesia. St Louis: Mosby; 1994.
Souter AJ, Fredman B, White PF. Controversies in the perioperative use of nonsterodial antiinflammatory drugs. Anesth Analg. 1994;79:1178–90.
Place RJ, Coloma M, White PF, et al. Ketorolac improves recovery after outpatient anorectal surgery. Dis Colon Rectum. 2000;43:804–8.
White PF, Joshi GP, Carpenter RL, et al. A comparison of oral ketorolac and hydrocodone–acetaminophen for analgesia after ambulatory surgery: arthroscopy versus laparoscopic tubal ligation. Anesth Analg. 1997;85:37–43.
Raeder JC, Steine S, Vatsgar TT. Oral ibuprofen versus paracetamol plus codeine for analgesia after ambulatory surgery. Anesth Analg. 2001;92:1470–2.
Chan A, Doré CJ, Ramachandra V. Analgesia for day surgery. Evaluation of the effect of diclofenac given before or after surgery with or without bupivacaine infiltration. Anesthesia. 1996;51:592–5.
Legeby M, Sandelin K, Wickman M, Olofsson C. Analgesic efficacy of diclofenac in combination with morphine and paracetamol after mastectomy and immediate breast reconstruction. Acta Anaesthesiol Scand. 2005;49:1360–6.
Bosek V, Cox CE. Comparison of analgesic effect of locally and systemically administered ketorolac in mastectomy patients. Ann Surg Oncol. 1996;3:62–6.
Kelly AM. Setting the benchmark for research in the management of acute pain in emergency departments. Emerg Med. 2001;13:57–60.
Todd KH, Funk KG, Funk JP, et al. Clinical significance of reported changes in pain severity. Ann Emerg Med. 1996;27:485–9.
Talbot H, Hutchinson SP, Edbrooke DL, Wrench I, Kohlhardt SR. Evaluation of a local anesthesia regimen following mastectomy. Anesthesia. 2004;59:664–7.
Jensen MP, Chen C, Brugger AM. Interpretation of visual analog scale ratings and change scores: a reanalysis of two clinical trials of postoperative pain. J Pain. 2003;4:407–14.
Mitchell AD, VanZanten S, Inglis KM, Porter GA. A randomized controlled trial comparing acetaminophen plus ibuprofen versus acetaminophen plus codeine plus caffeine (Tylenol #3®) after outpatient general surgery. J Am College Surg. 2008;206:472–9.
Dexter F, Chestnut DH. Analysis of statistical tests to compare visual analog scale measurements among groups. Anesthesiology. 1995;82:896–902.
Revill SI, Robinson JO, Rosen M, et al. The reliability of a linear analogue for evaluating pain. Anesthesia. 1976;31:1191–8.
Nauta M, Landsmeer ML, Koren G. Codeine–acetominophen versus nonsteroidal anti-inflammatory drugs in the treatment of post-abdominal surgery pain: a systematic review of randomized trials. Am J Surg. 2009;198:256–61.
Yeh CC, Yu JC, Wu CT, Ho ST, Chang TM, Wong CS. Thoracic epidural anesthesia for pain relief and postoperation recovery with modified radical mastectomy. World J Surg. 1999;23:256–60.
Sundarathiti P, Pasutharnchat K, Kongdan Y, Suranutkarin PE. Thoracic epidural anesthesia (TEA) with 0.2 % ropivacaine in combination with ipsilateral brachial plexus block (BPB) for modified radical mastectomy (MRM). J Med Assoc Thai. 2005;88:513–20.
Atanassoff PG, Alon E, Weiss BM. Intercostal nerve block for lumpectomy: superior postoperative pain relief with bupivacaine. J Clin Anesth. 1994;6:47–51.
Thavaneswaran P, Rudkin GE, Cooter RD, Moyes DG, Perera CL, Maddern GJ. Paravertebral block for anesthesia: a systematic review. Anesth Analg. 2010;110:1740–4.
Terheggen MA, Wille F, Borel Rinkes IH, Ionescu TI, Knape JT. Paravertebral blockade for minor breast surgery. Anesth Analg. 2002;94:355–9.
Grover VK, Mathew PJ, Yaddanapudi S, Sehgal S. A single dose of preoperative gabapentin for pain reduction and requirement of morphine after total mastectomy and axillary dissection: randomized placebo-controlled double-blind trial. J Postgrad Med. 2009;55:257–60.
Williams DG, Patel A, Howard RF. Pharmacogenetics of codeine metabolism in an urban population of children and its implications for analgesic reliability. Br J Anaesth. 2002;89:839–45.
Govindarajan R, Ghosh B, Sathyamoorthy MK, et al. Efficacy of ketorolac in lieu of narcotics in the operative management of laparoscopic surgery for morbid obesity. Surg Obes Relat Dis. 2005;1:530–5.
Pillai Riddell RR, Craig KD. Time-contingent schedules for postoperative analgesia: a review of the literature. J Pain. 2003;4:169–75.
Acknowledgment
Funded by a Capital District Health Authority Research grant and the Ramia Chair in Surgical Oncology Research. Lucy Helyer, MD, FRCSC, Trevor Topp, MD, FRCSC, FACS, Virginia Calverly, MD, FRCSC, and Carmen Giacomantonio, MD, FRCSC, greatly contributed by recruiting their patients to this trial. We thank Kevin Druhan for his assistance in data entry and management; Hoan Linh Banh, PhD, for her assistance with the pharmacy; and the clinic and perioperative nursing staff at the Victoria General Hospital and IWK Hospital in Halifax, Nova Scotia, for their enthusiastic support of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mitchell, A., McCrea, P., Inglis, K. et al. A Randomized, Controlled Trial Comparing Acetaminophen Plus Ibuprofen versus Acetaminophen Plus Codeine Plus Caffeine (Tylenol 3) after Outpatient Breast Surgery. Ann Surg Oncol 19, 3792–3800 (2012). https://doi.org/10.1245/s10434-012-2447-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2447-7